Abstract
Objective
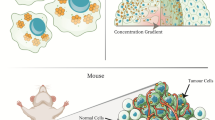
Focal therapy has emerged as a treatment option for low- to intermediate-risk localized prostate cancer (PCa) patients, to balance the risks for urinary and sexual morbidity of radical treatment with the psychological burden of active surveillance. In this context, we developed ST-4PC, an injectable, polymeric paste formulation containing docetaxel (dtx) and bicalutamide (bic) for image-guided focal therapy of PCa. The objective of this work was to evaluate the in vitro characteristics and in vivo toxicity and efficacy of ST-4PC.
Material and methods
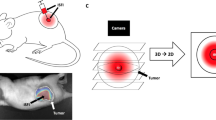
In vitro drug release was evaluated using high-performance liquid chromatography. In vivo toxicity of blank- and drug-loaded ST-4PC was assessed in mice and rats. Tumor growth inhibition was evaluated in LNCaP subcutaneous (s.c.) and LNCaP-luc orthotopic xenograft models. Using the s.c. model, mice were monitored weekly for weight loss, tumor volume (TV) and serum PSA. For the orthotopic model, mice were additionally monitored for bioluminescence as measure of tumor growth.
Results
ST-4PC demonstrated a sustained and steady release of incorporated drugs with 50% dtx and 20% bic being released after 14 days. While no systemic toxicity was observed, dose-dependent local side effects from dtx developed in the s.c. but not in the orthotopic model, illustrating the limitations of s.c. models for evaluating local cytotoxic therapy. In the s.c. model, 0.1%/4% and 0.25%/4% dtx/bic ST-4PC paste significantly reduced PSA progression, but did not have a significant inhibitory effect on TV. ST-4PC loaded with 1%/4% dtx/bic significantly reduced TV, serum PSA, and bioluminescence in the orthotopic xenograft model. Compared with drugs dissolved in DMSO, ST-4PC significantly delayed tumor growth.
Conclusion
Image-guided focal therapy using ST-4PC demonstrated promising inhibition of PSA progression and orthotopic tumor growth in vivo without significant toxicity, and warrants further clinical evaluation.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Ferlay J, Colombet M, Soerjomataram I, Mathers C, Parkin DM, Piñeros M, et al. Estimating the global cancer incidence and mortality in 2018: GLOBOCAN sources and methods. Int J Cancer. https://doi.org/10.1002/ijc.31937. Accessed 14 Nov 2018.
Ploussard G, Epstein JI, Montironi R, Carroll PR, Wirth M, Grimm M-O, et al. The contemporary concept of significant versus insignificant prostate cancer. Eur Urol. 2011;60:291–303.
Hamdy FC, Donovan JL, Lane JA, Mason M, Metcalfe C, Holding P, et al. 10-year outcomes after monitoring, surgery, or radiotherapy for localized prostate cancer. N. Engl J Med. 2016;375:1415–24.
Ahmed HU, Akin O, Coleman JA, Crane S, Emberton M, Goldenberg L, et al. Transatlantic Consensus Group on active surveillance and focal therapy for prostate cancer. BJU Int. 2012;109:1636–47.
Valerio M, Cerantola Y, Eggener SE, Lepor H, Polascik TJ, Villers A, et al. New and established technology in focal ablation of the prostate: a systematic review. Eur Urol. 2017;71:17–34.
Silvia Garcia-Barreras, Rafael Sanchez-Salas, Arjun Sivaraman, Eric Barret, Fernando Secin, Igor Nunes-Silva, et al. Comparative analysis of partial gland ablation and radical prostatectomy to treat low and intermediate risk prostate cancer: oncologic and functional outcomes. J Urol. 2018;199:140–6.
Bahn D, de Castro Abreu AL, Gill IS, Hung AJ, Silverman P, Gross ME, et al. Focal cryotherapy for clinically unilateral, low-intermediate risk prostate cancer in 73 men with a median follow-up of 3.7 years. Eur Urol. 2012;62:55–63.
Bass R, Fleshner N, Finelli A, Barkin J, Zhang L, Klotz L. Oncologic and functional outcomes of partial gland ablation with high intensity focused ultrasound for localized prostate cancer. J Urol. 2019;201:113–9.
von Hardenberg J, Westhoff N, Baumunk D, Hausmann D, Martini T, Marx A, et al. Prostate cancer treatment by the latest focal HIFU device with MRI/TRUS-fusion control biopsies: a prospective evaluation. Urol Oncol. 2018;36:401.e1–9.
Stein CA. Mechanisms of action of taxanes in prostate cancer. Semin Oncol. 1999;26(5 Suppl 17):3–7.
Kolvenbag GJCM, Blackledge GRP, Gotting‐Smith K. Bicalutamide (Casodex®) in the treatment of prostate cancer: history of clinical development. Prostate. 1998;34:61–72.
Sweeney CJ, Chen Y-H, Carducci M, Liu G, Jarrard DF, Eisenberger M, et al. Chemohormonal therapy in metastatic hormone-sensitive prostate cancer. N. Engl J Med. 2015;373:737–46.
James ND, Sydes MR, Clarke NW, Mason MD, Dearnaley DP, Spears MR, et al. Addition of docetaxel, zoledronic acid, or both to first-line long-term hormone therapy in prostate cancer (STAMPEDE): survival results from an adaptive, multiarm, multistage, platform randomised controlled trial. Lancet Lond Engl. 2016;387:1163–77.
Mitragotri S, Burke PA, Langer R. Overcoming the challenges in administering biopharmaceuticals: formulation and delivery strategies. Nat Rev Drug Disco. 2014;13:655–72.
Xu Y, Kim C-S, Saylor DM, Koo D. Polymer degradation and drug delivery in PLGA-based drug–polymer applications: a review of experiments and theories. J Biomed Mater Res B Appl Biomater. 2017;105:1692–716.
Aghabegi Moghanjoughi A, Khoshnevis D, Zarrabi A. A concise review on smart polymers for controlled drug release. Drug Deliv Transl Res. 2016;6:333–40.
Grudén S, Sandelin M, Rasanen V, Micke P, Hedeland M, Axén N, et al. Antitumoral effect and reduced systemic toxicity in mice after intra-tumoral injection of an in vivo solidifying calcium sulfate formulation with docetaxel. Eur J Pharm Biopharm. 2017;114:186–93.
Sheu M-T, Jhan H-J, Su C-Y, Chen L-C, Chang C-E, Liu D-Z, et al. Codelivery of doxorubicin-containing thermosensitive hydrogels incorporated with docetaxel-loaded mixed micelles enhances local cancer therapy. Colloids Surf B Biointerfaces. 2016;143:260–70.
Yamamoto Y, Yoshida M, Sato M, Sato K, Kikuchi S, Sugishita H, et al. Feasibility of tailored, selective and effective anticancer chemotherapy by direct injection of docetaxel-loaded immunoliposomes into Her2/neu positive gastric tumor xenografts. Int J Oncol. 2011;38:33–9.
Yoo GH, Subramanian G, Boinpally RR, Iskander A, Shehadeh N, Oliver J, et al. An in vivo evaluation of docetaxel delivered intratumorally in head and neck squamous cell carcinoma. Arch Otolaryngol Neck Surg. 2005;131:418–29.
Anderson JM. Biological responses to materials. Annu Rev Mater Res. 2001;31:81–110.
Jackson JK, Gleave ME, Yago V, Beraldi E, Hunter WL, Burt HM. The suppression of human prostate tumor growth in mice by the intratumoral injection of a slow-release polymeric paste formulation of paclitaxel. Cancer Res. 2000;60:4146–51.
Potten CS, Saffhill R, Maibach HI. Measurement of the transit time for cells through the epidermis and stratum corneum of the mouse and guinea-pig. Cell Tissue Kinet. 1987;20:461–72.
Kenmotsu H, Tanigawara Y. Pharmacokinetics, dynamics and toxicity of docetaxel: why the Japanese dose differs from the Western dose. Cancer Sci. 2015;106:497–504.
Denis L, Mahler C. Pharmacodynamics and pharmacokinetics of bicalutamide: defining an active dosing regimen. Urology. 1996;(47 Suppl 1):26–8.
Tammela TL, Häggman M, Ladjevardi S, Taari K, Isotalo T, Lennernäs H, et al. an intraprostatic modified release formulation of antiandrogen 2-hydroxyflutamide for localized prostate cancer. J Urol. 2017;198:1333–9.
Shanmugabavan Y, Bass E, Hulme A, Freeman A, Brew-Graves C, Potyka I, et al. Intra-prostatic injection of PRX302 to focally ablate clinically significant prostate cancer: an open label, phase 2a study. Eur Urol Suppl. 2017;16:e1308–9.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
University of British Columbia has granted patents on the polymer paste formulation in ST-4PC, listing MEG, JKJ, VS, and CK as co-inventors, which have been outlicensed to Sustained Therapeutics, an early-stage biotech company founded by MEG.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Kesch, C., Schmitt, V., Bidnur, S. et al. A polymeric paste-drug formulation for intratumoral treatment of prostate cancer. Prostate Cancer Prostatic Dis 23, 324–332 (2020). https://doi.org/10.1038/s41391-019-0190-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41391-019-0190-x
This article is cited by
-
A polymeric paste for intratumoural therapy
Nature Reviews Urology (2020)