Abstract
Serious concerns have been raised about the negative effects of the COVID-19 pandemic on population psychological well-being. However, limited data exist on the long-term effects of the pandemic on incident psychiatric morbidities among individuals with varying exposure to the pandemic. Leveraging prospective data from the community-based UK Biobank cohort, we included 308,400 participants free of diagnosis of anxiety or depression, as well as 213,757 participants free of anxiolytics or antidepressants prescriptions, to explore the trends in incident diagnoses and drug prescriptions for anxiety and depression from 16 March 2020 to 31 August 2021, compared to the pre-pandemic period (i.e., 1 January 2017 to 31 December 2019) and across populations with different exposure statuses (i.e., not tested for COVID-19, tested negative and tested positive). The age- and sex-standardized incidence ratios (SIRs) were calculated by month which indicated an increase in incident diagnoses of anxiety or depression among individuals who were tested for COVID-19 (tested negative: SIR 3.05 [95% confidence interval 2.88–3.22]; tested positive: 2.03 [1.76–2.34]), especially during the first six months of the pandemic (i.e., March-September 2020). Similar increases were also observed for incident prescriptions of anxiolytics or antidepressants (tested negative: 1.56 [1.47–1.67]; tested positive: 1.41 [1.22–1.62]). In contrast, individuals not tested for COVID-19 had consistently lower incidence rates of both diagnoses of anxiety or depression (0.70 [0.67–0.72]) and prescriptions of respective psychotropic medications (0.70 [0.68–0.72]) during the pandemic period. These data suggest a distinct rise in health care needs for anxiety and depression among individuals tested for COVID-19, regardless of the test result, in contrast to a reduction in health care consumption for these disorders among individuals not tested for and, presumably, not directly exposed to the disease.
Similar content being viewed by others
Introduction
The coronavirus disease (COVID-19) pandemic continues to be a world-wide public health threat [1, 2]. Serious concerns have been raised about the negative effects of the pandemic on population psychological well-being, including new-onset psychiatric symptoms and disorders in people without preexisting problems [3, 4]. Indeed, a Canadian online survey reported that the proportion of generalized anxiety disorder and depression increased by 12% and 29%, respectively, during the pandemic [4]. Based on representative primary care data, Jacob et al. also found an increase in the number of patients newly diagnosed with anxiety disorder between March and June 2020 in Germany [5]. However, a significant reduction in first diagnoses of depression and anxiety between March and September 2020 was observed in UK, especially for adults of working age [6]. Likewise, psychiatric emergency consultations were also dramatically decreased across all psychiatric disorders during the lockdown (i.e., March-April 2020) in Paris and suburbs [7]. In terms of dispensing rate for antidepressants, a study in Canada showed a temporary reduction in April 2020 which then returned to the pre-pandemic levels by August 2020 [8].
Notably, previous studies have also suggested varying effects of the pandemic on population mental health across time [9] and degree of pandemic exposure [10,11,12]. For example, several countries have reported fluctuating levels of anxiety and depression across and between the different pandemic “waves” (i.e., according to numbers of COVID-19 cases, hospitalizations, and deaths) [13]. Based on cross-sectional data collected at the beginning of the pandemic, a study in China reported that clinical symptoms of anxiety and depression was predominately increased among patients with COVID-19 infection, compared to individuals under quarantine or the general public [11]. In the UK, Abel et al. observed an increased risk of fatigue, sleep problems, and psychotropic medication use among patients with negative COVID-19 test result, in contrast to matched controls in the general population [12]. Altogether, those findings indicated that patients who sought or received COVID-19 test may, irrespective of the test results, be at a higher exposure level of the pandemic (i.e., close to infected individuals or experiencing COVID-19 like symptoms) and thereby suffer a higher psychological burden.
Yet, limited data exist on the long-term effects of the pandemic on incident psychiatric disorders among individuals with varying exposure to the pandemic (e.g., COVID diagnosis), with careful control of potential confounding including seasonal effects. To this end, we leveraged routinely collected administrative data from the UK Biobank to assess trends in incident diagnoses of common psychiatric disorders – anxiety and depression – and prescriptions of respective psychotropic medications (i.e., anxiolytics and antidepressants) during the first 18 months of the pandemic, by history of COVID-19 testing (not tested, tested negative, and tested positive) as an indicator of pandemic exposure.
Methods
Study population and design
The UK Biobank is a population-based cohort study that recruited 502,507 men and women aged 40–69 years from England, Scotland, and Wales between 2006 and 2010, accounting for 5.5% of the UK population. Health-related outcomes of the participants are obtained regularly through linkage to multiple datasets [14]. Specifically, hospital inpatient data are obtained from Hospital Episode Statistics (HES) for England, Scottish Morbidity Record for Scotland, and Patient Episode Database for Wales. Mortality data are obtained from National Health Service (NHS) Digital and NHS Central Register. The hospital inpatient data (available since 1997) and mortality data (available since 2006) in England are currently updated to 30 September 2021. Furthermore, to facilitate COVID-19 related research, the UK Biobank also provided records of COVID-19 test results (by RT-PCR of nose/throat swab samples, available from 16 March 2020 to 30 September 2021) through linkage to Public Health England (PHE) [15], as well as updated primary care data obtained from two major general practice (GP) data system suppliers (EMIS and TPP) for approximately 450,000 UK Biobank participants in England (available from 1938 onward to 31 August 2021) [16]. More details about the UK Biobank are described elsewhere [17].
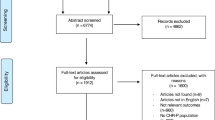
In this study, the outcomes of interest are incident diagnoses of anxiety and depression as well as prescriptions of the respective psychotropic medications during the COVID-19 pandemic. As the World Health Organization (WHO) declared the COVID-19 as a pandemic on 11 March 2020 and given the availability of COVID-19 related data in the UK Biobank, we defined the pandemic exposure period from 16 March 2020 to 31 August 2021. After excluding participants who withdrew from the UK Biobank (n = 94), had no available primary care data (n = 90,715), or died before 16 March 2020 (n = 10,518), we included 401,180 participants registered in England in the study (Fig. 1). Among these participants, we first constructed a cohort for the analysis of incident diagnoses of depression or anxiety, including 308,400 participants who were free of anxiety (International Classification of Diseases, Tenth Revision (ICD-10), F40-F41) and depression (ICD-10, F32-F33), as of 16 March 2020, to examine the trend of incident diagnoses of these psychiatric disorders during the COVID-19 pandemic. Then, to study the trend of incident prescriptions of respective psychotropic medications (i.e., anxiolytics and antidepressants), we constructed another cohort including 213,757 participants who were free of prescription of these medications on 16 March 2020. We followed up those participants from baseline (i.e., 16 March 2020) until the occurrence of any outcomes of interest, death, or the end of followup (i.e., 31 August 2021). In comparison, we used the three preceding years before the pandemic (i.e., from 1 January 2017 to 31 December 2019) as the reference pre-pandemic period. Supplementary Fig. S1 shows the flow chart of the pre-pandemic population selection.
* The primary care data were only available for participants registered in England and registered at a practice using TPP or EMIS as their data system supplier. † Considering the results of COVID-19 tests was available in England through linkage to Public Health England database since 16 March 2020 onwards, thus, we defined the pandemic period start from 16 March 2020.
The UK Biobank collected all data after written informed consent obtained from each participant and the study has full ethical approval from the NHS National Research Ethics Service (16/NW/0274). This present study was also approved by the biomedical research ethics committee of West China Hospital (2020.661).
Ascertainment of anxiety, depression, and psychotropic medications
Diagnoses of anxiety and depression were retrieved from the UK Biobank hospital inpatient data (according to ICD-10 codes) [18] and primary care data (according to SNOMED CT, local EMIS codes, Clinical Terms Version 3, and Local TPP codes) [19]. The diagnoses of psychiatric disorders from HES in England have been validated, indicating a positive predictive value of up to 75% for depression and <60% for anxiety [20]. Prescription of psychotropic medications was ascertained through mapping the UK Biobank prescription codes (i.e., dm+d and local EMIS codes) to their corresponding active ingredients using dm+d XML Transformation Tool and UK Biobank Data-Coding 7678 resource [19]. The active ingredients were then matched to the WHO Atomical Therapeutic Chemical (ATC) classification system [21], and the ingredients (e.g., doxepin, esketamine) with more than one matched ATC codes were discarded as it is difficult to disentangle therapeutic targets. We extracted information (i.e., prescription code and date) about anxiolytics (N05B) and antidepressants (N06A) in the analysis. Supplementary Table S1 provides a list of the active ingredients and their corresponding ATC codes used in this study.
Stratification by history of COVID-19 testing
Accounting for the reported variations in psychological implications of COVID-19 pandemic among populations with different exposure level, we categorized the participants into three pandemic exposure groups, using the history COVID-19 testig as an indicator (i.e., not tested, tested negative, and tested positive). As the testing status could change over time, the categorization was done in a time-varying manner, namely that all participants were in the “not tested” group on 16 March 2020, while those with a record of negative test result in PHE were moved to the “tested negative” group on the date of the corresponding COVID-19 test. Further, individuals not tested or tested negative could move to “tested positive” group on the date of a positive test result as recorded in PHE, or the date of a COVID-19 diagnosis (ICD-10 codes, U07.1 and U07.2) as documented in the UK Biobank inpatient hospital data, if any. Although the UK Biobank population is not representative of the entire UK population, we found largely similar trend in the daily number of COVID-19 cases in the study cohort as that in the whole England (i.e., publicly announced number of cases, Supplementary Fig. S2) [22].
Statistical analysis
We first calculated the crude incidence rates (IRs, dividing the number of outcomes by accumulated person-years at risk) of the incident diagnoses of anxiety or depression as well as prescriptions of psychotropic medications during the pandemic period, respectively. We then calculated the IRs by history of COVID-19 testing (i.e., not tested, tested negative, and tested positive). The comparison between the pandemic and pre-pandemic periods was achieved by applying indirect standardization method to calculate the standardized incidence ratios (SIRs, standardized by age and sex) and their 95% confidence intervals (95%CIs). As psychological well-being may be influenced by seasonal variation, we further calculated the monthly SIRs during the 18-month pandemic period, using the average month-, sex-, and age-specific incidence rate of the studied outcomes from the pre-pandemic period as reference.
Moreover, we performed separate analyses for anxiety and depression as well as for anxiolytics and antidepressants. In addition, to test the robustness of our results to severe somatic conditions, we repeated all analyses after excluding participants with severe somatic diseases (i.e., those included in Charlson comorbidity index calculation, see Supplementary Table S2) on 16 March 2020. We also conducted a sensitivity analysis by re-defining the pandemic period as 18 May 2020 (i.e., when COVID-19 test was available to everyone with symptoms in the UK) [23] to 31 August 2021.
Results
Among the 308,400 participants of the cohort for incident diagnoses of anxiety or depression (mean age = 68.2, 47.9% male) (Table 1), 4 439 received their first diagnosis of anxiety or depression during the pandemic period, corresponding to an IR of 9.7 per 1000 person-years. The IR was 7.5, 33.2, and 21.3 per 1000 person-years for participants who had not been tested, had tested negative, and tested positive for COVID-19, respectively. When compared with the IR of the pre-pandemic period (10.4 per 1000 person-years), we observed a decrease in incident diagnoses of anxiety or depression among participants not tested for COVID-19 (SIR 0.70 [95% CI 0.67–0.72]), but an increase in incident diagnoses of anxiety or depression among participants tested for COVID-19, irrespective of test result (tested negative: 3.05 [2.88–3.22]; tested positive: 2.03 [1.76–2.34]). Among the 213 757 participants included in the cohort of incident prescriptions of psychotropic medications (mean age = 67.9, 52.3% male) (Table 1), we observed largely similar risk patterns. For instance, there was a decrease in incident medication prescriptions among those not tested (0.70 [0.68–0.72]), but an increase in incident medication prescriptions among those tested for COVID-19 (tested negative: 1.56 [1.47–1.67]; tested positive: 1.41 [1.22–1.62]) during the pandemic period, compared with the pre-pandemic period.
The analysis of seasonal variation showed a lower overall risk for incident diagnoses of anxiety or depression during the pandemic period when compared to the pre-pandemic period, except in June 2021 (1.30 [1.17–1.45]) and July 2021 (1.34 [1.20–1.49]) (Fig. 2). We again obtained different results when separately analyzing by history of COVID-19 testing, with an increased incidence rate among individuals tested for COVID-19, especially during the beginning of the pandemic (i.e., March 2020 - September 2020; tested negative: SIRs 3.61–7.05, tested positive: SIRs 2.33–9.38), whereas a decreased incidence rate among those not tested during the entire 18-month period (SIRs 0.55–0.90). Similar results were obtained for incident prescriptions of anxiolytics or antidepressants (Fig. 3). There was an increase in incidence rate of these psychotropic medications during the first six months of the pandemic among individuals tested for COVID-19 (tested negative: SIRs 1.78–3.38; tested positive: SIRs 1.57–6.66), but a constantly lower incidence rates among those not tested for COVID-19 (SIRs 0.64–0.82).
Note, IR incidence rate, SIR standardized incidence ratio. * Three preceding years as the pre-pandemic period (i.e., from 1 January 2017 to 31 December 2019). † The expectation was calculated by multiplying the number of persons by the average month-specific, sex-specific, and age-specific (1-year strata) incidence rate derived from pre-pandemic period. ‡ The standardized incidence ratio was calculated by comparing the number of observed incident cases with the expectation.
Note, IR incidence rate, SIR standardized incidence ratio. * Three preceding years as the pre-pandemic period (i.e., from 1 January 2017 to 31 December 2019). † The expectation was calculated by multiplying the number of persons by the average month-specific, sex-specific, and age-specific (1-year strata) incidence rate derived from pre-pandemic period. ‡ The standardized incidence ratio was calculated by comparing the number of observed incident cases with the expectation.
We observed largely comparable results when analyzing anxiety and depression, as well as anxiolytics and antidepressants, separately (Supplementary Figs. S3 and S4). These findings remained robust after excluding participants with pre-existing severe somatic diseases (Supplementary Figs. S5 and S6) and after re-defining the pandemic period from 18 May 2020 (Supplementary Figs. S7 and S8).
Discussion
In general, the findings of this study based on the UK Biobank indicate that individuals tested for COVID-19, irrespective of the test result, experienced a rise in the incident diagnosis of anxiety and depression as well as respective medication use, particularly at the beginning of the pandemic. In contrast, we observed a decrease in incident diagnoses of anxiety and depression as well as prescriptions of respective psychotropic medications during the pandemic in the general population not tested for COVID-19, yet with an increase beyond pre-pandemic levels in mid 2021.
The finding on lower incidence rates of anxiety and depression as well as prescriptions of psychotropic medications in the general population may reflect a decrease in general psychiatric healthcare utilization during the first 18 months of the pandemic. In line with our findings, a drop in psychiatric emergency visits and hospital admission during the pandemic has previously been reported in other European countries [24, 25]. For instance, in Italy, a 37.5% decrease in the number of psychiatric emergency consultations was observed during the lockdown (March-May 2020) and 17.9% after the lockdown period [26]. Similarly, a retrospective study in Spain suggested that the most marked reduction in admission rates during lockdown (March-June 2020) was observed for anxiety-related disorders [27]. Moreover, addition to the political restriction [23], as SARS-CoV-2 is highly infectious, people may intentionally delay or avoid seeking medical care during the unprecedented period. The findings of Czeisler et al. reported that 12% of US adults delayed or avoided emergency care and 32% avoided routine medical care [28]. Existing evidence about the trends of incident antidepressants and anxiolythics prescriptions during the pandemic is inconsistent. For instance, Antonazzo et al suggested an abrupt reduction of incident antidepressants use during the lockdown in Italy, with a following rebound during the post-lockdown period [29], while a continuing increase in new antidepressant use was observed during the first year of the pandemic in Australia [30]. Furthermore, age-group differences have been noted in the consumption of psychotropic medications, with the most significant increase found in the younger population [30, 31].
The observed decrease in incident diagnoses in the general population appeared to be mainly attributable to individuals not tested for COVID-19. Thus, it is also possible that the decrease in incident diagnoses might reflect lower prevalence of psychiatric morbidity in this population because people might have spent more time with family and friends or had slower pace of daily life during the pandemic [32]. Indeed, the protective effects of family and friends’ support on depressive symptoms and PTSD symptoms are well-documented [33, 34]. Additionally, a recent study from France reported improved sleep in the general population during the pandemic which might positively affect mental health [35]. Regardless, as the effect of pandemic on population mental health is complex and profound, future research focused on both negative and positive aspects of the crisis is needed.
In contrast, the increase in incident psychiatric morbidities among individuals tested for COVID-19 may have several explanations. It is conceivable that people tested for COVID-19 might have been exposed to infected individuals or be symptomatic, and the psychological burden of suspecting to be infected may contribute to the observed increase. Testing for COVID-19 itself and waiting for the test result might also be stressful and associated with increased anxiety [36]. One study showed that more than half of patients suspected to have COVID-19 had increased psychotropic medication prescriptions [37]. Alternatively, individuals who had taken a COVID-19 test might also have temporarily reduced social contact, i.e., being quarantined or isolated, to avoid infecting others, resulting in negative impact on mental health [38]. On the other hand, studies conducted by our [39, 40] and other research groups [41] demonstrated a bidirectional association between COVID-19 and psychiatric disorders, suggesting that individuals with propensity for psychiatric disorders may be more vulnerable for COVID-19 infection and adverse outcomes. With respect to the test result, we observed a similar increased risk of anxiety and depression for individuals with both negative and positive results, which is in agreement with Abel et al.’s finding [12]. Likewise, when compared to tested negative individuals, a Danish registry study found that there was no significant increase in risk for initiation of new antidepressants among tested positive individuals [42]. However, Klaser et al reported that symptoms of anxiety and depression were slightly more prevalent among individuals tested positive compared to those tested negative for COVID-19 [43].
The most notable increase in incident diagnoses of anxiety and depression among COVID-19 tested group was found at the beginning of the pandemic. One reason for the temporary spike at the initial stage of the pandemic is the uncertainty about the virus at that timpoint [44]. Fear of being infected or infecting others may trigger psychological distress. The less or insignificantly elevated incidence rates in later periods of pandemic in this population may be attributed to population adaptation of the COVID-19 crisis [45] and the wide implementation of vaccination in the UK [46], which might have reduced stress or distress. Regardless, as the increased incidence rates persisted nearly the entire 18-month pandemic period, further research with longer follow-up is warranted to understand the continued impact of the pandemic on population mental health.
Study strengths include the use of timely updated UK Biobank primary care and PHE data, which enabled us to explore the long-term psychological consequences among individuals with different history of COVID-19 testing during the pandemic. Moreover, the application of self-comparison analysis, where the rate of incident events during the pandemic period was compared with the corresponding age- and sex-specific rate of the three preceding years in the same study population, inherently allows for the control for potential confounders that are constant over time, including genetic factors and many environmental factors that did not change greatly within the study period. In addition, we carefully considered the impact of seasonal variation through analyzing monthly SIRs.
One major concern of our study is the varying access to COVID-19 testing between groups of the study participants and during different parts of the pandemic period. We therefore performed sensitivity analyses through excluding participants with severe pre-pandemic comorbidities or re-defining pandemic period from 18 May 2020, which suggested some but limited influence of this concern. Also, regardless of test result, it is further possible that some other factors determined the likelihood of taking a COVID-19 test. For example, seeking or receiving a COVID-19 tests may indicate higher level of medical care utilization and therefore increased possibility of being diagnosed or prescribed for existing psychiatric symptoms (i.e., surveillance bias). However, the impact of such a concern, if any, should be constant throughout the whole study period, whilst the change in incident diagnoses and drug prescriptions for anxiety and depression was indeed time-varying, suggesting potential contribution of other causes, such as temporary psychological burden caused by COVID-19-related exposures or reduced social contacts. In addition, considering the overloaded healthcare system during the pandemic period, our outcome identification strategy (using diagnoses and drug prescriptions from both primary care and hospital inpatient data) is likely to only capture patients with more severe psychiatric symptoms. Conditions for individuals with less severe symptoms who did not seek medical care need to be studied in future studies. Likewise, as our identification of COVID-19 cases relies solely on RT-PCR testing (but not self-tests which became available in UK since January 2021 [47]), individuals testing positive for COVID-19 on RT-PCR are more likely represented by those have been symptomatic. Moreover, the sample size of individuals tested positive for COVID-19 was relatively small yielding insufficient precision to depict the monthly variations during the pandemic period, and the absence of data on acute COVID-19 severity prohibit the assessment of trends by varying COVID-19 severity. Also, varying mortality rates in the studied groups and the resulting competing risks may have resulted in an underestimated relative risks of psychiatric outcomes, particularly among individuals with COVID-19 [48]. Furthermore, the UK Biobank primary care data are only available for participants registered at TPP and EMIS system in England, whereas the prescriptions of psychotropic medications cannot be assumed to equal actual consumption of these medications [19]. Finally, the UK Biobank only recruited 5.5% of the UK population, mainly elderly white people, thus, our results cannot necessarily be generalized to the entire UK population or other populations.
Conclusion
In conclusion, the findings of this study suggest differential population mental health care utilization during the COVID-19 pandemic by level of pandemic exposure indicated by history of COVID-19 testing. Compared to the pre-pandemic period, we observed a decrease in incident diagnoses of anxiety and depression as well as prescriptions of respective psychotropic medications among individuals not tested for COVID-19, but an increase in incident psychiatric morbidity among those tested for COVID-19, irrespective of the test result, particularly at the beginning of COVID-19 pandemic.
Data availability
Data from the UK Biobank (http://www.ukbiobank.ac.uk/) are available to all researchers upon making an application.
Code availability
All analyses were performed in R version 4.0. Codes associated with the current submission is available and can be requested by contacting the corresponding author.
References
Wang C, Horby PW, Hayden FG, Gao GF. A novel coronavirus outbreak of global health concern. Lancet. 2020;395:470–3.
Zaninotto P, Iob E, Demakakos P, Steptoe A. Immediate and longer-term changes in the mental health and well-being of older adults in England during the COVID-19 pandemic. JAMA Psychiatry. 2022;79:151–9.
Pfefferbaum B, North CS. Mental health and the Covid-19 pandemic. N Engl J Med. 2020;383:510–2.
Robillard R, Daros AR, Phillips JL, Porteous M, Saad M, Pennestri M-H, et al. Emerging new psychiatric symptoms and the worsening of pre-existing mental disorders during the COVID-19 pandemic: a Canadian Multisite Study: Nouveaux symptômes psychiatriques émergents et détérioration des troubles mentaux préexistants durant la pandémie de la COVID-19: une étude canadienne multisite. Can J Psychiatry Rev Canadienne De Psychiatr. 2021;66:815–26.
Jacob L, Smith L, Koyanagi A, Oh H, Tanislav C, Shin JI, et al. Impact of the coronavirus 2019 (COVID-19) pandemic on anxiety diagnosis in general practices in Germany. J Psychiatr Res. 2021;143:528–33.
Carr MJ, Steeg S, Webb RT, Kapur N, Chew-Graham CA, Abel KM, et al. Effects of the COVID-19 pandemic on primary care-recorded mental illness and self-harm episodes in the UK: a population-based cohort study. Lancet Public Health. 2021;6:e124–e135.
Pignon B, Gourevitch R, Tebeka S, Dubertret C, Cardot H, Dauriac-Le Masson V, et al. Dramatic reduction of psychiatric emergency consultations during lockdown linked to COVID-19 in Paris and suburbs. Psychiatry Clin Neurosci. 2020;74:557–9.
Uthayakumar S, Tadrous M, Vigod SN, Kitchen SA, Gomes T. The effects of COVID‐19 on the dispensing rates of antidepressants and benzodiazepines in Canada. Depression anxiety. 2022;39:156–62.
Wu YY, Walkover M, Zhang W. Trends in psychological distress and COVID-19 incidence across 15 U.S. metropolitan statistical areas in 2020. Soc Sci Med (1982). 2021;285:114285–114285.
Wang M, Zhao Q, Hu C, Wang Y, Cao J, Huang S, et al. Prevalence of psychological disorders in the COVID-19 epidemic in China: a real world cross-sectional study. J Affect Disord. 2021;281:312–20.
Zhang J, Lu H, Zeng H, Zhang S, Du Q, Jiang T, et al. The differential psychological distress of populations affected by the COVID-19 pandemic. Brain Behav Immun. 2020;87:49–50.
Abel KM, Carr MJ, Ashcroft DM, Chalder T, Chew-Graham CA, Hope H, et al. Association of SARS-CoV-2 infection with psychological distress, psychotropic prescribing, fatigue, and sleep problems among UK primary care patients. JAMA Netw Open. 2021;4:e2134803–e2134803.
Hewlett E, Takino S, Nishina Y, Prinz C. Tackling the mental health impact of the COVID-19 crisis: an integrated, whole-of-society response. Organisation for Economic Co-operation and Development (OECD). 2021.
Bycroft C, Freeman C, Petkova D, Band G, Elliott LT, Sharp K, et al. The UK Biobank resource with deep phenotyping and genomic data. Nature. 2018;562:203–9.
Armstrong J, Rudkin JK, Allen N, Crook DW, Wilson DJ, Wyllie DH, et al. Dynamic linkage of COVID-19 test results between Public Health England’s Second Generation Surveillance System and UK Biobank. Microb Genomics. 2020;6:mgen000397.
UK Biobank Data providers and dates of data availability. 2022. https://biobank.ndph.ox.ac.uk/showcase/exinfo.cgi?src=Data_providers_and_dates.
Fry A, Littlejohns TJ, Sudlow C, Doherty N, Adamska L, Sprosen T, et al. Comparison of sociodemographic and health-related characteristics of UK biobank participants with those of the general population. Am J Epidemiol. 2017;186:1026–34.
UK Biobank Hospital inpatient data. 2020. https://www.ukbiobank.ac.uk/.
UK Biobank primary care data for COVID-19 research. 2021. www.ukbiobank.ac.uk.
Davis KA, Sudlow CL, Hotopf M. Can mental health diagnoses in administrative data be used for research? A systematic review of the accuracy of routinely collected diagnoses. BMC Psychiatry. 2016;16:263.
The Anatomical Therapeutic Chemical (ATC) classification system. 2022. https://www.whocc.no/.
Cases in England. 2022. https://coronavirus.data.gov.uk/details/cases?areaType=nation&areaName=England.
COVID-19 policy tracker. 2020. https://www.health.org.uk/news-and-comment/charts-and-infographics/covid-19-policy-tracker.
Hoyer C, Ebert A, Szabo K, Platten M, Meyer-Lindenberg A, Kranaster L. Decreased utilization of mental health emergency service during the COVID-19 pandemic. Eur Arch Psychiatry Clin Neurosci. 2020;271:377–9.
Bonello F, Zammit D, Grech A, Camilleri V, Cremona R. Effect of COVID-19 pandemic on mental health hospital admissions: comparative population-based study. BJPsych Open. 2021;7:e141–e141.
Balestrieri M, Rucci P, Amendola D, Bonizzoni M, Cerveri G, Colli C, et al. Emergency psychiatric consultations during and after the COVID-19 lockdown in Italy. A multicentre study. Front Psychiatry. 2021;12:929.
Gómez-Ramiro M, Fico G, Anmella G, Vázquez M, Sagué-Vilavella M, Hidalgo-Mazzei D, et al. Changing trends in psychiatric emergency service admissions during the COVID-19 outbreak: report from a worldwide epicentre. J Affect Disord. 2021;282:26–32.
Czeisler MÉ, Marynak K, Clarke KE, Salah Z, Shakya I, Thierry JM, et al. Delay or avoidance of medical care because of COVID-19–related concerns—United States, June 2020. Morbidity Mortal Wkly Rep. 2020;69:1250.
Antonazzo IC, Fornari C, Maumus-Robert S, Cei E, Paoletti O, Ferrara P, et al. Antidepressants drug use during COVID-19 waves in the Tuscan general population: an interrupted time-series analysis. J Personalized Med. 2022;12:178.
de Oliveira Costa J, Gillies MB, Schaffer AL, Peiris D, Zoega H, Pearson S-A. Changes in antidepressant use in Australia: a nationwide analysis (2015–2021). Aust N Z J Psychiatry. 2023;57:49–57.
Levaillant M, Wathelet M, Lamer A, Riquin E, Gohier B, Hamel-Broza J-F. Impact of COVID-19 pandemic and lockdowns on the consumption of anxiolytics, hypnotics and antidepressants according to age groups: a French nationwide study. Psychol Med. 2021. https://doi.org/10.1017/S0033291721004839.
Kowalski RM, Carroll H, Britt J. Finding the silver lining in the COVID-19 crisis. J Health Psychol. 2022;27:1507–14.
Tortella-Feliu M, Fullana MA, Pérez-Vigil A, Torres X, Chamorro J, Littarelli SA, et al. Risk factors for posttraumatic stress disorder: an umbrella review of systematic reviews and meta-analyses. Neurosci Biobehav Rev. 2019;107:154–65.
Liu C, Huang N, Fu M, Zhang H, Feng XL, Guo J. Relationship between risk perception, social support, and mental health among general Chinese population during the COVID-19 pandemic. Risk Manag Health Policy. 2021;14:1843.
Beck F, Leger D, Cortaredona S, Verger P, Peretti-Watel P, Seror V, et al. Would we recover better sleep at the end of Covid-19? A relative improvement observed at the population level with the end of the lockdown in France. Sleep Med. 2021;78:115–9.
Managing anxiety after getting a COVID-19 test. 2022. https://uwaterloo.ca/campus-wellness/managing-anxiety-after-getting-covid-19-test.
Liu X, Lin H, Jiang H, Li R, Zhong N, Su H, et al. Clinical characteristics of hospitalised patients with schizophrenia who were suspected to have coronavirus disease (COVID-19) in Hubei Province, China. Gen Psychiatry. 2020;33:e100222.
Brooks SK, Webster RK, Smith LE, Woodland L, Wessely S, Greenberg N, et al. The psychological impact of quarantine and how to reduce it: rapid review of the evidence. Lancet. 2020;395:912–20.
Yang H, Chen W, Hu Y, Chen Y, Zeng Y, Sun Y, et al. Pre-pandemic psychiatric disorders and risk of COVID-19: a UK Biobank cohort analysis. Lancet Healthy Longev. 2020;1:e69–e79.
Chen W, Zeng Y, Suo C, Yang H, Chen Y, Hou C, et al. Genetic predispositions to psychiatric disorders and the risk of COVID-19. BMC Med. 2022;20:1–9.
Taquet M, Luciano S, Geddes JR, Harrison PJ. Bidirectional associations between COVID-19 and psychiatric disorder: retrospective cohort studies of 62 354 COVID-19 cases in the USA. Lancet Psychiatry. 2021;8:130–40.
Lund LC, Hallas J, Nielsen H, Koch A, Mogensen SH, Brun NC, et al. Post-acute effects of SARS-CoV-2 infection in individuals not requiring hospital admission: a Danish population-based cohort study. Lancet Infect Dis. 2021;21:1373–82.
Klaser K, Thompson EJ, Nguyen LH, Sudre CH, Antonelli M, Murray B et al. Anxiety and depression symptoms after COVID-19 infection: results from the COVID Symptom Study app. medRxiv. 2021, https://www.medrxiv.org/content/10.1101/2021.07.07.21260137v1.
de Sousa AR, Teixeira JRB, Palma EMS, Moreira WC, Santos MB, de Carvalho HEF, et al. Psychological distress in men during the COVID-19 pandemic in Brazil: the role of the sociodemographic variables, uncertainty, and social support. Int J Environ Res Public Health. 2021;19:350.
Daly M, Robinson E. Psychological distress and adaptation to the COVID-19 crisis in the United States. J Psychiatr Res. 2021;136:603–9.
Perez-Arce F, Angrisani M, Bennett D, Darling J, Kapteyn A, Thomas K. COVID-19 vaccines and mental distress. PLoS One. 2021;16:e0256406.
Covid-19: Rapid tests for asymptomatic people to be rolled out. 2021. https://www.bbc.com/news/uk-55604677.
Excess deaths associated with COVID-19. 2022. https://www.cdc.gov/nchs/nvss/vsrr/covid19/excess_deaths.htm.
Acknowledgements
This work was supported with grants from NordForsk (COVIDMENT, NO. 105668 to UAV) and 1.3.5 project for disciplines of excellence, West China Hospital, Sichuan University (No. ZYYC21005 to HS). YW was supported by China Scholarship Council (NO. 202106240012 to YW) and HZs was supported by an UNSW Scientia Program Award during the conduct of this study. This research has been conducted using the UK Biobank Resource under Application 54803. We thank the team members involved in West China Biomedical Big Data Center at Sichuan University for their support.
Author information
Authors and Affiliations
Contributions
UAV and HS were responsible for the study’s concept and design. HY did the data and project management. YW, FG, and JW did the data cleaning and analysis. YW, UAV, and HS interpreted the data. YW, UAV, and HS drafted the manuscript. All the authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Competing interests
UAV has received grants for the current work from Nordforsk and grants outside the current work from the Icelandic Research Fund, Swedish Research Council, Swedish Cancer Society, and the European Research Council. HZ was an employee of the Centre for Big Data Research in Health at UNSW, which received a research grant from AbbVie Australia in 2020, unrelated to the current study. All other authors declare that they have no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Wang, Y., Ge, F., Wang, J. et al. Trends in incident diagnoses and drug prescriptions for anxiety and depression during the COVID-19 pandemic: an 18-month follow-up study based on the UK Biobank. Transl Psychiatry 13, 12 (2023). https://doi.org/10.1038/s41398-023-02315-7
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41398-023-02315-7
This article is cited by
-
Utilization of antidepressants, anxiolytics, and hypnotics during the COVID-19 pandemic
Translational Psychiatry (2024)