Abstract
Background
This research characterized mucociliary clearance (MCC) in young children with cystic fibrosis (CF).
Methods
Fourteen children (5–7 years old) with CF underwent: two baseline MCC measurements (Visits 1 and 2); one MCC measurement approximately 1 year later (Visit 3); and measurements of lung clearance index (LCI), a measure of ventilation inhomogeneity.
Results
Median (range) percent MCC through 60 min (MCC60) was similar on Visits 1 and 2 with 11.0 (0.9–33.7) and 12.8 (2.7–26.8), respectively (p = 0.95), and reproducible (Spearman Rho = 0.69; p = 0.007). Mucociliary clearance did not change significantly over 1 year with median percent MCC60 on Visit 3 [12.8 (3.7–17.6)] similar to Visit 2 (p = 0.58). Lower percent MCC60 on Visit 3 was significantly associated with higher LCI scores on Visit 3 (N = 14; Spearman Rho = −0.56; p = 0.04).
Conclusions
Tests of MCC were reproducible and reliable over a 2-week period and stable over a 1-year period in 5–7-year-old children with CF. Lower MCC values were associated with increased ventilation inhomogeneity. These results suggest that measurements of MCC could be used in short-term clinical trials of interventions designed to modulate MCC and as a new, non-invasive test to evaluate early lung pathology in children with CF.
Impact
-
This is the first study to characterize mucociliary clearance (MCC) in children with cystic fibrosis (CF) who were 5–7 years old.
-
Measurements of mucociliary clearance were reproducible and reliable over a 2-week period and stable over a 1-year period.
-
Variability in MCC between children was associated with differences in ventilation homogeneity, such that children with lower MCC values had increased ventilation inhomogeneity.
-
These results suggest that measurements of MCC could be used in short-term clinical trials of interventions designed to modulate MCC and as a new, non-invasive test to evaluate early lung pathology in children with CF.
Similar content being viewed by others
Introduction
Currently, the state-of-the-art, non-invasive method for evaluating lung pathology in people with cystic fibrosis (CF) is pulmonary function testing. However, many children who are <6 years of age cannot perform this test and physicians must rely on radiologic tests, oropharyngeal cultures, and cultures of bronchoalveolar lavage to assess lung disease objectively in this population. A non-invasive test that young children can perform is needed to impartially evaluate early lung pathology in CF.
Mucociliary clearance (MCC) measurements are non-invasive, and defective MCC is an integral step in the pathogenesis of CF lung disease. Mutations in the CF transmembrane conductance regulator (CFTR) gene lead to impaired mucus removal, accumulation of bacteria and fungi in the airways, and infection.1,2,3,4 Chronic infection of the airways is the major cause of morbidity and mortality.5
Previously, we have measured MCC in children with CF who are ≥7 years of age and found that MCC declines significantly when quantified over several years,6 and lower MCC values are associated with higher incidence of infection with Pseudomonas aeruginosa (PA), increased ventilation inhomogeneity, and increased peripheral lung damage.6,7 However, MCC has not been characterized in children with CF who are ≤7 years old. Thus, it is unknown whether younger children can perform the procedure and whether results are reproducible. It is also unknown whether MCC values in this population change over time and what factors lead to variability in MCC measurements.
We hypothesized that: (1) MCC measurements are reproducible and reliable in children with CF who are 5–7 years old; (2) MCC values decline significantly over a 1-year period; and (3) variability in MCC is associated with PA infection history, mucus composition, ventilation inhomogeneity, and/or peripheral lung damage. In two exploratory analyses, we examined variability in MCC in relation to environmental exposures and variants in genes related to pulmonary phenotype in CF or MCC. Results from these experiments would determine whether MCC measurements can be performed in young children with CF and whether they provide a novel test to evaluate early lung pathology.
Materials and methods
Study overview
The study consisted of Visits 1 and 2 during a 2-week period and Visit 3 approximately 1 year later. All visits were approved by the Johns Hopkins Institutional Review Board. Written, informed consent was obtained from parents, or guardians, of children who participated in the study. An historic group of adult subjects who had undergone an MCC procedure previously in our laboratory8 served as controls for MCC measurements.
Eligibility criteria for children with CF
(1) Males and females between the ages of 5 and 7 years; (2) diagnosis of CF by sweat chloride >60 meq/L or by the presence of two CFTR mutations known to cause CF; and (3) forced expiratory volume in 1 s (FEV1) ≥80% predicted. Children who could not perform spirometry reliably or whose FEV1 was <80% predicted were eligible if they had a minimal history of infection and chronic symptoms, as determined by a physician investigator.
Eligibility criteria for controls
Controls were healthy, nonsmoking adults with no history, or evidence, of lung disease.
Use of concomitant therapies
Use of concomitant therapies was documented through chart review. Short-acting bronchodilators, dornase alfa, and airway clearance with high-frequency chest wall oscillation were discontinued for 12 h and hypertonic saline for 72 h before all three study visits. Treatment with lumacaftor/ivacaftor was not discontinued. Visits were scheduled at least 2 weeks following completion of antibiotic treatment for a pulmonary exacerbation.
Lung function measurements
Initially, the protocol did not include spirometry. This was amended after the first child completed Visits 1 and 2. For all other children, FEV1 was measured on Visits 1 and 3, after MCC, using a MicroLab Mk8 spirometer (MD Spiro; Lewiston, ME), according to accepted guidelines.9 FEV1 was reported as percent of predicted values, calculated using Global Lung Function Initiative 2012 equations.10
High-resolution computed tomography (HRCT) lung scan
Peripheral lung damage was assessed from HRCT scans performed on Visit 3 and scored as described by Brody et al.11 A total combined score for severity of bronchiectasis, mucous plugging, peribronchial thickening, air trapping, and parenchymal opacities in both lungs was reported. HRCT scans were not performed on Visit 1 to avoid additional radiation exposure.
Multiple breath washout (MBW) test
MBW tests measure lung ventilation inhomogeneity.12 Lung clearance index (LCI), measured by MBW, is considered to be a more sensitive indicator of early lung disease than FEV1.13,14,15,16,17 Ventilation inhomogeneity was evaluated after MCC on Visits 1 and 3, in terms of absolute LCI2.5%, according to consensus guidelines.12 MBW tests were performed using the EXHALYZER® D (ECO Medics AG; Bubikonerstrasse, Switzerland).
PA infection and hospitalization history
Age of initial PA+ culture, number of PA+ cultures/year, and percent of respiratory cultures per year that were PA+ prior to Visit 2 and between Visits 2 and 3 were documented through chart review. Number of hospitalizations for a pulmonary exacerbation and/or treatment with antibiotics between Visits 2 and 3 were documented through questionnaires and review of medical records.
Environmental exposures
Caregivers completed questionnaires documenting their child’s exposure to pets, pests, secondhand tobacco smoke, gas combustion in the home, and respiratory syncytial virus (RSV) infection prior to Visits 2 and 3.
Genes of interest
The following genes were of interest. Each could have a deleterious clinical effect on CF lung disease: TGFβ1,18 MBL2,19 MUC4/MUC20,20,21 SLC9A3,20 AGTR2/SLC6A14,20 EHF/APIP,22 DNAH14, DNAAF3, DNAH6,23 DCNT4,24 MUC5AC,25 and MUC5B.26
Genetic testing
Blood was collected on Visit 1. DNA was sequenced by Broad Genomics (Cambridge, MA) using bead-based capture. Genetic variants were called using the Genomic Analysis Tool Kit (GATK) pipeline (Broad Genomics). All samples passed sample quality thresholds for contamination, chimera rate, and coverage, and only variants that passed Variant Quality Score Recalibration conducted by Broad Genomics were assessed. Variants in genes of interest were annotated with cDNA and protein change and frequency. Null variants (i.e., nonsense, frameshift, canonical+/−1, or 2, splice sites, initiation codon, single exon, or multi-exon deletion) and candidate variants (i.e., reported in the literature27,28 or pathogenic in ClinVar29) were evaluated.
Mucus composition
Sputum samples were collected on Visit 1, after MCC, using a standardized sputum induction procedure.30 MUC5B and MUC5AC quantities were determined by dot-blot enzyme-linked immunosorbent assay, using rabbit-anti-MUC5B (H-300, Santa Cruz Biotechnology, 1:5000) and rabbit anti-MUC5AC (MAN5AC, provided by Dr. David Thornton, University of Manchester, 1:2000). Irrelevant rabbit antisera used to verify observed signals were specific for each primary antibody, when used at the dilutions above. Standard curves for MUC5B were calibrated against mucin purified from human saliva (provided by Dr. Thornton). Standard curves for MUC5AC were generated using a sputum sample from a previous study.6 Because MUC5AC standards were not tested against the purified protein, MUC5AC data are presented in arbitrary units rather than mass concentrations.
Quantification of MCC
MCC was quantified immediately following inhalation of an aerosol containing the radioisotope 99mtechnetium sulfur-colloid (radioaerosol) and for 90 min thereafter, using a gamma camera.6,8,31 On all three visits, MCC endpoints were calculated for the right lung as average percent clearance through 60 min (MCC60) and 90 min (MCC90), as described previously.6,8,31 Between 60 and 90 min, children performed 30 programmed coughs.9
Radioaerosol deposition pattern
To determine whether MCC was influenced by the initial radioaerosol deposition pattern, we compared deposition in outer (O) and inner (I) regions of the lung for each visit as described previously.6,31 Deposition patterns were compared in terms of outer:inner (O:I) ratio, as recommended by a consensus of imaging experts.32
Sample size
Based on demographics of patients who attended the Johns Hopkins CF Clinic at the time of study design, we estimated that there would be approximately 35 eligible children on the projected study start date and approximately 20 of those children would be willing to participate in the study. The sample size of 20 was fixed by this estimate.
Statistical analysis
The following primary endpoints were selected a priori according to a pre-study protocol: percent MCC60 and MCC90, FEV1 percent predicted, absolute LCI2.5%, HRCT score, O:I ratio, PA infection history, and MUC5B and MUC5AC concentrations.
Due to the small sample size, all MCC, FEV1, LCI2.5%, HRCT, O:I ratio, PA, MUC5B, and MUC5AC data are presented as median (minimum–maximum) and non-parametric tests were used to test for statistical differences in comparisons and associations.
Data from Visits 1 and 2 were used to determine MCC reproducibility and reliability over the 2-week period. Data from Visit 2 were used for comparisons with data obtained on Visit 3 and for comparisons with other endpoints obtained during the 2-week period. We chose not to average MCC data on Visits 1 and 2 for comparisons because an average could lead to an artificially more stable estimate of the baseline value. We chose not to use MCC data from Visit 1 for comparisons for the following reason. Consistency in performing the breathing maneuvers during radioaerosol administration is key to reproducible aerosol deposition in the lungs, which leads to more reproducible MCC results. Children were first introduced to the breathing maneuvers on Visit 1. On Visit 2, children remembered the breathing maneuvers learned on Visit 1 and became more proficient with additional practice. We assumed the additional proficiency gained on Visit 2 would lead to the most reproducible results for comparisons.
Ad hoc comparisons were performed between percent MCC60 and O:I from historic controls8 and children with CF in the current study. Comparisons between percent MCC90 for the two groups were not performed because control subjects coughed 60 times between 60 and 90 min and children with CF coughed 30 times.
Reliability of MCC measurements was quantified in terms of intraclass correlation coefficients (ICCs), with ICCs >0.70 indicating good reliability.33
In the two exploratory analyses, we examined variability in MCC60 and MCC90 in relation to different environmental exposures and variants in genes related to pulmonary phenotype in CF or MCC. Associations between each environmental exposure (independent variable) and percent MCC60 or percent MCC90 (dependent variable) were assessed using mixed effects models adjusted for sex and age and nested by individual to account for values obtained on Visits 2 and 3.
Analyses were performed using SAS version 9.4 (SAS Institute, Inc., Cary, North Carolina), Microsoft Excel 2016, or Stata IC 14 (College Station, TX). All tests were two sided and significance was set at p < 0.05.
Results
Timeline
Visits 1 and 2 occurred between April 2014 and September 2018. Visit 3 occurred between July 2015 and July 2019.
Children with CF
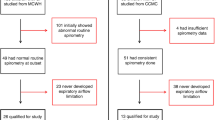
At the start of the project, the number of eligible children who attended the CF Clinic at Johns Hopkins was less than projected. To increase recruitment capabilities, we added two additional sites: the CF Centers at Walter Reed National Military Medical Center (Bethesda, MD) and Children’s Hospital Colorado (Aurora, CO). Nevertheless, we were only able to enroll 17 children from all 3 sites and 3 of the children discontinued their participation before completing any study visits. Therefore, a total of 14 children (n = 5 males) completed all 3 study visits. Nine children were referred by the CF Clinic at Johns Hopkins. Three children were referred by Walter Reed National Military Medical Center and two children were referred by Children’s Hospital Colorado.
Thirteen children were between 5 and 6 years old and one child was 7 years old at the time of Visits 1 and 2. Median age at Visit 1 was 5.7 (5.2–7.2) years. Two children were full genetic siblings. Twelve children were Caucasians. Seven of the 14 children were homozygous for F508del CFTR mutations. Five children had one F508del CFTR mutation, including one residual function mutation (R117H). Two children had no F508del CFTR mutations but other minimal function mutations. Those genotypes were I507del/621+1G>T and exon 2,3 del/R553X. Thirteen children were pancreatic insufficient.
Control subjects
There were 10 control subjects for the MCC60 measurements (n = 6 males). Median age was 24 (18–37) years. Median FEV1 was 103% predicted (82–115).
Use of concomitant therapies in children with CF
The use of concomitant therapies is shown in Table 1. The effect of treatment with lumacaftor/ivacaftor varied between children. In the two children treated with lumacaftor/ivacaftor at the time of Visit 2, percent MCC60 on Visit 2 was faster in one child and slower in the other, with 26.8 and 5.0%, respectively. In the five children treated with lumacaftor/ivacaftor after Visit 2, MCC60 at Visit 3 was slower compared to Visit 2 in two children and faster in three children.
Reproducibility, reliability, and stability of MCC measurements in children with CF
Percent MCC60 and MCC90 on Visits 1 and 2 are shown in Fig. 1a, b. Median number of days between the two visits was seven (4–14). Median percent MCC60 and MCC90 were similar on Visits 1 and 2 (Table 2).
Comparison of percent MCC60 (a) and MCC90 (b) for each of the 14 children on Visits 1 and 2. Visit 1 is represented as (1) and Visit 2 is represented as (2). Horizontal black lines represent median values. MCC60 and MCC90 were similar on the two visits (p = 0.95 and p = 0.99, respectively). MCC60 is average percent mucociliary clearance through 60 min, MCC90 is average percent mucociliary clearance through 90 min. p Values were determined by Wilcoxon signed-rank tests.
Percent MCC60 on Visit 1 was correlated with percent MCC60 on Visit 2 and 10/14 data points fell on, or near, the line of identity, indicating good reproducibility (Fig. 2a). Percent MCC90 on Visit 1 was also correlated with percent MCC90 on Visit 2 (Spearman Rho = 0.73, p = 0.003; data not shown). ICCs for the two MCC60 and MCC90 measurements were 0.72 and 0.77, respectively, indicating good reliability.
a Line of identity for average percent MCC60 measurements (N = 14 pairs) on Visits 1 and 2. Visit 1 is represented as (1) and Visit 2 is represented as (2). Percent MCC60 on the two visits was significantly correlated (p = 0.007). A similar result was obtained for MCC90 (rs = 0.73; p = 0.003; data not shown). b Line of identity for average percent MCC60 measurements (N = 14 pairs) on Visits 2 and 3. Visit 2 is represented as (2) and Visit 3 is represented as (3). Percent MCC60 on the two visits was not significantly correlated (p = 0.32). A similar result was obtained for MCC90 (rs = 0.14; p = 0.63; data not shown). rs values were determined by Spearman correlation test. MCC60 average percent mucociliary clearance through 60 min, MCC90 average percent mucociliary clearance through 90 min.
There was no significant difference between percent median MCC60 and MCC90 on Visits 2 and 3, showing stability over the 1-year period (Table 2). However, percent MCC60 on Visit 2 was not correlated with MCC60 on Visit 3 and intra-subject variability in MCC varied considerably over the longer time period (Fig. 2b). Percent MCC90 on Visit 2 also was not correlated with MCC90 on Visit 3 (Spearman Rho = 0.14, p = 0.63; data not shown). ICCs for the two MCC60 and MCC90 measurements were 0.25 and 0.17, respectively, indicating poor reliability.
Outer:inner (O:I) ratios
O:I ratios on Visits 1 and 2 were similar (Table 2) and significantly correlated (Fig. 3a), indicating good reproducibility. ICC for these O:I measurements was 0.72, indicating good reliability. O:I ratios on Visits 2 and 3 were also similar (Table 2). However, O:I ratios on Visits 2 and 3 were not correlated (Fig. 3b), indicating poor reproducibility, and the ICC for these O:I measurements was 0.35, indicating poor reliability. There were no significant associations between O:I ratio and MCC60 on any of the three visits (Spearman Rho = 0.26; p = 0.38; −0.38; p = 0.18 and −0.18; p = 0.53 on Visits 1, 2, and 3, respectively). Similar results were obtained for O:I ratio and MCC90 (Spearman Rho = 0.24, p = 0.40; −0.40, p = 0.16; and −0.17, p = 0.57 on Visits 1, 2, and 3, respectively).
a Line of identity for O:I ratio (N = 14 pairs) on Visits 1 and 2. Visit 1 is represented as (1) and Visit 2 is represented as (2). O:I ratio on the two visits was significantly correlated (p = 0.008). b Line of identity for O:I ratio (N = 14 pairs) on Visits 2 and 3. Visit 2 is represented as (2) and Visit 3 is represented as (3). O:I ratio on the two visits was not significantly correlated (p = 0.38). rs value was determined by Spearman correlation test. O:I ratio percent of radioactivity deposited in outer region of right lung divided by percent of radioactivity deposited in inner region of right lung.
Absolute change in O:I ratio on Visits 2 and 3 was significantly related to absolute change in MCC90 on Visits 2 and 3. Greater changes in O:I ratio were significantly correlated with greater changes in MCC90 (Spearman Rho = 0.56, p = 0.04). Absolute change in O:I ratio on Visits 2 and 3 was similarly associated with absolute change in MCC60. However, that relationship was not statistically significant (Spearman Rho = 0.51, p = 0.06).
Ad hoc analysis in controls subjects
Median percent MCC60 for control subjects was 12.4 (0.7–19.7), which was similar to median percent MCC60 reported for children with CF on Visit 2 (Table 2; Mann–Whitney U test; p = 0.73). Median O:I for control subjects was 0.52 (0.24–0.83), which was similar to median O:I reported for children with CF on Visit 2 (Table 2; Mann–Whitney U test; p = 0.33).
Relationship between MCC and age of initial PA+ culture
Seven children were PA− prior to Visit 2. Age of initial PA+ culture in the other seven children was 21 (3–69) months. There were no statistically significant associations between age of initial PA+ culture and percent MCC60, or MCC90, on Visit 2 (Spearman Rho = −0.20, p = 0.50 and −0.17, p = 0.57, respectively) (n = 14).
Relationship between MCC and PA+ cultures/year
Number of bacterial cultures performed/year prior to Visit 2 was 3.6 (1.1–8.0). Number of PA+ cultures/year prior to Visit 2 was 0.06 (0–1.08). Percent MCC60 and MCC90 in children with zero PA cultures/year prior to Visit 2 were not significantly different from MCC60 and MCC90 in children with positive PA cultures prior to Visit 2 (Mann–Whitney U test; p = 0.57 and p = 0.52, respectively). Percent MCC60 and MCC90 on Visit 2 were not significantly associated with number of PA+ cultures/year prior to Visit 2 (Spearman Rho = −0.33, p = 0.24 and −0.36, p = 0.21, respectively) or with percent of respiratory cultures that were PA+/year, prior to Visit 2 (Spearman Rho = −0.24, p = 0.40 and −0.28, p = 0.34, respectively) (n = 14).
Ten children were PA− between Visits 2 and 3. Median number of bacterial cultures performed between Visits 2 and 3 was 5.0 (1.0–8.0). Median number of PA+ cultures/year between Visits 2 and 3 was 0 (0–1.2). Percent MCC60 and MCC90 on Visit 3 were not significantly associated with the number of PA+ cultures/year between Visits 2 and 3 (Spearman Rho = 0.35, p = 0.22 and 0.28, p = 0.33, respectively) or with percent of respiratory cultures that were PA+/year between Visits 2 and 3 (Spearman Rho = 0.35; p = 0.22 and 0.28; p = 0.32, respectively).
Relationship between MCC, MUC5B, MUC5AC, and MUC5AC/MUC5B
Three children could not produce a sputum sample. Concentrations of MUC5B, MUC5AC, and MUC5AC/MUC5B in the sputa were, therefore, determined from the remaining 11 children. Concentrations of MUC5B and MUC5AC were 77.6 µg/mL (3.1–245.4) and 65.6 AU/mL (4.6–3984.0), respectively. Ratios of MUC5AC/MUC5B were 1.0 (0.4–16.23). There were no significant associations between MUC5B, MUC5AC, or MUC5AC/MUC5B and the number of PA+ cultures/year prior to Visit 2 (Spearman Rho = 0.49, p = 0.12; 0.03, p = 0.92; and −0.03, p = 0.93, respectively). Percent MCC60 was not significantly correlated with MUC5B, MUC5AC, or MUC5AC/MUC5B (Spearman Rho = −0.40; p = 0.22; −0.01, p = 0.98; and −0.03, p = 0.94, respectively). Percent MCC90 was not significantly correlated with MUC5B, MUC5AC, or MUC5AC/MUC5B (Spearman Rho = −0.46, p = 0.16; −0.01, p = 0.98; and 0.05, p = 0.89, respectively).
Relationship between MCC and LCI2.5%
LCI2.5% was measured in 13 children on Visit 1 (Year 1) and in 14 children on Visit 3 (Year 2). Median LCI2.5% increased from 7.7 to 8.2 between Visits 1 and 3 (n = 13) but was not statistically different on the two visits (Table 2).
Percent MCC60 on Visit 2 was not significantly associated with LCI2.5% in Year 1 (Fig. 4a), whereas lower percent MCC60 on Visit 3 was associated with higher LCI2.5% in Year 2 (Fig. 4b). Lower percent MCC90 on Visit 2 was associated with higher LCI2.5% in Year 1 (Fig. 5a), whereas percent MCC90 on Visit 3 was non-significantly associated with LCI2.5% in Year 2 (Fig. 5b).
a Non-significant correlation between percent MCC60 on Visit 2 (2) and LCI2.5% in Year 1 (N = 13) (p = 0.09). b Significant correlation between percent MCC60 on Visit 3 (3) and LCI2.5% in Year 2 (N = 14) (p = 0.04). Linear trendlines, or best-fit straight lines, for the data, are included. rs values were determined by Spearman correlation test. MCC60 average percent mucociliary clearance through 60 min.
a Significant correlation between percent MCC90 on Visit 2 (2) and LCI2.5% in Year 1 (N = 13) (p = 0.02). b Non-significant correlation between percent MCC60 on Visit 3 (3) and LCI2.5% in Year 2 (N = 14) (p = 0.07). Linear trendlines, or best-fit straight lines, for the data, are included. rs values were determined by Spearman correlation test. MCC90 average percent mucociliary clearance through 90 min.
Correlation tests between the directional change in percent MCC60 and percent MCC90 and the directional change in LCI2.5% between Years 1 and 2 showed no significant associations (Spearman Rho = 0.06, p = 0.86 and 0.03, p = 0.92, respectively).
Relationship between MCC and FEV1
FEV1 was obtained in 12 of the 14 children on Visit 1. Spirometry was not included in the protocol at the time of Visit 1 for one child and one child could not perform spirometry reliably. FEV1 was <80% predicted in 2 of the 12 children, with 75.1 and 76.9%, respectively. All four children remained in the study because they had a minimal history of infection and no chronic symptoms.
FEV1 values for the 12 children were similar on Visits 1 and 3 (Table 2). Percent MCC60 and MCC90 on Visit 2 were not significantly associated with FEV1 values measured on Visit 1 (Spearman Rho = −0.09, p = 0.78 and −0.06, p = 0.85, respectively). Percent MCC60 and MCC90 on Visit 3 were not significantly associated with FEV1 values measured on Visit 3 (Spearman Rho = −0.22, p = 0.45 and −0.32, p = 0.27, respectively).
Relationship between MCC and HRCT scores
HRCT scans were performed in 14 children on Visit 3. Median HRCT score for both lungs combined was 5.0 (0–58.0). There was no evidence of mucus plugging (n = 10) or bronchiectasis (n = 6) in either lung. Percent MCC60 and MCC90 on Visit 3 were not significantly associated with HRCT scores on Visit 3 (Spearman Rho = −0.10, p = 0.75 and −0.16, p = 0.59, respectively).
Relationship between MCC and genetic variants
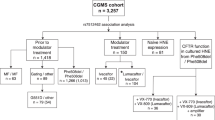
Null variants and candidate variants were identified in the following genes: MBL2, DNAH14, MUC5B, MUC5AC, and APIP. Seven children carried at least one candidate variant. Four children carried one null variant. The genetic variant and the number of individuals with each is shown in Table 3A, B. Two variants were identified in three individuals (#3, #4, and #13). Three variants were identified in one individual (#9). Median MCC60 and MCC90 on Visit 2 were not significantly different in children with no candidate variants [14.7 (2.7–26.8) and 18.9 (3.5–29.1), respectively], compared to children with at least one variant [10.3 (5.0–25.1) and 13.4 (6.9–29.8), respectively] (Mann–Whitney U test; p = 0.28 and p = 0.37, respectively). The sample size was too small to test for differences between MCC endpoints in children with one null variant.
Relationship between MCC and environmental exposures
Table 4 shows the percent of children whose caregivers reported exposures to pets, pests, secondhand smoke, gas combustion in the home, and RSV infection prior to Visits 2 and/or 3. MCC was not significantly associated with any of these exposures (Table 5).
Discussion
To our knowledge, this is the first study to show that mucus clearance from the lungs by ciliary mechanisms (MCC60) and ciliary/cough mechanisms combined (MCC90) can be measured and is reproducible and reliable over a 2-week period in 5–7-year-old children with CF. In addition, median MCC60 for these children, as well as the range of values, appear to be normal, since they were similar to values observed in a group of healthy, adult controls. Healthy, aged-matched children would have been the preferred control group. However, ethical considerations do not allow healthy children to be exposed to ionizing radiation for research purposes.
We hypothesized that MCC values would decline over the 1-year study period. However, this was not the case. Median MCC values for Visits 2 and 3 were not statistically different, indicating that MCC measurements were stable during this time period. Interestingly, PA infection rate in the majority of children was low over the 1-year period and there was only one hospitalization for a pulmonary exacerbation. This lack of infection with PA and hospitalization might account for the lack of a significant decline in MCC between Visits 2 and 3.
MCC measurements on Visits 2 and 3 were less reproducible and reliable than on Visits 1 and 2. These results suggest that the change in MCC over time varies and multiple observations will be most reproducible when made over a short time interval. Reduced reproducibility and reliability in MCC on Visits 2 and 3 could have been related to changes in the distribution of the radioaerosol used to measure MCC within the lung, possibly due to alterations in ventilation homogeneity. It is well known that changes in the deposition pattern of the radioaerosol, measured in this study in terms of O:I ratio, can influence MCC measurements32 and absolute change in MCC90 between the two visits was significantly associated with absolute change in O:I ratio.
LCI2.5% did not change significantly over the 1-year study period. However, MCC90 measurements on Visit 2 (Year 1) and MCC60 measurements on Visit 3 (Year 2) were significantly, negatively correlated with LCI2.5% values obtained at the same time points. These results suggest that variability in MCC is related to differences in ventilation homogeneity in this age group and lower MCC values are associated with increased ventilation inhomogeneity. It is unknown whether variability in MCC and changes in ventilation homogeneity are independent markers of lung disease or whether altered ventilation homogeneity impacts MCC tests directly via changes in deposition. It is also unclear why MCC60 on Visit 2 and MCC90 on Visit 3 were not correlated with LCI2.5% values. This could be due to the small number of study subjects.
Inter-subject variability in MCC measurements in these children does not appear to be due to differences in therapy, since the majority of children in the study were treated with similar drugs during the study protocol. A small number of children were treated with lumacaftor/ivacaftor during the study. However, the effect of this drug combination on MCC is unclear, since some children demonstrated faster clearance with treatment and others demonstrated slower clearance after starting the drug.
Inter-subject variability in MCC measurements was not associated with age of initial PA+ culture. This finding is similar to what we found in older children with CF.6 However, unlike the previous study, there was no significant association between MCC and PA infection rate. Also, unlike another study,7 there was no difference in MCC between children who were PA− vs. PA+, prior to the MCC test. It is unknown why variability in MCC in these young children was not associated with PA infection rate. However, only 4 of the 14 children in the present study were PA+ between Visits 2 and 3, with median PA+ cultures/year at zero. In the previous study,6 PA+ cultures/year between visits was much higher, averaging 0.90, and the time between visits was much longer with a median of 4.6 (3.1–10.0) years. This suggests that changes in MCC may be related to the length of time the infection is present. With such a low infection rate and short study period, it is not surprising that there was no association between MCC measurements and infection rate in the present study.
Similar to studies in older children with CF,6,7 FEV1 in these younger children did not change significantly during the 1-year study period and MCC measurements were not associated with FEV1 values.
In contrast to previous studies,6,7 there was no association between percent MCC and HRCT scores in these young children with CF. It is not clear why this was the case. However, the lack of an association could be due to the large percentage of children with scores of zero for both mucus plugging and bronchiectasis, two components of HRCT scoring that directly pertain to MCC. Additionally, the effects of changes in MCC on the parenchymal damage observed in CT scanning may be cumulative, such that abnormalities appear over time.6,7
Other investigators have compared MUC5B and MUC5AC concentrations in healthy adults and adults with CF. Henke et al. showed that MUC5AC and MUC5B are increased in adult patients with CF during a pulmonary exacerbation34 and Henderson et al. showed that concentrations of these two mucins are higher in young adults with CF who were infected with PA, compared to normal, uninfected adults.35 However, neither of these studies explored possible relationships between MCC and MUC5B and MUC5AC concentrations in these adults with CF.
To our knowledge, this is the first study to examine the relationship between MCC and these two mucins in young children with CF. Our results indicate that, during a period of stability (i.e., low infection rate with PA), MCC is not significantly related to MUC5B, or MUC5AC, concentrations, or MUC5B/MUC5AC ratio, measured in induced sputum in 5–7-year-old children with CF. Because of the small sample size, additional studies investigating the amounts and integrity of MUC5AC and MUC5B in larger cohorts are warranted.
In the two exploratory analyses, we found that MCC on Visit 2 was not significantly different in children with no candidate gene variants, compared to children with at least one variant. We also found no significant associations between MCC and reported environmental exposures.
In conclusion, this was the first study to characterize MCC in children with CF who were 5–7 years old. Findings from this study showed that measurements of MCC were reproducible and reliable over a 2-week period and stable over a 1-year period. In addition, variability in MCC between children was associated with differences in ventilation homogeneity, such that children with lower MCC values had increased ventilation inhomogeneity. These results suggest that measurements of MCC could be used in short-term clinical trials of interventions designed to modulate MCC and as a new, non-invasive test to evaluate early lung pathology in children with CF.
References
Hodson, M. E., Geddes, D. & Bush, A. Cystic Fibrosis 3rd edn (Hodder Arnold, 2007).
Matsui, H. et al. Evidence for periciliary liquid layer depletion, not abnormal ion composition, in the pathogenesis of cystic fibrosis airways disease. Cell 95, 1005–1015 (1998).
Matsui, H. et al. Reduced three-dimensional motility in dehydrated airway mucus prevents neutrophil capture and killing bacteria on airway epithelial surfaces. J. Immunol. 175, 1090–1099 (2005).
Ratjen, F. & Doring, G. Cystic fibrosis. Lancet 361, 681–689 (2003).
Davis, P. B., Drumm, M. & Konstan, M. W. Cystic fibrosis. Am. J. Respir. Crit. Care Med. 154, 1229–1256 (1996).
Laube, B. L. et al. Changes in mucociliary clearance over time on children with cystic fibrosis. Pediatr. Pulmonol. https://doi.org/10.1002/ppul.24858 (2020).
Laube, B. L., Sharpless, G., Benson, J., Carson, K. A. & Mogayzel, P. J. Jr. Mucus removal is impaired in children with cystic fibrosis who have been infected by Pseudomonas aeruginosa. J. Pediatr. 164, 839–845 (2014).
Bennett, W. et al. Multisite comparison of mucociliary and cough clearance measures using standardized methods. J. Aerosol Med. Pulm. Drug Deliv. 26, 157–164 (2013).
Miller, M. R. et al. ATS/ERS Task Force. Standardisation of spirometry. Eur. Respir. J. 26, 319–338 (2005).
Quanjer, P. H. et al. Multi-ethnic reference values for spirometry for the 3–95-yr age range: the global lung function 2012 equations. Eur. Respir. J. 40, 1324–1343 (2012).
Brody, A. S. et al. Reproducibility of a scoring system for computed tomography scanning in cystic fibrosis. J. Thorac. Imaging 21, 14–21 (2006).
Robinson, P. D. et al. Consensus statement for inert gas washout measurement using multiple- and single- breath tests. Eur. Respir. J. 41, 507–522 (2013).
Davies, J. C., Cunningham, S., Alton, E. W. & Innes, J. A. Lung clearance index in CF: a sensitive marker of lung disease severity. Thorax 63, 96–97 (2008).
Aurora, P. et al. Multiple-breath washout as a marker of lung disease in preschool children with cystic fibrosis. Am. J. Respir. Crit. Care Med. 171, 249–256 (2005).
Schaedel, C. et al. Predictors of deterioration of lung function in cystic fibrosis. Pediatr. Pulmonol. 33, 483–491 (2002).
Kraemer, R., Blum, A., Schibler, A., Ammann, R. A. & Gallati, S. Ventilation inhomogeneities in relation to standard lung function in patients with cystic fibrosis. Am. J. Respir. Crit. Care Med. 171, 371–378 (2005).
Gustafsson, P. M., De Jong, P. A., Tiddens, H. A. & Lindblad, A. Multiple-breath inert gas washout and spirometry versus structural lung disease in cystic fibrosis. Thorax 63, 129–134 (2008).
Cutting, G. R. Modifier genes in Mendelian disorders: the example of cystic fibrosis. Ann. NY Acad. Sci. 1214, 57–69 (2010).
Chalmers, J. D., Fleming, G. B., Hill, A. T. & Kilpatrick, D. C. Impact of mannose-binding lectin insufficiency on the course of cystic fibrosis: a review and meta-analysis. Glycobiology 21, 271–282 (2011).
Corvol, H., Cutting, G. R., Drumm, M. L., Knowles, M. R. & Strug, L. J. Genome-wide association meta-analysis in ~6,400 CF patients confirms previous findings and identifies new loci contributing to variation in lung disease. Pediatr. Pulmonol. 49, 271–272 (2014).
Kesimer, M. et al. Molecular organization of the mucins and glycocalyx underlying mucus transport over mucosal surfaces of the airways. Mucosal Immunol. 6, 379–392 (2013).
Wright, F. A. et al. Genome-wide association and linkage identify modifier loci of lung disease severity in cystic fibrosis at 11p13 and 20q13.2. Nat. Genet. 43, 539–546 (2011).
Blue, E. et al. Variation in cilia protein genes and progression of lung disease in cystic fibrosis. Ann. Am. Thorac. Soc. 15, 440–448 (2018).
Emond, M. J. et al. Exome sequencing of extreme phenotypes identifies DCTN4 as a modifier of chronic Pseudomonas aeruginosa infection in cystic fibrosis. Nat. Genet. 44, 886–889 (2013).
Evans, C. M. et al. The polymeric mucin Muc5ac is required for allergic airway hyperreactivity. Nat. Commun. 6, 6281 (2015).
Roy, M. G. et al. Muc5b is required for airway defense. Nature 505, 412–416 (2014).
Stock, C. J. et al. Mucin 5B promoter polymorphism is associated with idiopathic pulmonary fibrosis but not with development of lung fibrosis in systemic sclerosis or sarcoidosis. Thorax 68, 436–441 (2013).
Kamio, K. et al. Promoter analysis and aberrant expression of the MUC5B gene in diffuse panbronchiolitis. Am. J. Respir. Crit. Care Med 171, 949–957 (2005).
Landrum, M. J. et al. ClinVar: improving access to variant interpretations and supporting evidence. Nucleic Acids Res. 46, D1062–D1067 (2018).
Mayer-Hamblett, N. et al. Association between pulmonary function and sputum biomarkers in cystic fibrosis. Am. J. Respir. Crit. Care Med. 175, 822–828 (2007).
Laube, B. L., Carson, K. A., Sharpless, G., Paulin, L. M. & Hansel, N. N. Mucociliary clearance in former tobacco smokers with both chronic obstructive pulmonary disease and chronic bronchitis and the effect of Roflumilast. J. Aerosol Med. Pulm. Drug Deliv. 32, 189–199 (2019).
Newman, S. et al. Standardization of techniques for using planar (2D) imaging for aerosol deposition assessment of orally inhaled products. J. Aerosol Med. Pulm. Drug Deliv. 25, S10–S28 (2012).
Fleiss, J. L. In The Design and Analysis of Clinical Experiments 264–281 (Wiley, 1999).
Henke, M. O. et al. MUC5AC and MUC5B mucins increase in cystic fibrosis airway secretions during pulmonary exacerbation. Am. J. Respir. Crit. Care Med. 175, 816–821 (2007).
Henderson, A. G. et al. Cystic fibrosis airway secretions exhibit mucin hyperconcentration and increased osmotic pressure. J. Clin. Investig. 124, 3047–3060 (2014).
Acknowledgements
The authors wish to thank Douglas Walker for performing MBW and induced sputum tests and lung function procedures and Jane Benson, MD and Emily Dunn, MD for scoring HCRT scans. Douglas Walker, Jane Benson, and Emily Dunn were supported by the NIH (R01 HL129925). We also wish to thank Andrew Lipton, MD, Chief, Pediatric Pulmonology, the Walter Reed National Military Medical Center and his clinical coordinators, Funmilola Crawford and Jane Jacknewitz-Woolard, and Dr. Edith Zemanick, MD, Associate Professor, Pediatrics, University of Colorado Denver and her clinical coordinators, Dana Coyle and Meg Anthony, for their referrals to this study. B.L.L., K.A.C., J.M.C., P.J.M., P.L.Z., C.M.E. and G.S. were supported by the NIH (R01 HL129925). B.L.L. and K.A.C. were also supported by the Johns Hopkins Institute for Clinical and Translational Research, which was funded in part by the NIH (UL1 TR001079). C.M.E. and V.L.R. were supported by the NIH (R01 HL130938, R01 HL080396) and by the Cystic Fibrosis Foundation (CFF EVANS18I0).
Author information
Authors and Affiliations
Contributions
B.L.L., K.A.C., C.M.E., J.M.C., P.L.Z., G.R.C. and P.J.M. made substantial contributions to the study’s conception and design and analysis and interpretation of the data. M.A.A., V.L.R. and G.S. made substantial contributions to analysis and interpretation of the data. B.L.L. drafted the article. All authors contributed to revising the article critically for important intellectual content and all authors provided final approval of the version to be published.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Informed consent
Written, informed consent was obtained from parents, or guardians, of children who participated in the study. The study was approved by the Johns Hopkins Institutional Review Board.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Laube, B.L., Carson, K.A., Evans, C.M. et al. Characterizing mucociliary clearance in young children with cystic fibrosis. Pediatr Res 91, 612–620 (2022). https://doi.org/10.1038/s41390-021-01453-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-021-01453-2