Abstract
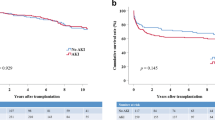
Posterior reversible encephalopathy syndrome (PRES) is a gradually recognised neurological complication of allogenic haematopoietic stem cell transplantation (allo-HSCT). However, there is a paucity of information on PRES after haploidentical HSCT (haplo-HSCT). We performed a retrospective nested case-control study in patients following haplo-HSCT for malignant and nonmalignant haematologic diseases between January 2009 and December 2018 in our centre. A total of 45 patients were diagnosed with PRES after transplant, accounting for an incidence of 1.17%. Grades II to IV acute graft-versus-host disease (aGVHD) (HR 2.370, 95% CI 1.277–4.397, p = 0.006) and hypertension (HR 14.466, 95% CI 7.107–29.443, p < 0.001) were identified as risk factors for developing PRES after haplo-HSCT. There was no difference in overall survival (OS), disease-free survival (DFS), the cumulative incidence of relapse or nonrelapse mortality (NRM) between patients with PRES and controls without PRES following haplo-HSCT in either adults or children. All but one patient with PRES showed nearly complete clinical and neurologic recovery. In conclusion, PRES is a rare condition with benign outcomes following haplo-HSCT. Further multicentre prospective studies are needed to confirm the results and help to establish the standard therapy for posttransplant PRES.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Hinchey J, Chaves C, Appignani B, Breen J, Pao L, Wang A, et al. A reversible posterior leukoencephalopathy syndrome. N Engl J Med. 1996;334:494–500.
Cordelli DM, Masetti R, Zama D, Gueraldi D, Rondelli R, Cottone C, et al. Etiology, characteristics and outcome of seizures after pediatric hematopoietic stem cell transplantation. Seizure. 2014;23:140–5. https://doi.org/10.1016/j.seizure.2013.11.003.
Gaziev J, Marziali S, Paciaroni K, Isgrò A, Di Giuliano F, Rossi G, et al. Posterior reversible encephalopathy syndrome after hematopoietic cell transplantation in children with hemoglobinopathies. Biol Blood Marrow Transpl. 2017;23:1531–40. https://doi.org/10.1016/j.bbmt.2017.05.033.
Chaudhary RK, Dhakal P, Aryal A, Bhatt VR. Central nervous system complications after allogeneic hematopoietic stem cell transplantation. Future Oncol. 2017;13:2297–312. https://doi.org/10.2217/fon-2017-0274.
Hammerstrom AE, Howell J, Gulbis A, Rondon G, Champlin RE, Popat U. Tacrolimus-associated posterior reversible encephalopathy syndrome in hematopoietic allogeneic stem cell transplantation. Am J Hematol. 2013;88:301–5. https://doi.org/10.1002/ajh.23402.
Zama D, Masetti R, Cordelli DM, Vendemini F, Giordano L, Milito G, et al. Risk factor analysis of posterior reversible encephalopathy syndrome after allogeneic hematopoietic SCT in children. Bone Marrow Transpl. 2014;49:1538–40. https://doi.org/10.1038/bmt.2014.182.
Tavares M, Arantes M, Chacim S, Júnior AC, Pinto A, Mariz JM, et al. Posterior reversible encephalopathy syndrome in children with hematologic malignancies. J Child Neurol. 2015;30:1669–75. https://doi.org/10.1177/0883073815578525.
Siegal D, Keller A, Xu W, Bhuta S, Kim DH, Kuruvilla J, et al. Central nervous system complications after allogeneic hematopoietic stem cell transplantation: incidence, manifestations, and clinical significance. Biol Blood Marrow Transpl. 2007;13:1369–79.
Lv M, Chang Y-J, Huang X-J. Update of the “Beijing Protocol” haplo-identical hematopoietic stem cell transplantation. Bone Marrow Transpl. 2019;54(Suppl 2):703–7. https://doi.org/10.1038/s41409-019-0605-2.
Huang X-j, Han W, Xu L-p, Chen Y-h, Liu D-h, Lu J, et al. A novel approach to human leukocyte antigen-mismatched transplantation in patients with malignant hematological disease. Chin Med J. 2004;117:1778–85.
Wang Y, Liu Q-F, Xu L-P, Liu K-Y, Zhang X-H, Ma X, et al. Haploidentical vs identical-sibling transplant for AML in remission: a multicenter, prospective study. Blood. 2015;125:3956–62. https://doi.org/10.1182/blood-2015-02-627786.
Wang Y, Liu Q-F, Xu L-P, Liu K-Y, Zhang X-H, Ma X, et al. Haploidentical versus matched-sibling transplant in adults with philadelphia-negative high-risk acute lymphoblastic leukemia: a biologically phase III randomized study. Clin Cancer Res. 2016;22:3467–76. https://doi.org/10.1158/1078-0432.CCR-15-2335.
Wang Y, Wang HX, Lai YR, Sun ZM, Wu DP, Jiang M, et al. Haploidentical transplant for myelodysplastic syndrome: registry-based comparison with identical sibling transplant. Leukemia. 2016;30:2055–63. https://doi.org/10.1038/leu.2016.110.
Xu L-P, Jin S, Wang S-Q, Xia L-H, Bai H, Gao S-J, et al. Upfront haploidentical transplant for acquired severe aplastic anemia: registry-based comparison with matched related transplant. J Hematol Oncol. 2017;10:25 https://doi.org/10.1186/s13045-017-0398-y.
Lu D-P, Dong L, Wu T, Huang X-J, Zhang M-J, Han W, et al. Conditioning including antithymocyte globulin followed by unmanipulated HLA-mismatched/haploidentical blood and marrow transplantation can achieve comparable outcomes with HLA-identical sibling transplantation. Blood. 2006;107:3065–73.
Lowenstein DH, Alldredge BK. Status epilepticus. N Engl J Med. 1998;338:970–6.
Zama D, Gasperini P, Berger M, Petris M, De Pasquale MD, Cesaro S, et al. A survey on hematology-oncology pediatric AIEOP centres: the challenge of posterior reversible encephalopathy syndrome. Eur J Haematol. 2018;100:75–82. https://doi.org/10.1111/ejh.12984.
Zhang X-H, Zhang J-M, Han W, Chen H, Chen Y-H, Wang F-R, et al. Viral encephalitis after haplo-identical hematopoietic stem cell transplantation: causative viral spectrum, characteristics, and risk factors. Eur J Haematol. 2017;98:450–8. https://doi.org/10.1111/ejh.12855.
Loscalzo J. Endothelial injury, vasoconstriction, and its prevention. Tex Heart Inst J. 1995;22:180–4.
Sandoo A, van Zanten JJCSV, Metsios GS, et al. The endothelium and its role in regulating vascular tone. Open Cardiovasc Med J. 2010;4:302–12. https://doi.org/10.2174/1874192401004010302.
Bartynski WS. Posterior reversible encephalopathy syndrome, part 2: controversies surrounding pathophysiology of vasogenic edema. Am J Neuroradiol. 2008;29:1043–9. https://doi.org/10.3174/ajnr.A0929.
Bartynski WS, Boardman JF. Distinct imaging patterns and lesion distribution in posterior reversible encephalopathy syndrome. Am J Neuroradiol. 2007;28:1320–7.
Reddy P, Ferrara JLM. Immunobiology of acute graft-versus-host disease. Blood Rev. 2003;17:187–94.
Wong R, Beguelin GZ, de Lima M, Giralt SA, Hosing C, Ippoliti C, et al. Tacrolimus-associated posterior reversible encephalopathy syndrome after allogeneic haematopoietic stem cell transplantation. Br J Haematol. 2003;122:128–34.
Erer B, Polchi P, Lucarelli G, Angelucci E, Baronciani D, Galimberti M, et al. CsA-associated neurotoxicity and ineffective prophylaxis with clonazepam in patients transplanted for thalassemia major: analysis of risk factors. Bone Marrow Transpl. 1996;18:157–62.
Tam CS, Galanos J, Seymour JF, Pitman AG, Stark RJ, Prince HM. Reversible posterior leukoencephalopathy syndrome complicating cytotoxic chemotherapy for hematologic malignancies. Am J Hematol. 2004;77:72–6.
Wu Q, Marescaux C, Wolff V, Jeung M-Y, Kessler R, Lauer V, et al. Tacrolimus-associated posterior reversible encephalopathy syndrome after solid organ transplantation. Eur Neurol. 2010;64:169–77. https://doi.org/10.1159/000319032.
Misawa A, Takeuchi Y, Hibi S, Todo S, Imashuku S, Sawada T. FK506-induced intractable leukoencephalopathy following allogeneic bone marrow transplantation. Bone Marrow Transpl×. 2000;25:331–4.
Kanekiyo T, Hara J, Matsuda-Hashii Y, Fujisaki H, Tokimasa S, Sawada A, et al. Tacrolimus-related encephalopathy following allogeneic stem cell transplantation in children. Int J Hematol. 2005;81:264–8.
Acknowledgements
The work was supported by the Beijing Municipal Science and Technology Commission (No. Z171100001017084), the Beijing Natural Science Foundation (H2018206423), the Key Program of the National Natural Science Foundation of China (No. 81730004), the Foundation for Innovative Research Groups of the National Natural Science Foundation of China (81621001), the Beijing Natural Science Foundation (No. 7171013), National Natural Science Foundation of China (No. 81670116) and the National Key Research and Development Program of China (No. 2017YFA0105500, No. 2017YFA0105503).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chen, Q., Zhao, X., Fu, HX. et al. Posterior reversible encephalopathy syndrome (PRES) after haploidentical haematopoietic stem cell transplantation: incidence, risk factors and outcomes. Bone Marrow Transplant 55, 2035–2042 (2020). https://doi.org/10.1038/s41409-020-0894-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41409-020-0894-5
This article is cited by
-
Posterior Reversible Encephalopathy Syndrome
Current Pain and Headache Reports (2021)