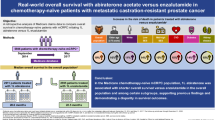
Abstract
Background
Although 5-alpha-reductase inhibitors (5ARIs) have been shown to benefit men with prostate cancer (PCa) on active surveillance (AS), their long-term safety remains controversial. Our objective is to describe the long-term association of 5ARI use with PCa progression in men on AS.
Materials/subjects and methods
The cohort of men with low-risk PCa was derived from a prospectively maintained AS database at the Princess Margaret (1995–2016). Pathologic, grade, and volume progression were the primary end points. Kaplan–Meier time-to-event analysis was performed and Cox proportional hazards regression was used to determine predictors of progression where 5ARI exposure was analyzed as a time-dependent variable. Patients who came off AS prior to any progression events were censored at that time.
Results
The cohort included 288 men with median follow-up of 82 months (interquartile range: 37–120 months). Among non-5ARI users (n = 203); 114 men (56.2%) experienced pathologic progression compared with 24 men (28.2%) in the 5ARI group (n = 85), (p < 0.001). Grade and volume progression were higher in the non-5ARI group compared with the 5ARI group (n = 82; 40.4% vs. n = 19; 22.4% respectively, p = 0.003 for grade progression; n = 87; 43.1% and n = 15; 17.7%, respectively for volume progression p < 0.001). Lack of 5ARI use was independently positively associated with pathologic progression (HR: 2.65; CI: 1.65–4.24), grade progression (HR: 2.75; CI: 1.49–5.06), and volume progression (HR: 3.15; CI: 1.78–5.56). The frequency of progression to high-grade (Grade Group 4–5) tumors was not significantly different between the groups.
Conclusions
Use of 5ARIs diminished both grade and volume progression without an increased risk of developing Grade Groups 4–5 disease.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Tosoian JJ, Carter HB, Lepor A, Loeb S. Active surveillance for prostate cancer: current evidence and contemporary state of practice. Nat Rev Urol. 2016;13:205–15.
Cooperberg MR. Active Surveillance for low-risk prostate cancer—an evolving international standard of care. JAMA Oncol. 2017;3:1398–9.
Klotz L, Vesprini D, Sethukavalan P, Jethava V, Zhang L, Jain S, et al. Long-term follow-up of a large active surveillance cohort of patients with prostate cancer. J Clin Oncol. 2015;33:272–7.
Tosoian JJ, Trock BJ, Landis P, Feng Z, Epstein JI, Partin AW, et al. Active surveillance program for prostate cancer: an update of the Johns Hopkins experience. J Clin Oncol. 2011;29:2185–90.
Tosoian JJ, Mamawala M, Epstein JI, Landis P, Wolf S, Trock BJ, et al. Intermediate and longer-term outcomes from a prospective active-surveillance program for favorable-risk prostate cancer. J Clin Oncol. 2015;33:3379–85.
Bruinsma SM, Bangma CH, Carroll PR, Leapman MS, Rannikko A, Petrides N, et al. Active surveillance for prostate cancer: a narrative review of clinical guidelines. Nat Rev Urol. 2016;13:151–67.
Loeb S. Active surveillance offers functional advantages without impacting survival for low-risk prostate cancer. Eur Urol. 2018;73:868–9.
Loeb S, Folkvaljon Y, Curnyn C, Robinson D, Bratt O, Stattin P. Uptake of active surveillance for very-low-risk prostate cancer in Sweden. JAMA Oncol. 2017;3:1393–8.
Komisarenko M, Timilshina N, Richard PO, Alibhai SM, Hamilton R, Kulkarni G, et al. Stricter active surveillance criteria for prostate cancer do not result in significantly better outcomes: a comparison of contemporary protocols. J Urol. 2016;196:1645–50.
Wong LM, Ferrara S, Alibhai SM, Evans A, Van der Kwast T, Trottier G, et al. Diagnostic prostate biopsy performed in a non-academic center increases the risk of re-classification at confirmatory biopsy for men considering active surveillance for prostate cancer. Prostate Cancer Prostatic Dis. 2015;18:69–74.
Wong LM, Trottier G, Toi A, Lawrentschuk N, Van der Kwast TH, Zlotta A, et al. Should follow-up biopsies for men on active surveillance for prostate cancer be restricted to limited templates? Urology. 2013;82:405–9.
Weiss B, Loeb S. Standard and targeted biopsy during follow-up for active surveillance. Rev Urol. 2015;17:112–3.
Violette PD, Saad F. Chemoprevention of prostate cancer: myths and realities. J Am Board Fam Med. 2012;25:111–9.
Vemana G, Hamilton RJ, Andriole GL, Freedland SJ. Chemoprevention of prostate cancer. Annu Rev Med. 2014;65:111–23.
Richard PO, Finelli A. 5-Alpha reductase inhibitors in active surveillance. Curr Opin Urol. 2014;24:324–8.
Jayalath VH, Nayan M, Finelli A, Komisarenko M, Timilshina N, Kulkarni GS, et al. Statin use and time to progression in men on active surveillance for prostate cancer. Prostate Cancer Prostatic Dis. 2018;21:509–15.
Finelli A, Trottier G, Lawrentschuk N, Sowerby R, Zlotta AR, Radomski L, et al. Impact of 5alpha-reductase inhibitors on men followed by active surveillance for prostate cancer. Eur Urol 2011;59:509–14.
Shelton PQ, Ivanowicz AN, Wakeman CM, Rydberg MG, Norton J, Riggs SB, et al. Active surveillance of very-low-risk prostate cancer in the setting of active treatment of benign prostatic hyperplasia with 5alpha-reductase inhibitors. Urology. 2013;81:979–84.
Ross AE, Feng Z, Pierorazio PM, Landis P, Walsh PC, Carter HB, et al. Effect of treatment with 5-alpha reductase inhibitors on progression in monitored men with favourable-risk prostate cancer. BJU Int. 2012;110:651–7.
Vidal AC, Howard LE, Moreira DM, Castro-Santamaria R, Andriole GL, Freedland SJ. Aspirin, NSAIDs, and risk of prostate cancer: results from the REDUCE study. Clin Cancer Res. 2015;21:756–62.
Wong LM, Fleshner N, Finelli A. Impact of 5-alpha reductase inhibitors on men followed by active surveillance for prostate cancer: a time-dependent covariate reanalysis. Eur Urol. 2013;64:343.
Babaian RJ, Toi A, Kamoi K, Troncoso P, Sweet J, Evans R, et al. A comparative analysis of sextant and an extended 11-core multisite directed biopsy strategy. J Urol. 2000;163:152–7.
Fleshner NE, Lucia MS, Egerdie B, Aaron L, Eure G, Nandy I, et al. Dutasteride in localised prostate cancer management: the REDEEM randomised, double-blind, placebo-controlled trial. Lancet. 2012;379:1103–11.
Dai C, Ganesan V, Zabell J, Nyame YA, Almassi N, Greene DJ, et al. Impact of 5alpha-reductase inhibitors on disease reclassification among men on active surveillance for localized prostate cancer with favorable features. J Urol. 2018;199:445–52.
Komisarenko M, Wong LM, Richard PO, Timilshina N, Toi A, Evans A, et al. An increase in gleason 6 tumor volume while on active surveillance portends a greater risk of grade reclassification with further followup. J Urol. 2016;195:307–12.
Iremashvili V, Pelaez L, Manoharan M, Jorda M, Rosenberg DL, Soloway MS. Pathologic prostate cancer characteristics in patients eligible for active surveillance: a head-to-head comparison of contemporary protocols. Eur Urol. 2012;62:462–8.
Andriole GL, Bostwick D, Brawley OW, Gomella L, Marberger M, Montorsi F, et al. The effect of dutasteride on the usefulness of prostate specific antigen for the diagnosis of high grade and clinically relevant prostate cancer in men with a previous negative biopsy: results from the REDUCE study. J Urol. 2011;185:126–31.
Thompson IM, Goodman PJ, Tangen CM, Lucia MS, Miller GJ, Ford LG, et al. The influence of finasteride on the development of prostate cancer. N Engl J Med. 2003;349:215–24.
Andriole GL, Bostwick DG, Brawley OW, Gomella LG, Marberger M, Montorsi F, et al. Effect of dutasteride on the risk of prostate cancer. N Engl J Med. 2010;362:1192–202.
Unger JM, Hershman DL, Till C, Tangen CM, Barlow WE, Ramsey SD, et al. Using Medicare claims to examine long-term prostate cancer risk of finasteride in the prostate cancer prevention trial. J Natl Cancer Inst. 2018.
Preston MA, Wilson KM, Markt SC, Ge R, Morash C, Stampfer MJ, et al. 5Alpha-reductase inhibitors and risk of high-grade or lethal prostate cancer. JAMA Intern Med. 2014;174:1301–7.
Wallerstedt A, Strom P, Gronberg H, Nordstrom T, Eklund M. Risk of prostate cancer in men treated with 5alpha-reductase inhibitors—a Large Population-Based Prospective Study. J Natl Cancer Inst. 2018;110:1216–21.
Kulkarni GS, Lockwood G, Evans A, Toi A, Trachtenberg J, Jewett MA, et al. Clinical predictors of Gleason score upgrading: implications for patients considering watchful waiting, active surveillance, or brachytherapy. Cancer. 2007;109:2432–8.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Finelli, A., Komisarenko, M., Martin, L.J. et al. Long-term use of 5-alpha-reductase inhibitors is safe and effective in men on active surveillance for prostate cancer. Prostate Cancer Prostatic Dis 24, 69–76 (2021). https://doi.org/10.1038/s41391-020-0218-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41391-020-0218-2