Abstract
Background
Interpretation of the results of steroid hormone measurements is challenging at early infancy. The liquid chromatography-tandem mass spectrometry (LC-MS/MS) method provides a powerful tool for diagnosing steroidogenesis disorders. We aimed to develop normative data for a 14-steroid panel and four adrenal enzyme activity indices, determined by LC-MS/MS from 3 days to 6 months of age.
Methods
Age- and sex-specific plasma steroid concentrations were calculated in 324 healthy full-term neonates and infants (151 females). Percentile curves were devised. Steroid ratios were evaluated as biomarkers of adrenal enzyme activities. The steroid profiles of four patients with adrenal enzyme deficiencies were included to test the diagnostic efficiency.
Results
Nine steroids showed age, but none showed sex specificity. The concentrations of progestins and androgens were higher at 7–14 days than at 3–7 days. After the first month, adrenal androgen concentrations decreased significantly. Adrenal enzyme activities changed towards increasing cortisol over the first 6 months. There were several-fold differences in diagnostic steroids and related adrenal enzyme activity indices between the patients and the healthy group.
Conclusions
The majority of adrenal steroids show age-related variations in the neonatal period and early infancy. Our data will enable accurate interpretation of steroid measurements for etiologic diagnosis of disorders of steroidogenesis.
Impact
-
LC-MS/MS method is capable of quantitating numerous analytes simultaneously, which provides an integrated picture of adrenal steroidogenesis in a small amount of sample.
-
The development of LC-MS/MS-based normative data of steroid hormones in healthy infants is crucial to differentiate physiologic alterations from steroidogenic defects during the first 3–6 months of infancy.
-
Previous studies had limitations due to the small numbers of samples available by sex and by age groups.
-
Our detailed normative data and percentile curves will enable accurate interpretation of steroid measurements for etiologic diagnosis of disorders of steroidogenesis without the need for further invasive testing.
Similar content being viewed by others
Introduction
A mature human adrenal cortex produces mineralocorticoids, glucocorticoids, and adrenal androgens. The fetal zone at the antenatal period also produces large amounts of adrenal androgens.1 The adrenocortical steroid profile demonstrates dynamic changes in the first 6 months of infancy. These temporal variations in steroid production may limit accurate interpretation of steroid measurements and correct diagnosis of congenital steroidogenic disorders, most of which present in this critical period of time.2 Therefore, there is a need for detailed normative data of steroid hormones in healthy infants, to differentiate physiologic alterations from steroidogenic defects.
Liquid chromatography-tandem mass spectrometry (LC-MS/MS) has been recognized as the technique of choice for clinical use, due to high analytical sensitivity even at low steroid concentrations and reduced interference from analytes, which are commonly encountered with immunoassays.3 In addition, the LC-MS/MS method is able to quantitate numerous analytes simultaneously. It, therefore, is capable of providing an integrated picture of adrenal steroidogenesis in a small amount of sample in infants.
Adrenal enzyme deficiencies lead to reduced biosynthesis of the steroids distal to the block and accumulation of the precursors proximal to the block. This allows LC-MS/MS-based steroid panels to calculate precursor-to-product ratios in steroid hormone metabolism, which enables accurate localization of the enzyme deficiency in disorders of steroidogenesis.3,4 As in all assay methods, appropriate interpretation of steroid data obtained by MS-based techniques requires the development of well-established normative data, which is currently scarce. Previous studies in that respect had limitations due to the small numbers of samples available both by sex and by age group. Furthermore, these studies used inappropriate age groups such as combining neonates with older infants and thus, potentially, missing the clinically significant changes in the concentrations of steroids that occur in the most critical neonatal/early infancy period.5,6,7,8,9,10,11
In this study, we have produced reference ranges for 14 adrenal steroid hormones and four precursor-to-product steroid ratios for 21-hydroxylase, 11β-hydroxylase, 3β-hydroxysteroid dehydrogenase, and 11β-hydroxysteroid dehydrogenase-2 activities in 324 healthy infants from 3 days to 6 months of age using LC-MS/MS. In addition, we have evaluated temporal changes in the adrenal steroid metabolome in the first 6 months of infancy.
Methods
Study population
Healthy infants from 3 days to 6 months of age, who were appropriate for gestational age and had a history of uncomplicated vaginal or cesarean section delivery at term, were enrolled. Infants with a maternal history of diabetes or any other chronic disease and steroid therapy for any condition were excluded. Infants born in Marmara University Hospital or in Umraniye Training and Research Hospital neonatal care units, and/or attending well-baby clinics for growth monitoring or for routine vaccination procedures, were enrolled into the study after informed consent was obtained from the parents. The measurements of steroid hormones were expressed in short intervals and five groups were defined, according to age: Group 1, 3–7 days (n = 65, 30 male/35 female); Group 2, 8–14 days (n = 61, 37 male/24 female); Group 3, 15–28 days (n = 67, 36 male/31 female); Group 4, 28–90 days (n = 64, 35 male/29 female); and Group 5, 91–180 days (n = 67, 35 male/32 female). Gestational age and height, weight and head circumference at birth, delivery method, and the time of blood sampling were recorded.
Studies were performed with the approval of the Ethics Committee of Marmara University Faculty of Medicine, Istanbul, Turkey (09.2016.342). Parents provided written informed consent, and all studies were conducted in accordance with the principles of the Declaration of Helsinki.
Blood samples
Venous blood samples were collected between 08:00 and 09:00 a.m. into ethylenediaminetetracetic acid-containing tubes (Becton Dickenson, USA). The samples were immediately transferred to the laboratory and centrifuged. Plasma samples were stored at −80 °C until analysis.
Steroid hormone analysis
LC-MS/MS-based panel of plasma adrenal steroids was evaluated using Eureka kit (Eureka Lab Division, Ancona, Italy) as previously described (https://www.eurekakit.com/wp-content/uploads/2020/12/BROCHURE-STEROIDS-HORMONES-WEB.pdf). The Poroshell 120 EC-C18 (50 × 2.1 mm2, 2.7 μm; Agilent Technologies, Santa Clara, CA) column was used. Analyses were performed on a Shimadzu LCMS 8050 tandem mass spectrometer equipped with a Nexera XR LC-20AD HPLC system (Shimadzu Corporation, Japan) that was operated using electrospray ionization source in positive and multiple reactions monitoring mode. Method validation was performed according to the Clinical and Laboratory Standards Institute (CLSI) C62-A guideline. The steroids simultaneously assessed by the LC-MS/MS method were: aldosterone, corticosterone, 11-deoxycorticosterone, pregnenolone, 17OH-pregnenolone (17OHPreg), progesterone, 17OH-progesterone (17OHP), 21-deoxycortisol, 11-deoxycortisol, cortisol, cortisone, dehydroepiandrosterone (DHEA), Δ4-androstenedione, and androsterone.12
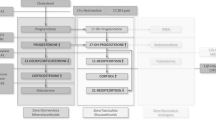
The product-to-substrate ratios for each adrenal steroid biosynthetic step were calculated and are subsequently referred to as the enzymatic maturity index. The following ratios (17OHP + 21-deoxycortisol)/cortisol, 11-deoxycortisol/cortisol, 17OHPreg/cortisol, and cortisol/cortisone) were evaluated as indices of 21-hydroxylase, 11β-hydroxylase, 3β-hydroxysteroid dehydrogenase, and 11β-hydroxysteroid dehydrogenase-2 activities, respectively (Fig. 1). For validation purposes, and to test the efficiency in the differential diagnosis of our panel, we included four patients with molecularly proven 21-hydroxylase, 11β-hydroxylase, 3β-hydroxysteroid dehydrogenase, and aldosterone synthase deficiencies. To compare our data with the existing literature, we have collated and appraised six peer-reviewed publications, which reported plasma LC-MS/MS reference intervals in healthy cohorts including infants below 6 months of age. To test the diagnostic efficiency of our data, the steroid profiles of four patients with molecular-proven 21-hydroxylase, 11β-hydroxylase, 3β-hydroxysteroid dehydrogenase, and aldosterone synthase deficiencies were also analyzed and presented separately.
The following ratios (17OH-progesterone + 21-deoxycortisol)/cortisol, 11-deoxycortisol/cortisol, 17OH-pregnenolone/cortisol and cortisol/cortisone) were evaluated as indices of 21-hydroxylase*, 11β-hydroxylase**, 3β-hydroxysteroid dehydrogenase (3β-HSD2)***, and 11β-hydroxysteroid dehydrogenase-2 (11 β-HSD2)**** activities, respectively. A ratio of the sum of 17OHP and 21-deoxycortisol levels divided by the cortisol level is currently used as the second-tier testing in the neonatal screening for congenital adrenal hyperplasia in Turkey and is superior to 17OHP alone in the diagnosis of 21-hydroxylase deficiency.29
Statistics
Percentile curves were derived for each of the 14 plasma steroid metabolites and four precursor-to-product ratios, based on linear mixed models,13 incorporating age and sex as dependent variables. Assuming the logarithm of metabolite concentrations to be normally distributed, the curves were fitted in several combinations of a linear mixed model. Age was transformed based on Royston and Wright’s recommendation.14 To validate the model, the assumption of the linear mixed model was checked. The residual plot of the models revealed that the data be nonlinear, and then the data were transformed (log transform and Royston and Wright’s transform) to make the model fit to data in an advanced way.15 Statistical analyses were performed with R 3.5.3 by using the lme4 package.16
Results
Corticosterone, 17OHP, 17OHPreg, and DHEA showed no association with age. None of the metabolites and ratios showed association with sex. The concentrations of the majority of the C21 steroids, except aldosterone, progesterone, 11-deoxycortisol and cortisone, and all C19 steroids in this study, were higher at 7–14 days of age than at 3–7 days.
Among the C21-steroid hormones from progesterone to corticosterone and aldosterone, the most striking age-related changes were found in progesterone and aldosterone concentrations, which decreased ~10- and 2-folds, respectively, over the first 6 months of infancy.
Plasma cortisol increased ~3-fold, whereas cortisone concentrations showed a decline in the first 6 months of infancy. While 17OHP does not show an age-related change, 11-deoxycortisol showed a trend towards decrease, and 21-deoxycortisol towards increase, by nearly 1.5–2-folds.
Androstenedione concentrations were higher at 7–14 days compared to those at 3–7 days. However, these concentrations decreased, particularly after 1 month, while androsterone concentrations increased between 1 and 6 months.
The 2.5th, 50th, and 97.5th percentiles of the plasma steroid metabolites and precursor-to-product ratios are given in Table 1 and separate data are presented by sex and age dependency in Supplemental Table 1. The comparison of our data with the previous six peer-reviewed publications on plasma LC-MS/MS reference intervals in healthy infants is presented in Supplemental Table 2.
Age-specific estimated percentiles of ten plasma steroid metabolites and four precursor-to-product ratios are shown in Figs. 2, 3, and 4, respectively.
Estimated percentile curves of four plasma adrenal steroid hormones (a cortisol, b aldosterone, c androstenedione, d dehydroepiandrosterone) from 3 days to 6 months of age (transformed ages 0.01, 0.25, 0.50, 0.75, and 1 on the X-axis correspond to 0.5, 0.14, 0.07, 0.035 and 0.008 years of decimal chronological age).
Estimated percentile curves of three plasma adrenal steroid hormone precursors (a 11-deoxycorticosterone, b 11-deoxycortisol, c 21-deoxycortisol) from 3 days to 6 months of age (Transformed ages 0.01, 0.25, 0.50, 0.75 and 1 on the X-axis correspond to 0.5, 0.14, 0.07, 0.035 and 0.008 years of decimal chronological age).
Estimated percentile curves of four precursor-to-product ratios (a 11-deoxycortisol/cortisol, b 17OH-pregnenolone/cortisol, c 17OH-progesterone + 21-deoxycortisol)/cortisol, d cortisol/cortisone) from three days to six months of age (Transformed age 0.01, 0.25, 0.50, 0.75 and 1 on the X-axis correspond to 0.5, 0.14, 0.07, 0.035 and 0.008 years of decimal chronological age).
To test the clinical efficiency of our data, plasma was analyzed from one 46,XY patient with classic 11β-hydroxylase deficiency (patient 1) who was recalled from neonatal CAH screening test, one 46,XY patient with aldosterone synthase deficiency (patient 2) who presented with salt-wasting, vomiting, and failure to thrive, one 46,XY patient with classic salt-wasting 21-hydroxylase deficiency (patient 3), and one 46,XX patient with classic 3β-hydroxysteroid dehydrogenase deficiency (patient 4) who presented with salt wasting. (Table 2). In patient 1, 11-deoxycortisol and 11-deoxycortisol/cortisol concentrations were 280- and 650-folds higher compared with the respective age group, respectively. Patient 2 had normal cortisol concentrations, while his corticosterone and 11-deoxycorticosterone concentrations were 17- and 9-folds higher than the control group at the same age, respectively. In patient 3, 17OHP, 21-deoxycortisol, and (17OHP + 21-deoxycortisol)/cortisol ratios were 80-, 87-, and 45-folds higher compared with the respective age group, respectively. Patient 4 had 6-fold elevated DHEA and 8-fold elevated 17OHPreg concentrations as well as a high 17OHPreg/cortisol ratio compared to the control group at the same age, respectively (Table 2).
Discussion
The present study provides detailed reference ranges for 14 adrenal steroid hormones and activity indices of four steroidogenic enzymes from 3 days to 6 months of age in a large cohort of healthy infants, using an LC-MS/MS technique.
In recent years, LC-MS/MS has progressively replaced immunoassays for the diagnosis of steroidogenic disorders in pediatrics.17 However, shifting from an immunoassay to an LC-MS/MS method necessitates the development of reference intervals to interpret the steroid hormone measurements for accurate clinical decision making. There are several studies of normative data of plasma adrenal steroids in children by LC-MS/MS. However, in most of them, a small number of samples were enrolled for each sex and age group, especially for infants under 6 months. Moreover, the age intervals in those studies were too broad, disregarding the dynamic changes that happen in the first months of infancy when steroid hormone concentrations vary widely.5,6,7,8,9,10,11 Nevertheless, steroid concentrations obtained in our study were in agreement with those in the previous studies with comparable ages except for minor differences. The strength of our study comes from a larger number of neonates and infants, which allowed us to construct reference ranges with centiles in a sex-specific manner with five different age groups reflecting dynamic changes in steroids more precisely. It is important to note that our study did not include preterm subjects who have an entirely different steroid profile.
Overall, the data indicated an age-dependent progressive decrease in the key steroids of the zona glomerulosa (corticosterone), zona fasciculata (11-deoxycortisol), and zona reticularis (DHEA) in relation to cortisol in the 6 months of infancy, suggesting maturation of the adrenal enzymes to produce more cortisol. Furthermore, the inactivation of cortisol, which is represented by the cortisone/cortisol ratio catalyzed by 11β-HSD type 2 enzyme is decreased during this period of time. This shows that both anabolic and catabolic pathways favor bioactive glucocorticoid production during the maturation of the adrenal cortex in early infancy (Fig. 5).
Longitudinal changes in the major adrenal zone steroids in relation to cortisol production (a corticosterone/cortisol, b 11-deoxycortisol/cortisol, c DHEA/cortisol, d cortisone/cortisol) from three days to six months of age with regression (solid black) and 95% CI (dotted black) lines. The name of the adrenal enzyme presented by the related ratio is given on top of each graph.
It is important to consider these dynamic changes in androgen concentrations particularly for the discrimination of “physiological” states from “pathologic” hyperandrogenism associated with congenital adrenal hyperplasia (CAH). The majority of CAH patients present during the second or third weeks of age with salt wasting, which can be fatal if not diagnosed and treated early.18 Therefore, our detailed data will be helpful in the differential diagnosis of “transient physiological adrenal hyperandrogenism” from “pathological adrenal androgen excess” caused by CAH in the first months of infancy. Neonatal screening programs have been implemented in many countries aiming at reducing the morbidity and mortality related to the delayed diagnosis of CAH. LC-MS/MS-based steroid panels and 21-deoxycortisol are becoming increasingly used as the second-tier screen of CAH screening in neonates.19,20,21 The normative data generated in our study can be used in clinics for efficient and rapid evaluation of infants recalled due to positive CAH screening results.
The present study also provided important information about the temporal changes in certain adrenal steroids. In particular, it was notable that higher progestin and androgen concentrations were found in the 7–14th postnatal day period compared to the 3–7th postnatal day period. This pattern may be attributable to the withdrawal of placental CRH during the transition to postnatal life and an acute withdrawal effect of the placental–fetal unit at 3–7th days followed by the recovery of the fetal zone, making a peak secretion of adrenal androgens and progressively involuting thereafter. Therefore, there is a clear lag phase of adrenal androgen output for ~1 week post partum.21 This tempo may also be evident in disease states. In fact, even some severe CAH cases display almost normal steroidogenic profiles in the first week of age and subsequent increase of diagnostic adrenal androgen precursors after the first week.22 Likewise, in neonatal screening for CAH, some classical CAH cases demonstrate a delayed rise in 17OHP and androgen levels. The second-tier screen, obtained on the 8–14th postnatal days, diagnose a further 30% of classical CAH cases.23
Another notable pattern in steroids that the present study uncovers is the progressive increase in androsterone concentrations up to 10 ng/mL in the first 6 months of infancy. We think that this finding is caused by minipuberty. Minipuberty is the transient activation of the hypothalamic-pituitary-gonadal (HPG) axis in early infancy. Minipuberty is important for early and late postnatal sexual differentiation in males including postnatal phallic growth, increase in testicular volume, seminiferous tubules, Sertoli and germ cell numbers, and masculinization of the brain. A lag phase in gonadotropin and gonadal steroid secretion in the first week of life before minipuberty is similar to the lag phase of adrenal androgen output for ~1 week post partum shown in our study. This lag phase before minipuberty is explained by the removal of placental hormones from the neonate’s circulation, which results in a lack of negative feedback on the GnRH pulse generator and reactivation of the HPG axis about 1 week after birth. It has been shown that particularly androsterone, which is produced by the alternative backdoor pathway during minipuberty, contributes to a transient surge of androgen production.24
The cortisol production capacity of a newborn is quite limited, which explains very low cortisol concentrations in the earliest days of life, although this improves progressively, a pattern that has been reported previously and is supported by our findings.25 11β-HSD type 2 enzyme converts both maternally derived cortisol and that synthesized by the fetus to biologically inactive cortisone in order to maintain delicate cortisol homeostasis at low cord cortisol concentrations. The placenta and kidney have high expression of 11β-HSD type 2 protecting the fetus from glucocorticoid excess.26 We have demonstrated a progressive decline in the cortisone/cortisol ratio, indicating a progressive decrease in 11β-HSD type 2 enzyme activity over the first 6 months of infancy. This adaptation is probably one of the main mechanisms leading to sufficient cortisol concentration in the circulation of young infants. In parallel with this finding, we have also shown a longitudinal improvement of CYP21A2, CYP11B1, and HSD3B2 enzyme activities, which would favor the production of cortisol. All of these changes contribute to the maintenance of adequate plasma cortisol concentrations during the maturation of the neonatal adrenal cortex.
11-Deoxycorticosterone and corticosterone have weaker mineralocorticoid activity than aldosterone, but their measurement provides important diagnostic information about certain forms of adrenal disorders, including CYP17A1 and aldosterone synthase deficiency.27,28 Nevertheless, reference values for these metabolites are also scarce. Hence, the establishment of reference values for 11-deoxycorticosterone and corticosterone in the present study will facilitate the clinical diagnosis of these rare forms of CAH, which are characterized by changes in these metabolites.
In the system of interlinked pathways in adrenal steroidogenesis, the concentration of a metabolic intermediate is determined by its production and disappearance rates. Therefore, the concentration of an intermediate alone cannot precisely predict the changes in abnormality in adrenal enzyme activity. In light of this, the precursor-to-product ratios can be used as surrogate measures of steroidogenetic enzyme activities. Although repeated measures on the same infants would have reflected temporal changes in the steroid concentrations more reliably, in this cross-sectional study, we provided ample normative data for the precursor-to-product ratios. The diagnostic validity of these ratios was tested in genetically confirmed CAH cohorts.10,21 It is important to note that in cases with CAH even the lowest value of these ratios are at least several folds above the highest values in the healthy group allowing identification of the patients quite easily. These patients, who presented in early infancy, have achieved a fast and accurate biochemical diagnosis in a single run test with LC-MS/MS.
In conclusion, we have demonstrated significant, age-related changes in the majority of the adrenal steroid hormones over the first 6 months of infancy, which reflect the changes in adrenal morphology and steroidogenic enzyme expression. The comprehensive reference intervals of steroid concentrations using LC-MS/MS established in this study will be valuable in the diagnosis of steroidogenic disorders, which mostly present within the first months of life. The data generated in this study will also be useful for the evaluation of infants recalled by neonatal CAH screening programmes.
References
Xing, Y., Lerario, A. M., Rainey, W. & Hammer, G. D. Development of adrenal cortex zonation. Endocrinol. Metab. Clin. N. Am. 44, 243–274 (2015).
Krone, N. in Oxford Textbook of Endocrinology (eds Wass, J. A. H. & Stewart, P. M.) 865–878 (Oxford Univ. Press, 2011).
Rauh, M. Steroid measurement with LC-MS/MS. Application examples in pediatrics. J. Steroid Biochem. Mol. Biol. 121, 520–527 (2010).
Taylor, A. E., Keevil, B. & Huhtaniemi, I. T. Mass spectrometry and immunoassay: how to measure steroid hormones today and tomorrow. Eur. J. Endocrinol. 173, D1–D12 (2015).
Soldin, O. P., Sharma, H., Husted, L. & Soldin, S. J. Pediatric reference intervals for aldosterone, 17alpha-hydroxyprogesterone, dehydroepiandrosterone, testosterone and 25-hydroxy vitamin D3 using tandem mass spectrometry. Clin. Biochem. 42, 823–827 (2009).
Kushnir, M. M. et al. Liquid chromatography-tandem mass spectrometry assay for androstenedione, dehydroepiandrosterone, and testosterone with pediatric and adult reference intervals. Clin. Chem. 57, 1138–1147 (2010).
Kyriakopoulou, L. et al. A sensitive and rapid mass spectrometric method for the simultaneous measurement of eight steroid hormones and CALIPER pediatric reference intervals. Clin. Biochem. 46, 642–651 (2013).
Kulle, A. E., Welzel, M., Holterhus, P. M. & Riepe, F. G. Implementation of a liquid chromatography tandem mass spectrometry assay for eight adrenal C-21 steroids and pediatric reference data. Horm. Res. Paediatr. 79, 22–31 (2013).
Kulle, A. E., Reinehr, T., Simic-Schleicher, G., Hornig, N. C. & Holterhus, P. M. Determination of 17OHPreg and DHEAS by LC-MS/MS: impact of age, sex, pubertal stage, and BMI on the Δ5 steroid pathway. J. Clin. Endocrinol. Metab. 102, 232–241 (2017).
Fiet, J. et al. A liquid chromatography/tandem mass spectometry profile of 16 serum steroids, including 21-deoxycortisol and 21-deoxycorticosterone, for management of congenital adrenal hyperplasia. J. Endocr. Soc. 1, 186–201 (2017).
Bae, Y. J. et al. Reference intervals of nine steroid hormones over the life-span analyzed by LC-MS/MS: effect of age, gender, puberty, and oral contraceptives. J. Steroid Biochem. Mol. Biol. 193, 105409 (2019).
Guran, T. et al. Revisiting classical 3β-hydroxysteroid dehydrogenase 2 deficiency: lessons from 31 pediatric cases. J. Clin. Endocrinol. Metab. 105, dgaa022 (2020).
Dhayat, N. A. et al. Estimation of reference curves for the urinary steroid metabolome in the first year of life in healthy children: tracing the complexity of human postnatal steroidogenesis. J. Steroid Biochem. Mol. Biol. 154, 226–236 (2015).
Wright, E. M. & Royston, P. Simplified estimation of age-specific reference intervals for skewed data. Stat. Med. 16, 2785–2803 (1997).
Schielzeth, H. et al. Robustness of linear mixed-effects models to violations of distributional assumptions. Methods Ecol. Evol. 11, https://doi.org/10.1111/2041-210X.13434 (2020).
Bates, D., Maechler, M., Bolker, B., & Walker, S. lme4: linear mixed-effects models using Eigen and S4. http://CRAN.R-project.org/package=lme4 (2014).
Shackleton, C., Pozo, O. J. & Marcos, J. GC/MS in recent years has defined the normal and clinically disordered steroidome: will it soon be surpassed by LC/tandem MS in this role? J. Endocr. Soc. 2, 974–996 (2018).
Webb, E. A. & Krone, N. Current and novel approaches to children and young people with congenital adrenal hyperplasia and adrenal insufficiency. Best. Pract. Res. Clin. Endocrinol. Metab. 29, 449–468 (2015).
Güran, T. et al. Neonatal screening for congenital adrenal hyperplasia in turkey: a pilot study with 38,935 infants. J. Clin. Res. Pediatr. Endocrinol. 11, 13–23 (2019).
Güran, T. et al. Neonatal screening for congenital adrenal hyperplasia in Turkey: outcomes of extended pilot study in 241,083 infants. J. Clin. Res. Pediatr. Endocrinol. 12, 287–294 (2020).
Christakoudi, S., Cowan, D. A., Christakudis, G. & Taylor, N. F. 21-Hydroxylase deficiency in the neonate—trends in steroid anabolism and catabolism during the first weeks of life. J. Steroid Biochem. Mol. Biol. 138, 334–347 (2013).
El-Maouche, D., Arlt, W. & Merke, D. P. Congenital adrenal hyperplasia. Lancet 390, 2194–2210 (2017).
Chan, C. L. et al. Congenital adrenal hyperplasia and the second newborn screen. J. Pediatr. 163, 109–13.e1 (2013).
Dhayat, N. A. et al. Androgen biosynthesis during minipuberty favors the backdoor pathway over the classic pathway: Insights into enzyme activities and steroid fluxes in healthy infants during the first year of life from the urinary steroid metabolome. J. Steroid Biochem. Mol. Biol. 165, 312–322 (2017).
Taylor, N. F., Curnow, D. H. & Shackleton, C. H. Analysis of glucocorticoid metabolites in the neonatal period: catabolism of cortisone acetate by an infant with 21-hydroxylase deficiency. Clin. Chim. Acta 85, 219–229 (1978).
Fahlbusch, F. B., Ruebner, M., Rascher, W. & Rauh, M. Combined quantification of corticotropin-releasing hormone, cortisol-to-cortisone ratio and progesterone by liquid chromatography-Tandem mass spectrometry in placental tissue. Steroids 78, 888–895 (2013).
Riepe, F. G., Krone, N., Peter, M., Sippell, W. G. & Partsch, C. J. Chromatographic system for the simultaneous measurement of plasma 18-hydroxy-11-deoxycorticosterone and 18-hydroxycorticosterone by radioimmunoassay: reference data for neonates and infants and its application in aldosterone-synthase deficiency. J. Chromatogr. B 785, 293–301 (2003).
Biglieri, E. G. & Kater, C. E. Mineralocorticoids in congenital adrenal hyperplasia. J. Steroid Biochem. Mol. Biol. 40, 493–499 (1991).
Janzen, N. et al. Newborn screening for congenital adrenal hyperplasia: additional steroid profile using liquid chromatography-tandem mass spectrometry. J. Clin. Endocrinol. Metab. 92, 2581–2589 (2007).
Acknowledgements
We would like to acknowledge the subjects and their families without whom this study could not have been performed. The authors would like to thank Prof. Richard Auchus for reading the manuscript and for his valuable suggestions. The authors would also like to thank Mr. Jeremy Jones for his assistance in editing the English used.
Funding
We acknowledge funding by Marmara University Research Committee Grant (SAG-C-TUP-131216-0528 to E.E.O). This work has been supported by the Medical Research Council of Marmara University (SAG-C-TUP-131216-0528 to E.E.O.).
Author information
Authors and Affiliations
Contributions
Conceptualization: T.G., E.E.O., A.B.; study design: T.G., E.E.O., A.B., G.H.; investigation: P.V., E.E.O., O.G., L.B.; data analysis: T.G., A.B., E.E.O.; funding acquisition: E.E.O., T.G.; resources: O.G., L.B., P.B.; supervision: G.H., A.B., T.G.; writing—original draft: E.E.O., T.G., A.B., G.H., A.B.; writing—review and editing: A.B., S.T., T.G.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Patient consent
Parents provided written informed consent, and all studies were conducted in accordance with the principles of the Declaration of Helsinki
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Enver, E.O., Vatansever, P., Guran, O. et al. Adrenal steroids reference ranges in infancy determined by LC-MS/MS. Pediatr Res 92, 265–274 (2022). https://doi.org/10.1038/s41390-021-01739-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-021-01739-5