Abstract
Background
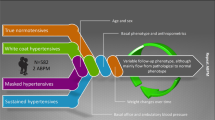
Patterns of blood pressure (BP) change from early adolescence to young adulthood have not been well-described. The objective of this study was to examine the predictive value of pediatric BP classification on BP change and identify subpopulations with large BP increases during adolescence and early adulthood.
Methods
Baseline data were obtained from medical checkups of Japanese adolescents aged 12–13 years in 2009 or 2010 and subsequent BP values were followed for a 9-year period. Mixed-effects models were used to estimate the effects of baseline factors on subsequent BP changes.
Results
Hypertensive and elevated BP group consistently had higher BP values than normal BP group throughout the observation period. Multivariate mixed-effects model analyses revealed group-by-time interactions between systolic BP change and BP category in males and uric acid category in females, and between diastolic BP change and white blood cell count in males and obesity and high-density lipoprotein cholesterol in females; however, these factors had limited effects on the rate of BP increase, indicating that they are not suitable as clinical predictors of BP increase.
Conclusions
Pediatric BP category predicted BP values, but there was no factor that identified subpopulations with large BP increases in adolescence and early adulthood.
Impact
-
Blood pressure category in the American Academy of Pediatrics clinical practice guideline at age 12–13 years predicted subsequent blood pressure values during adolescence and early adulthood.
-
No baseline factor that identified a subpopulation with large increase in blood pressure during adolescence and early adulthood in clinical practice was found.
-
Our study contributes to the existing literature by demonstrating the usefulness of the American Academy of Pediatrics clinical practice guideline for blood pressure classification in a Japanese population.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 14 print issues and online access
$259.00 per year
only $18.50 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The data used to support the findings of the present study are included in the main text or supplementary materials. Any remaining information are available from the corresponding author upon reasonable request.
References
Theodore, R. F. et al. Childhood to early-midlife systolic blood pressure trajectories: early-life predictors, effect modifiers, and adult cardiovascular outcomes. Hypertension 66, 1108–1115 (2015).
Azegami, T., Uchida, K., Tokumura, M. & Mori, M. Blood pressure tracking from childhood to adulthood. Front Pediatr. 9, 785356 (2021).
Yano, Y. et al. Association of blood pressure classification in young adults using the 2017 American College of Cardiology/American Heart Association Blood Pressure guideline with cardiovascular events later in life. JAMA 320, 1774–1782 (2018).
Yang, L., Magnussen, C. G., Yang, L., Bovet, P. & Xi, B. Elevated blood pressure in childhood or adolescence and cardiovascular outcomes in adulthood: a systematic review. Hypertension 75, 948–955 (2020).
Azegami, T. et al. Association of childhood anthropometric measurements and laboratory parameters with high blood pressure in young adults. Hypertens. Res. 44, 711–719 (2021).
Vos, L. E. et al. Does a routinely measured blood pressure in young adolescence accurately predict hypertension and total cardiovascular risk in young adulthood? J. Hypertens. 21, 2027–2034 (2003).
Juhola, J. et al. Childhood physical, environmental, and genetic predictors of adult hypertension: the cardiovascular risk in young Finns study. Circulation 126, 402–409 (2012).
Urbina, E. M. et al. Relation of blood pressure in childhood to self-reported. Hypertension 73, 1224–1230 (2019).
Alper, A. B. Jr. et al. Childhood uric acid predicts adult blood pressure: the Bogalusa Heart Study. Hypertension 45, 34–38 (2005).
Chan, K. C., Au, C. T., Hui, L. L., Wing, Y. K. & Li, A. M. Childhood OSA is an independent determinant of blood pressure in adulthood: longitudinal follow-up study. Thorax 75, 422–431 (2020).
Benisty, K. et al. Kidney and blood pressure abnormalities 6 years after acute kidney injury in critically ill children: a prospective cohort study. Pediatr. Res. 88, 271–278 (2020).
Kagura, J., Adair, L. S., Munthali, R. J., Pettifor, J. M. & Norris, S. A. Association between early life growth and blood pressure trajectories in Black South African children. Hypertension 68, 1123–1131 (2016).
Hao, G. et al. Blood pressure trajectories from childhood to young adulthood associated with cardiovascular risk: results from the 23-year longitudinal Georgia Stress and Heart Study. Hypertension 69, 435–442 (2017).
Cnaan, A., Laird, N. M. & Slasor, P. Using the general linear mixed model to analyse unbalanced repeated measures and longitudinal data. Stat. Med. 16, 2349–2380 (1997).
Murphy, J. I., Weaver, N. E. & Hendricks, A. E. Accessible analysis of longitudinal data with linear mixed effects models. Dis. Model Mech. 15, dmm048025 (2022).
Kuczmarski, R. J. et al. CDC Growth Charts for the United States: methods and development. Vital-. Health Stat. 11, 1–190 (2002).
Barlow, S. E. & Expert, C. Expert committee recommendations regarding the prevention, assessment, and treatment of child and adolescent overweight and obesity: summary report. Pediatrics 120, S164–S192 (2007).
Kato, N., Sato, K., Takimoto, H. & Sudo, N. BMI for age references for Japanese children-based on the 2000 growth survey. Asia Pac. J. Public Health 20, 118–127 (2008).
Kato, N., Takimoto, H. & Sudo, N. The cubic functions for spline smoothed L, S and M values for BMI reference data of Japanese children. Clin. Pediatr. Endocrinol. 20, 47–49 (2011).
Umemura, S. et al. The Japanese Society of Hypertension guidelines for the management of hypertension (JSH 2019). Hypertens Res. 42, 1235–1481 (2019).
Flynn, J. T. et al. Clinical practice guideline for screening and management of high blood pressure in children and adolescents. Pediatrics 140, e20171904 (2017).
Khoury, M. et al. Prevalence implications of the 2017 American Academy of Pediatrics Hypertension guideline and associations with adult hypertension. J. Pediatr. 241, 22–28.e4 (2022).
National High Blood Pressure Education Program Working Group on High Blood Pressure in Children and Adolescents. The fourth report on the diagnosis, evaluation, and treatment of high blood pressure in children and adolescents. Pediatrics 114, 555–576 (2004).
Urbina, E. M. et al. Association of blood pressure level with left ventricular mass in adolescents. Hypertension 74, 590–596 (2019).
Haley, J. E. et al. Association of blood pressure-related increase in vascular stiffness on other measures of target organ damage in youth. Hypertension 79, 2042–2050 (2022).
Jacobs, D. R. Jr. et al. Childhood cardiovascular risk factors and adult cardiovascular events. N. Engl. J. Med. 386, 1877–1888 (2022).
Nelson, M. J., Ragland, D. R. & Syme, S. L. Longitudinal prediction of adult blood pressure from juvenile blood pressure levels. Am. J. Epidemiol. 136, 633–645 (1992).
De Livera, A. M., Zaloumis, S. & Simpson, J. A. Models for the analysis of repeated continuous outcome measures in clinical trials. Respirology 19, 155–161 (2014).
Murtaugh, M. A. et al. Relationship of sodium intake and blood pressure varies with energy intake: secondary analysis of the DASH (Dietary Approaches to Stop. Hypertension)-Sodium trial. Hypertension 71, 858–865 (2018).
Mitsumata, K., Saitoh, S., Ohnishi, H., Akasaka, H. & Miura, T. Effects of parental hypertension on longitudinal trends in blood pressure and plasma metabolic profile: mixed-effects model analysis. Hypertension 60, 1124–1130 (2012).
Kotchen, J. M., McKean, H. E., Neill, M. & Kotchen, T. A. Blood pressure trends associated with changes in height and weight from early adolescence to young adulthood. J. Clin. Epidemiol. 42, 735–741 (1989).
Acknowledgements
We gratefully acknowledge all of the staff at Keio University Health Center who were involved in this research.
Funding
This work was supported by the Keio University Academic Development Funds for Joint Research (T.A.).
Author information
Authors and Affiliations
Contributions
Conception: T.A. and K.U.; Design: T.A. and K.U.; Acquisition of data: T.A. and U.K.; Analysis: T.A.; Interpretation of Data: T.A., K.U., and Y.S.; Drafting the article: T.A.; Revising the article: K.U., Y.S., A.M.-T., M.I., H.I., and M.M. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Azegami, T., Uchida, K., Sato, Y. et al. Pediatric blood pressure category predicts longitudinal blood pressure change in adolescence and early adulthood. Pediatr Res 94, 1731–1737 (2023). https://doi.org/10.1038/s41390-023-02675-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-023-02675-2