Abstract
Objective
To investigate postnatal neural conduction in the auditory brainstem in neonatal bronchopulmonary dysplasia (BPD) survivors.
Methods
Thirty-two very preterm BPD survivors were studied at 57–58 weeks of postconceptional age. Brainstem auditory-evoked response was studied using maximum length sequence. Wave latencies and intervals were analyzed in detail. The controls were 37 normal term infants and 35 very preterm non-BPD infants.
Results
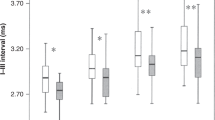
Compared with normal term controls, BPD survivors showed significantly shortened I–III interval but significantly prolonged III–V interval and greater III–V/I–III interval ratio. Compared with very preterm non-BPD controls, BPD survivors showed a significant shortening in waves III latency and I–III interval, moderate prolonged III–V interval, and significantly greater III–V/I–III interval ratio. These differences were generally similar at all click rates used. The slopes of latency- and interval-click rate functions in BPD survivors did not differ significantly from the two control groups.
Conclusions
Brainstem neural conduction in BPD survivors differed from normal term and age-matched non-BPD infants; neural maturation is accelerated in caudal brainstem regions but delayed in rostral regions. Neonatal BPD survivors are associated with differential maturation in neural conduction at caudal and rostral brainstem regions, which may constitute an important risk for postnatal neurodevelopment in BPD survivors.
Impact
-
We found that brainstem neural conduction at PCA 57–58 weeks in neonatal BPD survivors differs from normal term and age-matched non-BPD infants.
-
No major differences were found between normal term and very preterm non-BPD infants in brainstem auditory conduction.
-
Neural conduction in BPD survivors is accelerated in caudal brainstem regions but delayed in rostral regions.
-
Neonatal BPD survivors are associated with differential maturation in neural conduction at caudal and rostral brainstem regions.
-
The abnormality may constitute an important risk for postnatal neurodevelopment in BPD survivors.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 14 print issues and online access
$259.00 per year
only $18.50 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
The datasets analyzed during the current study are available from the corresponding author on reasonable request.
References
Lapcharoensap, W. et al. Hospital variation and risk factors for bronchopulmonary dysplasia in a population-based cohort. JAMA Pediatr. 169, e143676 (2015).
Sahni, M. & Bhandari, V. Recent advances in understanding and management of bronchopulmonary dysplasia. F1000Res 14, 9, https://doi.org/10.12688/f1000research.25338.1 (2020). F1000 Faculty Rev-703eCollection 2020.
Tracy, M. K. & Berkelhamer, S. K. Bronchopulmonary dysplasia and pulmonary outcomes of prematurity. Pediatr. Ann. 48, e148–e153 (2019).
Deakins, K. M. Bronchopulmonary dysplasia. Respir. Care 54, 1252–1262 (2009).
Doyle, L. W. & Anderson, P. J. Long-term outcomes of bronchopulmonary dysplasia. Semin. Fetal Neonatal Med. 14, 391–395 (2009).
Jeng, S. F. et al. Bronchopulmonary dysplasia predicts adverse developmental and outcomes in very-low-birthweight infants. Dev. Med. Child Neurol. 50, 51–57 (2008).
Karagianni, P. et al. Neuromotor outcomes in infants with bronchopulmonary dysplasia. Pediatr. Neurol. 44, 40–46 (2011).
van Marter, L. J. Epidemiology of bronchopulmonary dysplasia. Semin. Fetal Neonatal Med. 14, 358–366 (2009).
Raman, L., Georgieff, M. K. & Rao, R. The role of chronic hypoxia in the development of neurocognitive abnormalities in preterm infants with bronchopulmonary dysplasia. Dev. Sci. 9, 359–367 (2006).
Suppiej, A. et al. Neonatal cortical auditory evoked potentials are affected by clinical conditions occurring in early prematurity. J. Clin. Neurophysiol. 32, 419–423 (2015).
Neubauer, V., Junker, D., Griesmaier, E., Schocke, M. & Kiechl-Kohlendorfer, U. Bronchopulmonary dysplasia is associated with delayed structural brain maturation in preterm infants. Neonatology 107, 179–184 (2015).
Wilkinson, A. R., Brosi, D. M. & Jiang, Z. D. Functional impairment of the brainstem in infants with bronchopulmonary dysplasia. Pediatrics 120, 362–371 (2007).
Jiang, Z. D. Auditory impairment is alleviated after term in infants with neonatal chronic lung disease. Acta Paediatr. 106, 926–929 (2017).
Jiang, Z. D. Maximum length sequence technique improves detection of neuropathology involving infant brainstem. In: Pediatric Neurology (eds Lawson, P. N. & McCarthy, E. A.) 1–38 (Nova Science Publishers, New York, 2012).
Jiang, Z. D. Evoked potentials in pediatric brainstem lesions. In: Clinical Neurophysiology in Pediatrics: A Practical Approach to Neurodiagnostic Testing and Management (ed Galloway, G.) 187–213 (Demos Medical Publishing, LLC, New York, 2015).
Wilkinson, A. R. & Jiang, Z. D. Brainstem auditory evoked response in neonatal neurology. Semin. Fet. Neonatol. 11, 444–451 (2006).
Jiang, Z. D., Pin, L. L. & Wilkinson, A. R. Functional abnormality of the auditory brainstem in high-risk late preterm infants. Clin. Neurophysiol. 123, 993–1001 (2012).
Chess, P. R., D’Angio, C. T., Pryhuber, G. S. & Maniscalco, W. M. Pathogenesis of bronchopulmonary dysplasia. Semin. Perinatol. 30, 171–178 (2006).
Gagliardi, L., Bellù, R., Zanini, R. & Dammann, O. Bronchopulmonary dysplasia and brain white matter damage in the preterm infant: a complex relationship. Paediatr. Perinat. Epidemiol. 23, 582–590 (2009).
Gien, J. & Kinsella, J. P. Pathogenesis and treatment of bronchopulmonary dysplasia. Curr. Opin. Pediatr. 23, 305–313 (2011).
Jiang, Z. D., Brosi, D., Wu, Y. Y. & Wilkinson, A. R. Relative maturation of the peripheral and central regions of the auditory brainstem from preterm to term and the influence of preterm birth. Pediatr. Res. 65, 657–662 (2009).
Jiang, Z. D. & Ping, L. L. Functional integrity of rostral regions of the immature brainstem is impaired in babies born extremely preterm. Clin. Neurophysiol. 127, 1581–1588 (2016).
Collet, L., Soares, I., Morgon, A. & Salle, B. Is there a difference between extrauterine and intrauterine maturation on BAEP? Brain Dev. 11, 293–296 (1989).
Pasman, J. W., Rotteveel, J. J., de Graaf, R., Stegeman, D. F. & Visco, Y. M. The effect of preterm birth on brainstem, middle latency and cortical auditory evoked responses (BMC AERs). Early Hum. Dev. 31, 113–129 (1992).
Pasman, J. W., Rotteveel, J. J., de Graaf, R., Maassen, B. & Visco, Y. M. The effects of early and late preterm birth on brainstem and middle-latency auditory evoked responses in children with normal neurodevelopment. J. Clin. Neurophysiol. 13, 234–241 (1996).
Amiel-Tison, C. & Pettigrew, A. G. Adaptive changes in the developing brain during intrauterine stress. Brain Dev. 13, 67–76 (1991).
Kim, C. R., Vohr, B. R. & Oh, W. Effects of maternal preeclampsia on brain-stem auditory evoked response in very low birth weight infants. J. Pediatr. 127, 123–127 (1995).
Takashima, S. & Becker, L. E. Developmental neuropathology in bronchopulmonary dysplasia: alteration of glial fibrillary acidic protein and myelination. Brain Dev. 6, 451–457 (1984).
Thompson, D. K. et al. Perinatal risk factors altering regional brain structure in the preterm infant. Brain 130, 667–677 (2007).
Borenstein-Levin, L. et al. Effects of neurodevelopmental risk factors on brainstem maturation in premature infants. Pediatr. Res. https://doi.org/10.1038/s41390-021-01849-0 (2021).
Acknowledgements
We are indebted to doctors and nurses at Neonatal Division of Children’s Hospital for their enthusiastic assistance in the recruitment of the subjects and collection of data.
Author information
Authors and Affiliations
Contributions
J.K.J. made a major contribution to data analysis and manuscript writing. C.W. was responsible for recording MLS BAER and collecting clinical data. Z.D.J. designed and supervised the study and was responsible for the final version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Consent to participate
Informed parental consent was obtained for each infant.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Jiang, J.K., Wang, C. & Jiang, Z.D. Postnatal abnormality in brainstem neural conduction in neonatal bronchopulmonary dysplasia survivors. Pediatr Res 93, 1679–1686 (2023). https://doi.org/10.1038/s41390-022-02222-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-022-02222-5