Abstract
Background
The aims of this study were to find the normal value of fronto-temporal horn ratio (FTHR) as a marker of ventriculomegaly on cranial ultrasound (CUS) in premature newborns and the relation to white matter injury (WMI) and cerebral palsy (CP).
Methods
This is a retrospective study of newborns admitted between 2011 and 2014. Inclusion criteria were: (1) gestation <29 weeks, (2) birth weight ≤1500 g, (3) referred within 7 days of life, (4) at least two CUS preformed, (5) brain magnetic resonance imaging (MRI) at term age-equivalent. Intraventricular hemorrhage (IVH) grade was identified and FTHR was measured on all CUS. WMI on MRI was evaluated through (1) injury score (Kidokoro 2013) and (2) fractional anisotropy (FA) on the MRI diffusion tensor imaging. CP was estimated using the gross motor function classification system (GMFCS).
Results
One hundred neonates met the inclusion criteria: 37 with no IVH, 36 with IVH grade 1–2, and 27 with IVH grade 3–4. The FTHR cut-point of 0.51 had the highest sensitivity and specificity for moderate-to-severe WMI. In the IVH grade 3–4 group, the elevated FTHR correlated with lower FA and higher GMFCS.
Conclusions
FTHR is a useful quantitative biomarker of ventriculomegaly in preterm newborns. It may help standardize ventricular measurement and direct intervention.
Impact
-
The fronto-temporal horn ratio has the potential to become a standardized tool that can provide an actionable measure to direct intervention for post-hemorrhagic ventricular dilation.
-
This current study will provide the basis of a future clinical trial to optimize intervention timing to decrease the risk of white matter injury in this vulnerable population.
Similar content being viewed by others
Extremely preterm infants born <29 weeks gestational age (GA) are at high risk for cerebral palsy (CP) and other brain injuries.1 Infants with intraventricular hemorrhage (IVH) followed by post-hemorrhagic ventricular dilation (PHVD) are at the highest risk.2,3,4,5 PHVD can compromise the developing white matter tracts around the ventricles, leading to the white matter injury (WMI) associated with CP.6,7 In recent decades, bedside cranial ultrasound (CUS) has allowed clinicians to identify IVH and monitor progression of PHVD.8
The increase in size of the lateral ventricles on a two-dimensional plane, as a marker of PHVD, correlates with adverse long-term outcome.4 There is no expert consensus, however, on how to estimate the dilation of the lateral ventricles. There is also lack of agreement on the degree of PHVD that requires treatment to avoid life-long sequelae,9 largely because the point at which PHVD leads to WMI has not been determined. The ventricular index (VI) and anterior horn width10 are two parameters that have been used to estimate the size of the lateral ventricles on CUS. The recent ELVIS trial that used these two parameters to decide early vs. late treatment for PHVD did not show a difference in the composite outcome of ventriculoperitoneal shunt (VPS) placement and death between the two groups, but an improvement in the composite outcome of death, CP, and cognitive outcome in the early intervention group at the 2 years follow-up.11,12,13
Alternatively, the fronto-temporal horn ratio (FTHR) (Fig. 1) is a CUS parameter to estimate lateral ventricular dilation. FTHR demonstrates excellent inter-rater reliability and correlates well with three-dimensional ventricular volumes in older children.14,15 It also accounts for the bi-parietal diameter of the brain, and the major marking point for measurement (the foramen of Monro) is relatively easy to identify on the coronal sections of the CUS images. A similar parameter, the fronto-occipital horn ratio (FOHR), was recently used to develop a standardized algorithm to decide intervention for PHVD among multiple centers.16 However, the value of this parameter for the different grades of IVH in premature newborns has not been studied nor its relation to WMI.
In this study, we aim to define normative FTHR measures across GA in preterm infants and to relate the FTHR trajectories to WMI assessed on brain magnetic resonance imaging (MRI) at term age-equivalent and the motor developmental outcome at 15–20 months corrected age. We hypothesize that accelerated FTHR trajectories in infants with IVH will be associated with higher degree of WMI assessed by qualitative and quantitative MRI.
Method and design
This is a retrospective study of out-born extremely premature infants who were admitted to the level IV neonatal intensive care unit (NICU) at Children’s National Hospital (CNH) between the years 2011 and 2014. The institutional review board approved the study. Inclusion criteria were: (1) birth at <29 weeks GA, (2) birth weight (BW) ≤1500 g, (3) referral to CNHs within 7 days of life and survived till term equivalent age, (4) at least two CUS performed, and (5) brain MRI at term age-equivalent. Exclusion criteria were: (1) newborns with significant congenital brain anomalies/malformations and (2) extra-axial hemorrhage.
All charts were reviewed to identify the exact GA at birth in weeks, BW in grams, sex, twin gestation, and significant neonatal comorbidities (necrotizing enterocolitis defined as feeding intolerance with abdominal distention, sepsis with a positive blood culture, patent ductus arteriosus on echocardiogram requiring either medical and/or surgical treatments, and bronchopulmonary dysplasia with supplemental oxygen requirement at 36 weeks postmenstrual age (PMA)).
We also identified the different procedures performed during the NICU course, whether temporizing or permanent, to drain the cerebrospinal fluid (CSF) as a treatment for PHVD. This included serial lumbar punctures (LPs), transfontanelle ventricular taps, ventricular access devices (VADs), and VPSs. The decision to perform a procedure to drain CSF is done by the pediatric neurosurgeon and based on the finding of progressive ventriculomegaly on weekly CUS and excessive head growth on daily head circumference measurement.
Cranial ultrasound
As part of our center’s guidelines, CUS is done on all premature newborns <32 weeks GA within 24 h after admission. If no IVH, CUS is repeated at 7, 14, and 42 days of life per the American Academy of Neurology practice parameters.8 In cases of IVH, CUS is repeated weekly to monitor for PHVD, until IVH and/or PHVD is stable or resolved on at least two consecutive scans. If there is progression of PHVD on two or more CUS, a neurosurgical consultation is requested to evaluate for a temporizing or permanent surgical intervention to divert CSF. CUS were performed using a GE LOGIQ E9 (GE Healthcare Ultrasound, Waukesha, WI). All CUS were reviewed by the primary investigator (R.O.) to identify the presence or absence of the IVH. If IVH was present, we identified the date of CUS when IVH first appeared and the grade of IVH based on Papile et al.17 We followed the IVH progression on serial CUS and considered the highest IVH grade in the final analysis. We considered IVH grade 4 if there was hemorrhage in the germinal matrix and an echogenic focus in the frontal and/or parietal regions consistent with a periventricular hemorrhagic infarct (PVHI). The IVH grade was assigned by the primary investigator and then compared with the official report in the medical chart. In case of disagreement, a consensus was reached after reviewing the case with a pediatric radiologist (A.B.). We divided the sample into three groups: No IVH, IVH grade 1–2, and IVH grade 3–4.
The FTHR was measured and calculated by a neonatal neurologist (R.O.) on all the CUSs as shown in Fig. 1. We tried to include the borders of the lateral ventricles only in the measurement of the ventricular dilation and to exclude the ex vacuo porencephaly from the contiguous periventricular WMI.
Inter-rater reliability of FTHR measurement was assessed based on 26 random CUS cases that were evaluated by both the primary investigator (R.O.) and an experienced pediatric radiologist (A.B.).
Brain MRI
Brain MRI was performed using a 3-T scanner (Signa HCx; GE Healthcare, Milwaukee, WI) with an eight-channel receiver head coil (In Vivo Corp., Gainesville, FL). When feasible, infants were scanned after feeding and bundling without the use of sedation. Standard sequences included coronal volume T1- and T2-weighted images, axial spin echo proton density, diffusion-weighted, susceptibility-weighted, arterial spin labeling, and sagittal midline T2-weighted images.
Term equivalent brain MRIs for all the included newborns were identified and reviewed to assess WMI through two different modalities. First, WMI was characterized with a previously validated injury score.18 The score ranges between 0 and 17 (0 being normal). We considered a score of 8 as a cut-point to differentiate between either normal or mild injury (score <8) vs. moderate-to-severe injury (score ≥8).18 The brain MRI images were scored by the PI after establishing inter-rater reliability with an experienced pediatric neuro-radiologist (J.G.M.) based on 39 brain MRI images.
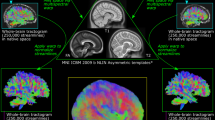
Second, we used diffusion tensor imaging (DTI), performed routinely at term equivalent age to derive quantitative measures of white matter integrity. Fractional anisotropy (FA) value, which reflects the directional coherence of fiber tracts and integrity of cellular structures on the DTI image, was measured from FA maps generated by the GE FUNCTOOL software. The quantitative measurement of FA was performed on the General Electric advantage windows workstation by placing manual regions of interest (ROIs), each measuring between 9 and 9.8 mm2, in distinct regions of the white matter on the axial view (Fig. 2): (1) the anterior third of the posterior limb of the internal capsule (PLIC), (2) the optic radiation next to the lateral ventricle at the level of the trigon, and (3) the three parts of the corpus callosum (genu, body, and splenium). Symmetrical ROIs were obtained for structures present bilaterally.
Long-term motor outcome
Infants with IVH are usually scheduled for an outpatient clinic visit with either neurology or physical medicine. The motor function was extrapolated from the clinic visits at 15–20 months corrected age via chart review. If CP was suspected, we used the gross motor function classification system-extended and revised (GMFCS-E&R)19 to estimate the degree of motor disability with 1 being independent walking with no assistance and 5 being no independent walking and requiring significant assistance.
Statistical analysis
Analysis of variance with pairwise comparisons was used to compare continuous variables, and Fisher Exact test to compare categorical variables between IVH groups. Inter-rater reliability was assessed by the intraclass correlation coefficient (ICC). The association between the FTHR recorded at the first week of life and GA in weeks was assessed using a linear regression model. Subsequently, generalized estimating equation (GEE) models were used to assess whether FTHR trajectories differed between the IVH groups, both overall and stratified by IVH severity subgroup, using PMA at the time of CUS as a measure of time and with group-by-time interaction terms. To evaluate the association between FTHR trajectories and WMI by qualitative and quantitative MRI, generalized linear models with a time-varying covariate clustered on patient were used controlling for PMA at the time of CUS and brain MRI. To establish the measure most strongly associated with WMI, multiple measures were assessed, including IVH group, raw FTHR measure, and individual FTHR slope trajectories. Based on these analyses, the area under receiver operating curve (AUC) estimated using binomial-logit GEE models was used to establish a cut-point for FTHR for moderate-to-severe WMI. Ordinal regression based on cumulative logit models was used to estimate the association between FTHR and GMFCS score.
Results
Of the 1424 premature newborns who were admitted to our hospital between the years of 2011 and 2014, 100 met the inclusion criteria; a total of 759 CUSs were performed during their NICU course (Fig. 3). After CUS review, IVH groups were as follows: 37 with No IVH, 36 with IVH grades 1–2, and 27 with IVH grades 3–4. IVH was diagnosed on CUS at a median age of 3 days after birth (range 1–23 days). There were 12 newborns who progressed from IVH grade 1–2 to IVH grade 3–4 over a median of 3 days (range 1–12 days). There were only two disagreements on IVH grading between the reviewer and the CUS report in the chart. Demographics and comorbidities by IVH group are shown in Table 1. Overall, 20% (13/63) of infants with IVH received at least one temporizing intervention to treat PHVD during the NICU course. The first intervention was either serial LPs and/or transfontanel ventricular tap (13/13) followed by the placement of a VAD (8/13); 10/13 newborns needed a VPS prior to discharge (all 8 who had a VAD got a VPS and 2 more). The first temporizing intervention (LP and/or transfontanel ventricular tap) happened at a median of 28 weeks PMA (range 26–32 weeks). VPS was inserted at a median of 38 weeks PMA (range 34–57 weeks).
The ICC for the FTHR measurement was 0.92, suggesting a high level of reliability. Initial mean FTHR values on CUS in the first week of life adjusting for GA were: No IVH (n = 36) 0.44 ± 0.02, IVH grade 1–2 (n = 32) 0.45 ± 0.02, and IVH grade 3–4 (n = 25) 0.46 ± 0.05 (p = 0.08 and 0.0004, respectively, compared to the No IVH group). Linear modeling suggested a borderline association between GA at birth and FTHR during the first week of life (β = −0.004, p = 0.07).
When comparing FTHR trajectories across PMA adjusting for GA, there were no significant difference between the trajectories of the No IVH and IVH grade 1–2 groups (p = 0.84). There was, however, a significant difference between these group trajectories and trajectories for IVH grade 3–4 (p = 0.0007 and 0.0004, respectively; Fig. 4).
Top: FTHR trajectories for the three pre-specified groups based on postmenstrual age in weeks after adjusting for GA [IVH 0 and IVH 1–2 significantly different from IVH 3–4 (p = 0.0007 and p = 0.0004, respectively); no difference between IVH 0 and IVH 1–2 (p = 0.84)]. Bottom: FTHR trajectories looking at every IVH group separately [significant differences: 0 vs. 4 (p = 0.0006), 1 vs. 4 (p = 0.01), and 2 vs. 4 (p = 0.001); 3 vs. 4 borderline significant (p = 0.07)].
Term equivalent brain MRIs were done at an average of 40 ± 4 weeks PMA; no significant differences in timing of MRI was noted between the IVH groups (p = 0.07). The ICC for brain MRI image scoring was 0.90 (high reliability). The median score of WMI on brain MRI at term age-equivalent for the whole group was 3 (range 0–15). Newborns with IVH grade 3–4 were significantly more likely to have moderate-to-severe brain injury (score ≥ 8) when compared to the No IVH and IVH grade 1–2 groups (44% vs. 3% and 0%, p < 0.0001). The odds of moderate-to-severe brain injury for a 0.05 unit increase in FTHR was 3.19 (95% CI 1.87–5.43, p < 0.05) adjusting for GA, BW, sex, and neonatal comorbidities. AUC was 0.91 suggesting that FTHR is a strong predictor of moderate-to-severe injury. FTHR cut-point of 0.51 had the highest sensitivity and specificity (90% and 89%, respectively), as determined by the Youden’s J Index.
The FA values on DTI images were significantly lower in the majority of brain regions in the grade 3–4 IVH group (Table 2). The FTHR values for the whole sample inversely correlated with the FA in all parts of the corpus callosum and optic radiations (Table 3).
Outcome at 15–20 months corrected age was available for 77% (21/27) of the infants in the grade 3–4 IVH group and 53% (19/36) of the infants in the grade 1–2 IVH group. In all, 3/19 in grade 1–2 IVH were diagnosed with CP [median GMFCS of 2 (range 2–3)] vs. 16/21 in grade 3–4 IVH [median GMFCS of 4 (range 1–5)] (p < 0.01). Using an ordinal regression model, there was a significant association between higher FTHR and higher GMFCS values (β = 14.02, p = 0.001), which remained significant even after controlling for IVH group and neonatal comorbidities (p = 0.03 and p < 0.0001, respectively).
Because of the clustering of elevated FTHR values in the grade 3–4 IVH group and the likelihood of intervention, we conducted a sub-analysis of this group separately. Within the grade 3–4 IVH group, a subset (n = 13, 48%) had a temporizing intervention to drain CSF due to progressive PHVD. FTHR values were significantly higher in this subset compared to the subjects in the same group who did not receive an intervention (average 0.63 vs. 0.48, p < 0.0001). Looking at the FTHR slopes on CUS in the intervention subset (considering FTHR values for the CUS done prior to and after the temporizing intervention separately), the FTHR increased significantly by 0.03 per week (p < 0.0001) and stabilized after the temporizing intervention (Fig. 5). The FA values on the DTI images in the subjects who received a temporizing intervention were significantly lower in the genu (p = 0.01), splenium (p < 0.0001), and body (p = 0.04) of the corpus callosum compared to the no intervention counterparts. When using a generalized linear model, individual FTHR slopes were significantly associated with FA in the genu and splenium of corpus callosum (Table 4) after controlling for age at MRI and neonatal comorbidities. In the same IVH grade 3–4 group, the GMFCS scores for the intervention subset were higher compared to the no intervention counterparts [median 4 (range 1–5) compared to a median of 2 (range 1–5) p = 0.06]. Looking at the FTHR slopes on CUS and GMFCS scores in the intervention subset (n = 12), the association was not statistically significant (β = 15.2, p = 0.1).
In the grade 3 IVH group (n = 8), 3/8 had a temporizing intervention to treat PHVD. The median Kidokoro score of WMI on term equivalent brain MRI was 4 (range 1–10) for grade 3 vs. 11 (range 4–15) for grade 4 (p = 0.02). The averages FA in all regions in grade 3 IVH were higher when compared to the same regions in grade 4 IVH but did not reach clinical significance. Of note, when comparing between grade 3 IVH (n = 8) and No IVH (n = 37), the Kidokoro score was higher in grade 3 IVH (p = 0.04) and the FA values were lower and statistically significant in parts the corpus callosum only [genu (p = 0.02), splenium (p = 0.02), and body (p = 0.2)]. In all, 4/8 had information about long-term outcome, only 1 patient developed CP with a GMFCS score of 4.
Discussion
In our study, we applied a previously described parameter to evaluate the ventricular dilation in extremely premature newborns for the first time. We were able to estimate the normal values of FTHR in preterm infants with relatively normal brains (no IVH) and to evaluate the FTHR as a measure of PHVD in preterm infants with the different grades of IVH. Radhakrishnan et al.15 found a strong relation between the FTHR on CUS in preterm infants and MRI-derived ventricular volume. Our study included a larger number of newborns and evaluated FTHR at an earlier PMA. A previous study in a similar population used the FOHR on coronal CUS images as a marker to decide treatment for PHVD and considered a cut-off of 0.55 to define moderate dilation and plan intervention.16 This threshold was estimated based on subjective clinical experience rather than the data driven approach (via ROC analyses) used in the current study. Our FTHR threshold of 0.51 had the highest specificity and sensitivity to predict moderate-to-severe WMI based on a validated scale.18
To be more thorough in evaluating the significance of FTHR as a measure of PHVD and its effects on the developing white matter, we used advanced quantitative DTI to measure FA in the white matter regions that are known to be affected the most by the ventricular dilation.20 We considered the FA values from the symmetric structures independently due to the statistically significant differences noted between the right and left optic radiations in the No IVH and IVH grade 1–2 groups (p = 0.04 and 0.05, respectively). The FTHR values for the whole sample inversely correlated with the FA values in all parts of the corpus callosum, which was independent of the IVH grade and other neonatal comorbidities. Even when considering the grade 3–4 IVH group only, where the FTHR values were significantly higher compared to the other groups, faster FTHR progression over time was associated with lower FA values in most parts of the corpus callosum, suggesting it as a sensitive marker for WMI in high-risk newborns. An exploratory analysis of the grade 3 IVH subjects only (to eliminate the effect of PVHI in grade 4 IVH on the outcome) showed an elevated FTHR and comparable pattern of WMI, although less severe. The sample was too small to compare long-term motor outcome. It is worth mentioning that 1 of the 4 patients with grade 3 IVH and known motor outcome developed CP with a GMFCS score of 4, this patient had severe ventriculomegaly and the only one who needed a VAD and then a VPS. Similar results have been found in animal models and older children with communicating hydrocephalus causing white matter loss, which correlated with developmental outcome.7,21,22,23,24 The length and thickness of the corpus callosum in premature infants was found to be associated with neurobehavioral development during the early life.25,26 This indicates that PHVD, especially if progressing, may be associated with a certain pattern of WMI in premature infants that can have significant developmental sequelae.
The diagnosis of CP was more prevalent in grade 3–4 IVH and the GMFCS scores, as a marker of CP severity, were also higher in this group. It correlated significantly with the FTHR values of the whole sample, even after adjusting for the IVH group, adding another evidence of the potential utility of FTHR.
There was also a direction toward higher GMFCS scores in the intervention subset of the IVH 3–4 group with CP (where there was a relative rapid increase in FTHR over time before a temporizing intervention is performed at a median age of 28 weeks PMA) compared to the subset with no intervention (no PHVD) but did not reach clinical significance. Of note, we identified two patients with CP in the IVH 3–4 group with GMFCS scores of 5 and who did not receive an intervention for PHVD. However, they may have qualified for an intervention due to significant ventriculomegaly. When we excluded these two patients from the analysis, the difference in GMFCS scores became significant (p < 0.001) indicating that the rate of change in FTHR is associated with worse motor outcome in infancy and suggesting that earlier intervention could improve the outcome.
Other measures have been described to measure PHVD. de Vries et al.27,28 investigated retrospectively two different thresholds of the VI to estimate PHVD on CUS and decide intervention. There was a tendency for a favorable outcome when interventions were performed at a relatively low threshold (VI < 97th + 4 mm percentile). A recent prospective study using the same VI thresholds to decide treatment (early vs. late) did not show a significant improvement in short-term outcome (VPS placement).11 However, the early intervention group had lower Kidokoro scores on brain MRI done at term equivalent age,29 and showed a better composite outcome of death, CP, and Bayley scores <−2 SD at 2 years follow-up.13 While we did not compare our results to the VI, our parameter (FTHR) has the advantage of correlating with volumetric measurement of the lateral ventricles and takes the brain diameter into account. Our study also adds to the evidence that PHVD is a risk factor for significant WMI, supporting the rationale that early treatment for PHVD may improve outcome.
Our study has several limitations. First, the retrospective nature of the design and the out-born cohort may have biased the results. It is difficult to estimate the outcome of PHVD in isolation to the other comorbidities in the extremely premature newborns. Despite this limitation, we were able to show significant associations between FTHR and degree of WMI after adjusting for modalities to evaluate the correlation. Second, there is a potential bias since all the ultrasound and brain MRI were reviewed by one reviewer. We tried to solve this bias by blinding the reviewer to the clinical history when reviewing the imaging. The scoring results were verified with multiple neuro-radiologists on the study group. Third, the lack of a comprehensive long-term outcome of PHVD is another limitation with regard to clinical implications, as the GMFCS score is a tool to assess the degree of CP only, and it may miss other aspect of the development that could be more affected by PHVD (like cognition). It may not be as reliable in children <24 months of age. Moreover, we did not account for the size of the infarcts in the periventricular regions in group 4 IVH, which can cause injury to the PLIC and lead to hemiplegia and worse motor outcome.
Conclusion
In this study, we established FTHR as an easily applied and quantitative biomarker of ventricular dilation and WMI in the preterm infant. The FTHR has the potential to become a standardized tool that can provide an actionable measure to direct intervention for PHVD. This study will provide the basis of a future clinical trial to optimize intervention timing to decrease the risk of WMI in this vulnerable population.
References
Winter, S., Autry, A., Boyle, C. & Yeargin-Allsopp, M. Trends in the prevalence of cerebral palsy in a population-based study. Pediatrics 110, 1220–1225 (2002).
Shankaran, S. et al. Outcome after posthemorrhagic ventriculomegaly in comparison with mild hemorrhage without ventriculomegaly. J. Pediatr. 114, 109–114 (1989).
Hintz, S. R. et al. Neuroimaging and neurodevelopmental outcome in extremely preterm infants. Pediatrics 135, e32–e.42 (2015).
Srinivasakumar, P. et al. Posthemorrhagic ventricular dilatation-impact on early neurodevelopmental outcome. Am. J. Perinatol. 30, 207–214 (2013).
Dyet, L. E. et al. Natural history of brain lesions in extremely preterm infants studied with serial magnetic resonance imaging from birth and neurodevelopmental assessment. Pediatrics 118, 536–548 (2006).
Del Bigio, M. R., Kanfer, J. N. & Zhang, Y. W. Myelination delay in the cerebral white matter of immature rats with kaolin-induced hydrocephalus is reversible. J. Neuropathol. Exp. Neurol. 56, 1053–1066 (1997).
Del Bigio, M. R., Wilson, M. J. & Enno, T. Chronic hydrocephalus in rats and humans: white matter loss and behavior changes. Ann. Neurol. 53, 337–346 (2003).
Ment, L. R. et al. Practice parameter: neuroimaging of the neonate: report of the Quality Standards Subcommittee of the American Academy of Neurology and the Practice Committee of the Child Neurology Society. Neurology 58, 1726–1738 (2002).
Riva-Cambrin, J. et al. Center effect and other factors influencing temporization and shunting of cerebrospinal fluid in preterm infants with intraventricular hemorrhage. J. Neurosurg. Pediatr. 9, 473–481 (2012).
Brouwer, M. J. et al. New reference values for the neonatal cerebral ventricles. Radiology 262, 224–233 (2012).
de Vries, L. S. et al. Treatment thresholds for intervention in posthaemorrhagic ventricular dilation: a randomised controlled trial. Arch. Dis. Child. Fetal Neonatal Ed. 104, F70–F75 (2019).
Cizmeci, M. N. et al. Periventricular hemorrhagic infarction in very preterm infants: characteristic sonographic findings and association with neurodevelopmental outcome at age 2 years. J. Pediatr. 217, 79.e1–85.e1 (2020).
Cizmeci, M. N. et al. Randomized controlled early versus late ventricular intervention study in posthemorrhagic ventricular dilatation: outcome at 2 years. J. Pediatr. 226, 28.E3–35.E3 (2020).
Antes, S. et al. The frontal and temporal horn ratio to assess dimension of paediatric hydrocephalus: a comparative volumetric study. Acta Neurochir. Suppl. 118, 211–214 (2013).
Radhakrishnan, R. et al. Frontal occipital and frontal temporal horn ratios: comparison and validation of head ultrasound-derived indexes with mri and ventricular volumes in infantile ventriculomegaly. AJR Am. J. Roentgenol. 213, 925–931 (2019).
Wellons, J. C. 3rd et al. Shunting outcomes in posthemorrhagic hydrocephalus: results of a Hydrocephalus Clinical Research Network prospective cohort study. J. Neurosurg. Pediatr. 20, 19–29 (2017).
Papile, L. A. et al. Posthemorrhagic hydrocephalus in low-birth-weight infants: treatment by serial lumbar punctures. J. Pediatr. 97, 273–277 (1980).
Kidokoro, H., Neil, J. J. & Inder, T. E. New MR imaging assessment tool to define brain abnormalities in very preterm infants at term. AJNR Am. J. Neuroradiol. 34, 2208–2214 (2013).
Palisano, R. J., Copeland, W. P. & Galuppi, B. E. Performance of physical activities by adolescents with cerebral palsy. Phys. Ther. 87, 77–87 (2007).
Akbari, S. H. et al. Periventricular hyperintensity in children with hydrocephalus. Pediatr. Radiol. 45, 1189–1197 (2015).
Zhang, S. et al. Alterations in cortical thickness and white matter integrity in mild-to-moderate communicating hydrocephalic school-aged children measured by whole-brain cortical thickness mapping and DTI. Neural Plast. 2017, 5167973 (2017).
Olopade, F. E., Shokunbi, M. T. & Siren, A. L. The relationship between ventricular dilatation, neuropathological and neurobehavioural changes in hydrocephalic rats. Fluids Barriers CNS 9, 19 (2012).
Yuan, W. et al. Diffusion tensor imaging properties and neurobehavioral outcomes in children with hydrocephalus. AJNR Am. J. Neuroradiol. 34, 439–445 (2013).
Cardoso, E. J., Lachat, J. J., Lopes, L. S., Santos, A. C. & Colli, B. O. Changes caused by hydrocephalus, induced by kaolin, in the corpus callosum of adult dogs. Acta Cir. Bras. 26, 8–14 (2011).
Liu, F. et al. Ultrasound measurement of the corpus callosum and neural development of premature infants. Neural Regen. Res. 8, 2432–2440 (2013).
Malavolti, A. M. et al. Association between corpus callosum development on magnetic resonance imaging and diffusion tensor imaging, and neurodevelopmental outcome in neonates born very preterm. Dev. Med. Child Neurol. 59, 433–440 (2017).
de Vries, L. S. et al. Early versus late treatment of posthaemorrhagic ventricular dilatation: results of a retrospective study from five neonatal intensive care units in The Netherlands. Acta Paediatr. 91, 212–217 (2002).
Leijser, L. M. et al. Posthemorrhagic ventricular dilatation in preterm infants: when best to intervene? Neurology 90, e698–e706 (2018).
Cizmeci, M. N. et al. Assessment of brain injury and brain volumes after posthemorrhagic ventricular dilatation: a nested substudy of the randomized controlled ELVIS trial. J. Pediatr. 208, 191.e2–197.e2 (2019).
Acknowledgements
This work was funded by an Early Career Award through the Thrasher Foundation.
Author information
Authors and Affiliations
Contributions
R.O. conceptualized and designed the study and acquired the data, including the chart review and the technical analysis of the cranial ultrasound and brain MRI images. He drafted the article and revised it multiple times. He approved the final version for publication. T.C. conceptualized and designed the study and helped drafting the manuscript and revising it for important intellectual content. She approved the final version for publication. E.B. helped in acquiring and managing the data in Redcap. She also helped in analyzing the data. She critically reviewed and approved the final version of the manuscript for publication. J.G.M. helped conceptualize and design the study. He contributed significantly to the data acquisition by reviewing the brain imaging (brain MRI). He also helped critically revising the final manuscript for important intellectual content and approved the final version to be published. D.B. conceptualized and designed the study, helped in reviewing the cranial ultrasound images, reviewed the manuscript critically for important intellectual content, and approved the final version to be published. A.B. contributed to the acquisition of the data, reviewed the cranial ultrasound images, helped in revising the article for important intellectual content, and approved the final version to be published. C.O. conceptualized and designed the study and reviewed the manuscript for important intellectual content. He reviewed the manuscript and approved the final version to be published. M.J. conceptualized and designed the study, performed the statistical analysis and helped in interpreting the data. She reviewed the manuscript and approved the final version for publication. A.N.M. conceptualized and designed the study, planned the statistical analysis, helped significantly in interpreting the data, reviewed the manuscript critically, and approved the final version to be published. A.A.P. conceptualized and designed the study, mentored the primary investigator, planned the statistical analysis, helped with data interpretation, critically reviewed the manuscript, and approved the final version to be published. All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Patient consent statement
Patient consent was not required.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Obeid, R., Jacobs, M., Chang, T. et al. The utility of the fronto-temporal horn ratio on cranial ultrasound in premature newborns: a ventriculomegaly marker. Pediatr Res 89, 1715–1723 (2021). https://doi.org/10.1038/s41390-020-01337-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-020-01337-x
This article is cited by
-
Prediction of short- and long-term outcomes using pre-operative ventricular size in infants with post-hemorrhagic ventricular dilation
Child's Nervous System (2024)
-
Post-hemorrhagic ventricular dilatation affects white matter maturation in extremely preterm infants
Pediatric Research (2022)
-
Degree of ventriculomegaly predicts school-aged functional outcomes in preterm infants with intraventricular hemorrhage
Pediatric Research (2022)
-
Ventriculomegaly thresholds for prediction of symptomatic post-hemorrhagic ventricular dilatation in preterm infants
Pediatric Research (2022)