Abstract
Background
To evaluate efficacy and morbidity prospectively in a contemporary multi-institutional salvage radical prostatectomy (SRP) series.
Methods
Forty-one men were enrolled between 1997 and 2006, who suffered biopsy-proven recurrent prostate cancer (CaP) after receiving ≥ 60c Gy radiation as primary treatment for cT1–2NXM0 disease. Surgical morbidity, quality of life, biochemical progression-free survival (BPFS) and overall survival (OS) were evaluated.
Results
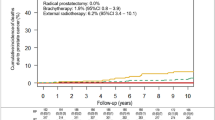
Twenty-four men had undergone external beam radiotherapy, 11 brachytherapy, and six both. Median time between radiation and SRP was 64 months. Median age at SRP was 64 years. Pathologic staging revealed 44% pT2, 54% pT3, and 3% pT4. Surgical margins were positive in 17 and 88% were pN0. Twenty-two percent required intraoperative blood transfusion. Three rectal and one obturator nerve injuries occurred. Seventeen of 38 evaluable patients (45%) had urinary incontinence ( ≥ 3 pads/day) prior to SRP; 88% reported urinary incontinence at 6 months, 85% at 12 months, 63% at 24 months after SRP. Furthermore, 37% of men reported impotence prior to SRP; 78% reported impotence at 6 months, 82% at 12 months, and 44% at 24 months after SRP. The 2-, 5- and 10-year BPFS rates were 51, 39, and 33% respectively; the 2-, 5- and 10-year OS rates were 100, 89, and 52%, respectively, at median follow-up 91 months.
Conclusions
Modern surgical techniques continue to be associated with significant peri-operative complication rates. Nevertheless, SRP may benefit carefully selected patients through durable oncologic control
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Meng MV, Elkin EP, Latini DM, Duchane J, Carroll PR. Treatment of patients with high risk localized prostate cancer: results from cancer of the prostate strategic urological research endeavor (CaPSURE). J Urol. 2005;173:1557–61.
Cooperberg MR, Lubeck DP, Meng MV, Mehta SS, Carroll PR. The changing face of low-risk prostate cancer: trends in clinical presentation and primary management. J Clin Oncol. 2004;22:2141–9.
Kupelian PA, Buchsbaum JC, Patel C, Elshaikh M, Reddy CA, Zippe C et al. Impact of biochemical failure on overall survival after radiation therapy for localized prostate cancer in the PSA era. Int J Radiat Oncol Biol Phys. 2002;52:704–11.
Zelefsky MJ, Fuks Z, Hunt M, Lee HJ, Lombardi D, Ling CC et al. High dose radiation delivered by intensity modulated conformal radiotherapy improves the outcome of localized prostate cancer. J Urol. 2001;166:876–81.
Shipley WU, Thames HD, Sandler HM, Hanks GE, Zietman AL, Perez CA et al. Radiation therapy for clinically localized prostate cancer: a multi-institutional pooled analysis. JAMA. 1999;281:1598–604.
Zelefsky MJ, Chan H, Hunt M, Yamada Y, Shippy AM, Amols H. Long-term outcome of high dose intensity modulated radiation therapy for patients with clinically localized prostate cancer. J Urol. 2006;176:1415–9.
Pollack A, Zagars GK, Antolak JA, Kuban DA, Rosen II. Prostate biopsy status and PSA nadir level as early surrogates for treatment failure: analysis of a prostate cancer randomized radiation dose escalation trial. Int J Radiat Oncol Biol Phys. 2002;54:677–85.
Crook J, Malone S, Perry G, Bahadur Y, Robertson S, Abdolell M. Postradiotherapy prostate biopsies: what do they really mean? Results for 498 patients. Int J Radiat Oncol Biol Phys. 2000;48:355–67.
Borghede G, Aldenborg F, Wurzinger E, Johansson KA, Hedelin H. Analysis of the local control in lymph-node staged localized prostate cancer treated by external beam radiotherapy, assessed by digital rectal examination, serum prostate-specific antigen and biopsy. Br J Urol. 1997;80:247–55.
Holzman M, Carlton CE Jr, Scardino PT. The frequency and morbidity of local tumor recurrence after definitive radiotherapy for stage C prostate cancer. J Urol. 1991;146:1578–82.
Fuks Z, Leibel SA, Wallner KE, Begg CB, Fair WR, Anderson LL et al. The effect of local control on metastatic dissemination in carcinoma of the prostate: long-term results in patients treated with 125I implantation. Int J Radiat Oncol Biol Phys. 1991;21:537–47.
Brenner PC, Russo P, Wood DP, Morse MJ, Donat SM, Fair WR. Salvage radical prostatectomy in the management of locally recurrent prostate cancer after 125I implantation. Br J Urol. 1995;75:44–7.
Pontes JE, Montie J, Klein E, Huben R. Salvage surgery for radiation failure in prostate cancer. Cancer. 1993;71:976–80.
Ahlering TE, Lieskovsky G, Skinner DG. Salvage surgery plus androgen deprivation for radioresistant prostatic adenocarcinoma. J Urol. 1992;147:900–2.
Stein A, Smith RB, deKernion JB. Salvage radical prostatectomy after failure of curative radiotherapy for adenocarcinoma of prostate. Urology. 1992;40:197–200.
Rainwater LM, Zincke H. Radical prostatectomy after radiation therapy for cancer of the prostate: feasibility and prognosis. J Urol. 1988;140:1455–9.
Nguyen PL, D’Amico AV, Lee AK, Suh WW. Patient selection, cancer control, and complications after salvage local therapy for postradiation prostate-specific antigen failure: a systematic review of the literature. Cancer. 2007;110:1417–28.
Mitchell JM. Urologists’ use of intensity-modulated radiation therapy for prostate cancer. N Engl J Med. 2013;369:1629–37.
Chade DC, Shariat SF, Cronin AM, Savage CJ, Karnes RJ, Blute ML et al. Salvage radical prostatectomy for radiation-recurrent prostate cancer: a multi-institutional collaboration. Eur Urol. 2011;60:205–10.
Stephenson AJ, Eastham JA. Role of salvage radical prostatectomy for recurrent prostate cancer after radiation therapy. J Clin Oncol. 2005;23:8198–203.
Grossfeld GD, Li YP, PL DP, Carroll PR. Patterns of failure after primary local therapy for prostate cancer and rationale for secondary therapy. Urology. 2002;60:57–62. discussion62-3
Touma NJ, Izawa JI, Chin JL. Current status of local salvage therapies following radiation failure for prostate cancer. J Urol. 2005;173:373–9.
Ward JF, Sebo TJ, Blute ML, Zincke H. Salvage surgery for radiorecurrent prostate cancer: contemporary outcomes. J Urol. 2005;173:1156–60.
Stephenson AJ, Scardino PT, Bianco FJ Jr, DiBlasio CJ, Fearn PA, Eastham JA. Morbidity and functional outcomes of salvage radical prostatectomy for locally recurrent prostate cancer after radiation therapy. J Urol. 2004;172:2239–43.
Bianco FJ Jr, Scardino PT, Stephenson AJ, Diblasio CJ, Fearn PA, Eastham JA. Long-term oncologic results of salvage radical prostatectomy for locally recurrent prostate cancer after radiotherapy. Int J Radiat Oncol Biol Phys. 2005;62:448–53.
Heidenreich A, Richter S, Thuer D, Pfister D. Prognostic parameters, complications, and oncologic and functional outcome of salvage radical prostatectomy for locally recurrent prostate cancer after 21st-century radiotherapy. Eur Urol. 2010;57:437–43.
Sanderson KM, Penson DF, Cai J, Groshen S, Stein JP, Lieskovsky G et al. Salvage radical prostatectomy: quality of life outcomes and long-term oncological control of radiorecurrent prostate cancer. J Urol. 2006;176:2025–31. discussion 2031-2
Krupski TL, Saigal CS, Hanley J, Schonlau M, Litwin MS. Patterns of care for men with prostate cancer after failure of primary treatment. Cancer. 2006;107:258–65.
Van Der Poel HG, Moonen L, Horenblas S. Sequential treatment for recurrent localized prostate cancer. J Surg Oncol. 2008;97:377–82.
Leonardo C, Simone G, Papalia R, Franco G, Guaglianone S, Gallucci M. Salvage radical prostatectomy for recurrent prostate cancer after radiation therapy. Int J Urol. 2009;16:584–6.
Kaffenberger SD, Keegan KA, Bansal NK, Morgan TM, Tang DH, Barocas DA et al. Salvage robotic assisted laparoscopic radical prostatectomy: A single institution, 5-year experience. J Urol 2013;189:507–513.
Yuh B, Ruel N, Muldrew S, Mejia R, Novara G, Kawachi M et al. Complications and outcomes of salvage robot-assisted radical prostatectomy: a single-institution experience. BJU Int 2014; 113: 769–76.
Chauhan S, Patel MB, Coelho R, Liss M, Rocco B, Sivaraman AK et al. Preliminary Analysis of the Feasibility and Safety of Salvage Robot-Assisted Radical Prostatectomy After Radiation Failure: Multi-Institutional Perioperative and Short-Term Functional Outcomes. J Endourol 2011;25:1013–19.
Strope SA, Coelho M, Wood DP, Hollenbeck BK. Robot-assisted salvage prostatectomy: evaluation of initial patient-reported outcomes. J Endourol. 2010;24:425–7.
Boris RS, Bhandari A, Krane LS, Eun D, Kaul S, Peabody JO. Salvage robotic-assisted radical prostatectomy: initial results and early report of outcomes. BJU Int. 2009;103:952–6.
Spiess PE, Given RW, Jones JS. Achieving the “bifecta” using salvage cryotherapy for locally recurrent prostate cancer: analysis of the Cryo On-Line Data (COLD) Registry data. BJU Int. 2012;110:217–20.
Pisters LL, Leibovici D, Blute M, Zincke H, Sebo TJ, Slezak JM et al. Locally Recurrent Prostate Cancer After Initial Radiation Therapy: A Comparison of Salvage Radical Prostatectomy Versus Cryotherapy. J Urol 2009;182:517–27.
Song J, Li M, Zagaja GP, Taxy JB, Shalhav AL, Al-Ahmadie HA. Intraoperative frozen section assessment of pelvic lymph nodes during radical prostatectomy is of limited value. BJU Int. 2010;106:1463–7.
Epstein JI, Allsbrook WC, Amin MB, Egevad LL, ISUP Grading Committee. The 2005 International Society of Urological Pathology (ISUP) Consensus Conference on Gleason grading of prostatic carcinoma. Am J Surg Pathol. 2005;29:1228–42.
Acknowledgements
The research for CALGB 9687 (Alliance) was supported, in part, by grants from the National Cancer Institute (CA31946) to the Alliance for Clinical Trials in Oncology (Monica M. Bertagnolli, MD, Chair) and to the Alliance Statistics and Data Center (Daniel J. Sargent, Ph.D., CA33601). The content of this manuscript is solely the responsibility of the authors and does not necessarily represent the official views of the National Cancer Institute.
The following institutions participated in this study:
Cedars-Sinai Medical Center, Los Angeles, CA, Armando Giuliano, MD
Duke University Medical Center, Durham, NC, Jeffrey Crawford, MD, supported by CA47577
Memorial Sloan-Kettering Cancer Center, New York, NY, Clifford A. Hudis, MD, supported by CA77651
University of California at San Francisco, San Francisco, CA, Charles J. Ryan, MD, supported by CA60138
University of Chicago, Chicago, IL, Hedy L. Kindler, MD, supported by CA41287
University of Massachusetts Medical School, Worcester, MA, William V. Walsh, MD, supported by CA37135
University of North Carolina at Chapel Hill, Chapel Hill, NC, Thomas C. Shea, MD, supported by CA47559
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Mohler, J.L., Halabi, S., Ryan, S.T. et al. Management of recurrent prostate cancer after radiotherapy: long-term results from CALGB 9687 (Alliance), a prospective multi-institutional salvage prostatectomy series. Prostate Cancer Prostatic Dis 22, 309–316 (2019). https://doi.org/10.1038/s41391-018-0106-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41391-018-0106-1
This article is cited by
-
Enrichment of “Cribriform” morphologies (intraductal and cribriform adenocarcinoma) and genomic alterations in radiorecurrent prostate cancer
Modern Pathology (2022)
-
Salvage re-irradiation using stereotactic body radiation therapy for locally recurrent prostate cancer: the impact of castration sensitivity on treatment outcomes
Radiation Oncology (2021)
-
Salvage prostatectomy for recurrent disease
Nature Reviews Urology (2019)