Abstract
Background
Prostate cancer in black men is associated with poorer outcomes than their white counterparts. However, most studies reporting this disparity were conducted in localized prostate cancer and primarily in the United States.
Methods
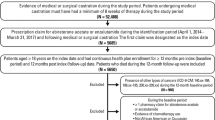
Data regarding prostate cancer incidence and mortality for East London between 2008 and 2010 were obtained from the UK National Disease Registration Service. We further evaluated survival outcomes of 425 cases of mCRPC in St Bartholomew’s Hospital, East London, between 1997 and 2016, and analyzed whether ethnicity impacted on responses to different treatment types.
Results
The incidence of prostate cancer in black men was higher than white men in East London. Prostate cancer-specific mortality was proportional to incidence based on ethnic groups. In the detailed analysis of 425 patients, 103 patients (24%) were black (B), and the remainder white (W). Baseline characteristics were comparable in both groups, although black patients had a lower baseline hemoglobin (p < 0.001). Median overall survival for the total cohort was 25.5 months (B) vs 21.8 months (W) (hazard ratio (HR) = 0.81, p = 0.08). There was prolonged survival in the black population in those who only received hormone-based treatment throughout their treatment course; 39.7 months (B) vs 17.1 months (W) (HR = 0.54, p = 0.019).
Conclusion
Black men may do better than white men with mCRPC, in the context of equal access to healthcare. The study also suggests a greater margin of benefit of hormone-based therapy in the black subpopulation.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Ben-Shlomo Y, Evans S, Ibrahim F, Patel B, Anson K, Chinegwundoh F, et al. The risk of prostate cancer amongst black men in the United Kingdom: the PROCESS cohort study. Eur Urol. 2008;53:99–105.
Evans S, Metcalfe C, Ibrahim F, Persad R, Ben-Shlomo Y. Investigating black-white differences in prostate cancer prognosis: a systematic review and meta-analysis. Int J Cancer. 2008;123:430–5.
Ellis L, Nyborg H. Racial ethnic variations in male testosterone levels—a probable contributor to group-differences in health. Steroids. 1992;57:72–5.
Okobia MN, Zmuda JM, Ferrell RE, Patrick AL, Bunker CH. Chromosome 8q24 variants are associated with prostate cancer risk in a high risk population of African ancestry. Prostate. 2011;71:1054–63.
Presley CJ, Raldow AC, Cramer LD, Soulos PR, Long JB, Yu JB, et al. A new approach to understanding racial disparities in prostate cancer treatment. J Geriatr Oncol. 2013;4:1–8.
Tyson MD II, Castle EP. Racial disparities in survival for patients with clinically localized prostate cancer adjusted for treatment effects. Mayo Clin Proc. 2014;89:300–7.
Wang C, Kamrava M, King C, Steinberg ML. Racial disparity in prostate cancer-specific mortality for high-risk prostate cancer: a population-based study. Cureus. 2017;9:e961.
Thompson I, Tangen C, Tolcher A, Crawford E, Eisenberger M, Moinpour C. Association of African-American ethnic background with survival in men with metastatic prostate cancer. J Natl Cancer Inst. 2001;93:219–25.
Park HS, Lloyd S, Decker RH, Wilson LD, Yu JB. Limitations and biases of the surveillance, epidemiology, and end results database. Curr Probl Cancer. 2012;36:216–24.
Armstrong AJ, Halabi S, Luo J, Nanus DM, Giannakakou P, Szmulewitz RZ, et al. Prospective multicenter validation of androgen receptor splice variant 7 and hormone therapy resistance in high-risk castration-resistant prostate cancer: the PROPHECY study. J Clin Oncol. 2019;37:1120–9.
Lloyd T, Hounsome L, Mehay A, Mee S, Verne J, Cooper A. Lifetime risk of being diagnosed with, or dying from, prostate cancer by major ethnic group in England 2008-2010. BMC Med. 2015;13:171.
Gov.UK. Population of England and Wales.
Gov.UK. Regional Ethnic Diversity.
European Association of Urology guideline version 2015. http://www.uroweb.org/guidelines/.
Dess RT, Hartman HE, Mahal BA, Soni PD, Jackson WC, Cooperberg MR, et al. Association of black race with prostate cancer-specific and other-cause mortality. JAMA Oncol. 2019;5:975–83.
Paller CJ, Wang L, Brawley OW. Racial inequality in prostate cancer outcomes-socioeconomics. Not Biol JAMA Oncol. 2019;5:983–4.
McNamara MA GD, et al. Overall survival by race in chemotherapy-naïve metastatic castration-resistant prostate cancer (mCRPC) patients treated with abiraterone acetate or enzalutamide. J Clin Oncol. 2019;37:212.
Zhao H, Howard LE, De Hoedt A, Terris MK, Amling CL, Kane CJ, et al. Racial discrepancies in overall survival among men treated with (223)Radium. J Urol. 2020;203:331–7.
Dai D, Han S, Li L, Guo Y, Wei Y, Jin H, et al. Anemia is associated with poor outcomes of metastatic castration-resistant prostate cancer, a systematic review and meta-analysis. Am J Transl Res. 2018;10:3877–86.
Ramalingam S, Humeniuk MS, Hu R, Rasmussen J, Healy P, Wu Y, et al. Prostate-specific antigen response in black and white patients treated with abiraterone acetate for metastatic castrate-resistant prostate cancer. Urol Oncol. 2017;35:418–24.
Edwards A, Hammond HA, Jin L, Caskey CT, Chakraborty R. Genetic variation at five trimeric and tetrameric tandem repeat loci in four human population groups. Genomics. 1992;12:241–53.
Karakas C, Wang C, Deng F, Huang H, Wang D, Lee P. Molecular mechanisms involving prostate cancer racial disparity. Am J Clin Exp Urol. 2017;5:34–48.
O’Donnell PH, Dolan ME. Cancer pharmacoethnicity: ethnic differences in susceptibility to the effects of chemotherapy. Clin Cancer Res. 2009;15:4806–14.
Lopez RFA, Goel S, Peeke S, Sharma J, Shenoy N. Genomic profiling of prostate cancer at a diverse academic center. J Clin Oncol. 2020;38; abstr. 64.
Ladoire S, Eymard JC, Zanetta S, Mignot G, Martin E, Kermarrec I, et al. Metronomic oral cyclophosphamide prednisolone chemotherapy is an effective treatment for metastatic hormone-refractory prostate cancer after docetaxel failure. Anticancer Res. 2010;30:4317–23.
Shamash J, Jacob J, Agrawal S, Powles T, Mutsvangwa K, Wilson P, et al. Whole blood stem cell reinfusion and escalated dose melphalan in castration-resistant prostate cancer: a phase 1 study. Clin Cancer Res. 2012;18:2352–9.
Shamash J, Dancey G, Barlow C, Wilson P, Ansell W, Oliver RT. Chlorambucil and lomustine (CL56) in absolute hormone refractory prostate cancer: re-induction of endocrine sensitivity an unexpected finding. Br J Cancer. 2005;92:36–40.
Belderbos BPS, de Wit R, Hoop EO, Nieuweboer A, Hamberg P, van Alphen RJ, et al. Prognostic factors in men with metastatic castration-resistant prostate cancer treated with cabazitaxel. Oncotarget. 2017;8:106468–74.
Halabi S, Small EJ, Kantoff PW, Kattan MW, Kaplan EB, Dawson NA, et al. Prognostic model for predicting survival in men with hormone-refractory metastatic prostate cancer. J Clin Oncol. 2003;21:1232–7.
Putt M, Long JA, Montagnet C, Silber JH, Chang VW, Kaijun L, et al. Racial differences in the impact of comorbidities on survival among elderly men with prostate cancer. Med Care Res Rev. 2009;66:409–35.
Norman G, Dean ME, Langley RE, Hodges ZC, Ritchie G, Parmar MK, et al. Parenteral oestrogen in the treatment of prostate cancer: a systematic review. Br J Cancer. 2008;98:697–707.
Venkitaraman R, Thomas K, Huddart RA, Horwich A, Dearnaley DP, Parker CC. Efficacy of low-dose dexamethasone in castration-refractory prostate cancer. BJU Int. 2008;101:440–3.
Acknowledgements
This work uses data that have been provided by patients and collected by the NHS as part of their care and support. The data are collated, maintained, and quality assured by the National Cancer Registration and Analysis Service, which is part of Public Health England (PHE).
Funding
No funding was received specifically for this project. KN is currently funded by a Cancer Research UK Clinical Research Training Fellowship (Award Number 549580).
Author information
Authors and Affiliations
Contributions
Conception and design: KM, LH, and JS. Acquisition of data: KN, PW, and JS. Analysis and interpretation of data: KN, PW, and JS. Drafting of the manuscript: KN and JS. Critical revision of the manuscript for important intellectual content: KN, KM, LH, and JS. Statistical analysis: KN and PW. Supervision: JS.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical statement
Patient outcomes are regularly reviewed in our hospital Trust consistent with the NHS Clinical Governance Framework. In accordance with criteria outlined by the Health Research Authority, NHS Research Ethics Committee approval was not required for this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Ng, K., Wilson, P., Mutsvangwa, K. et al. Overall survival of black and white men with metastatic castration-resistant prostate cancer (mCRPC): a 20-year retrospective analysis in the largest healthcare trust in England. Prostate Cancer Prostatic Dis 24, 718–724 (2021). https://doi.org/10.1038/s41391-020-00316-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41391-020-00316-x
This article is cited by
-
The impact of race on survival in metastatic prostate cancer: a systematic literature review
Prostate Cancer and Prostatic Diseases (2023)
-
Genetic and biological drivers of prostate cancer disparities in Black men
Nature Reviews Urology (2023)
-
From molecular mechanisms of prostate cancer to translational applications: based on multi-omics fusion analysis and intelligent medicine
Health Information Science and Systems (2023)
-
Overall survival and prognostic factors prostate cancer in Kurdistan Province-Iran: a population-based study (2011-2018)
BMC Cancer (2021)