Abstract
Background
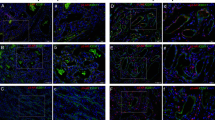
We report a 3-month-old female with cardiovascular anomalies and diffuse intestinal infantile hemangioma (IIH) of the small bowel suggesting possible diagnosis of PHACE syndrome (posterior fossa anomalies, hemangioma, arterial lesions, cardiac abnormalities/coarctation of the aorta, eye anomalies). The GI symptoms persisted under treatment with propranolol, whereas the addition of sirolimus led to regression of the IIH.
Methods
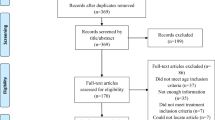
A systematic review was conducted using PubMed, EMBASE, and Ovid MEDLINE databases between 1982 and 2021.
Results
A total of 4933 articles were identified; 24 articles met inclusion criteria with 46 IIH cases. The most common GI presentations were unspecified GI bleed (40%) and anemia (38%). The most common treatments were corticosteroids (63%), surgical resection (32.6%), and propranolol (28%). Available outcomes were primarily bleeding arrest (84%). Nine cases (19.5%) were diagnosed with definite PHACE, 5 (11%) with possible PHACE, and 32 (69.5%) no PHACE. Our case presented with symptoms most consistent with those of possible PHACE and definite PHACE. No cases in this review underwent treatment with sirolimus.
Conclusions
This is the first reported case of successful treatment of IIH with sirolimus. Our case, along with other patients who present with IIH and PHACE features, suggests consideration of IIH as a diagnostic criterion for PHACE syndrome.
Impact
-
This is the first reported case in which sirolimus showed regression of an intestinal infantile hemangioma.
-
This study serves to demonstrate the presentation, treatment, outcomes of intestinal infantile hemangioma, and correlation with PHACE.
-
The potential correlation between intestinal infantile hemangioma and PHACE deserves more study in consideration of intestinal infantile hemangioma as a diagnostic criterion of PHACE.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 14 print issues and online access
$259.00 per year
only $18.50 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Bandera, A. I. R., Sebaratnam, D. F., Wargon, O. & Wong, L. C. F. Infantile hemangioma. Part 1: Epidemiology, pathogenesis, clinical presentation and assessment. J. Am. Acad. Dermatol. 85, 1379–1392 (2021).
Anderson, K. et al. Increasing incidence of infantile hemangiomas (IH) over the past 35 years: correlation with decreasing gestational age at birth and birth weight. J. Am. Acad. Dermatol. 74, 120–126 (2016).
Metry, D. W., Hawrot, A., Altman, C. & Frieden, I. J. Association of solitary, segmental hemangiomas of the skin with visceral hemangiomatosis. Arch. Dermatol. 140, 591–596 (2004).
Frieden, I. J., Reese, V. & Cohen, D. PHACE syndrome: the association of posterior fossa brain malformations, hemangiomas, arterial anomalies, coarctation of the aorta and cardiac defects, and eye abnormalities. Arch. Dermatol. 132, 307–311 (1996).
Metry, D. et al. Consensus statement on diagnostic criteria for PHACE syndrome. Pediatrics 124, 1447–1456 (2009).
Garzon, M. C. et al. PHACE syndrome: consensus-derived diagnosis and care recommendations. J. Pediatr. 178, 24–33 (2016).
Moher, D. et al. Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst. Rev. 4, 1–9 (2015).
Ouzzani, M., Hammady, H., Fedorowicz, Z. & Elmagarmid, A. Rayyan—a web and mobile app for systematic reviews. Syst. Rev. 5, 1–10 (2016).
Maruani, A. et al. Sirolimus (Rapamycin) for slow-flow malformations in children: the observational-phase randomized clinical PERFORMUS trial. JAMA Dermatol. 157, 1289–1298 (2021).
Dávila‐Osorio, V. L., Iznardo, H., Roé, E., Puig, L. & Baselga, E. Propranolol‐resistant infantile hemangioma successfully treated with sirolimus. Pediatr. Dermatol. 37, 684–686 (2020).
Greenberger, S. et al. Rapamycin suppresses self-renewal and vasculogenic potential of stem cells isolated from infantile hemangioma. J. Investig. Dermatol. 131, 2467–2476 (2011).
Hutchins, K. K., Ross, R. D., Kobayashi, D., Martin, A. & Rajpurkar, M. Treatment of refractory infantile hemangiomas and pulmonary hypertension with sirolimus in a pediatric patient. J. Pediatr. Hematol. Oncol. 39, e391–e393 (2017).
Sebaratnam, D. F., Rodríguez Bandera, A. L., Wong, L. F. & Wargon, O. Infantile hemangioma. Part 2: Management. J. Am. Acad. Dermatol. 85, 1395–1404 (2021).
Enjolras, O., Riche, M. C., Merland, J. J. & Escande, J. P. Management of alarming hemangiomas in infancy: a review of 25 cases. Pediatrics 85, 491–498 (1990).
Enjolras, O. & Gelbert, F. Superficial hemangiomas: associations and management. Pediatr. Dermatol. 14, 173–179 (1997).
Ezekowitz, R. A., Mulliken, J. B. & Folkman, J. Interferon alfa-2a therapy for life-threatening hemangiomas of infancy. N. Engl. J. Med. 326, 1456–1463 (1992).
Ge, Z. Z. et al. Clinical application of wireless capsule endoscopy in pediatric patients for suspected small bowel diseases. Eur. J. Pediatr. 166, 825–829 (2007).
Metry, D. W. et al. A comparison of disease severity among affected male versus female patients with PHACE syndrome. J. Am. Acad. Dermatol. 58, 81–87 (2008).
Metry, D. W. et al. A prospective study of PHACE syndrome in infantile hemangiomas: demographic features, clinical findings, and complications. Am. J. Med. Genet. A 140, 975–986 (2006).
Papparella, A. et al. Laparoscopic approach to Meckel’s diverticulum. World J. Gastroenterol. 20, 8173–8178 (2014).
Al-Musalhi, B. & Al-Balushi, Z. PHACES syndrome with intestinal hemangioma causing recurrent intussusceptions: a case report and literature review of associated intestinal hemangioma. Oman Med. J. 35, e204 (2020).
Bank, E. R., Hernandez, R. J. & Byrne, W. J. Gastrointestinal hemangiomatosis in children: demonstration with CT. Radiology 165, 657–658 (1987).
Chattopadhyay, A., Kumar, V., Maruliah, M. & Rao, P. L. N. G. Duodenojejunal obstruction by a hemangioma. Pediatr. Surg. Int. 18, 501–502 (2002).
Coleman, J., Phillips, R. & Steiner, R. Small bowel hemangioma in a 2-year-old female with recurrent anemia. Ochsner J. 18, 428–432 (2018).
Destro, F., Maestri, L., Vella, C., Baraldini, V. & Riccipetitoni, G. Infantile hemangioma as cause of neonatal gastrointestinal bleeding. J. Pediatr. Surg. Case Rep. 31, 71–76 (2018).
Drolet, B. A. et al. Gastrointestinal bleeding in infantile hemangioma: a complication of segmental, rather than multifocal, infantile hemangiomas. J. Pediatr. 160, 1021–1026 (2012).
Ghandour, R. M. et al. Prevalence and treatment of depression, anxiety, and conduct problems in US children. J. Pediatr. 206, 256–267 (2019).
Fishman, S. J., Burrows, P. E., Leichtner, A. M. & Mulliken, J. B. Gastrointestinal manifestations of vascular anomalies in childhood: varied etiologies require multiple therapeutic modalities. J. Pediatr. Surg. 33, 1163–1167 (1998).
Fu, J. X., Zou, Y. N., Han, Z. H., Yu, H. & Wang, X. J. Small bowel racemose hemangioma complicated with obstruction and chronic anemia: a case report and review of literature. World J. Gastroenterol. 26, 1674 (2020).
Hayek, S., Amin, M. B. & Trupiano, J. K. Diffuse neonatal hemangiomatosis with gastrointestinal involvement in a 4-month-old infant [Abstract]. Pediatr. Dev. Pathol. 13, 132–168 (2010).
Jarvi, K. et al. Successful treatment of extensive infantile hemangiomatosis of the small bowel in a 3-month-old with thalidomide and somatostatin analog. J. Pediatr. Gastroenterol. Nutr. 46, 593–597 (2008).
Kella, N., Rathi, P. K., Rathi, S. & Qureshi, M. A. Small bowel haemangioma. A rare cause of intestinal obstruction in infant. Pak. J. Med. Sci. 24, 629–631 (2008).
Krick, J., Riehle, K., Chapman, T. & Chabra, S. Recurrent bloody stools associated with visceral infantile haemangioma in a preterm twin girl. BMJ Case Rep. 11, bcr-2018 (2018).
Madan, V., Lloyd, I. C., Wakefield, R. M., Kaleem, M. & Judge, M. R. PHACE syndrome. Clin. Exp. Dermatol. 34, 651–652 (2009).
Metry, D. et al. Propranolol use in PHACE syndrome with cervical and intracranial arterial anomalies: collective experience in 32 infants. Pediatr. Dermatol. 30, 71–89 (2013).
Morris, G. A., Stratchko, L. & Sabri, M. Intestinal hemangioma presenting as recurrent hematochezia in a 6-week-old male. J. Pediatr. Surg. Case Rep. 3, 280–282 (2015).
September 10-14 Munich, Germany CIRSE 2011. Cardiovasc Intervent Radiol. 34 331 https://doi.org/10.1007/s00270-011-0216-9 (2011).
Patel, S. D., Cohen, B. A. & Kan, J. S. Extensive facial hemangioma associated with cardiac and abdominal anomalies. J. Am. Acad. Dermatol. 36, 636–638 (1997).
Peterman, C. M., Gibson, R. S., Lillis, A. P., Fishman, S. J. & Liang, M. G. Clinical and radiological characteristics of patients with retroperitoneal infantile hemangiomas. Pediatr. Dermatol. 36, 823–829 (2019).
Rao, A. B., Pence, J. & Mirkin, D. L. Diffuse infantile hemangiomatosis of the ileum presenting with multiple perforations: a case report and review of the literature. J. Pediatr. Surg. 45, 1890–1892 (2010).
Scafidi, D. E., McLeary, M. S. & Young, L. W. Diffuse neonatal gastrointestinal hemangiomatosis: CT findings. Pediatr. Radiol. 28, 512–514 (1998).
Shukri, N., Amara, R., Malik, S., Taher, H. & Kilany, M. Neonatal intestinal perforation-a rare complication of small bowel hemangioma. Eur. J. Pediatr. Surg. Rep. 1, 30–31 (2013).
Soukoulis, I. W. et al. Gastrointestinal infantile hemangioma: presentation and management. J. Pediatr. Gastroenterol. Nutr. 61, 415–420 (2015).
Stillman, A. E., Hansen, R. C., Hallinan, V. & Strobel, C. Diffuse neonatal hemangiomatosis with severe gastrointestinal involvement. Favorable response to steroid therapy. Clin. Pediatr. 22, 589–591 (1983).
Acknowledgements
We would like to acknowledge Tali Mualem, MD in management of this patient.
Author information
Authors and Affiliations
Contributions
All authors meet the Pediatric Research authorship requirements.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
Not applicable.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kleinman, E.P., Blei, F., Adams, D. et al. Sirolimus for diffuse intestinal infantile hemangioma with PHACE features: systematic review. Pediatr Res 93, 1470–1479 (2023). https://doi.org/10.1038/s41390-022-02325-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-022-02325-z