Abstract
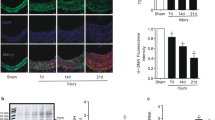
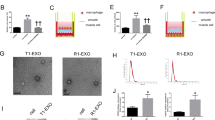
The proliferation and migration of vascular smooth muscle cells (VSMCs) after vascular injury lead to neointimal hyperplasia, thus aggravating vascular diseases. However, the molecular mechanisms underlying neointima formation are not fully elucidated. Extracellular vesicles (EVs) are mediators of various intercellular communications. The potential of EVs as regulators in cardiovascular diseases has raised significant interest. In the current study we investigated the role of circulating small extracellular vesicles (csEVs), the most abundant EVs (1010 EVs/mL serum) in VSMC functions. csEVs were prepared from bovine, porcine or rat serum. We showed that incubation with csEVs (0.5 × 1010−2 × 1010) dose-dependently enhanced the proliferation and migration of VSMCs via the membrane phosphatidylserine (PS). In rats with ligation of right carotid artery, we demonstrated that application of csEVs in the ligated vessels aggravated neointima formation via interaction of membrane PS with injury. Furthermore, incubation with csEVs markedly enhanced the phosphorylation of AXL and MerTK in VSMCs. Pretreatment with BSM777607 (pan-TAM inhibitor), bemcentinib (AXL inhibitor) or UNC2250 (MerTK inhibitor) blocked csEV-induced proliferation and migration of VSMCs. We revealed that csEV-activated AXL and MerTK shared the downstream signaling pathways of Akt, extracellular signal-regulated kinase (ERK) and focal adhesion kinase (FAK) that mediated the effects of csEVs. We also found that csEVs increased the expression of AXL through activation of transcription factor YAP, which might constitute an AXL-positive feedback loop to amplify the signals. Finally, we demonstrated that dual inhibition of AXL/MerTK by ONO-7475 (0.1 µM) effectively hindered csEV-mediated proliferation and migration of VSMCs in ex vivo mouse aorta injury model. Based on these results, we propose an essential role for csEVs in proliferation and migration of VSMCs and highlight the feasibility of dual AXL/MerTK inhibitors in the treatment of vascular diseases.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout










Similar content being viewed by others
Data availability
Supplementary information is available at the website of Acta Pharmacologica Sinica.
References
Iqbal J, Gunn J, Serruys PW. Coronary stents: historical development, current status and future directions. Br Med Bull. 2013;106:193–211.
Ross R. The pathogenesis of atherosclerosis: a perspective for the 1990s. Nature. 1993;362:801–9.
Shi N, Chen SY. Smooth muscle cell differentiation: model systems, regulatory mechanisms, and vascular diseases. J Cell Physiol. 2016;231:777–87.
Rzucidlo EM, Martin KA, Powell RJ. Regulation of vascular smooth muscle cell differentiation. J Vasc Surg. 2007;45:A25–A32.
Bennett MR, Sinha S, Owens GK. Vascular smooth muscle cells in atherosclerosis. Circ Res. 2016;118:692–702.
Nishida-Aoki N, Tominaga N, Takeshita F, Sonoda H, Yoshioka Y, Ochiya T. Disruption of circulating extracellular vesicles as a novel therapeutic strategy against cancer metastasis. Mol Ther. 2017;25:181–91.
Jansen F, Nickenig G, Werner N. Extracellular vesicles in cardiovascular disease: potential applications in diagnosis, prognosis, and epidemiology. Circ Res. 2017;120:1649–57.
Raposo G, Stoorvogel W. Extracellular vesicles: exosomes, microvesicles, and friends. J Cell Biol. 2013;200:373–83.
Wang Z, Zhu H, Shi H, Zhao H, Gao R, Weng X, et al. Exosomes derived from M1 macrophages aggravate neointimal hyperplasia following carotid artery injuries in mice through miR-222/CDKN1B/CDKN1C pathway. Cell Death Dis. 2019;10:422.
Vajen T, Benedikter BJ, Heinzmann ACA, Vasina EM, Henskens Y, Parsons M, et al. Platelet extracellular vesicles induce a pro-inflammatory smooth muscle cell phenotype. J Extracell Vesicles. 2017;6:1322454.
Sorrentino TA, Duong P, Bouchareychas L, Chen M, Chung A, Schaller MS, et al. Circulating exosomes from patients with peripheral artery disease influence vascular cell migration and contain distinct microRNA cargo. JVS Vasc Sci. 2020;1:28–41.
Johnsen KB, Gudbergsson JM, Andresen TL, Simonsen JB. What is the blood concentration of extracellular vesicles? Implications for the use of extracellular vesicles as blood-borne biomarkers of cancer. Biochim Biophys Acta Rev Cancer. 2019;1871:109–16.
Wang Y, Xie Y, Zhang A, Wang M, Fang Z, Zhang J. Exosomes: an emerging factor in atherosclerosis. Biomed Pharmacother. 2019;115:108951.
Park M, Kim JW, Kim KM, Kang S, Kim W, Kim JK, et al. Circulating small extracellular vesicles activate TYRO3 to drive cancer metastasis and chemoresistance. Cancer Res. 2021;81:3539.
Linger RMA, Keating AK, Earp HS, Graham DK. TAM receptor tyrosine kinases: biologic functions, signaling, and potential therapeutic targeting in human cancer. Adv Cancer Res. 2008;100:35–83.
Melaragno MG, Fridell YWC, Berk BC. The Gas6/Axl system: a novel regulator of vascular cell function. Trends Cardiovasc Med. 1999;9:250–3.
Skotland T, Hessvik NP, Sandvig K, Llorente A. Exosomal lipid composition and the role of ether lipids and phosphoinositides in exosome biology. J Lipid Res. 2019;60:9–18.
Yan X, Doffek K, Yin C, Krein M, Phillips M, Sugg SL, et al. Annexin-V promotes anti-tumor immunity and inhibits neuroblastoma growth in vivo. Cancer Immunol Immunother. 2012;61:1917–27.
Krahling S, Callahan MK, Williamson P, Schlegel RA. Exposure of phosphatidylserine is a general feature in the phagocytosis of apoptotic lymphocytes by macrophages. Cell Death Differ. 1999;6:183–9.
Nakano T, Higashino K, Kikuchi N, Kishino J, Nomura K, Fujita H, et al. Vascular smooth muscle cell-derived, Gla-containing growth-potentiating factor for Ca2+-mobilizing growth factors. J Biol Chem. 1995;270:5702–5.
Kasikara C, Kumar S, Kimani S, Tsou W-I, Geng K, Davra V, et al. Phosphatidylserine sensing by TAM receptors regulates AKT-dependent chemoresistance and PD-L1 expression. Mol Cancer Res. 2017;15:753.
Goruppi S, Ruaro E, Varnum B, Schneider C. Requirement of phosphatidylinositol 3-kinase-dependent pathway and Src for Gas6-Axl mitogenic and survival activities in NIH 3T3 fibroblasts. Mol Cell Biol. 1997;17:4442–53.
Hu Y-L, Lu S, Szeto KW, Sun J, Wang Y, Lasheras JC, et al. FAK and paxillin dynamics at focal adhesions in the protrusions of migrating cells. Sci Rep. 2014;4:6024.
Linger RM, Cohen RA, Cummings CT, Sather S, Migdall-Wilson J, Middleton DH, et al. Mer or Axl receptor tyrosine kinase inhibition promotes apoptosis, blocks growth and enhances chemosensitivity of human non-small cell lung cancer. Oncogene. 2013;32:3420–31.
Ghiso E, Migliore C, Ciciriello V, Morando E, Petrelli A, Corso S, et al. YAP-dependent AXL overexpression mediates resistance to EGFR inhibitors in NSCLC. Neoplasia. 2017;19:1012–21.
Mudduluru G, Leupold JH, Stroebel P, Allgayer H. PMA up‐regulates the transcription of Axl by AP‐1 transcription factor binding to TRE sequences via the MAPK cascade in leukaemia cells. Biol Cell. 2011;103:21–33.
Lachowski D, Cortes E, Robinson B, Rice A, Rombouts K, Del Rio Hernandez AE. FAK controls the mechanical activation of YAP, a transcriptional regulator required for durotaxis. FASEB J. 2018;32:1099–107.
Song X, Xu H, Wang P, Wang J, Affo S, Wang H, et al. Focal adhesion kinase (FAK) promotes cholangiocarcinoma development and progression via YAP activation. J Hepatol. 2021;75:888–99.
Lu Q, Lemke G. Homeostatic regulation of the immune system by receptor tyrosine kinases of the Tyro 3 family. Science. 2001;293:306–11.
Ye F, Li Q, Ke Y, Lu Q, Han L, Kaplan HJ, et al. TAM receptor knockout mice are susceptible to retinal autoimmune induction. Invest Ophthalmol Vis Sci. 2011;52:4239–46.
Togliatto G, Dentelli P, Rosso A, Lombardo G, Gili M, Gallo S, et al. PDGF-BB carried by endothelial cell–derived extracellular vesicles reduces vascular smooth muscle cell apoptosis in diabetes. Diabetes. 2018;67:704.
Otani K, Yokoya M, Fujioka Y, Okada M, Yamawaki H. Small extracellular vesicles from rat plasma promote migration and proliferation of vascular smooth muscle cells. J Vet Med Sci. 2020;82:299–306.
McShane L, Tabas I, Lemke G, Kurowska-Stolarska M, Maffia P. TAM receptors in cardiovascular disease. Cardiovasc Res. 2019;115:1286–95.
Jin CW, Wang H, Chen YQ, Tang MX, Fan GQ, Wang ZH, et al. Gas6 delays senescence in vascular smooth muscle cells through the PI3K/ Akt/FoxO signaling pathway. Cell Physiol Biochem. 2015;35:1151–66.
Korshunov Vyacheslav A. Axl-dependent signalling: a clinical update. Clin Sci. 2012;122:361.
Dagamajalu S, Rex DAB, Palollathil A, Shetty R, Bhat G, Cheung LWT, et al. A pathway map of AXL receptor-mediated signaling network. J Cell Commun Signal. 2021;15:143–8.
Cummings CT, DeRyckere D, Earp HS, Graham DK. Molecular pathways: MERTK signaling in cancer. Clin Cancer Res. 2013;19:5275.
Louis SF, Zahradka P. Vascular smooth muscle cell motility: from migration to invasion. Exp Clin Cardiol. 2010;15:e75–e85.
Jeong K, Kim J-H, Murphy JM, Park H, Kim S-J, Rodriguez YA, et al. Nuclear focal adhesion kinase controls vascular smooth muscle cell proliferation and neointimal hyperplasia through GATA4-mediated cyclin D1 transcription. Circ Res. 2019;125:152–66.
Melaragno MG, Wuthrich DA, Poppa V, Gill D, Lindner V, Berk BC, et al. Increased expression of Axl tyrosine kinase after vascular injury and regulation by G protein–coupled receptor agonists in rats. Circ Res. 1998;83:697–704.
Saab S, Chang OS, Nagaoka K, Hung MC, Yamaguchi H. The potential role of YAP in Axl-mediated resistance to EGFR tyrosine kinase inhibitors. Am J Cancer Res. 2019;9:2719–29.
Kimura TE, Duggirala A, Smith MC, White S, Sala-Newby GB, Newby AC, et al. The Hippo pathway mediates inhibition of vascular smooth muscle cell proliferation by cAMP. J Mol Cell Cardiol. 2016;90:1–10.
Acknowledgements
This research was funded by the National Research Foundation of Korea (NRF) grants funded by the Korean Government; 2021R1A4A1021787 and 2022M3A9B6017654. Graphical representation was created with ©biorender.com.
Author information
Authors and Affiliations
Contributions
YJL: conceptualization, investigation, validation, writing - original draft. MP: writing - review and editing. HYK: writing - review and editing. JKK: resources. WKK: methodology. SCL: methodology. KWK: conceptualization, writing - review and editing, funding acquisition, supervision.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lee, Y.J., Park, M., Kim, H.Y. et al. Circulating small extracellular vesicles promote proliferation and migration of vascular smooth muscle cells via AXL and MerTK activation. Acta Pharmacol Sin 44, 984–998 (2023). https://doi.org/10.1038/s41401-022-01029-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41401-022-01029-8