Abstract
Background
Although previous studies have shown a decreased incidence of prostate cancer in men with HIV/AIDS, the consensus has not been reached. Our aim is to conduct a systematic review and meta-analysis to assess the risk of prostate cancer among people with HIV/AIDS.
Methods
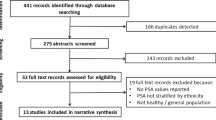
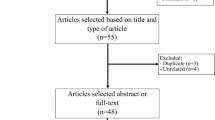
We systematically searched PubMed, Web of Science, Embase, and Cochrane Library until March 2020. Cohort studies were included if they compared the prostate cancer risk between people with HIV/AIDS and uninfected controls or the general population. The summary standardized incidence ratio (SIR) and 95% confidence interval (CI) were calculated using a random-effects model.
Results
A total of 27 studies were included for analysis, with more than 2780 males with HIV/AIDS developing prostate cancer. The results showed that HIV infection was associated with a decreased risk of prostate cancer incidence (SIR, 0.76; 95% CI, 0.64–0.91; P = 0.003), with significant heterogeneity (P < 0.001; I2 = 91.6%). A range of sensitivity analyzes did not significantly change the results.
Conclusions
Our study shows that people with HIV/AIDS have a lower incidence of prostate cancer compared with the general population. However, significant heterogeneity exists among the included studies. Further prospective studies with better designs are needed to elucidate the association between HIV infection and prostate cancer.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
World Health Organization. Global Health Observatory data repository 2019. https://www.who.int/hiv/data/en/.
Robbins HA, Pfeiffer RM, Shiels MS, Li J, Hall HI, Engels EA. Excess cancers among HIV-infected people in the United States. J Natl Cancer Inst. 2015;107:dju503.
Silverberg MJ, Lau B, Achenbach CJ, Jing Y, Althoff KN, D’Souza G, et al. Cumulative incidence of cancer among persons with HIV in North America: a cohort study. Ann Intern Med. 2015;163:507–18.
Park LS, Tate JP, Sigel K, Rimland D, Crothers K, Gibert C, et al. Time trends in cancer incidence in persons living with HIV/AIDS in the antiretroviral therapy era: 1997–2012. AIDS. 2016;30:1795–806.
Shiels MS, Cole SR, Kirk GD, Poole C. A meta-analysis of the incidence of non-AIDS cancers in HIV-infected individuals. J Acquir Immune Defic Syndr. 2009;52:611–22.
Grulich AE, van Leeuwen MT, Falster MO, Vajdic CM. Incidence of cancers in people with HIV/AIDS compared with immunosuppressed transplant recipients: a meta-analysis. Lancet. 2007;370:59–67.
Dal Maso L, Polesel J, Serraino D, Lise M, Piselli P, Falcini F, et al. Pattern of cancer risk in persons with AIDS in Italy in the HAART era. Br J Cancer. 2009;100:840–7.
Patel P, Hanson DL, Sullivan PS, Novak RM, Moorman AC, Tong TC, et al. Incidence of types of cancer among HIV-infected persons compared with the general population in the United States, 1992–2003. Ann Intern Med. 2008;148:728–36.
Herida M, Mary-Krause M, Kaphan R, Cadranel J, Poizot-Martin I, Rabaud C, et al. Incidence of non-AIDS-defining cancers before and during the highly active antiretroviral therapy era in a cohort of human immunodeficiency virus-infected patients. J Clin Oncol. 2003;21:3447–53.
Gallagher B, Wang Z, Schymura MJ, Kahn A, Fordyce EJ. Cancer incidence in New York State acquired immunodeficiency syndrome patients. Am J Epidemiol. 2001;154:544–56.
Wunder DM, Bersinger NA, Fux CA, Mueller NJ, Hirschel B, Cavassini M, et al. Hypogonadism in HIV-1-infected men is common and does not resolve during antiretroviral therapy. Antivir Ther. 2007;12:261–5.
Dobs AS, Few WL 3rd, Blackman MR, Harman SM, Hoover DR, Graham NM. Serum hormones in men with human immunodeficiency virus-associated wasting. J Clin Endocrinol Metab. 1996;81:4108–12.
Carlini F, Ridolfi B, Molinari A, Parisi C, Bozzuto G, Toccacieli L, et al. The reverse transcription inhibitor abacavir shows anticancer activity in prostate cancer cell lines. PLoS ONE. 2010;5:e14221.
Bellisai C, Sciamanna I, Rovella P, Giovannini D, Baranzini M, Pugliese GM, et al. Reverse transcriptase inhibitors promote the remodelling of nuclear architecture and induce autophagy in prostate cancer cells. Cancer Lett. 2020;478:133–45.
Godbole SV, Nandy K, Gauniyal M, Nalawade P, Sane S, Koyande S, et al. HIV and cancer registry linkage identifies a substantial burden of cancers in persons with HIV in India. Medicine. 2016;95:e4850.
Chen M, Jen I, Chen Y-H, Lin M-W, Bhatia K, Sharp GB, et al. Cancer incidence in a Nationwide HIV/AIDS patient cohort in Taiwan in 1998-2009. J Acquir Immune Defic Syndr. 2014;65:463–72.
Mbulaiteye SM, Katabira ET, Wabinga H, Parkin DM, Virgo P, Ochai R, et al. Spectrum of cancers among HIV-infected persons in Africa: the Uganda AIDS-Cancer Registry Match Study. Int J Cancer. 2006;118:985–90.
Serraino D, Boschini A, Carrieri P, Pradier C, Dorrucci M, Dal Maso L, et al. Cancer risk among men with, or at risk of, HIV infection in southern Europe. AIDS. 2000;14:553–9.
Tanaka LF, MRDO Latorre, Gutierrez EB, Curado MP, Froeschl G, Heumann C, et al. Risk for cancer among people living with AIDS, 1997-2012: the Sao Paulo AIDS-cancer linkage study. Eur J Cancer Prev. 2018;27:411–7.
Hessol NA, Whittemore H, Vittinghoff E, Hsu LC, Ma D, Scheer S, et al. Incidence of first and second primary cancers diagnosed among people with HIV, 1985–2013: a population-based, registry linkage study. Lancet HIV. 2018;5:e647–55.
Dutta A, Uno H, Holman A, Lorenz DR, Gabuzda D. Racial differences in prostate cancer risk in young HIV-positive and HIV-negative men: a prospective cohort study. Cancer Causes Control. 2017;28:767–77.
Yanik EL, Katki HA, Engels EA. Cancer risk among the HIV-infected elderly in the United States. AIDS. 2016;30:1663–8.
Lee JY, Dhakal I, Casper C, Noy A, Palefsky JM, Haigentz M, et al. Risk of cancer among commercially insured HIV-infected adults on antiretroviral therapy. J Cancer Epidemiol. 2016;2016:2138259.
Raffetti E, Albini L, Gotti D, Segala D, Maggiolo F, di Filippo E, et al. Cancer incidence and mortality for all causes in HIV-infected patients over a quarter century: a multicentre cohort study. BMC Public Health. 2015;15:235.
Castilho JL, Luz PM, Shepherd BE, Turner M, Ribeiro SR, Bebawy SS, et al. HIV and cancer: a comparative retrospective study of Brazilian and US clinical cohorts. Infect Agents Cancer. 2015;10:4.
Marcus JL, Chao CR, Leyden WA, Xu L, Klein DB, Horberg MA, et al. Prostate cancer incidence and prostate-specific antigen testing among HIV-positive and HIV-negative men. J Acquir Immune Defic Syndr. 2014;66:495–502.
Akarolo-Anthony SN, Maso LD, Igbinoba F, Mbulaiteye SM, Adebamowo CA. Cancer burden among HIV-positive persons in Nigeria: preliminary findings from the Nigerian AIDS-cancer match study. Infect Agents Cancer. 2014;9:1.
Albini L, Calabresi A, Gotti D, Ferraresi A, Festa A, Donato F, et al. Burden of non-AIDS-defining and non-virus-related cancers among HIV-infected patients in the combined antiretroviral therapy era. AIDS Res Hum Retrovir. 2013;29:1097–104.
Franceschi S, Lise M, Clifford GM, Rickenbach M, Levi F, Maspoli M, et al. Changing patterns of cancer incidence in the early- and late-HAART periods: the Swiss HIV Cohort Study. Br J Cancer. 2010;103:416–22.
Coghill AE, Engels EA, Schymura MJ, Mahale P, Shiels MS. Risk of breast, prostate, and colorectal cancer diagnoses among HIV-infected individuals in the United States. J Natl Cancer Inst. 2018;110:959–66.
Shiels MS, Goedert JJ, Moore RD, Platz EA, Engels EA. Reduced risk of prostate cancer in US men with AIDS. Cancer Epidemiol Biomark Prev. 2010;19:2910–5.
Moher D, Liberati A, Tetzlaff J, Altman DG. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med. 2009;151:264–9.
Kim J, Bang Y, Lee WJ. Living near nuclear power plants and thyroid cancer risk: a systematic review and meta-analysis. Environ Int. 2016;87:42–8.
Franzetti M, Adorni F, Parravicini C, Vergani B, Antinori S, Milazzo L, et al. Trends and predictors of non-AIDS-defining cancers in men and women with HIV infection: a single-institution retrospective study before and after the introduction of HAART. J Acquir Immune Defic Syndr. 2013;62:414–20.
Rothman KJ, Boice HD, Austin H. Epidemiologic analysis with a programmable calculator. Boston, Massachusetts, USA: Epidemiology Resources, Incorporated; 1982.
van Leeuwen MT, Vajdic CM, Middleton MG, McDonald AM, Law M, Kaldor JM, et al. Continuing declines in some but not all HIV-associated cancers in Australia after widespread use of antiretroviral therapy. AIDS. 2009;23:2183–90.
DerSimonian R, Laird N. Meta-analysis in clinical trials. Control Clin Trials. 1986;7:177–88.
Higgins JP, Thompson SG, Deeks JJ, Altman DG. Measuring inconsistency in meta-analyses. BMJ. 2003;327:557–60.
Romanowski K, Baumann B, Basham CA, Ahmad Khan F, Fox GJ, Johnston JC. Long-term all-cause mortality in people treated for tuberculosis: a systematic review and meta-analysis. Lancet Infect Dis. 2019;19:1129–37.
Patsopoulos NA, Evangelou E, Ioannidis JP. Sensitivity of between-study heterogeneity in meta-analysis: proposed metrics and empirical evaluation. Int J Epidemiol. 2008;37:1148–57.
Newnham A, Harris J, Evans HS, Evans BG, Møller H. The risk of cancer in HIV-infected people in southeast England: a cohort study. Br J Cancer. 2005;92:194–200.
Long JL, Engels EA, Moore RD, Gebo KA. Incidence and outcomes of malignancy in the HAART era in an urban cohort of HIV-infected individuals. AIDS. 2008;22:489–96.
Helleberg M, Gerstoft J, Afzal S, Kronborg G, Larsen CS, Pedersen C, et al. Risk of cancer among HIV-infected individuals compared to the background population: impact of smoking and HIV. AIDS. 2014;28:1499–508.
Legarth R, Omland LH, Dalton SO, Kronborg G, Larsen CS, Pedersen C, et al. Association between educational level and risk of cancer in HIV-infected individuals and the background population: population-based cohort study 1995-2011. J Infect Dis. 2015;212:1552–62.
Zlotorzynska M, Spaulding AC, Messina LC, Coker D, Ward K, Easley K, et al. Retrospective cohort study of cancer incidence and mortality by HIV status in a Georgia, USA, prisoner cohort during the HAART era. BMJ Open. 2016;6:e009778.
Bender Ignacio R, Ghadrshenas M, Low D, Orem J, Casper C, Phipps W. HIV status and associated clinical characteristics among adult patients with cancer at the Uganda Cancer Institute. J Glob Oncol. 2018;4:1–10.
Sitas F, Pacella-Norman R, Carrara H, Patel M, Ruff P, Sur R, et al. The spectrum of HIV-1 related cancers in South Africa. Int J Cancer. 2000;88:489–92.
Hsiao W, Anastasia K, Hall J, Goodman M, Rimland D, Ritenour CWM, et al. Association between HIV status and positive prostate biopsy in a study of US veterans. Sci World J. 2009;9:102–8.
Dhokotera T, Bohlius J, Spoerri A, Egger M, Ncayiyana J, Olago V, et al. The burden of cancers associated with HIV in the South African public health sector, 2004-2014: a record linkage study. Infect Agents Cancer. 2019;14:12.
Mpunga T, Znaor A, Uwizeye FR, Uwase A, Munyanshongore C, Franceschi S, et al. A case-control study of HIV infection and cancer in the era of antiretroviral therapy in Rwanda. Int J Cancer. 2018;143:1348–55.
Dal Maso L, Zanetti R, Orengo MA, Tagliabue G, Guzzinati S, Cavallieri F, et al. Methodological issues and first results of a record linkage between AIDS and Cancer Registries in Italy. Epidemiol Prev. 2000;24:109–16.
Mosthaf FA, Hanhoff NJ, Goetzenich A, Wolf E, Knechten H. High incidence of non-AIDS-defined cancers among HIV-infected patients in Germany: analysis of data collected over a period of 3 years. Dtsch Med Wochenschr. 2006;131:1849–52.
García-Abellán J, Del Río L, García JA, Padilla S, Vivancos MJ, Del Romero J, et al. Risk of cancer in HIV-infected patients in Spain, 2004-2015. The CoRIS cohort study. Enferm Infecc Microbiol Clin. 2019;37:502–8.
Canas-Ruano E, Martin-Castillo M, Raventos B, Burgos J, Curran A, Navarro J, et al. Incidence of malignancy in a Spanish cohort of patients infected by the human immunodeficiency virus. Med Clin. 2020. https://doi.org/10.1016/j.medcli.2019.12.001 [Epub ahead of print].
Collaborative Group on AIDS Incubation and HIV Survival including the CASCADE EU Concerted Action. Time from HIV-1 seroconversion to AIDS and death before widespread use of highly-active antiretroviral therapy: a collaborative re-analysis. Lancet. 2000;355:1131–7.
Shiels MS, Pfeiffer RM, Engels EA. Age at cancer diagnosis among persons with AIDS in the United States. Ann Intern Med. 2010;153:452–60.
Silverberg MJ, Chao C, Leyden WA, Xu L, Horberg MA, Klein D, et al. HIV infection, immunodeficiency, viral replication, and the risk of cancer. Cancer Epidemiol Biomark Prev. 2011;20:2551–9.
Hernández-Ramírez RU, Shiels MS, Dubrow R, Engels EA. Cancer risk in HIV-infected people in the USA from 1996 to 2012: a population-based, registry-linkage study. Lancet HIV. 2017;4:e495–504.
Dal Maso L, Franceschi S, Polesel J, Braga C, Piselli P, Crocetti E, et al. Risk of cancer in persons with AIDS in Italy, 1985-1998. Br J Cancer. 2003;89:94–100.
Simard EP, Pfeiffer RM, Engels EA. Spectrum of cancer risk late after AIDS onset in the United States. Arch Intern Med. 2010;170:1337–45.
Powles T, Robinson D, Stebbing J, Shamash J, Nelson M, Gazzard B, et al. Highly active antiretroviral therapy and the incidence of non-AIDS-defining cancers in people with HIV infection. J Clin Oncol. 2009;27:884–90.
Silverberg MJ, Chao C, Leyden WA, Xu L, Tang B, Horberg MA, et al. HIV infection and the risk of cancers with and without a known infectious cause. AIDS. 2009;23:2337–45.
Engels EA, Pfeiffer RM, Fraumeni JF Jr, Kasiske BL, Israni AK, Snyder JJ, et al. Spectrum of cancer risk among US solid organ transplant recipients. JAMA. 2011;306:1891–901.
Carter HB, Albertsen PC, Barry MJ, Etzioni R, Freedland SJ, Greene KL, et al. Early detection of prostate cancer: AUA Guideline. J Urol. 2013;190:419–26.
May MT, Gompels M, Delpech V, Porter K, Orkin C, Kegg S, et al. Impact on life expectancy of HIV-1 positive individuals of CD4+ cell count and viral load response to antiretroviral therapy. AIDS. 2014;28:1193–202.
Biggar RJ, Kirby KA, Atkinson J, McNeel TS, Engels E. AIDS Cancer Match Study Group. Cancer risk in elderly persons with HIV/AIDS. J Acquir Immune Defic Syndr. 2004;36:861–8.
Suneja G, Shiels MS, Angulo R, Copeland GE, Gonsalves L, Hakenewerth AM, et al. Cancer treatment disparities in HIV-infected individuals in the United States. J Clin Oncol. 2014;32:2344–50.
Loeb S, Vellekoop A, Ahmed HU, Catto J, Emberton M, Nam R, et al. Systematic review of complications of prostate biopsy. Eur Urol. 2013;64:876–92.
Baggaley RF, Boily MC, White RG, Alary M. Risk of HIV-1 transmission for parenteral exposure and blood transfusion: a systematic review and meta-analysis. AIDS. 2006;20:805–12.
Vannappagari V, Nkhoma ET, Atashili J, Laurent SS, Zhao H. Prevalence, severity, and duration of thrombocytopenia among HIV patients in the era of highly active antiretroviral therapy. Platelets. 2011;22:611–8.
Massie CE, Lynch A, Ramos-Montoya A, Boren J, Stark R, Fazli L, et al. The androgen receptor fuels prostate cancer by regulating central metabolism and biosynthesis. Embo J. 2011;30:2719–33.
Crum NF, Furtek KJ, Olson PE, Amling CL, Wallace MR. A review of hypogonadism and erectile dysfunction among HIV-infected men during the pre- and post-HAART eras: diagnosis, pathogenesis, and management. AIDS Patient Care STDs. 2005;19:655–71.
Yang Y, Ikezoe T, Takeuchi T, Adachi Y, Ohtsuki Y, Takeuchi S, et al. HIV-1 protease inhibitor induces growth arrest and apoptosis of human prostate cancer LNCaP cells in vitro and in vivo in conjunction with blockade of androgen receptor STAT3 and AKT signaling. Cancer Sci. 2005;96:425–33.
Pajonk F, Himmelsbach J, Riess K, Sommer A, McBride WH. The human immunodeficiency virus (HIV)-1 protease inhibitor saquinavir inhibits proteasome function and causes apoptosis and radiosensitization in non-HIV-associated human cancer cells. Cancer Res. 2002;62:5230–5.
Chao C, Leyden WA, Xu L, Horberg MA, Klein D, Towner WJ, et al. Exposure to antiretroviral therapy and risk of cancer in HIV-infected persons. AIDS. 2012;26:2223–31.
Houédé N, Pulido M, Mourey L, Joly F, Ferrero JM, Bellera C, et al. A phase II trial evaluating the efficacy and safety of efavirenz in metastatic castration-resistant prostate cancer. Oncologist. 2014;19:1227–8.
Hessol NA, Ma D, Scheer S, Hsu LC, Schwarcz SK. Changing temporal trends in non-AIDS cancer mortality among people diagnosed with AIDS: San Francisco, California, 1996-2013. Cancer Epidemiol. 2018;52:20–7.
Coghill AE, Shiels MS, Suneja G, Engels EA. Elevated cancer-specific mortality among HIV-infected patients in the United States. J Clin Oncol. 2015;33:2376–83.
Coghill AE, Suneja G, Rositch AF, Shiels MS, Engels EA. HIV infection, cancer treatment regimens, and cancer outcomes among elderly adults in the United States. JAMA Oncol. 2019;5:e191742.
Rositch AF, Jiang S, Coghill AE, Suneja G, Engels EA. Disparities and determinants of cancer treatment in elderly Americans living with human immunodeficiency virus/AIDS. Clin Infect Dis. 2018;67:1904–11.
Acknowledgements
This work was supported by Sanming Project of Medicine in Shenzhen (grant number: SZSM201911015); Innovation Fund for Medical Sciences (CIFMS; grant number: 2016-I2M-2-004). The funders had no role in the study design, data collection, analysis and interpretation, or writing of the paper.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Sun, D., Cao, M., Li, H. et al. Risk of prostate cancer in men with HIV/AIDS: a systematic review and meta-analysis. Prostate Cancer Prostatic Dis 24, 24–34 (2021). https://doi.org/10.1038/s41391-020-00268-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41391-020-00268-2