Abstract
Sepsis is a life-threatening organ dysfunction caused by a dysregulated host response to infection. It is a major health concern and causes substantial morbidity and mortality. It is imperative that the signs of sepsis are identified early in both adult and paediatric patients and appropriately escalated to initiate early treatment and improve prognosis. This paper aims to discuss the change in classification from the previous systemic inflammatory response syndrome (SIRS) criteria to the current definition in adults and also the unchanged definition in children. The hallmark signs of sepsis (both red and amber flags) are discussed in relation to their underlying cellular mechanisms to provide a comprehensive overview for clinicians in primary care, hospital and community settings. The rise of antimicrobial resistance is also an increasing global health concern with resistant bacteria from common infections likely to result in greater patient morbidity and worse outcomes.
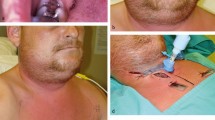
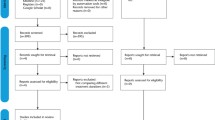
A literature search identified reported sepsis cases in dentistry through searches in Ovid Medline and Embase from January 1990 to December 2019. Only primary studies were included with no restrictions on languages. Four articles were identified which reported sepsis associated with tooth extractions, dental abscess and submental/submandibular cellulitis. It is well known that locoregional infections of dental origin have the potential to cause sepsis. Therefore, dental healthcare professionals need to be vigilant and understand the specific signs and escalation protocols to ensure patient safety.
Key points
-
The aim of this review is to provide a comprehensive overview of sepsis, including its classification, cellular mechanisms and clinical signs.
-
A summary of the literature on dental infections causing sepsis is also provided.
-
Clinicians in primary care, hospital settings and community will be able to identify the red and amber flags of sepsis and understand their responsibilities with regards to appropriate antimicrobial prescribing.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Singer M, Deutschman C S, Seymour C W et al. The Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3). JAMA 2016; 315: 801-810.
Rudd K E, Johnson S C, Agesa K M et al. Global, regional, and national sepsis incidence and mortality, 1990-2017: analysis for the Global Burden of Disease Study. Lancet 2020; 395: 200-211.
The UK Sepsis Trust. Summary Information United Kingdom. 2018. Available at https://sepsistrust.org/wp-content/uploads/2018/12/Summary-Information-re-UKST-1.pdf (accessed April 2020).
Office for National Statistics. Number of sepsis deaths and age-standardised mortality rates by sex, England and Wales: 2001 to 2017. 2019. Available online at https://www.ons.gov.uk/peoplepopulationandcommunity/birthsdeathsandmarriages/deaths/adhocs/009600 numberofsepsisdeathsandagestandardisedmortality ratesbysexenglandandwales2001to2017 (accessed April 2020).
The UK Sepsis Trust. The Sepsis Manual United Kingdom. 2017. Available at https://sepsistrust.org/wp-content/uploads/2018/06/Sepsis_Manual_2017_web_download.pdf (accessed April 2020).
World Health Organisation. Improving the prevention, diagnosis and clinical management of sepsis. 2017. Available at https://apps.who.int/gb/ebwha/pdf_files/WHA70/A70_13-en.pdf (accessed April 2020).
NHS England. Improving outcomes for patients with sepsis. 2015. Available at https://www.england.nhs.uk/wp-content/uploads/2015/08/Sepsis-Action-Plan-23.12.15-v1.pdf (accessed April 2020).
Carter L, Lowis E. Death from overwhelming odontogenic sepsis: a case report. Br Dent J 2007; 203: 241-242.
Coelho C, Mead M. Sepsis: the applicability to dental care professionals. Br Dent J 2018; 225: 1078-1081.
Kaukonen K M, Bailey M, Pilcher D, Cooper D J, Bellomo R. Systemic inflammatory response syndrome criteria in defining severe sepsis. N Engl J Med 2015; 372: 1629-1638.
Marik P E, Taeb A M. SIRS, qSOFA and new sepsis definition. J Thorac Dis 2017; 9: 943-945.
National Institute for Health and Care Excellence. Sepsis. 2019. Available online at https://cks.nice.org.uk/sepsis (accessed March 2020).
Kawasaki T. Update on paediatric sepsis: a review. J Intensive Care 2017; 5: 47.
Goldstein B, Giroir B, Randolph A. International paediatric sepsis consensus conference: definitions for sepsis and organ dysfunction in paediatrics. Pediatr Crit Care Med 2005; 6: 2-8.
Cvetkovic M, Lutman D, Ramnarayan P, Pathan N, Inwald D P, Peters M J. Timing of death in children referred for intensive care with severe sepsis: implications for interventional studies. Pediatr Crit Care Med 2015; 16: 410-417.
Weiss S L, Fitzgerald J C, Pappachan J et al. Global epidemiology of paediatric severe sepsis: the sepsis prevalence, outcomes, and therapies study. Am J Respir Crit Care Med 2015; 191: 1147-1157.
The UK Sepsis Trust. Clinical Tools. 2020. Available at https://sepsistrust.org/professional-resources/clinical-tools/ (accessed April 2020).
Gudiol C, Bodro M, Simonetti A et al. Changing aetiology, clinical features, antimicrobial resistance, and outcomes of bloodstream infection in neutropenic cancer patients. Clin Microbiol Infect 2013; 19: 474-479.
Akira S, Uematsu S, Takeuchi O. Pathogen Recognition and Innate Immunity. Cell 2006; 124: 783-801.
Freire M O, Van Dyke T E. Natural resolution of inflammation. Periodontol 2000 2013; 63: 149-164.
National Institute for Health and Care Excellence. Do Not Do Recommendation. 2016. Available at https://www.nice.org.uk/donotdo/do-not-rely-on-fever-or-hypothermia-to-rule-sepsis-either-in-or-out (accessed April 2020).
Minasyan H. Sepsis: mechanisms of bacterial injury to the patient. Scand J Trauma Resusc Emerg Med 2019; 27: 19.
Wang H. Disseminated intravascular coagulation. 2020. Available at https://bestpractice.bmj.com/topics/en-gb/184 (accessed April 2020).
Hotchkiss R S, Moldawer L L, Opal S M, Reinhart K, Turnbull I R, Vincent J-L. Sepsis and septic shock. Nat Rev Dis Primers 2016; 2: 16045.
Simmons J, Pittet J-F. The coagulopathy of acute sepsis. Curr Opin Anaesthesiol 2015; 28: 227-236.
Stearns-Kurosawa D J, Osuchowski M F, Valentine C, Kurosawa S, Remick D G. The pathogenesis of sepsis. Annu Rev Pathol 2011; 6: 19-48.
Kim W-Y, Hong S-B. Sepsis and Acute Respiratory Distress Syndrome: Recent Update. Tuberc Respir Dis (Seoul) 2016; 79: 53-57.
Dremsizov T, Clermont G, Kellum J A, Kalassian K G, Fine M J, Angus D C. Severe Sepsis in Community-Acquired Pneumonia: When Does It Happen, and Do Systemic Inflammatory Response Syndrome Criteria Help Predict Course? Chest 2006; 129: 968-978.
NICE. Pneumonia in adults. 2016. Available at https://www.nice.org.uk/guidance/qs110/chapter/Quality-statement-1-Mortality-risk-assessment-in-primary-care-using-CRB65-score (accessed May 2020).
Drosatos K, Lymperopoulos A, Kennel P J, Pollak N, Schulze P C, Goldberg I J. Pathophysiology of sepsis-related cardiac dysfunction: driven by inflammation, energy mismanagement, or both? Curr Heart Fail Rep 2015; 12: 130-140.
Antonucci E, Fiaccadori E, Donadello K, Taccone F S, Franchi F, Scolletta S. Myocardial depression in sepsis: From pathogenesis to clinical manifestations and treatment. J Crit Care 2014; 29: 500-511.
Merx M W, Weber C. Sepsis and the Heart. Circulation 2007; 116: 793-802.
Schrier R W, Wang W. Acute renal failure and sepsis. N Engl J Med 2004; 351: 159-169.
Majumdar A. Sepsis-induced acute kidney injury. Indian J Crit Care Med 2010; 14: 14-21.
Choi H M, Kim S C, Kim M-G, Jo S-K, Cho W Y, Kim H K. Etiology and outcomes of anuria in acute kidney injury: a single centre study. Kidney Res Clin Pract 2015; 34: 13-19.
Prowle J R, Liu Y-L, Licari E et al. Oliguria as predictive biomarker of acute kidney injury in critically ill patients. Crit Care 2011; 15: R172.
Royal College of Physicians of Edingburgh. Acute kidney injury. 2013. Available at https://www.rcpe.ac.uk/sites/default/files/files/aki-app-content.pdf (accessed May 2020).
Tsuruta R, Oda Y. A clinical perspective of sepsis-associated delirium. J Intensive Care 2016; 4: 18.
van de Beek D, de Gans J, Spanjaard L, Weisfelt M, Reitsma J B, Vermeulen M. Clinical Features and Prognostic Factors in Adults with Bacterial Meningitis. N Engl J Med 2004; 351: 1849-1859.
Meningitis Research Foundation. Symptoms checker. 2020. Available online at https://www.meningitis.org/meningitis/check-symptoms (accessed May 2020).
The UK Sepsis Trust. ED/AMU Sepsis Screening & Action Tool. 2018. Available at https://sepsistrust.org/wp-content/uploads/2018/06/ED-adult-NICE-Final-1107.pdf (accessed April 2020).
Lee J J, Hahn L J, Kao T P et al. Post-tooth extraction sepsis without locoregional infection-a population-based study in Taiwan. Oral Dis 2009; 15: 602-607.
Moss H, Collier J M, Collier S. 'An unusual response of dental sepsis to antibiotics: parallels with the Jarisch-Herxheimer reaction'. BMJ Case Rep 2012; DOI: 10.1136/bcr.07.2011.4500.
Currie W J R, Ho V. An unexpected death associated with an acute dentoalveolar abscess - report of a case. Br J Oral Maxillofac Surg 1993; 31: 296-298.
Heimdahl A, Hall G, Hedberg M et al. Detection and quantitation by lysis-filtration of bacteraemia after different oral surgical procedures. J Clin Microbiol 1990; 28: 2205-2209.
Roberts G J, Holzel H S, Sury M R, Simmons N A, Gardner P, Longhurst P. Dental bacteraemia in children. Pediatr Cardiol 1997; 18: 24-27.
National Institute for Health and Care Excellence. Sepsis. 2020. Available at https://www.nice.org.uk/guidance/ng51 (accessed April 2020).
World Health Organisation. Global action plan on antimicrobial resistance. 2015. Available at https://apps.who.int/iris/bitstream/handle/10665/193736/9789241509763_eng.pdf (accessed April 2020).
Fitzpatrick F, Tarrant C, Hamilton V, Kiernan F M, Jenkins D, Krockow E M. Sepsis and antimicrobial stewardship: two sides of the same coin. BMJ Qual Saf 2019; 28: 758-761.
National Institute for Health and Care Excellence. Antimicrobial stewardship: systems and processes for effective antimicrobial medicine use. 2015. Available at https://www.nice.org.uk/guidance/NG15/chapter/recommendations#antimicrobial-stewardship (accessed May 2020).
UK Government. Antimicrobial resistance: UK launches 5-year action plan and 20-year vision. 2019. Available at https://www.gov.uk/government/news/antimicrobial-resistance-uk-launches-5-year-action-plan-and-20-year-vision (accessed April 2020).
Thompson W, Pavitt S, Sandoe J, McEachan R, Douglas G. Antimicrobial stewardship in dentistry: an arts-based approach to intervention development. Lancet 2019; 394: S10.
Sturrock A, Landes D, Robson T, Bird L, Ojelabi A, Ling J. An audit of antimicrobial prescribing by dental practitioners in the north east of England and Cumbria. BMC Oral Health 2018; 18: 206.
Cope A L, Wood F, Francis N A, Chestnutt I G. General dental practitioners' perceptions of antimicrobial use and resistance: a qualitative interview study. Br Dent J 2014; 217: E9.
Stein K, Farmer J, Singhal S, Marra F, Sutherland S, Quinonez C. The use and misuse of antibiotics in dentistry: A scoping review. J Am Dent Assoc 2018; 149: 869-884.e5.
Bunce J T, Hellyer P. Antibiotic resistance and antibiotic prescribing by dentists in England 2007-2016. Br Dent J 2018; 225: 81.
Jones E, Cope A. Knowledge and attitudes of recently qualified dentists working in Wales towards antimicrobial prescribing and resistance. Eur J Dent Educ 2018; DOI: 10.1111/eje.12387.
Public Health England. English Surveillance Programme for Antimicrobial Utilisation and Resistance (ESPAUR). 2019. Available at https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/936199/ESPAUR_Report_2019-20.pdf (accessed August 2020).
Pradipta I S, Sodik D C, Lestari K et al. Antibiotic resistance in sepsis patients: evaluation and recommendation of antibiotic use. N Am J Med Sci 2013; 5: 344-352.
Prestinaci F, Pezzotti P, Pantosti A. Antimicrobial resistance: a global multifaceted phenomenon. Pathog Glob Health 2015; 109: 309-318.
Acknowledgements
We wish to extend our sincere appreciations to the UK Sepsis Trust for their support in writing this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
None declared
Rights and permissions
About this article
Cite this article
Dave, M., Barry, S., Coulthard, P. et al. An evaluation of sepsis in dentistry. Br Dent J 230, 351–357 (2021). https://doi.org/10.1038/s41415-021-2724-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41415-021-2724-6