Abstract
Background
Obesity has been proposed as a risk factor for prostate cancer (PCa). In obesity, serum levels of the appetite-regulating hormones—leptin, adiponectin, and ghrelin—become deregulated.
Objective
To explore whether serum levels of appetite-regulating hormones associate with the incidence of PCa, the incidence of advanced disease, or PCa-specific mortality.
Methods
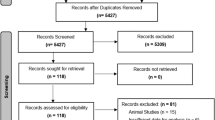
PRISMA guidelines were followed. A systematic search for relevant articles published until March 2019 was performed using the databases PubMed, EMBASE, and Web of Science. Observational studies with data on serum levels of leptin, adiponectin, or ghrelin and PCa outcome were included. Meta-analysis was used to combine risk estimates. Meta-relative risks (mRRs) were calculated using random effects models. When available, raw data was pooled. Publication bias was assessed by funnel plot and Begg’s test.
Results
Thirty-five studies were eligible for inclusion. The qualitative analysis indicated that leptin was not consistently associated with any PCa outcome, although several cohorts reported decreased adiponectin levels in men who later developed advanced PCa. Based on the meta-analysis, there was no significant effect of leptin on PCa incidence (mRR = 0.93 (95% CI 0.75–1.16), p = 0.52) or advanced PCa (mRR = 0.90 (95% CI 0.74–1.10), p = 0.30). There were insufficient studies to estimate the mRR of PCa incidence for men with the highest levels of adiponectin. The combined risk of advanced PCa for men with the highest levels of adiponectin was reduced but did not reach significance (mRR = 0.81 (95% CI 0.61–1.08), p = 0.15).
Conclusions
The current evidence does not suggest an association between leptin and PCa outcome. However, there may be an inverse association between adiponectin and the incidence of advanced PCa that should be investigated by further studies. Serum ghrelin has not been largely investigated.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Calle EE, Kaaks R. Overweight, obesity and cancer: epidemiological evidence and proposed mechanisms. Nat Rev Cancer. 2004;4:579–91.
Freedland SJ, Platz EA. Obesity and prostate cancer: making sense out of apparently conflicting data. Epidemiol Rev. 2007;29:88–97.
Lauby-Secretan B, Scoccianti C, Loomis D, Grosse Y, Bianchini F, Straif K. Body Fatness and Cancer — Viewpoint of the IARC Working Group. N Engl J Med. 2016;375:794–8.
Mottet, N. et al. ‘EAU-ESTRO-SIOG Guidelines on Prostate Cancer. Part 1: Screening, Diagnosis, and Local Treatment with Curative Intent’, Eur Urol, 2017;71:618–29. https://doi.org/10.1016/j.eururo.2016.08.003.
World Cancer Research Fund International. Prostate cancer | How diet, nutrition and physical activity affect prostate cancer. 2014 [cited 2019 Mar 19]. https://www.wcrf.org/dietandcancer/prostate-cancer
Park J, Morley TS, Kim M, Clegg DJ, Scherer PE. Obesity and cancer--mechanisms underlying tumour progression and recurrence. Nat Rev Endocrinol. 2014;10:455–65.
Vansaun MN. Molecular pathways: adiponectin and leptin signaling in cancer. Clin Cancer Res. 2013;19:1926–32.
Kubota N, Yano W, Kubota T, Yamauchi T, Itoh S, Kumagai H, et al. Adiponectin stimulates AMP-activated protein kinase in the hypothalamus and increases food intake. Cell Metab. 2007;6:55–68.
Tschöp M, Weyer C, Tataranni PA, Devanarayan V, Ravussin E, Heiman ML. Circulating ghrelin levels are decreased in human obesity. Diabetes. 2001;50:707–9.
Alshaker H, Sacco K, Alfraidi A, Muhammad A, Winkler M, Pchejetski D. Leptin signalling, obesity and prostate cancer: Molecular and clinical perspective on the old dilemma. Oncotarget. 2015;6:35556–63.
Lin T-C, Hsiao M. Ghrelin and cancer progression. Biochim Biophys Acta - Rev Cancer. 2017;1868:51–7.
Muppala S, Konduru SKP, Merchant N, Ramsoondar J, Rampersad CK, Rajitha B, et al. Adiponectin: Its role in obesity-associated colon and prostate cancers. Crit Rev Oncol Hematol. 2017;116:125–33.
Hu M-B, Xu H, Hu J-M, Zhu W-H, Yang T, Jiang H-W, et al. Genetic polymorphisms in leptin, adiponectin and their receptors affect risk and aggressiveness of prostate cancer: evidence from a meta-analysis and pooled-review. Oncotarget. 2016;7:81049–61.
Moher D, Liberati A, Tetzlaff J, Altman DG, Altman D. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;6:e1000097.
Michalakis K, Williams CJ, Mitsiades N, Blakeman J, Balafouta-Tselenis S, Giannopoulos A, et al. Serum adiponectin concentrations and tissue expression of adiponectin receptors are reduced in patients with prostate cancer: a case control study. Cancer Epidemiol Biomark Prev. 2007;16:308–13.
Baillargeon J, Platz EA, Rose DP, Pollock BH, Ankerst DP, Haffner S, et al. Obesity, adipokines, and prostate cancer in a prospective population-based study. Cancer Epidemiol Biomark Prev. 2006;15:1331–5.
Serretta V, Abrate A, Siracusano S, Gesolfo CS, Vella M, Di Maida F, et al. Clinical and biochemical markers of visceral adipose tissue activity: body mass index, visceral adiposity index, leptin, adiponectin, and matrix metalloproteinase-3. Correlation with Gleason patterns 4 and 5 at prostate biopsy. Urol Ann. 2018;10:280–6.
DerSimonian R, Laird N. Meta-analysis in clinical trials. Control Clin Trials. 1986;7:177–88.
Glass AS, Cary KC, Cooperberg MR. Risk-based prostate cancer screening: who and how? Curr Urol Rep. 2013;14:192–8.
Higgins JPT, Thompson SG. Quantifying heterogeneity in a meta-analysis. Stat Med. 2002;21:1539–58.
Begg CB, Mazumdar M. Operating characteristics of a rank correlation test for publication bias. Biometrics. 1994;50:1088–101.
Copenhagen: The Nordic Cochrane Centre TCC. Review Manager (RevMan) [Computer program]. Version 5.3. 2014.
Hsing AW, Chua S, Gao YT, Gentzschein E, Chang L, Deng J, et al. Prostate cancer risk and serum levels of insulin and leptin: a population-based study. J Natl Cancer Inst. 2001;93:783–9.
Lai GY, Giovannucci EL, Pollak MN, Peskoe SB, Stampfer MJ, Willett WC, et al. Association of C-peptide and leptin with prostate cancer incidence in the Health Professionals Follow-up Study. Cancer Causes Control. 2014;25:625–32.
Li HJ, Stampfer MJ, Mucci L, Rifai N, Qiu WL, Kurth T, et al. A 25-year prospective study of plasma adiponectin and leptin concentrations and prostate cancer risk and survival. Clin Chem. 2010;56:34–43.
Stattin P, Kaaks R, Johansson R, Gislefoss R, Söderberg S, Alfthan H, et al. Plasma leptin is not associated with prostate cancer risk. Cancer Epidemiol Biomark Prev. 2003;12:474–5.
Touvier M, Fezeu L, Ahluwalia N, Julia C, Charnaux N, Sutton A, et al. Association between pre-diagnostic biomarkers of inflammation and endothelial function and cancer risk: a nested case-control study. Am J Epidemiol. 2013;177:3–13.
Burton A, Martin RM, Holly J, Lane JA, Donovan JL, Hamdy FC, et al. Associations of adiponectin and leptin with stage and grade of PSA-detected prostate cancer: The ProtecT study. Cancer Causes Control. 2013;24:323–34.
Arisan ED, Arisan S, Atis G, Palavan-Unsal N, Ergenekon E. Serum adipocytokine levels in prostate cancer patients. Urol Int. 2009;82:203–8.
Gade-Andavolu R, Cone LA, Shu S, Morrow A, Kowshik B, Andavolu MVS. Molecular interactions of leptin and prostate cancer. Cancer J. 2006;12:201–6.
Grosman H, Fabre B, Lopez M, Scorticati C, Lopez Silva M, Mesch V, et al. Complex relationship between sex hormones, insulin resistance and leptin in men with and without prostatic disease. Aging Male. 2016;19:40–5.
Nishimura K, Soda T, Nakazawa S, Yamanaka K, Hirai T, Kishikawa H, et al. Serum adiponectin and leptin levels are useful markers for prostate cancer screening after adjustments for age, obesity-related factors, and prostate volume. Minerva Urol e Nefrol. 2012;64:199–208.
Saǧlam K, Aydur E, Yilmaz MI, Göktaş S. Leptin influences cellular differentiation and progression in prostate cancer. J Urol. 2003;169:1308–11.
Singh SK, Grifson JJ, Mavuduru RS, Agarwal MM, Mandal AK, Jha V. Serum leptin: a marker of prostate cancer irrespective of obesity. Cancer Biomark. 2010;7:11–5.
Tewari R, Rajender S, Natu SM, Goel A, Dalela D, Goel MM, et al. Significance of obesity markers and adipocytokines in high grade and high stage prostate cancer in North Indian men - A cross-sectional study. Cytokine. 2013;63:130–4.
Duarte, M. F. et al. ‘Clinical and metabolic implications of obesity in prostate cancer: is testosterone a missing link?’, The Aging Male, EPub ahead of print, 2018, p. 1–13. https://doi.org/10.1080/13685538.2018.1519695.
Fryczkowski M, Buldak RJ, Hejmo T, Kukla M, Zwirska-Korczala K. Circulating levels of omentin, leptin, VEGF, and HGF and their clinical relevance with PSA marker in prostate cancer. Dis Markers. 2018;2018:3852401.
Fontana CML, Maselli ME, Elizalde RFP, Monaco NAD, Recupero ALU, Laur JDL. Leptin increases prostate cancer aggressiveness. J Physiol Biochem. 2011;67:531–8.
Sieminska L, Borowski A, Marek B, Nowak M, Kajdaniuk D, Warakomski J, et al. Serum concentrations of adipokines in men with prostate cancer and benign prostate hyperplasia. Endokrynol Pol. 2018;69:120–7.
Medina EA, Shi XY, Grayson MH, Ankerst DP, Livi CB, Medina MV, et al. The Diagnostic value of Adiponectin multimers in healthy men undergoing screening for prostate cancer. Cancer Epidemiol Biomark Prev. 2014;23:309–15.
Wang Y, Lam KSL, Chan L, Chan KW, Lam JBB, Lam MC, et al. Post-translational modifications of the four conserved lysine residues within the collagenous domain of Adiponectin are required for the formation of its high molecular weight oligomeric complex. J Biol Chem. 2006;281:16391–400.
Fowke JH, Motley S, Dai Q, Concepcion R, Barocas DA. Association between biomarkers of obesity and risk of high-grade prostatic intraepithelial neoplasia and prostate cancer - Evidence of effect modification by prostate size. Cancer Lett. 2013;328:345–52.
Stevens VL, Jacobs EJ, Sun JZ, Gapstur SM. No association of plasma levels of Adiponectin and c-peptide with risk of aggressive prostate cancer in the cancer prevention study II nutrition cohort. Cancer Epidemiol Biomark Prev. 2014;23:890–2.
Sher DJ, Oh WK, Jacobus S, Regan MM, Lee GS, Mantzoros C. Relationship between serum adiponectin and prostate cancer grade. Prostate . 2008;68:1592–8.
Freedland SJ, Sokoll LJ, Platz EA, Mangold LA, Bruzek DJ, Mohr P, et al. Association between serum adiponectin, and pathological stage and grade in men undergoing radical prostatectomy. J Urol. 2005;174(4 Pt 1):1266–70.
Goktas S, Mahmut IY, Caglar K, Sonmez A, Kilic S, Bedir S. Prostate cancer and adiponectin. Urology. 2005;65:1168–72.
Grosman H, Fabre B, Mesch V, Lopez MA, Schreier L, Mazza O, et al. Lipoproteins, sex hormones and inflammatory markers in association with prostate cancer. Aging Male. 2010;13:87–92.
Housa D, Vernerová Z, Heráček J, Procházka B, Čechák P, Kuncová J, et al. Adiponectin as a potential marker of prostate cancer progression: Studies in organ-confined and locally advanced prostate cancer. Physiol Res. 2008;57:451–8.
Ikeda A, Nakagawa T, Kawai K, Onozawa M, Hayashi T, Matsushita Y, et al. Serum adiponectin concentration in 2,939 Japanese men undergoing screening for prostate cancer. Prostate Int. 2015;3:87–92.
Michalakis K, Venihaki M, Mantzoros C, Vazaiou A, Ilias I, Gryparis A, et al. In prostate cancer, low adiponectin levels are not associated with insulin resistance. Eur J Clin Invest. 2015;45:572–8.
Kang M, Byun SS, Lee SE, Hong SK. Clinical significance of serum adipokines according to body mass index in patients with clinically localized prostate cancer undergoing radical prostatectomy. World J Mens Health. 2018;36:57–65.
Malendowicz W, Ziolkowska A, Szyszka M, Kwias Z. Elevated blood active ghrelin and unaltered total ghrelin and obestatin concentrations in prostate carcinoma. Urol Int. 2009;83:471–5.
Hormaechea-Agulla D, Gahete MD, Jiménez-Vacas JM, Gómez-Gómez E, Ibáñez-Costa A, L-López F, et al. The oncogenic role of the In1-ghrelin splicing variant in prostate cancer aggressiveness. Mol Cancer. 2017;16:146.
Buschemeyer WC, Freedland SJ. Obesity and prostate cancer: epidemiology and clinical implications. Eur Urol. 2007;52:331–43.
Allott EH, Hursting SD. Obesity and cancer: mechanistic insights from transdisciplinary studies. Endocr Relat Cancer. 2015;22:R365–86.
Alfaqih MA, Allott EH, Hamilton RJ, Freeman MR, Freedland SJ. The current evidence on statin use and prostate cancer prevention: are we there yet? Nat Rev Urol. 2017;14:107–19.
Raval AD, Thakker D, Vyas A, Salkini M, Madhavan S, Sambamoorthi U. Impact of metformin on clinical outcomes among men with prostate cancer: a systematic review and meta-analysis. Prostate Cancer Prostatic Dis. 2015;18:110–21.
van Roermund JGH, Hinnen KA, Tolman CJ, Bol GH, Witjes JA. Bosch JLHR, et al. Periprostatic fat correlates with tumour aggressiveness in prostate cancer patients. BJU Int. 2011;107:1775–9.
Luque RM, Sampedro-Nuñez M, Gahete MD, Ramos-Levi A, Ibáñez-Costa A, Rivero-Cortés E, et al. In1-ghrelin, a splice variant of ghrelin gene, is associated with the evolution and aggressiveness of human neuroendocrine tumors: evidence from clinical, cellular and molecular parameters. Oncotarget. 2015;6:19619–33.
Ibáñez-Costa A, Gahete MD, Rivero-Cortés E, Rincón-Fernández D, Nelson R, Beltrán M, et al. In1-ghrelin splicing variant is overexpressed in pituitary adenomas and increases their aggressive features. Sci Rep. 2015;5:8714.
Gahete MD, Córdoba-Chacón J, Hergueta-Redondo M, Martínez-Fuentes AJ, Kineman RD, Moreno-Bueno G, et al. A Novel Human Ghrelin Variant (In1-Ghrelin) and Ghrelin-O-Acyltransferase Are Overexpressed in Breast Cancer: Potential Pathophysiological Relevance. Ulasov I, editor. PLoS ONE. 2011;6:e23302.
Seim I, Jeffery PL, de Amorim L, Walpole CM, Fung J, Whiteside EJ, et al. Ghrelin O-acyltransferase (GOAT) is expressed in prostate cancer tissues and cell lines and expression is differentially regulated in vitro by ghrelin. Reprod Biol Endocrinol. 2013;11:70.
Gómez-Gómez, E et al. ‘Plasma ghrelin O-acyltransferase (GOAT) enzyme levels: A novel non-invasive diagnosis tool for patients with significant prostate cancer’. J Cell Mol Med. John Wiley & Sons, Ltd (10.1111), 2018;22, p. 5688–97. https://doi.org/10.1111/jcmm.13845.
Thompson IM, Ankerst DP, Chi C, Goodman PJ, Tangen CM, Lucia MS, et al. Assessing prostate cancer risk: results from the prostate cancer prevention trial. J Natl Cancer Inst. 2006;98:529–34.
Brawley, OW ‘Prostate cancer epidemiology in the United States’, World J Urol 2012;30:195–200. https://doi.org/10.1007/s00345-012-0824-2.
Helpap B, Egevad L. Modified Gleason grading. An updated review. Histol Histopathol. 2009;24:661–6.
Gordetsky J, Epstein J. Grading of prostatic adenocarcinoma: current state and prognostic implications.
Kryvenko ON, Epstein JI. Prostate Cancer Grading A Decade After the 2005 Modified Gleason Grading System.
Allott EH, Masko EM, Freedland SJ. Obesity and prostate cancer: weighing the evidence. Eur Urol. 2013;63:800–9.
Capoun O, Soukup V, Kalousová M, Sobotka R, Pešl M, Zima T, et al. Diagnostic Importance of Selected Protein Serum Markers in the Primary Diagnostics of Prostate Cancer. Urol Int. 2015;95:429–35.
Medina EA, Shi X, Grayson MH, Ankerst DP, Livi CB, Medina MV, et al. The Diagnostic Value of Adiponectin Multimers in Healthy Men Undergoing Screening for Prostate Cancer. Cancer Epidemiol Prev. 2014;23:309–15.
Stattin P, Söderberg S, Hallmans G, Bylund A, Kaaks R, Stenman U-H, et al. Leptin Is Associated with Increased Prostate Cancer Risk: A Nested Case-Referent Study. J Clin Endocrinol Metab. 2001;86:1341–5.
Chang S, Hursting SD, Contois JH, Strom SS, Yamamura Y, Babaian RJ, et al. Leptin and prostate cancer. Prostate. 2001;46:62–67.
Housa D, et al. ‘Adiponectin as a potential marker of prostate cancer progression: Studies in organ-confined and locally advanced prostate cancer’. Physiol Res. 2008;57:451–8.
Lagiou P, Signorello LB, Trichopoulos D, Tzonou A, Trichopoulou A, Mantzoros CS. Leptin in relation to prostate cancer and benign prostatic hyperplasia. Int J Cancer. 1998;76:25–28.
Sieminska L, et al. ‘Serum concentrations of adipokines in men with prostate cancer and benign prostate hyperplasia’. Endokrynol Pol. 2018;69:120–7.
Touvier M, Fezeu L, Ahluwalia N, Julia C, Charnaux N, Sutton A, et al. Association Between Prediagnostic Biomarkers of Inflammation and Endothelial Function and Cancer Risk: A Nested Case-Control Study. Am J Epidemiol. 2012;177:3–13.
Stocks T, Lukanova A, Rinaldi S, Biessy C, Dossus L, Lindahl B, et al. Insulin resistance is inversely related to prostate cancer: A prospective study in Northern Sweden. Int J Cancer. 2007;120:2678–86.
Disclaimer
Where authors are identified as personnel of the International Agency for Research on Cancer / World Health Organization, the authors alone are responsible for the views expressed in this article and they do not necessarily represent the decisions, policy or views of the International Agency for Research on Cancer / World Health Organization.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Angel, C.Z., Iguacel, I., Mullee, A. et al. Appetite-regulating hormones—leptin, adiponectin and ghrelin—and the development of prostate cancer: a systematic review and exploratory meta-analysis. Prostate Cancer Prostatic Dis 23, 11–23 (2020). https://doi.org/10.1038/s41391-019-0154-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41391-019-0154-1