Abstract
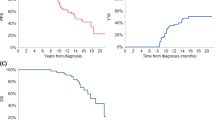
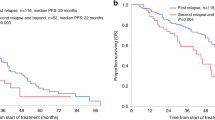
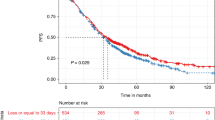
The effectiveness of early treatment for biochemical relapse of multiple myeloma (MM) is unclear. To clarify this issue, this retrospective study was performed to evaluate the survival outcomes of 315 patients with relapsed MM after upfront autologous stem cell transplantation (ASCT). Over a median follow-up of 66.6 months (range, 15.1–195.5 months), 48.2% of patients showed biochemical relapse, 41.3% showed clinical relapse, and 10.5% showed significant biochemical relapse. Progression-free survival (PFS) and overall survival (OS) were inferior for patients with clinical relapse compared to the other patients. Multivariate analysis showed that clinical relapse was an independent prognostic factor for OS. In patients with biochemical relapse, there was no significant difference in survival between patients treated while asymptomatic and those treated once clinical symptoms had appeared. Relapse type after upfront ASCT was a significant prognostic factor in patients with MM. In addition, no survival benefit of early treatment at biochemical relapse was observed, but a triplet regimen may be beneficial for MM patients with biochemical relapse.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The dataset is available from the corresponding author upon reasonable request (the fighshare doi- https://figshare.com/s/cf4a0697a07156ffea9b).
References
Kyle RA, Rajkumar SV. Multiple myeloma. N Engl J Med. 2004;351:1860–1873.
Cavo M, Gay F, Beksac M, Pantani L, Petrucci MT, Dimopoulos MA, et al. Autologous haematopoietic stem-cell transplantation versus bortezomib-melphalan-prednisone, with or without bortezomib-lenalidomide-dexamethasone consolidation therapy, and lenalidomide maintenance for newly diagnosed multiple myeloma (EMN02/HO95): a multicentre, randomised, open-label, phase 3 study. Lancet Haematol. 2020;7:e456–e468.
Zamarin D, Giralt S, Landau H, Lendvai N, Lesokhin A, Chung D, et al. Patterns of relapse and progression in multiple myeloma patients after auto-SCT: implications for patients’ monitoring after transplantation. Bone Marrow Transpl. 2013;48:419–424.
Laubach J, Garderet L, Mahindra A, Gahrton G, Caers J, Sezer O, et al. Management of relapsed multiple myeloma: recommendations of the International Myeloma Working Group. Leukemia. 2016;30:1005–1017.
Kumar SK, Rajkumar SV, Dispenzieri A, Lacy MQ, Hayman SR, Buadi FK, et al. Improved survival in multiple myeloma and the impact of novel therapies. Blood. 2008;111:2516–2520.
Kumar SK, Dispenzieri A, Lacy MQ, Gertz MA, Buadi FK, Pandey S, et al. Continued improvement in survival in multiple myeloma: changes in early mortality and outcomes in older patients. Leukemia. 2014;28:1122–1128.
Palumbo A, Rajkumar SV, San Miguel JF, Larocca A, Niesvizky R, Morgan G, et al. International Myeloma Working Group consensus statement for the management, treatment, and supportive care of patients with myeloma not eligible for standard autologous stem-cell transplantation. J Clin Oncol. 2014;32:587–600.
Fernández de Larrea C, Jiménez R, Rosiñol L, Giné E, Tovar N, Cibeira MT, et al. Pattern of relapse and progression after autologous SCT as upfront treatment for multiple myeloma. Bone Marrow Transpl. 2014;49:223–227.
Chim CS, Kumar SK, Orlowski RZ, Cook G, Richardson PG, Gertz MA, et al. Management of relapsed and refractory multiple myeloma: novel agents, antibodies, immunotherapies and beyond. Leukemia. 2018;32:252–262.
Turesson I, Velez R, Kristinsson SY, Landgren O. Patterns of improved survival in patients with multiple myeloma in the twenty-first century: a population-based study. J Clin Oncol. 2010;28:830–834.
Pulte D, Jansen L, Castro FA, Emrich K, Katalinic A, Holleczek B, et al. Trends in survival of multiple myeloma patients in Germany and the United States in the first decade of the 21st century. Br J Haematol. 2015;171:189–196.
Katodritou E, Kyrtsonis MC, Delimpasi S, Kyriakou D, Symeonidis A, Spanoudakis E, et al. Real-world data on Len/Dex combination at second-line therapy of multiple myeloma: treatment at biochemical relapse is a significant prognostic factor for progression-free survival. Ann Hematol. 2018;97:1671–1682.
Mina R, Belotti A, Petrucci MT, Zambello R, Capra A, Di Lullo G, et al. Bortezomib-dexamethasone as maintenance therapy or early retreatment at biochemical relapse versus observation in relapsed/refractory multiple myeloma patients: a randomized phase II study. Blood Cancer J. 2020;10:58.
Sun Z, Zheng F, Wu S, Liu Y, Guo H, Liu Y. Triplet versus doublet combination regimens for the treatment of relapsed or refractory multiple myeloma: A meta-analysis of phase III randomized controlled trials. Crit Rev Oncol Hematol. 2017;113:249–255.
Dimopoulos MA, Moreau P, Terpos E, Mateos MV, Zweegman S, Cook G, et al. Multiple myeloma: EHA-ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up(†). Ann Oncol. 2021;32:309–322.
Moreau P, Kumar SK, San Miguel J, Davies F, Zamagni E, Bahlis N, et al. Treatment of relapsed and refractory multiple myeloma: recommendations from the International Myeloma Working Group. Lancet Oncol. 2021;22:e105–e118.
Author information
Authors and Affiliations
Contributions
KK and JJL designed the study; SHJ prepared the manuscript; CKM, JHL, YCM, SMB, DHY, and HSL critically reviewed the manuscript. All authors have read and approved the final manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval and consent to participate
This study was approved by the institutional ethics committee of each participating institution and conducted in accordance with the Declaration of Helsinki. The committee waived the need for informed patient consent because of the retrospective nature of the study.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Jung, SH., Min, CK., Lee, J.H. et al. Optimal timing of treatment at relapse after autologous stem cell transplantation in patients with multiple myeloma: a study of the Korean Multiple Myeloma Working Party (KMM-1909). Bone Marrow Transplant 57, 1797–1802 (2022). https://doi.org/10.1038/s41409-022-01818-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41409-022-01818-z