Abstract
Study design
Qualitative study.
Objective
Use an integrated knowledge translation (IKT) and theory-based approach, to (1) explore factors influencing smoking cessation behaviour among people with SCI, and (2) explore the preferred intervention and implementation options for smoking cessation interventions for persons with SCI.
Setting
Community.
Methods
Aligned with an IKT approach, an SCI organization was meaningfully engaged throughout the research process. Semi-structured interviews were conducted with people with SCI who have quit or tried to quit smoking. Barriers and facilitators to smoking cessation were extracted and deductively coded using the Theoretical Domains Framework (TDF) and inductively analysed. To identify intervention options, a behavioural analysis was conducted using the Behaviour Change Wheel. To identify implementation options, modes of delivery and intervention messengers were extracted. Modes of delivery were deductively coded, and themes relating to intervention messengers were constructed.
Results
Among the 12 participants (7 males; 6 with tetraplegia), seven had quit and five had relapsed. Across the 12 interviews, 130 barriers and 218 facilitators were coded to the TDF. The prominent TDF domains were beliefs about consequences, social influences, environmental context and resources, and behavioural regulation, and served as themes in the inductive analysis. Multiple modes of delivery and intervention messengers were considered important for the delivery of smoking cessation interventions.
Conclusion
This study is the first to use IKT and theory-based approaches to explore factors influencing smoking cessation among persons with SCI. Findings from this study resulted in the co-development of practical recommendations for future SCI-specific smoking cessation interventions.
Similar content being viewed by others
Introduction
Tobacco use is attributed to more than eight million deaths annually and is a leading cause of preventable disease and death [1]. The risks associated with smoking may be particularly concerning for persons with spinal cord injury (SCI) as they experience a disproportionate burden of tobacco-related health disparities, including an increased risk for urinary tract infections, more severe respiratory problems, and longer pressure injury recovery times compared to persons with SCI who do not smoke [2,3,4,5]. Furthermore, persons with SCI report smoking rates higher than those of the general population (19–48% vs. 13–15%, respectively) [3, 6,7,8].
High smoking rates among the SCI population may be partially attributable to low engagement with conventional smoking cessation services (i.e., behavioural counselling and nicotine replacement therapy). Among a population-based cohort of 833 adults with SCI in the US, 75.4% of current smokers with SCI reported trying to quit at least once [7]. However, of those attempting to quit, less than 30% sought professional help through counselling, pharmacotherapy, or both [7]. Comparatively, in a representative sample of 12,000 daily smokers in the US who attempted quitting in the past year, 36.1% reported using counselling, pharmacotherapy, or a combination of counselling and pharmacotherapy [9]. Despite high smoking rates, tobacco-related health disparities, and low smoking cessation treatment engagement, interventions have not been developed to support persons with SCI stop smoking.
Systematic application of behaviour change theory may be advantageous when designing, testing, and implementing behavioural interventions and may result in more effective interventions [10,11,12]. The Behaviour Change Wheel (BCW) is a theory-based intervention design tool developed from a synthesis of 19 frameworks of behaviour change [13]. The BCW is comprised of three layers that aim to understand the target behaviour in context, and link mechanisms of action to evidence-based intervention strategies (e.g., behaviour change techniques, intervention functions).
The innermost layer is the Capability-Opportunity-Motivation Behaviour (COM-B) model that identifies sources of behaviour (capability, opportunity, motivation) to be targeted by interventions [13]. The BCW recommends using the Theoretical Domains Framework (TDF) to conduct interviews to understand the behaviour in context (i.e., COM-B analysis) and identify the sources of behaviour to target in an intervention [11, 14]. Barriers and facilitators of a behaviour are identified and coded to the 14 domains of the TDF, which have been linked to the COM-B model through expert consensus [15]. Together the BCW and TDF provide a systematic method for linking context-dependent behavioural outcomes to mechanisms of action to evidence-based intervention and implementation options.
However, being theory-based does not necessarily mean that the intervention will be implemented in practice or be relevant to the target population. Integrated knowledge translation (IKT) aims to address this gap by meaningfully involving research users as partners alongside researchers throughout the research process to co-create research that is relevant, useful, and usable to research users [16]. In previous studies using an IKT approach, the establishment of meaningful partnerships with SCI organizations aimed to eliminate tokenism, improve meaningful engagement, and co-create usable research among the SCI population [17, 18]. Therefore, the aims of this qualitative study were to use an IKT approach and the theory-based BCW and TDF to:
-
(1)
Explore factors influencing smoking cessation behaviour among people with SCI; and
-
(2)
Explore the preferred intervention and implementation options for a smoking cessation intervention for persons with SCI.
Methods
Study design
This qualitative study uses IKT and theory-based approaches to explore barriers and facilitators to smoking cessation encountered by persons with SCI and explore the preferred intervention and implementation options for smoking cessation interventions for persons with SCI. As this study is based in British Columbia, Spinal Cord Injury British Columbia (SCI BC) was identified as a research user and was meaningfully involved as a partner throughout the entire research process. SCI BC is a not-for-profit organization dedicated to helping persons with SCI, and related disabilities, adjust, adapt, and thrive. SCI BC’s connection with and supports for persons with SCI made them the appropriate research user and partner for this study. Regular meetings were held throughout this project to evaluate methods, share findings, gather feedback, and enhance the interpretation of the findings for persons with SCI. (Details of the meetings are available in Supplementary File 1).
Procedures
Recruitment was done in partnership with SCI BC. The study was promoted through emails by our partner and on a multi-disciplinary SCI research website. Individuals were eligible to participate if they: (1) had been living with an SCI for at least 2 years; (2) currently or formerly smoked cigarettes; (3) if currently smoking, had ever tried to quit; (4) were at least 18 years of age; (5) currently resided in British Columbia; and (6) did not have a diagnosed co-morbidity affecting cognitive function. Guidance for conducting TDF interviews [14], recommends conducting and analysing an initial ten interviews and then three more until data saturation is achieved. However, we were constrained by time and availability of participants and were only able to conduct 12 interviews.
Prior to the interview, participants completed a survey requesting demographic, injury, and smoking history information. Following the completion of the survey, participants were contacted to schedule an interview. Upon completion of the interview, participants received a $25.00 gift card or e-gift card to the retailer of their choice.
Co-development of the interview guide was informed by previous qualitative studies specific to the SCI population [19] and guidelines for using the TDF to investigate implementation problems [14] (see Supplementary File 2 for interview guide). To address aim 1, open-ended questions promoted a discussion of the lived experiences of individuals with SCI quitting smoking and provided an open forum for individuals to expand on those lived experiences. If needed, probing questions tailored to the COM-B model were used to gain a deeper understanding of the participant’s identified barriers and facilitators. To address aim 2, we asked participant’s how or in what format they would prefer the intervention be delivered (i.e., mode of delivery) and who they would prefer to deliver the intervention (i.e., intervention messenger). If participants did not have a clear preference, the participant was prompted with examples of modes of delivery (e.g., face-to-face counselling, nicotine patch) and intervention messengers (e.g., physician, peer counsellor). The interview guide was piloted with one research assistant and one researcher with expertise in TDF interviews.
One researcher (KRW) conducted all interviews via telephone. Interviews were audio-recorded and transcribed verbatim by one researcher and four undergraduate research assistants. Each transcript was reviewed for accuracy by the researcher (KRW) before data analysis commenced.
Data analysis
Research paradigm and methodology
We approached this study using a pragmatic perspective which focused on the usefulness of research findings for solving practical, “real-world” problems [20]. Pragmatism promotes flexibility of investigative techniques and collaboration between researchers and community partners with differing philosophical assumptions, aligning with an IKT approach [21].
This study used a crystallisation methodology which encourages the use of multiple types of analyses (e.g., inductive and deductive analyses) to generate a complex interpretation of the phenomenon [22]. Using an inductive and deductive analysis (i.e., abductive analysis) to deepen understanding of the problem and contrast findings has been used previously to develop practical recommendations within the SCI population [19]. Furthermore, our approach was guided by the eight “Big-Tent” criteria for trustworthiness in qualitative research [23] to enhance rigour. See Supplementary File 4 for information on rigour and methodological coherence.
Aim 1: Explore factors influencing smoking cessation behaviour
Deductive analysis
Barriers and facilitators to smoking cessation were extracted by two reviewers independently (KRW, JDB) until agreement reached 70% to enhance interrater reliability of barrier and facilitator extraction. One researcher (KRW) then extracted barriers and facilitators from the remaining transcripts. The double-extracted barriers and facilitators were independently coded by two reviewers (KRW, JDB) to the 14 TDF domains until agreement reached substantial (κ = 0.61–0.80) [24], at which point, coding of the remaining barriers and facilitators was accomplished by one researcher (KRW).
Inductive analysis
The inductive thematic analysis enabled a deeper understanding of the context around the barriers and facilitators identified in the deductive analysis. The most prominent TDF domains identified in the deductive analysis served as themes within the inductive analysis. Within each theme, subthemes were constructed from the barriers and facilitators coded to their respective TDF domain. The analysis and construction of the subthemes followed guidelines for conducting a reflexive thematic analysis [25].
Aim 2: Identify intervention and implementation options
Intervention options
Intervention options refer to intervention functions and policy categories. The prominent TDF domains were linked to the COM-B model to determine sources of behaviour (i.e., capability, opportunity, motivation). The sources of behaviour were mapped to intervention functions (i.e., broad categories, such as education and training, for changing behaviour) and policy categories (i.e., broad methods for supporting the delivery of intervention functions, such as service provision or guidelines) using previously developed matrices [11] (see Supplementary File 3 for the matrices).
Implementation options
Implementation options refer to mode of delivery (i.e., “how” an intervention is delivered) and intervention messengers (i.e., “who” delivers the intervention). Modes of delivery and intervention messengers were extracted by two reviewers independently (KRW, JDB) until agreement reached 70%, at which point one researcher (KRW) extracted modes of delivery and intervention messengers from the remaining transcripts. The agreed-upon modes of delivery from four transcripts were coded to the Mode of Delivery Taxonomy version 0 (MoDtv0) [26] by two reviewers independently (KRW, JDB) until agreement reached substantial (κ = 0.61–0.80), at which point the remaining modes of delivery were coded to the MoDtv0 by one researcher (KRW). As no framework or taxonomy exists from which intervention messengers can be coded, intervention messengers were grouped into broad themes.
Disagreements between reviewers for all extraction and coding were resolved through discussion. If consensus could not be reached between the reviewers, a third reviewer (HLG) was consulted.
Results
Nineteen individuals expressed interest in participating; however, only 12 individuals were interviewed (see Table 1 for participant demographics). One individual did not provide contact information (n = 1), three individuals provided contact information but were unable to be reached (n = 3), and three individuals did not meet eligibility criteria (resided outside of BC, n = 2; does not have an SCI that occurred more than 2 years ago, n = 1). Interviews were between 30 and 63 min long (Mean = 42.1 min). Details of interrater reliability and methodological coherence can be found in Supplementary File 4.
Aim 1: Explore factors influencing smoking cessation behaviour—deductive analysis
A total of 265 factors (103 barriers, 162 facilitators) were extracted by two reviewers independently (KRW, JDB) from seven transcripts until 70% agreement was reached. From the remaining five transcripts, an additional 96 factors (61 facilitators, 35 facilitators) were extracted by KRW, resulting in a total of 361 factors (138 barriers, 223 facilitators). During TDF coding, 13 factors (8 barriers, 5 facilitators) were excluded as they were barriers/facilitators to smoking (n = 8), or they did not provide enough context to categorise to a TDF domain (n = 5), leaving a total of 348 factors (130 barriers, 218 facilitators) (see https://osf.io/k96nr/ for a detailed list of barriers and facilitators). Twenty-six factors (15 facilitators, 11 barriers) were coded to two TDF domains, resulting in a total of 374 TDF codes.
Figures 1 and 2 present the number and percent of barriers and facilitators identified across TDF domains. Figure 1 highlights environmental context and resources (n = 31, 22.0%), social influences (n = 24, 17.0%), behavioural regulation (n = 24, 17.0%), and beliefs about consequences (n = 23, 16.3%) as the most commonly coded domains among the barriers. As seen in Fig. 2, beliefs about consequences (n = 64, 27.6%), social influence (n = 47, 20.3%), behavioural regulation (n = 46, 19.8%), and environmental context and resources (n = 30, 12.9%) were the most commonly coded TDF domains among the facilitators.
The inner ring is COM-B sources of behaviour and outer ring is TDF domains. Some barriers were coded to more than one domain. Capability category “Other” includes memory, attention, and decision processes, and skills. Motivation category “Other” includes goals, optimism, and social/professional roles and identity. Behavioural Reg. behavioural regulation, Know. knowledge, Beliefs about Cons. beliefs about consequences, Intent intention, ECR environmental context and resources.
The inner ring is COM-B sources of behaviour and outer ring is TDF domains. Some facilitators were coded to more than one domain. Capability category “Other” includes memory, attention, and decision processes, and skills. Motivation category “Other” includes emotions, goals, and social/professional roles and identity. Behavioural Reg. behavioural regulation, Know. knowledge, Beliefs about Cons. beliefs about consequences, Intent intention, BCap beliefs about capabilities, ECR environmental context and resources.
Aim 1: Explore factors influencing smoking cessation behaviour—inductive analysis
The four most prominent TDF domains (i.e., beliefs about consequences, social influences, environmental context and resources, and behavioural regulation) served as themes for the inductive analysis. A brief description of each theme is presented below. Table 2 describes each subtheme and provides accompanying quotes that characterises each subtheme.
Beliefs about consequences
This theme focusses on participants’ motivation to quit smoking, whereby individuals weigh the perceived risks of continuing to smoke against the perceived risks of quitting smoking. When the risks of smoking outweighed the risks of quitting, participants often voiced intentions and efforts to stop smoking. Significant events (e.g., a loved one getting sick) served as “wake-up calls” for participants, in which they suddenly perceived a high vulnerability to the risks of smoking, and this often led to smoking cessation efforts. The beliefs about consequences theme includes three subthemes: (1) perceived risks of smoking; (2) the risks of quitting are more distressing than those of smoking; and (3) wake-up calls.
Social influences
This theme focusses on the crucial role that relationships play in altering one’s smoking behaviour. Participants’ decision to stop smoking was influenced by societal norms and values and their social network. However, the ability to stay quit was influenced by the accommodations made by others to support the individual while they stopped smoking. The social influences theme includes two subthemes: (1) adhering to social norms and values; and (2) expected and received support from others who smoke.
Environmental context and resources
This theme focusses on the environmental circumstances that may support smoking cessation. The introduction of smoke-free legislation and other tobacco control policies restricted participants’ opportunity to smoke, and as a result, many chose to quit smoking at these times for convenience. Similarly, when persons with SCI sustain their injury, the hospital environment and life-altering circumstances force these newly injured individuals to stop smoking. While the above circumstances showcase how the environment can act as a facilitator, the environment can just as often act as a barrier to smoking cessation. Boredom, habitual smoking environment (i.e., places where participants regularly smoke), and easy access to cigarettes represent barriers that persons with SCI encounter that impede their smoking cessation efforts. The environmental context and resources theme contains two subthemes: (1) reconciling pre- and post-injury ways of life; and (2) government actions made it convenient to quit.
Behavioural regulation
This theme focusses on the concept of self-regulation, including challenges related to self-regulatory ability that often leads to relapse as participants struggle to overcome intense cravings and urges to smoke. The presence of stressful circumstances (e.g., secondary health conditions) or alcohol use can exacerbate self-regulation, which made some participants more susceptible to relapse. The behavioural regulation theme contains three subthemes: (1) managing cravings requires a tailored approach; (2) quitting smoking is just one more thing to cope with, and (3) alcohol and cigarettes go “hand-in-hand”.
Aim 2: Identifying intervention and implementation options
Intervention options
When linked to the COM-B model of the BCW, the four prominent TDF domains suggest that all intervention functions and all policy categories are potentially relevant to support smoking cessation for persons with SCI.
Implementation options
A total of 98 implementation options (55 modes of delivery, 43 intervention messengers) were extracted. Somatic forms of delivery (e.g., pharmacotherapy), such as inhalers/vaporisers (n = 10), patches (n = 8), pills (n = 7), or other (n = 2), were identified most frequently by participants accounting for 45.0% of the total codes. Human forms of delivery, such as face-to-face (n = 13), audio and video calls (n = 2), or unspecified (n = 4), were the second most frequently identified mode of delivery accounting for 31.8% of the total codes. Digital and printed material comprised 15.0% and 8.4% of the total codes, respectively. Preferred intervention messengers included health care professionals, disability organizations, and peers with SCI. See Tables 3 and 4 for mode of delivery coding and intervention messenger themes, respectively.
Discussion
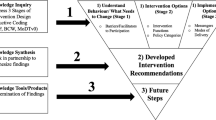
This study used IKT and theory-based approaches, to (1) explore factors influencing the smoking cessation behaviour among persons with SCI and (2) explore the preferred intervention and implementation options for smoking cessation interventions for persons with SCI. This study found the factors participants most frequently discussed as influential to their smoking cessation behaviours were related to the TDF domains of beliefs about consequences, social influences, environmental context and resources, and behavioural regulation. Additionally, findings suggest that all intervention options (i.e., intervention functions and policy categories) are potentially relevant in developing smoking cessation interventions. Furthermore, persons with SCI indicated a preference for face-to-face interventions supplemented with pharmacotherapy delivered by a variety of intervention messengers. The findings from this study have important implications for what, when, how, and who delivers smoking cessation interventions for persons with SCI. Figure 3 summarises how findings might be used to inform an intervention. These recommendations were co-developed with SCI BC.
Our findings are similar to those found in a previous study exploring barriers and facilitators to smoking cessation among persons with SCI in the US [26]. Cost associated with smoking and health concerns were identified as facilitators to smoking cessation in both this study and the study by Saunders et al. [27], while co-morbid alcohol use was a commonly identified barrier among both studies. Although boredom was identified as a barrier in both studies, Saunders et al. [27] reported that participants related feelings of boredom with unemployment; whereas, in our study, unemployment was never discussed by participants and boredom was primarily related to returning home after their injury or coping with a secondary health condition. This difference in boredom may be related to a difference in national contexts and policies, and/or years post-injury as the participants in our study had on average been living with their injury for longer than those in Saunders et al. [27] (28.5 years vs. 6.5 years post-injury, respectively). Research suggests that employment among persons with SCI increases with time post-injury [28], therefore, the participants in our study may have been more likely to be employed. Furthermore, we identified barriers and facilitators not identified by Saunders et al. [27] including concerns about post-cessation weight gain, coping with secondary health conditions while stopping smoking, and the risk of relapse during rehabilitation and community reintegration after injury.
Our study expands on the work done by Saunders et al. [27] through the use of behaviour change theory and through the exploration of preferred intervention and implementation options. While similar barriers and facilitators were identified in both studies, our study links the barriers and facilitators to behaviour change theory which may aid in the development of a future theory-informed smoking cessation intervention for persons with SCI [11]. Furthermore, our study explored preferred modes of delivery and intervention messengers which may enhance the likelihood that a smoking cessation intervention is relevant and addresses the needs and priorities of persons with SCI stopping smoking.
Limitations
Our recruitment was constrained by convenience sampling. Specific demographic parameters were not represented in our sample (e.g., under the age of 30, those with injuries having occurred less than 5 years ago, individuals with SCI who ambulate, and persons of colour and indigenous persons with SCI). Qualitative data is inherently situational and contextual, and therefore, not typically generalisable, but rather transferable (i.e., the story of the research evokes vicarious emotional experience in the reader and they intuitively transfer the research to their own actions) [23]. Using the eight “Big Tent” criteria [23], we have aimed to achieve thick and rich descriptions and findings that evoke transferability.
The frequency of TDF codes does not necessarily indicate the importance or lack of importance of TDF domains. Instead, frequency refers to the number of times across transcripts participants discussed each domain. As the TDF does not necessarily imply importance, we used a thematic analysis to illustrate important elements within the most heavily discussed domains. Another limitation of using the TDF is that the TDF is a framework and not a theory. As a framework, the TDF describes the factors that are suggested to influence behaviour but does not specify how the factors might relate to or influence each other [29]. Lack of clarity on the relationship between domains may provide difficulties when trying to develop future theory-based smoking cessation interventions. However, findings informed the selection of behaviour change theory that may be useful for developing smoking cessation interventions for persons with SCI, such as the Health Action Process Approach [30, 31].
Future directions
Future research efforts should focus on understanding the smoking cessation behaviours of individuals with injuries that occurred less than 5 years ago as our study revealed a susceptibility to relapse upon returning home from the hospital and rehabilitation after their injury. Additional demographic parameters that research should address include individuals with SCI under the age of 30, individuals with SCI who ambulate, and persons of colour and indigenous persons with SCI. Individuals within these demographic parameters may encounter different barriers to smoking cessation than those represented in this study. Also, further research is needed to explore the influence of sex and gender-related factors in smoking cessation among persons with SCI.
Future research should study the effects of theory-based and co-developed smoking cessation interventions for persons with SCI. Rigorous testing will be needed to ensure the efficacy, feasibility, and effectiveness of the interventions for persons with SCI.
Conclusion
To our knowledge, this study is the first to use an IKT approach and the BCW and TDF to explore factors influencing the smoking cessation behaviours of persons with SCI and identify the intervention and implementation options for smoking cessation interventions preferred by persons with SCI. Our findings suggest that conventional smoking cessation interventions may need to be optimised to address the unique circumstances encountered by persons with SCI when stopping smoking. Continued efforts are needed to ensure these findings are translated in partnership with SCI organizations and contribute to improvements in health among persons with SCI.
Data availability
The data that support the findings of this study are available from the corresponding author on reasonable request. The data are not publicly available due to privacy or ethical reasons.
References
Fast Facts and Fact Sheets. Centers for Disease Control and Prevention. 2021. https://www.cdc.gov/tobacco/data_statistics/fact_sheets/index.htm?s_cid=osh-stu-home-spotlight-001.
Davies DS, McColl MA. Lifestyle risks for three disease outcomes in Spinal Cord Injury. Clin Rehabil. 2002;16:96–108.
Haisma JA, van der Woude LH, Stam HJ, Bergen MP, Sluis TA, Post MW, et al. Complications following spinal cord injury: occurrence and risk factors in a longitudinal study during and after inpatient rehabilitation. J Rehabil Med. 2007;39:393–8.
Lane CA, Selleck C, Chen Y, Tang Y. The impact of smoking and smoking cessation on wound healing in spinal cord–injured patients with pressure injuries. J Wound Ostomy Cont Nurs. 2016;43:483–7.
Spungen AM, Grimm DR, Lesser M, Bauman WA, Almenoff PL. Self-reported prevalence of pulmonary symptoms in subjects with spinal cord injury. Spinal Cord. 1997;35:652–7.
Krause JS, Cao Y, Saunders LL. Changes in cigarette smoking after traumatic spinal cord injury. Rehabil Psychol. 2015;60:379–82.
Saunders LL, Krause JS, Saladin M, Carpenter MJ. Prevalence of cigarette smoking and attempts to quit in a population-based cohort with spinal cord injury. Spinal Cord. 2015;53:641–5.
Brule S, McDonald H. Health fact sheets: smoking, 2019. Government of Canada, Statistics Canada; 2020. https://www150.statcan.gc.ca/n1/pub/82-625-x/2020001/article/00003-eng.htm.
Shiffman S, Brockwell SE, Pillitteri JL, Gitchell JG. Individual differences in adoption of treatment for smoking cessation: demographic and smoking history characteristics. Drug Alcohol Depend. 2008;93:121–31.
Michie S, Prestwich A. Are interventions theory-based? development of a theory coding scheme. Health Psychol. 2010;29:1–8.
Michie S, Atkins L, West R. The behaviour change wheel: a guide to designing interventions. Great Britain: Silverback Publishing; 2014.
Rothman AJ. “ Is there nothing more practical than a good theory?”: why innovations and advances in health behavior change will arise if interventions are used to test and refine theory. Int J Behav Nutr Phys Act. 2004;1:11.
Michie S, van Stralen MM, West R. The behaviour change wheel: a new method for characterising and designing behaviour change interventions. Implement Sci. 2011;6:1–12.
Atkins L, Francis J, Islam R, O’Connor D, Patey A, Ivers N, et al. A guide to using the theoretical domains framework of behaviour change to investigate implementation problems. Implement Sci. 2017;12:1–18.
Cane J, O’Connor D, Michie S. Validation of the theoretical domains framework for use in behaviour change and implementation research. Implement Sci. 2012;7:1–17.
Gainforth HL, Hoekstra F, McKay R, McBride CB, Sweet SN, Martin Ginis KA, et al. Integrated knowledge translation guiding principles for conducting and disseminating spinal cord injury research in partnership. Arch Phys Med Rehabil. 2021;102:656–63.
Martin Ginis KA, Latimer-Cheung A, Corkum S, Ginis S, Anathasopoulos P, Arbour-Nicitopoulos K, et al. A case study of a community-university multidisciplinary partnership approach to increasing physical activity participation among people with spinal cord injury. Transl Behav Med. 2012;2:516–22.
Ma JK, Cheifetz O, Todd KR, Chebaro C, Phang SH, Shaw RB, et al. Co-development of a physiotherapist-delivered physical activity intervention for adults with spinal cord injury. Spinal Cord. 2020;58:778–86.
Giroux EE, Casemore S, Clarke TY, McBride CB, Wuerstl KR, Gainforth HL. Enhancing participation while aging with spinal cord injury: applying behaviour change frameworks to develop intervention recommendations. Spinal Cord. 2020;59:665–74.
Yvonne Feilzer M. Doing mixed methods research pragmatically: Implications for the rediscovery of pragmatism as a research paradigm. J Mixed Methods Res. 2009;4:6–16.
Onwuegbuzie AJ, Leech NL. On becoming a pragmatic researcher: the importance of combining quantitative and qualitative research methodologies. Int J Soc Res Methodol. 2005;8:375–87.
Ellingson LL. Engaging crystallization in qualitative research: an introduction. Thousand Oaks: Sage Publications; 2009.
Tracy SJ. Qualitative quality: eight “big tent” criteria for excellent qualitative research. Qual Inq. 2010;16:837–51.
Landis JR, Koch GG. The measurement of observer agreement for categorical data. Biometrics. 1977;33:159.
Terry G, Hayfield N, Clarke V, Braun V. Thematic analysis. In: Willig C, Rogers WS, editors. The Sage handbook of qualitative research in psychology. London: SAGE; 2017.
Carey R, Evans F, Horan M, Johnston M, West R, Michie S. Mode of delivery of behaviour change interventions taxonomy version 0 (MoDTv0). 2016.
Saunders L, Newman S, Aust R, Krause JS. Qualitative study of barriers and facilitators to cigarette smoking after spinal cord injury. Rehabil Psychol. 2018;63:400–7.
Anderson D, Dumont S, Azzaria L, Bourdais ML, Noreau L. Determinants of return to work among spinal cord injury patients: a literature review. J Vocat Rehabil. 2007;27:57–68.
Nilsen P. Making sense of implementation theories, models and Frameworks. Implement Sci. 2015;10:53–79.
Michie SF, West R, Campbell R, Brown J, Gainforth HL. ABC of behaviour change theories. Sutton: Silverback; 2014.
Schwarzer R, Lippke S, Luszczynska A. Mechanisms of health behavior change in persons with chronic illness or disability: the Health Action Process Approach (HAPA). Rehabil Psychol. 2011;56:161–70.
Acknowledgements
We would like to acknowledge Emily Stone, Jiawin Lim, Lexington Kinnear, and Kylie Lundberg-Dorr for their help with interview transcription. We would also like to acknowledge Spinal Cord Injury British Columbia for their efforts with recruitment. The research team also acknowledges all participants for their time participating in the interviews.
Funding
HLG is supported by a Michael Smith Health Research BC Scholar Award (Formerly MSFHR, Canada, no. 16910). KRW is supported by a CIHR Frederick Banting and Charles Best Canada Graduate Scholarship—Doctoral Award (no. 175909).
Author information
Authors and Affiliations
Contributions
KRW, CBM, and HLG were responsible for co-developing the research question, selecting the methodology, co-developing all recruitment materials, and co-developing the interview guide. KRW conducted all interviews. KRW and JDB extracted and deductively coded all transcripts. HLG provided coding oversight. KRW inductively coded all transcripts. FH and HLG acted as critical friends and provided feedback on the thematic analysis. CBM provided partner oversight. HLG supervised the research. KRW wrote the manuscript. All authors contributed to the critical revision of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
We certify that all applicable institutional and governmental regulations concerning the ethical use of human volunteers were followed during the course of this research. Ethics approval for this study was obtained from the University of British Columbia Okanagan Behavioural Research Ethics Board (#H19–01020).
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wuerstl, K.R., McBride, C.B., Deschênes-Bilodeau, J. et al. Exploring smoking cessation experiences among persons with spinal cord injury: Informing theory-based recommendations for interventions. Spinal Cord 61, 27–36 (2023). https://doi.org/10.1038/s41393-022-00856-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41393-022-00856-0