Abstract
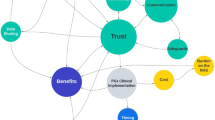
Pharmacogenomics (PGx) testing, which aims to identify the genes that affect our responses to drugs, has been favoured by healthcare professionals as a means of maximising drug efficacy and improving the safety and cost-effectiveness of healthcare. Support from the public is needed to determine the successful development of this technology and its implementation in society. Therefore, the objective of this paper was to analyse factors that influence stakeholders’ intentions to adopt pharmacogenomic testing in Malaysia. A validated instrument was administered through face-to-face interviews with a total of 421 adult respondents who were stratified according to 2 stakeholder groups: healthcare providers (n = 221) and patients/family members (n = 200). The data were then analysed using SPSS® version 24 software and the advanced multivariate statistical approach of Partial Least Square (PLS) path modelling in order to analyse the complex relationships among variables. Results of the studies indicated that the Malaysian stakeholders had a high amount of trust in the key players (mean score of 5.31), perceived high benefits (mean score of 5.53) and claimed to have high intentions of adopting PGx (mean score of 5.39). The majority of the predictors have significant direct relationships with the intention to adopt PGx, with the exception of moral concerns. Perceived benefits appeared to be the most important direct predictor of the intention to adopt PGx testing (ß = 0.371, P < 0.001) followed by trust in the key players (ß = 0.312, P < 0.001), engagement (ß = 0.272, P < 0.001) and religiosity (ß = 0.133, P < 0.01). In addition, perceived risks also had a direct negative association with the intention to adopt PGx (ß = −0.096, P < 0.05). At the same time, the perceived benefits also served as a mediator for all the other factors except risk. The results provide insights into the multidimensional nature of the determinants of the intention to adopt PGx testing in Malaysia. Although the results showed that the stakeholders in Malaysia were very positive towards PGx testing, they were also cautious about it. The predictors identified in this study can serve as indicators for social acceptance of PGx testing to facilitate the clinical research and implementation of PGx.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 print issues and online access
$259.00 per year
only $43.17 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Almomani B, Hawwa AF, Goodfellow NA, Millership JS, McElnay JC. Pharmacogenetics and the print media: What is the public told? BMC Med Genet. 2015;16:1–10.
Balasopoulou A, Mooy F-M, Baker DJ, Mitropoulou C, Skoufas E, Bulgiba A, et al. Advancing global precision medicine: an overview of genomic testing and counseling services in Malaysia. Omi J Integr Biol. 2017;21:733–40.
Sudia J. Exploring Barriers to the Adoption of Pharmacogenomic Technology in the Clinical Setting by Clinical Healthcare Providers. 2016. https://scholarship.shu.edu/cgi/viewcontent.dissertations.
Wolf CR, Smith G, Smith RL. Pharmacogenetics. BMJ. 2000;320:987–90.
Hudson J, Orviska M. European attitudes to gene therapy and pharmacogenetics. Drug Discov Today. 2011;16:843–7.
Bailey DS, Bondar A, Furness LM. Pharmacogenomics—it’s not just pharmacogenetics. Curr Opin Biotechnol. 1998;9:595–601.
Crews KR, Hicks JK, Pui CH, Relling MV, Evans WE. Pharmacogenomics and individualized medicine: translating science into practice. Clin Pharmacol Ther. 2012;92:467–75.
Lemke AA, Hulick PJ, Wake DT, Wang C, Sereika AW, Yu KD, et al. Patient perspectives following pharmacogenomics results disclosure in an integrated health system. Pharmacogenomics 2018;19:321–31.
Evans WE, Relling MV. Moving towards individualized medicine with pharmacogenomics. Nature 2004;429:464.
Cuffe S, Hon H, Qiu X, Tobros K, Wong CKA, De Souza B, et al. Cancer patients acceptance, understanding, and willingness-to-pay for pharmacogenomic testing. Pharmacogenet Genom. 2014;24:348–55.
Lachance K, Korol S, O’meara E, Ducharme A, Racine N, Liszkowski M, et al. Opinions, hopes and concerns regarding pharmacogenomics: a comparison of healthy individuals, heart failure patients and heart transplant recipients. Pharmacogenom J. 2015;15:13.
Trinidad SB, Coffin TB, Fullerton SM, Ralston J, Jarvik GP, Larson EB. “Getting off the Bus Closer to Your Destination”: patients’ views about pharmacogenetic testing. Perm J. 2015;19:31.
Daud ANA, Bergsma EL, Bergman JEH, De Walle HEK, Kerstjens-Frederikse WS, Bijker BJ, et al. Knowledge and attitude regarding pharmacogenetics among formerly pregnant women in the Netherlands and their interest in pharmacogenetic research. BMC Pregnancy Childbirth. 2017;17:120.
Chang MT, McCarthy JJ, Shin J. Clinical application of pharmacogenetics: focusing on practical issues. Pharmacogenomics. 2015;16:1733–41.
Luzum JA, Pakyz RE, Elsey AR, Haidar CE, Peterson JF, Whirl-Carrillo M, et al. The pharmacogenomics research network translational pharmacogenetics program: outcomes and metrics of pharmacogenetic implementations across diverse healthcare systems. Clin Pharmacol Ther. 2017;102:502–10.
Bank PC, Swen JJ, Guchelaar HJ. A nationwide cross-sectional survey of pharmacy students on pharmacogenetic testing in The Netherlands. Pharmacogenomics. 2018;19:311–9.
Just KS, Steffens M, Swen JJ, Patrinos GP, Guchelaar HJ, Stingl JC. Medical education in pharmacogenomics—results from a survey on pharmacogenetic knowledge in healthcare professionals within the European pharmacogenomics clinical implementation project Ubiquitous Pharmacogenomics (U-PGx). Eur J Clin Pharmacol. 2017;73:1247–52.
Amin L, Azad MAK, Ahmad Azlan NA, Zulkifli F. Factors influencing stakeholders’ attitudes toward cross-kingdom gene transfer in rice. New Genet Soc. 2014;33:370–99.
Amin L, Hashim H, Mahadi Z, Che Ngah A, Ismail K. Determinants of stakeholders’ attitudes to xenotransplantation. Xenotransplantation. 2018;22:e12430.
Bredahl L. Determinants of consumer attitudes and purchase intentions with regard to genetically modified foods—results of a cross-national survey. J Consum Policy. 2001;1:23–61.
Fishbein M, Ajzen I. Belief, attitude, intention, and behavior: an introduction to theory and research. Philos Rhetoric. 1975;10:130–2.
Master Z, Resnik DB. Hype and public trust in science. Sci Eng Ethics. 2013;19:321–35.
Amin L, Hashim H, Mahadi Z, Ibrahim M, Ismail K. Determinants of stakeholders’ attitudes towards biodiesel. Biotechnol Biofuels. 2017;10:219.
Gaskell G, Allum N, Stares S. Europeans and biotechnology in 2002. Eurobarometer 58.0. A report to the EC Directorate General for research from the project “Life Sciences in European Society” QLG7-CT-1999-00286. 2nd ed. Brussel: European Commission; 2003.
Pardo R, Midden C, Miller JD. Attitudes toward biotechnology in the European Union. J Biotechnol. 2002;98:9–24.
Stilgoe J, Lock SJ, Wilsdon J. Why should we promote public engagement with science? Public Underst Sci. 2014;23:4–15.
Samuel GN, Farsides B. Genomics England’s implementation of its public engagement strategy: Blurred boundaries between engagement for the United Kingdom’s 100,000 Genomes project and the need for public support. Public Underst Sci. 2018;27:352–64.
Frewer LJ, Howard C, Hedderley D, Shepherd R. What determines trust in information about food-related risks? Underlying psychological constructs. Risk Anal. 1996;16:473–86.
Hansen J, Holm L, Frewer L, Robinson P, Sandøe P. Beyond the knowledge deficit: recent research into lay and expert attitudes to food risks. Appetite. 2003;4:111–21.
Horst M, Kuttschreuter M, Gutteling JM. Perceived usefulness, personal experiences, risk perception and trust as determinants of adoption of e-government services in The Netherlands. Comput Hum Behav. 2007;23:1838–52.
Slovic P. The perception of risk: risk, society and policy. London (UK): Earthscan; 2000. p. 473.
Trumbo CW, McComas KA. The function of credibility in information processing for risk perception. Risk Anal. 2003;23:343–53.
Pin RR. Perceptions of nutrigenomics: affect, cognition & behavioral intention. Enschede: University of Twente; 2009. https://doi.org/10.3990/1.9789036528207.
Stewart-Knox B, Kuznesof S, Robinson J, Rankin A, Orr K, Duffy M, et al. Factors influencing European consumer uptake of personalised nutrition. Results of a qualitative analysis. Appetite. 2013;66:67–74.
Frewer LJ, Bergmann K, Brennan M, Lion R, Meertens R, Rowe G, et al. Consumer response to novel agri-food technologies: implications for predicting consumer acceptance of emerging food technologies. Trends Food Sci Technol. 2011;22:442–56.
Frewer LJ. Consumer acceptance and rejection of emerging agrifood technologies and their applications. Eur Rev Agric Econ. 2017;44:683–704.
Ghasemi S, Karami E, Azadi H. Knowledge, attitudes and behavioral intentions of agricultural professionals toward genetically modified (GM) foods: a case study in Southwest Iran. Sci Eng Ethics. 2013;19:1201–27.
Amin L, Hashim H, Mahadi Z, Ismail K. Determinants of the willingness to participate in biobanking among Malaysian stakeholders in the Klang Valley. BMC Med Res Methodol. 2018;18:163.
Ateeq-ur-Rehman, Shabbir MS. The relationship between religiosity and new product adoption. J Islam Mark. 2010;1:63–9.
Chen MF, Li HL. The consumer’s attitude toward genetically modified foods in Taiwan. Food Qual Prefer. 2007;18:662–74.
Amin L, Ahmad J, Jahi J, Nor AR, Osman M, Mahadi NM. Factors influencing malaysian public attitudes to agro-biotechnology. Public Underst Sci. 2011;20:674–89.
The Canadian Trade Commissioner Service. Welcome kit—Malaysia. 2016; 2019. http://www.infoexport.gc.ca/en.
Gaskell G, Allum N, Wagner W, Kronberger N, Torgersen H, Hampel J, et al. GM foods and the misperception of risk perception. Risk Anal. 2004;24:185–94.
Ronteltap A, van Trijp JCM, Renes RJ, Frewer LJ. Consumer acceptance of technology-based food innovations: lessons for the future of nutrigenomics. Appetite. 2007;49:1–7.
Verbeke W, Frewer LJ, Scholderer J, De Brabander HF. Why consumers behave as they do with respect to food safety and risk information. Anal Chim Acta. 2007;586:2–7.
Poínhos R, Van Der Lans IA, Rankin A, Fischer ARH, Bunting B, Kuznesof S, et al. Psychological determinants of consumer acceptance of personalised nutrition in 9 European countries. PLoS ONE. 2014;9:e110614.
Rankin A, Bunting BP, Poínhos R, van der Lans IA, Fischer AR, Kuznesof S, et al. Food choice motives, attitude towards and intention to adopt personalised nutrition. Public Health Nutr. 2018;14:2606–16.
Raats MM, Shepherd R, Sparks P. Including moral dimensions of choice within the structure of the theory of planned behavior. J Appl Soc Psychol. 1995;25:484–94.
Sparks P, Shepherd R. The role of moral judgments within expectancy-value-based attitude-behavior models. Ethics Behav. 2002;12:299–321.
Sparks P, Shepherd R, Frewer LJ. Assessing and structuring attitudes toward the use of gene technology in food production: the role of perceived ethical obligation. Basic Appl Soc Psychol. 1995;16:267–85.
Dean M, Raats MM, Shepherd R. Moral concerns and consumer choice of fresh and processed organic foods. J Appl Soc Psychol. 2008;38:2088–107.
Gaskell G, Allum N, Bauer M, Durant J, Allansdottir A, Bonfadelli H, et al. Biotechnology and the European public. Nat Biotechnol 2000;18:935.
Amin L, Jahi JM, Md. AR, Osman NM, Mahadi NM. Uncovering factors influencing Malaysian public attitude towards modern biotechnology. Asia-Pac J Mol Biol Biotechnol. 2006;14:33–9.
Bentler PM, Chou CP. Practical issues in structural modeling. Socio Methods Res. 1987;16:78–117.
Kline RB. Principles and practice of structural equation modeling: New York: Guilford Press Google Scholar; 2011.
Bandalos DL. Relative performance of categorical diagonally weighted least squares and robust maximum likelihood estimation. Struct Equ Model. 2014;21:102–16.
Kelley J. Public perceptions of genetic engineering: Australia, 1994. Canberra: Department of Industry, Science and Technology; 1995.
Kirk SFL, Greenwood D, Cade JE, Pearman AD. Public perception of a range of potential food risks in the United Kingdom. Appetite. 2002;38:189–97.
Rohrmann B. Risk perception of different societal groups: Australian findings and crossnational comparisons. Aust J Psychol. 1994;46:150–63.
Hair JF, Black WC, Babin BJ, Anderson RE. Multivariate Data Analysis. 7th ed. New York, NY, USA: Pearson; 2009.
Heale R, Twycross A. Validity and reliability in quantitative studies. Evid-Based Nurs. 2015;18:66–67.
Akter S, D’Ambra J, Ray P. Trustworthiness in mHealth information services: an assessment of a hierarchical model with mediating and moderating effects using partial least squares (PLS). J Am Soc Inf Sci Technol. 2011;62:100–16.
Memon AH, Rahman IA. Analysis of cost overrun factors for small scale construction projects in Malaysia using PLS-SEM method. Mod Appl Sci. 2013;7:78.
Tenenhaus M, Vinzi VE, Chatelin YM, Lauro C. PLS path modeling. Comput Stat Data Anal. 2005;48:159–205.
Chin WW. How to write up and report PLS analyses. In: Esposito Vinzi, V., Chin, W.W., Henseler, J., Wang, H., Eds, Handbook of Partial Least Squares: Concepts, Methods and Applications. Heidelberg, Dordrecht, London, New York: Springer; 2010. pp. 655-690. https://doi.org/10.1007/978-3-540-32827-8_29.
Hu LT, Bentler PM. Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Struct Equ Model. 1999;6:1–55.
Haga SB, O’Daniel JM, Tindall GM, Lipkus IR, Agans R. Survey of US public attitudes toward pharmacogenetic testing. Pharmacogenomics J. 2012;12:197.
Allum N, Sibley E, Sturgis P, Stoneman P. Religious beliefs, knowledge about science and attitudes towards medical genetics. Public Underst Sci. 2014;23:833–49.
Mustapa MAC, Amin L, Mahadi Z, Razman MR. Malaysian stakeholders’ intention to adopt genetic testing. Acad Strateg Manag J. 2019;18:1–5.
Haga SB, Barry WT, Mills R, Ginsburg GS, Svetkey L, Sullivan J, et al. Public knowledge of and attitudes toward genetics and genetic testing. Genet Test Mol Biomark. 2013;17:327–35.
Gaskell G, Allansdottir A, Allum N, Castro P, Esmer Y, Fischler C, et al. The 2010 Eurobarometer on the life sciences. Nat Biotechnol. 2011;29:113.
Vallée Marcotte B, Cormier H, Garneau V, Robitaille J, Desroches S, Vohl MC. Nutrigenetic testing for personalized nutrition: an evaluation of public perceptions, attitudes, and concerns in a Population of French Canadians. Lifestyle Genom. 2019;11:155–62.
Fallaize R, Macready AL, Butler LT, Ellis JA, Lovegrove JA. An insight into the public acceptance of nutrigenomic-based personalised nutrition. Nutr Res Rev. 2013;26:39–48.
Rogausch A, Prause D, Schallengerb A, Brockmöller J, Himmel W. Patients’ and physicians’ perspectives on pharmacogenetic testing. Pharmacogenomics. 2006;7:49–59.
Siegrist M. The influence of trust and perceptions of risks and benefits on the acceptance of gene technology. Risk Anal. 2000;20:195–204.
Frewer LJ, Scholderer J, Bredahl L. Communicating about the risks and benefits of genetically modified foods: the mediating role of trust. Risk Anal. 2003;23:1117–33.
Gutteling J, Haussen L, Van Der Veer N, Seydel E. Trust in governance and the acceptance of genetically modified food in the Netherlands. Public Underst Sci. 2006;15:103–12.
Hossain F, Onyango B. Product attributes and consumer acceptance of nutritionally enhanced genetically modified foods. Int J Consum Stud. 2004;28:255–67.
Tanaka Y. Major psychological factors affecting acceptance of gene-recombination technology. Risk Anal. 2004;24:1575–83.
Ho SS, Brossard D, Scheufele DA. Effects of value predispositions, mass media use, and knowledge on public attitudes toward embryonic stem cell research. Int J Public Opin Res. 2008;20:171–92.
Chatters LM. Religion and health: public health research and practice. Annu Rev Public Health. 2000;21:335–67.
Wallace JM, Forman TA. Religion’s role in promoting health and reducing risk among American youth. Heal Educ Behav. 1998;25:721–41.
Alves RR, da N, Alves H, da N, Barboza RRD, Souto W, de MS. Influência da religiosidade na saúde. Cienc e Saude Coletiva. 2010;15:2105–11.
Department of Statistics Malaysia. Current Population Estimates, Malaysia, 2018–2019; 2020. https://www.dosm.gov.my/v1/index.php.
Jamal R. Precision medicine: is Malaysia ready? Asia-Pacific. J Mol Med. 2017;7:1–4.
RinggitPlus. Best health insurance for cancer in Malaysia; 2020. https://ringgitplus.com/en/health-insurance.
Acknowledgements
The authors would like to thank all the respondents who took part in this study. The data collection was funded by Universiti Kebangsaan Malaysia under the project STEM-2014-005, while data analysis, writing and publication of the paper were funded by Universiti Kebangsaan Malaysia under the project DCP-2017-005/2.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This study has been approved by the Medical Research and Ethics Committee (MREC), Ministry of Health Malaysia (MOH), reference number (5)KKM/NIHSEC/P17-1382.
Informed consent
Written informed consent was given before the respondents answered the questionnaires and this was recorded by the enumerators.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Mustapa, M.A.C., Amin, L. & Mahadi, Z. Determinants of stakeholders’ intention to adopt pharmacogenomic. Pharmacogenomics J 20, 801–812 (2020). https://doi.org/10.1038/s41397-020-0167-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41397-020-0167-0