Abstract
Background
Approximately 5–10% of children exhibit developmental deviations in motor skills or other domains; however, physicians detect less than one-third of these abnormalities. Systematic tracking and early identification of motor deviations are fundamental for timely intervention.
Methods
Term and preterm neonates were prospectively assessed at the newborn (NB) period in a study of the psychometric properties of the Motor (MOT) domain of PediaTracTM v3.0, a novel caregiver-based development tracking instrument. Item response theory graded response modeling was used to model item parameters and estimate theta, an index of the latent trait, motor ability. Exploratory factor analysis (EFA) was conducted to examine the dimensionality and factor structure.
Results
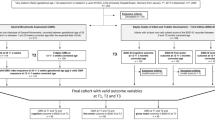
In a cohort of 571 caregiver/infant dyads (331 term, 240 preterm), NB MOT domain reliability was high (rho = 0.94). Item discrimination and item difficulty of each of the 15 items could be reliably modeled across the range of motor ability. EFA confirmed that the items constituted a single dimension with second-order factors, accounting for 43.20% of variance.
Conclusions
The latent trait, motor ability, could be reliably estimated at the NB period.
Impact
-
The caregiver-reported Motor domain of PediaTrac provides a reliable estimate of the latent trait of motor ability during the newborn period.
-
This is the first known caregiver-reported instrument that can assess motor ability in the newborn period with high reliability in term and preterm infants.
-
Item response theory methods were employed that will allow for future characterization of developmental subgroups and motor trajectories.
-
The PediaTrac Motor domain can support early identification of at-risk infants.
-
Including caregivers in digital reporting and child-centered monitoring of motor functioning may improve access to care.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 14 print issues and online access
$259.00 per year
only $18.50 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are not publicly available yet as this is a longitudinal investigation that is still underway. Upon completion of the longitudinal investigation, the datasets generated during this study will be deposited into the National Database for Autism Research (NDAR).
References
Grantham-McGregor, S. et al. Developmental potential in the first 5 years for children in developing countries. Lancet 369, 60–70 (2007).
Almas, A., Degnan, K. A., Nelson, C. A., Zeanah, C. H. & Fox, N. A. IQ at age 12 following a history of institutional care: findings from the Bucharest Early Intervention Project. Dev. Psychol. 52, 1858–1866 (2016).
Ferrari, F. et al. Motor and postural patterns concomitant with general movements are associated with cerebral palsy at term and fidgety age in preterm infants. J. Clin. Med. 8, 1189 (2019).
Ben-Itzchak, E. & Zachor, D. A. Toddlers to teenagers: long-term follow-up study of outcomes in autism spectrum disorder. Autism 24, 41–50 (2020).
Posar, A. & Visconti, P. Long-term outcome of autism spectrum disorder. Turk. Pediatr. Ars. 54, 207–212 (2019).
Dennis, M. et al. Functional plasticity in childhood brain disorders: when, what, how, and whom to assess Maureen. Neuropsychol. Rev. 24, 389–408 (2014).
Scattone, D., Raggio, D. J. & May, W. Comparison of The Vineland Adaptive Behavior Scales, second edition, and the Bayley scales of infant and toddler development, third edition. Psychol. Rep. 109, 626–634 (2011).
Beker, L. Principles of growth assessment. Pediatr. Rev. 27, 196–197 (2006).
Zubler, J. M., et al. Evidence-informed milestones for developmental surveillance tools. Pediatrics. 149, e2021052138. https://doi.org/10.1542/peds.2021-052138 (2022).
Allison, K. M., Cordella, C., Iuzzini-Seigel, J. & Green, J. R. Differential diagnosis of apraxia of speech in children and adults: a scoping review. J. Speech Lang. Hear Res. 63, 2952–2994 (2020).
Brothers, K. B., Glascoe, F. P. & Robertshaw, N. S. PEDS: developmental milestones-an accurate brief tool for surveillance and screening. Clin. Pediatr. (Philos.). 47, 271–279 (2008).
Bellman, M., Byrne, O. & Sege, R. Developmental assessment of children. BMJ 345, 31–35 (2013).
Shevell, M. et al. Evidence Report: genetic and metabolic testing on children with global developmental delay: report of the quality standards Subcommittee of the American Academy of Neurology and the Practice Committee of the Child Neurology Society. Neurology 60, 367–380 (2003).
Allotey, J. et al. Cognitive, motor, behavioural and academic performances of children born preterm: a meta-analysis and systematic review involving 64 061 children. BJOG Int J. Obstet. Gynaecol. 125, 16–25 (2018).
Novak, I. et al. Early, accurate diagnosis and early intervention in cerebral palsy: advances in diagnosis and treatment. JAMA Pediatr. 171, 897–907 (2017).
Romeo, D. M. et al. Early neurological assessment and long-term neuromotor outcomes in late preterm infants: a critical review. Medicina (Kaunas) 56, 1–13 (2020).
Bayley, N. & Aylward, G. P. Bayley Scales of Infant and Toddler Development 4th edn (NCS Pearson, Inc., Bloomington, MN, 2019).
Mullen, E. M. Mullen Scales of Early Learning (Circle Pines, MN, American Guidance Service Inc. National Research Council, 1995).
Macy, M. L., Huetteman, P. & Kan. K. Changes in primary care visits in the 24 weeks after COVID-19 stay-at-home orders relative to the comparable time period in 2019 in Metropolitan Chicago and Northern Illinois. J. Prim. Care Community Heal. 11, 2150132720969557 (2020).
Lajiness-O’Neill, R., et al. Development and validation of PediaTracTM: a web-based tool to track developing infants. Infant Behav. Dev. 50, 224–237. https://doi.org/10.1016/j.infbeh.2018.01.008 (2018).
Lajiness-O’Neill, R. et al. PediaTrac V.3.0 protocol: a prospective, longitudinal study of the development and validation of a web-based tool to measure and track infant and toddler development from birth through 18 months. BMJ Open. 11, e050488 (2021).
Squires, J., Bricker, D. & Twombly, E. Ages & Stages Questionnaires: a parent-completed child monitoring system-3 (Baltimore, MD, Brooks Publishing Company, 2009).
da Silva, M. A., de Mendonça Filho, E. J., Mônego, B. G. & Bandeira, D. R. Instruments for multidimensional assessment of child development: a systematic review. Early Child Dev. Care. 190, 1257–1271 (2020).
Sparrow, S., Cicchetti, D. V. & Saulnier C. A. Vineland Adaptive Behavior Scale 3rd edn (VABS-3). (San Antonio, TX, Pearson, 2016).
Voress, J. K. & Maddox, T. Developmental Assessment of Young Children 2nd edn (DAYC-2). (Austin, TX, PRO-ED, 2013).
Child Health & Development Interacteractive System (CHADIS). http://www.chadis.com/.
Cella, D. et al. The Patient-Reported Outcomes Measurement Information System (PROMIS). Med. Care. 45(5 Suppl 1), S3–S11 (2007).
Embretson, S. E. & Reise, S. P. Item Response Theory for Psychologists (Erlbaum, Mahwah, NJ, 2000).
Samejima, F. Graded response model. In Handbook of Modern Item Response Theory (eds van der Linden, W. J. & Hambleton, R. K.) (Springer, New York, NY, 1997). https://doi.org/10.1007/978-1-4757-2691-6_5
Kamata, A. & Bauer, D. J. A note on the relation between factor analytic and item response theory models. Struct. Equ. Model. 15, 136–153 (2008).
Thissen, D. & Orlando, M. Item response theory for items scored in two categories. In Test Scoring 1st edn (eds Thissen, D., Nelson, L., Rosa, K. & McLeod, L. D.) (Routledge, New York, 2001). https://doi.org/10.4324/9781410604729
Hambleton, R. K., Swaminathan, H. & Jane Rogers, H. Fundamentals of Item Response Theory (Sage Publications, Inc., Newbury Park, CA, 1991).
de Ayala, R. J. The theory and practice of item response theory. Ref. Res. B News. 24, 209–236 (2009).
Nguyen, T. H., Han, H.-R., Kim, M. T. & Chan, K. S. An introduction to item response theory for patient-reported outcome measurement. Patient 7, 23–35 (2014).
R Core Team. R: A Language and Environment for Statistical Computing (Vienna, Austria, 2020).
Kaiser, H. F. The application of electronic computers to factor analysis. Educ. Psychol. Meas. 20, 141–151 (1960).
Depaoli, S., Tiemensma, J. & Felt, J. M. Assessment of health surveys: fitting a multidimensional graded response model. Psychol. Heal Med. 23, 13–31 (2018).
Gibson, E. Exploratory behavior in the development of perceiving, acting, and the acquiring of knowledge. Annu Rev. Psychol. 39, 1–41 (1988).
Adolph, K. E. & Franchak, J. M. The development of motor behavior. Wiley Interdiscip. Rev. Cogn. Sci. 8, 1–30 (2017).
Adolph, K. E., Karasik, L. B. & Tamis-Lemonda, C. S. Motor skill. In: Handbook of Cultural Developmental Science (ed. Bornstein, M. H.) 61–88 (Psychology Press, 2010).
Hopkins, B. & Westra, T. Motor development, maternal expectations, and the role of handling. Infant Behav. Dev. 13, 117–122 (1990).
Blauw-Hospers, C. H., de Graaf-Peters, V. B., Dirks, T., Bos, A. F. & Hadders-Algra, M. Does early intervention in infants at high risk for a developmental motor disorder improve motor and cognitive development. Neurosci. Biobehav Rev. 31, 1201–1212 (2007).
Hua, J. et al. Early motor milestones in infancy and later motor impairments: a population-based data linkage study. Front Psychiatry 13, 1–11 (2022).
Fogel, A., Messinger, K., Dickson, L. & Hsu, H. Posture and gaze in early mother-infant communication: synchronization of developmental trajectories. Dev. Sci. 2, 325–332 (2001).
Rachwani, J. et al. Segmental trunk control acquisition and reaching in typically developing infants. Exp. brain Res. 228, 131–139 (2013).
Acknowledgements
The investigators express their sincere gratitude to caregivers who participated in the PediaTrac project. We would like to acknowledge the Corner Health Center for their support in helping recruit those with the greatest need.
Funding
This study was supported by the Eunice Kennedy Shriver National Institute of Child Health & Human Development of the National Institutes of Health under Award Number (R01HD095957). The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health. Efforts of S.W. were also supported in part by the Mildred E. Swanson Foundation.
Author information
Authors and Affiliations
Consortia
Contributions
Conception and design of the study: R.L.-O., T.R., S.W., P.B., A.H.-B., H.G.T., J.C.G.L., J.B., and A.L. Acquisition, analysis, and interpretation of data: T.R., P.B., A.D.S., J.C.G.L., R.L.-O., S.W., A.H.-B., and H.G.T.. Drafting and revising the manuscript (original): R.L.-O., T.R., P.B., S.W., A.H.-B., H.G.T., A.S., and J.C.G.L. Final approval: R.L.-O., T.R., P.B., A.H.-B., H.G.T., A.S., J.B., A.L., J.C.G.L., and S.W.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
Participant consent was required, with the study approved by the University of Michigan IRB of Record (HUM00151584).
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lajiness-O’Neill, R., Raghunathan, T., Berglund, P. et al. Caregiver-reported newborn term and preterm motor abilities: psychometrics of the PediaTracTM Motor domain. Pediatr Res 93, 1736–1744 (2023). https://doi.org/10.1038/s41390-022-02312-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-022-02312-4