Abstract
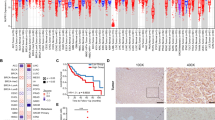
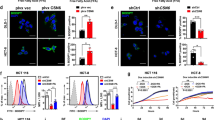
SLP2, a protein located on mitochondrial, has been shown to be associated with mitochondrial biosynthesis. Here we explored the potential mechanisms by which SLP2 regulates the development of hepatocellular carcinoma. SLP2 could bind to the c-terminal of JNK2 to affect the ubiquitinated proteasomal degradation pathway of JNK2 and maintain the protein stability of JNK2. The increase of JNK2 markedly increases SREBP1 activity, promoting SREBP1 translocation into the nucleus to promote de novo lipogenesis. Alteration of the JNK2 C-terminal disables SLP2 from mediating SLP2-enhanced de novo lipogenesis. YTHDF1 interacts with SLP2 mRNA in a METTL3/m6A-dependent manner. In a spontaneous HCC animal model, SLP2/c-Myc/sgP53 increases the incidence rate of spontaneous HCC, tumor volume, and tumor number. Importantly, statistical analyses show that levels of SLP2 correlate with tumor sizes, tumor metastasis, overall survival, and disease-free survival of the patients. Targeting the SLP2/SREBP1 pathway effectively inhibits proliferation and metastasis of HCC tumors with high SLP2 expression in vivo combined with lenvatinib. These results illustrate a direct lipogenesis-promoting role of the pro-oncogenic SLP2, providing a mechanistic link between de novo lipogenesis and HCC.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 50 print issues and online access
$259.00 per year
only $5.18 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout








Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this published article and its supplementary information files. The relevant mRNA databases can be found at the following sites. https://doi.org/10.6084/m9.figshare.20087705.
References
Siegel RL, Miller KD, Fuchs HE, Jemal A. Cancer statistics, 2021. CA Cancer J Clinicians. 2021;71:7–33.
Rich NE, Yopp AC, Singal AG. Medical management of hepatocellular carcinoma. J Oncol Pract. 2017;13:356–64.
Chen Q, Shu C, Laurence AD, Chen Y, Peng BG, Zhen ZJ, et al. Effect of Huaier granule on recurrence after curative resection of HCC: a multicentre, randomised clinical trial. Gut. 2018;67:2006–16.
Ruf B, Heinrich B, Greten TF. Immunobiology and immunotherapy of HCC: spotlight on innate and innate-like immune cells. Cell Mol Immunol. 2021;18:112–27.
Faubert B, Solmonson A, DeBerardinis RJ. Metabolic reprogramming and cancer progression. Sci (N. Y, NY). 2020;368:eaaw5473.
Wang M, Han J, Xing H, Zhang H, Li Z, Liang L, et al. Dysregulated fatty acid metabolism in hepatocellular carcinoma. Hepatic Oncol. 2016;3:241–51.
Li J, Huang Q, Long X, Zhang J, Huang X, Aa J, et al. CD147 reprograms fatty acid metabolism in hepatocellular carcinoma cells through Akt/mTOR/SREBP1c and P38/PPARα pathways. J Hepatol. 2015;63:1378–89.
Alannan M, Fayyad-Kazan H, Trézéguet V, Merched A. Targeting lipid metabolism in liver cancer. Biochemistry. 2020;59:3951–64.
Nguyen P, Leray V, Diez M, Serisier S, Le Bloc’h J, Siliart B, et al. Liver lipid metabolism. J Anim Physiol Anim Nutr. 2008;92:272–83.
Hall Z, Chiarugi D, Charidemou E, Leslie J, Scott E, Pellegrinet L, et al. Lipid remodeling in hepatocyte proliferation and hepatocellular carcinoma. Hepatol (Baltim, Md). 2021;73:1028–44.
Wang MD, Wu H, Fu GB, Zhang HL, Zhou X, Tang L, et al. Acetyl-coenzyme A carboxylase alpha promotion of glucose-mediated fatty acid synthesis enhances survival of hepatocellular carcinoma in mice and patients. Hepatol (Baltim, Md). 2016;63:1272–86.
Mitsopoulos P, Chang YH, Wai T, König T, Dunn SD, Langer T, et al. Stomatin-like protein 2 is required for in vivo mitochondrial respiratory chain supercomplex formation and optimal cell function. Mol Cell Biol. 2015;35:1838–47.
Christie DA, Mitsopoulos P, Blagih J, Dunn SD, St-Pierre J, Jones RG, et al. Stomatin-like protein 2 deficiency in T cells is associated with altered mitochondrial respiration and defective CD4+ T cell responses. J Immunol (Baltim, Md: 1950). 2012;189:4349–60.
Wang Y, Morrow JS. Identification and characterization of human SLP-2, a novel homologue of stomatin (band 7.2b) present in erythrocytes and other tissues. J Biol Chem. 2000;275:8062–71.
Lapatsina L, Brand J, Poole K, Daumke O, Lewin GR. Stomatin-domain proteins. Eur J cell Biol. 2012;91:240–5.
Chang D, Ma K, Gong M, Cui Y, Liu ZH, Zhou XG, et al. SLP-2 overexpression is associated with tumour distant metastasis and poor prognosis in pulmonary squamous cell carcinoma. Biomarkers Biochemical Indic Exposure, Response, Susceptibility Chem. 2010;15:104–10.
Feng Q, Hu ZY, Liu XQ, Zhang X, Lan X, Geng YQ, et al. Stomatin-like protein 2 is involved in endometrial stromal cell proliferation and differentiation during decidualization in mice and humans. Reprod Biomed Online. 2017;34:191–202.
Zhu W, Li W, Geng Q, Wang X, Sun W, Jiang H, et al. Silence of stomatin-like protein 2 represses migration and invasion ability of human liver cancer cells via inhibiting the nuclear factor kappa B (NF-κB) pathway. Med Sci Monit Int Med J Exp Clin Res. 2018;24:7625–32.
Luo A, Kong J, Hu G, Liew CC, Xiong M, Wang X, et al. Discovery of Ca2+-relevant and differentiation-associated genes downregulated in esophageal squamous cell carcinoma using cDNA microarray. Oncogene. 2004;23:1291–9.
Ma W, Chen Y, Xiong W, Li W, Xu Z, Wang Y, et al. STOML2 interacts with PHB through activating MAPK signaling pathway to promote colorectal Cancer proliferation. J Exp Clin Cancer Res CR. 2021;40:359.
Ma W, Xu Z, Wang Y, Li W, Wei Z, Chen T, et al. A positive feedback loop of SLP2 activates MAPK signaling pathway to promote gastric cancer progression. Theranostics. 2018;8:5744–57.
Zheng Y, Huang C, Lu L, Yu K, Zhao J, Chen M, et al. STOML2 potentiates metastasis of hepatocellular carcinoma by promoting PINK1-mediated mitophagy and regulates sensitivity to lenvatinib. J Hematol Oncol. 2021;14:16.
Song L, Liu L, Wu Z, Lin C, Dai T, Yu C, et al. Knockdown of stomatin-like protein 2 (STOML2) reduces the invasive ability of glioma cells through inhibition of the NF-κB/MMP-9 pathway. J Pathol. 2012;226:534–43.
Ito M, Nagasawa M, Omae N, Tsunoda M, Ishiyama J, Ide T, et al. A novel JNK2/SREBP-1c pathway involved in insulin-induced fatty acid synthesis in human adipocytes. J lipid Res. 2013;54:1531–40.
Chao D, Ariake K, Sato S, Ohtsuka H, Takadate T, Ishida M, et al. Stomatin‑like protein 2 induces metastasis by regulating the expression of a rate‑limiting enzyme of the hexosamine biosynthetic pathway in pancreatic cancer. Oncol Rep. 2021;45:90.
Wang Y, Cao W, Yu Z, Liu Z. Downregulation of a mitochondria associated protein SLP-2 inhibits tumor cell motility, proliferation and enhances cell sensitivity to chemotherapeutic reagents. Cancer Biol Ther. 2009;8:1651–8.
Hammouda MB, Ford AE, Liu Y, Zhang JY. The JNK signaling pathway in inflammatory skin disorders and cancer. Cells. 2020;9:857.
Kumar A, Singh UK, Kini SG, Garg V, Agrawal S, Tomar PK, et al. JNK pathway signaling: a novel and smarter therapeutic targets for various biological diseases. Future Med Chem. 2015;7:2065–86.
Hao Q, Liu Z, Lu L, Zhang L, Zuo L. Both JNK1 and JNK2 are indispensable for sensitized extracellular matrix mineralization in IKKβ-deficient osteoblasts. Front Endocrinol. 2020;11:13.
Takahashi H, Ogata H, Nishigaki R, Broide DH, Karin M. Tobacco smoke promotes lung tumorigenesis by triggering IKKbeta- and JNK1-dependent inflammation. Cancer Cell. 2010;17:89–97.
Chen YT, Lin CW, Su CW, Yang WE, Chuang CY, Su SC, et al. Magnolol triggers caspase-mediated apoptotic cell death in human oral cancer cells through JNK1/2 and p38 pathways. Biomedicines. 2021;9:1295.
Lepore A, Choy PM, Lee NCW, Carella MA, Favicchio R, Briones-Orta MA, et al. Phosphorylation and stabilization of PIN1 by JNK promote intrahepatic cholangiocarcinoma growth. Hepatol (Baltim, Md). 2021;74:2561–79.
Pu X, Dong C, Zhu W, Li W, Jiang H. Silencing stomatin-like protein 2 attenuates tumor progression and inflammatory response through repressing CD14 in liver cancer. OncoTargets Ther. 2019;12:7361–73.
Jones JE, Esler WP, Patel R, Lanba A, Vera NB, Pfefferkorn JA, et al. Clinical Significance of SLP-2 in Hepatocellular Carcinoma Tissues and Its Regulation in Cancer Cell Proliferation, Migration, and EMT [Retraction]. OncoTargets Ther. 2022;15:869–70.
Wang L, Zhang X, Lin ZB, Yang PJ, Xu H, Duan JL, et al. Tripartite motif 16 ameliorates nonalcoholic steatohepatitis by promoting the degradation of phospho-TAK1. Cell Metab. 2021;33:1372–88.e7.
Pavlova NN, Thompson CB. The emerging hallmarks of cancer metabolism. Cell Metab. 2016;23:27–47.
Jones JE, Esler WP, Patel R, Lanba A, Vera NB, Pfefferkorn JA, et al. Inhibition of Acetyl-CoA Carboxylase 1 (ACC1) and 2 (ACC2) reduces proliferation and de novo lipogenesis of EGFRvIII human glioblastoma cells. PloS one. 2017;12:e0169566.
Simeone P, Tacconi S, Longo S, Lanuti P, Bravaccini S, Pirini F, et al. Expanding roles of de novo lipogenesis in breast cancer. Int J Environ Res Public Health. 2021;18:3575.
Koundouros N, Poulogiannis G. Reprogramming of fatty acid metabolism in cancer. Br J Cancer. 2020;122:4–22.
Rysman E, Brusselmans K, Scheys K, Timmermans L, Derua R, Munck S, et al. De novo lipogenesis protects cancer cells from free radicals and chemotherapeutics by promoting membrane lipid saturation. Cancer Res. 2010;70:8117–26.
Toschi A, Lee E, Xu L, Garcia A, Gadir N, Foster DA. Regulation of mTORC1 and mTORC2 complex assembly by phosphatidic acid: competition with rapamycin. Mol Cell Biol. 2009;29:1411–20.
Basingab FS, Ahmadi M, Morgan DJ. IFNγ-Dependent Interactions between ICAM-1 and LFA-1 Counteract Prostaglandin E2-Mediated Inhibition of Antitumor CTL Responses. Cancer Immunol Res. 2016;4:400–11.
Zhang N, Zhang H, Liu Y, Su P, Zhang J, Wang X, et al. SREBP1, targeted by miR-18a-5p, modulates epithelial-mesenchymal transition in breast cancer via forming a co-repressor complex with Snail and HDAC1/2. Cell Death Differ. 2019;26:843–59.
Pascual G, Avgustinova A, Mejetta S, Martín M, Castellanos A, Attolini CS, et al. Targeting metastasis-initiating cells through the fatty acid receptor CD36. Nature. 2017;541:41–5.
Acknowledgements
We thank Qingsong Hu for his valuable daily discussions. We thank OEbiotech company for the technical support of RNAseq and mass spectrometry analysis.
Funding
This study was supported by the National Key R&D Program of China (grant no. 2019YFA0709300 and 2019YFC1605001), the National Natural Science Foundation of China (grant no. 81772588, U19A2008, 81972307, 82103219, 82102705, and 81773194), China Postdoctoral Science Foundation (2020M671911, 2020TQ0313, 2020M682023), and the Natural Science Foundation of Anhui Province (2008085QH376). Youth Innovation Key Fund Project of USTC (WK9110000153-2020,YD9100002003-2019).
Author information
Authors and Affiliations
Contributions
YL: formal analysis, investigation, methodology, writing – original draft. LS: investigation, data curation. HG: methodology, validation. SZ: investigation. WC: methodology, visualization. CJ: formal analysis, software. FM: methodology, validation. SL: methodology. BZ: data curation. YY: data curation. KM: validation, XL: validation, TC: validation; XG: formal analysis; NZ: formal analysis; JW: supervision; YL: writing– review & editing, methodology; LL: funding acquisition, conceptualization.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liu, Y., Sun, L., Guo, H. et al. Targeting SLP2-mediated lipid metabolism reprograming restricts proliferation and metastasis of hepatocellular carcinoma and promotes sensitivity to Lenvatinib. Oncogene 42, 374–388 (2023). https://doi.org/10.1038/s41388-022-02551-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41388-022-02551-z
This article is cited by
-
TM4SF1 upregulates MYH9 to activate the NOTCH pathway to promote cancer stemness and lenvatinib resistance in HCC
Biology Direct (2023)
-
Methyltransferase-like proteins in cancer biology and potential therapeutic targeting
Journal of Hematology & Oncology (2023)
-
Cancer metastasis under the magnifying glass of epigenetics and epitranscriptomics
Cancer and Metastasis Reviews (2023)