Abstract
Lysergic acid diethylamide (LSD) is a serotonergic psychedelic compound receiving increasing interest due to putative anxiolytic and antidepressant properties. However, the potential neurobiological mechanisms mediating these effects remain elusive. Employing in vivo electrophysiology, microionthophoresis, behavioral paradigms and morphology assays, we assessed the impact of acute and chronic LSD administration on anxiety-like behavior, on the cortical dendritic spines and on the activity of serotonin (5-HT) neurons originating in the dorsal raphe nucleus (DRN) in male mice exposed to chronic restraint stress. We found that while the acute intraperitoneal (i.p.) administration of LSD (5, 15 and 30 and 60 μg/kg) did not produce any anxiolytic or antidepressant effects in non-stressed mice, the dose of 30 µg/kg (daily for 7 days) prevented the stress-induced anxiety-like behavior and the stress-induced decrease of cortical spine densitiy. Interestingly, while LSD acutely decreased the firing activity of 5-HT neurons, repeated LSD increased their basal firing rate and restored the low 5-HT firing induced by stress. This effect was accompanied by a decreased inhibitory response of 5-HT neurons to microiontophoretic applications of the 5-HT1A agonist 8-OH-DPAT (8-hydroxy-N,N-dipropyl-2-aminotetralin). In conclusion, repeated LSD prevents the exacerbation of anxiety-like behavior following chronic stress exposure, but has no behavioral effects in non-stressed mice. These effects are paralleled by increased cortical spinogenesis and an enhancement of 5-HT neurotransmission which might be due to 5-HT1A receptors desensitization. Increased cortical spine density and enhancement of serotonergic neurotransmission may thus represent a candidate mechanism which mediate the therapeutic effects of serotonergic psychedelics on stress-induced anxiety.
Similar content being viewed by others
Introduction
In recent years, psychedelic compounds have come to the forefront as potential therapeutics in psychiatry [1,2,3]. In healthy individuals, the mixed serotonin (5-HT)1A/2A receptor agonist lysergic acid diethylamide (LSD) produces feelings of happiness, trust, and empathy [4, 5], positive mood changes and prosocial effects [6, 7]. Preliminary randomized controlled trials (RCTs) demonstrated the efficacy of LSD-assisted psychotherapy to treat anxiety and distress associated with life-threatening diseases [8, 9]. Ongoing clinical studies are assessing the efficacy of LSD for the treatment of major depressive disorders [10]. Despite promising preliminary evidence that they might be safe and efficacious in psychiatry, the mechanisms mediating their therapeutic effects remain elusive, hindering drug development.
In our previous published study, we observed that while at low doses LSD (5–20 µg/kg) administration decreases the firing activity of serotonergic (5-HT) neurons in the dorsal raphe nucleus (DRN), at higher doses (60–120 µg/kg) it decreases the firing activity of dopaminergic (DA) neurons in the ventral tegmental area. Corroborating the involvement of the DA system, this effect was prevented by the injection of the selective D2 antagonist haloperidol (50 µg/kg) [11]. This suggests that at low doses LSD only affects 5-HT neurotransmission, but at higher doses its effects extend to the DA system, thereby producing psychotic-like symptoms such as hyperlocomotion and stereotypic behaviors [12]. Similarly, other authors found a differential effect of LSD doses and timing administration over 5-HT and DA systems [13, 14]. For these reasons, we have then used LSD at a low dose range in a 7-day regimen, demonstrating that LSD (30 µg/kg, i.p., for 7 days) enhances sociability and the social novelty preference by potentiating the 5-HT2A and AMPA responses in glutamatergic neurons and activating the mTORC1 complex in excitatory neurons of the medial prefrontal cortex (mPFC) [15].
The 5-HT system is strongly involved in the neurobiology of stress-induced anxiety and depression [16, 17]. Chronic stress in rodents produces a decline of 5-HT firing activity [18], in addition to the development of anxiety-like phenotypes [19, 20]. Given that LSD is a serotonergic agent with anxiolytic properties, it seems plausible that LSD might affect certain facets of the neurobiological stress response, exerting a protective role over stress-induced neurobiological changes. However, whether repeated LSD confers behavioral and neurobiological resilience to stress preventing the exacerbation of stress-induced anxiety and/or depressive-like behavior and the stress-elicited low firing activity of serotonergic neurons, remains unknown. Moreover, while LSD is known to acutely decrease the firing activity of 5-HT neurons [11, 21], the effects of repeated LSD on 5-HT neurotransmission in baseline conditions or under a chronically stressful condition is yet to be investigated.
Here, we firstly tested if a single administration of different doses of LSD (5, 15, 30 and 60 µg/kg) elicit anxiolytic and/or antidepressant-like effect. Secondly, we investigated the ability of repeated LSD administration to prevent the stress-induced development of anxiety-like behavior. Lastly, we assessed if the protective effects of repeated LSD over stress-induced behaviors is paralleled by a protective effect over the stress-induced cortical spinogenesis and 5-HT neurotransmission decline.
Materials and methods
C57BL/6N male mice (8–12 weeks old, weighing 25–30 g, Charles River, Quebec, Canada) were used. All procedures were approved by the McGill University Ethics Committee and conducted in accordance with the Canadian Institute of Health Research for Animal Care and Scientific Use, and the Animal Care Committee of McGill University (protocol number 5764). All efforts were made to minimize animal suffering, and the 3Rs rule (reduce, refine, replace) applied where possible.
Acute and repeated LSD treatment
For acute studies, intraperitoneal (i.p.) LSD (Sigma-Aldrich, London, UK) doses of 5, 15, 30 and 60 µg/kg were employed. Immediately after administration, mice were placed in a transparent glass beaker to assess the head twitch response for 10 min. Subsequently, mice were returned to their home cage for 20 min before undergoing the other behavioral tests. For the repeated treatment, the doses of 5, 15 and 30 µg/kg (i.p.) were employed in the chronic restraint stress (CS) study and administered during the last 7 days of the (CS) paradigm. For in vivo electrophysiological recordings, cumulative acute injections were used. The doses tested were chosen based on previous experiments showing that 5–20 µg/kg acutely decreased the 5-HT DRN firing activity [11] and on behavioral experiment showing that 7 days of 30 µg/kg daily increased social behavior in mice without affecting locomotion [22]. For repeated treatment, behavioral or electrophysiological experiments were performed 24 h later the last LSD or vehicle injection. Detailed descriptions of the methods are presented in the online Supplementary Material section.
Results
Effects of acute LSD treatment on the head twitch response in non-stressed animals
Immediately after LSD injection (5, 15, 30 and 60 µg/kg, i.p.), mice were placed in a transparent Plexiglas cylinder (40 cm diameter) for HTR quantification. One-way ANOVA analysis detected a significant difference of the treatment (Fig. 1A, F (4,40) = 52,71, p < 0.0001). In particular, the doses of 30 and, more robustly, of 60 µg/kg, increased the number of head twitches, compared to mice treated with vehicle or lower LSD doses.
A Acute doses of LSD (30 and 60 μg/kg, i.p.) increasesd the number of head twitches. B Percentage of time spent in the open arms during the EPMT. C Number of entries in the open arm during the EPMT. D None of the LSD doses tested affected the time spent in the light compartment nor (E) the number of transitions between the dark and light compartment in the LDBT. F LSD fails to change the latency to feed in the novel environment during the NSFT or (G) in the home cage after the test. In the OFT, none of the LSD tested doses affects (H) the distance traveled, (I) the entries in the center and (J) the time spent in the center (J) of the arena. LSD (60 μg/kg) increases the duration of (K) grooming and (L) frequency of rearing during the OFT. M None of the doses of LSD affectes immobility time in the FST. One-way ANOVA followed by Bonferroni post-hoc comparison; *p < 0.05; ***p < 0.001; n.s. not significant, EPMT elevated plus maze, LDBT light-dark box test, NSFT novelty suppressed feeding test, OFT open field test, FST forced swim test.
Effects of acute LSD treatment on anxiety- and depressive-like behavior in non-stressed animals
Next, we performed a battery of behavioral tests to investigate the ability of different doses of LSD (5, 15, 30 and 60 µg/kg) to modulate anxiety-like and depression-like behaviors. Twenty minutes after the HTR measurement, anxiety-like behavior was quantified in the elevated plus maze (EPM) test. No statistical difference was detected in the percentage of time spent in the open arms (Fig. 1B, F (4,39) = 0.6857, p = 0.6058) or in the number of entries (Fig. 1C, F (4,39) = 1.063, p = 0.3881) in the open arms. After the EPM, animals underwent the light-dark box test (LDBT). No differences were observed in the time spent in the light compartment (Fig. 1D, F (4,39) = 1.044, p = 0.3969) nor in the number of transitions between the dark and light compartment (Fig. 1E, F (4,39) = 0.5721 p = 0.6844). Subsequently, mice were placed in a novel arena to undergo the novelty suppressed feeding test (NSFT). None of the tested doses of LSD produced changes in the latency to feed in the novel environment (Fig. 1F, F (4,40) = 0.3520, p = 0.8411). A different cohort of mice was tested in the open field test (OFT) and the forced swim test (FST). Thirty minutes after the injections, mice were placed in the OFT arena. A main effect of treatment was observed over the total distance traveled (Fig. 1H, F (4,39) = 4.045, p = 0.007). Although post-hoc analyses did not reveal statistically significant differences between any of the experimental groups, we found a non-statistically significant trend in the increased distance traveled by the mice treated with the 60 µg/kg dose, compared to vehicle-treated mice. Similarly, none of the tested doses produced significant differences in the number of entries into the center (Fig. 1I, F (4,39) = 0.2324 p = 0.9185) or the total time spent in the center area of the arena (Fig. 1J, F (4,39) = 0.4238, p = 0.7905). Stereotypies, which are abnormal repetitive, unvarying, and functionless behaviors that model a psychotic-like behavior [23] were also assessed during the 20 min of open field. Intriguingly, we found that while the dose of 60 µg/kg produced a significant increase of grooming duration (Fig. 1K, F (4,39) = 57, p < 0.001) and rearing episodes (Fig. 1L, F (4,39) = 11.25, p < 0.001), the dose of 30 µg/kg did not, confirming the dual activation of the 5-HT system at low doses of LSD and dopamine at higher doses as previously observed [11]. Finally, mice were tested in the FST and no differences were found regarding the immobility time in relation to the dose of LSD (Fig. 1M, F (4,39) = 0.3399 p = 0.8494). Given that the 60 μg/kg dose induced an increase in the stereotypies (grooming and rearing) in the OFT (Fig. 1K, L), we did not use this dose in further experiments.
Repeated LSD administration prevents chronic-stress induced anxiety-like behavior
Given the lack of behavioral effects in non-stressed animals, we investigated the ability of LSD to prevent the development of anxiety-like behavior following chronic restraint stress (CS, 15 days, 2 h/day). Twenty-four hours after the last restraint procedure, mice underwent the open field test (OFT) (Fig. 2A). Stressed mice showed no differences in locomotion compared to controls (CTL), and repeated LSD had no effect on the distance traveled at the tested doses (Fig. 2B, stress factor, F (1, 69) = 0.1772, p = 0.6751; treatment factor, F (3, 69) = 0.3122, p = 0.8165; interaction treatment × stress, F (3, 69) = 2.018, p = 0.1194). As expected, CS decreased the time spent in the center of the open field test arena (Fig. 2C, stress factor, F (1, 69) = 163.7, p < 0.001; treatment factor, F (3, 69) = 2.562, p = 0.0618; interaction treatment × stress, F (3, 69) = 3.529, p = 0.0193, Fig. 2C, G) and the number of entries to the center (Fig. 2D, G stress factor, F (1, 69) = 162.6, p < 0.001; treatment factor, F (3, 69) = 8.127, p = 0.0001; interaction treatment × stress, F (3, 69) = 5.148, p = 0.0029). Interestingly, the number of entries was statistically higher in CS mice treated with LSD at the dose of 30 µg/kg/day for 7 days (last injection 24 h before the test) compared to CS mice treated with veh (p < 0.001), indicating an anxiolytic-like effect of the 7-day repeated LSD regimen. On the contrary, the doses of 5 and 15 µg/kg failed to prevent the decrease in the number of entries in CS mice (Fig. 2D). In line with our previous work [15], repeated LSD administration did not affect the center time and entries. In addition, neither repeated LSD nor CS affected the duration of grooming (Fig. 2E, stress factor, F (1, 69) = 1.944, p = 0.1677; treatment factor, F (3, 69) = 0.6376, p = 0.5934; interaction treatment × stress, F (3, 69) = 0.6756, p = 0.5699) or the frequency of rearing (Fig. 2F, stress factor, F (1, 69) = 1.488, p = 0.2267; treatment factor, F (3, 69) = 1.648, p = 0.1864; interaction treatment × stress, F (3, 69) = 0.7582, p = 0.5214). These results demonstrate that amongst the doses not eliciting stereotypic behavior, only the repeated dose of 30 µg/kg prevented the CS-induced decrease in number of entries in the center of the arena, without affecting the grooming and rearing behavior.
A Schematic timeline showing the stress procedure, drug treatment and behavioral procedures. LSD does not affect the distance traveled (B), time spent in the center (C), and frequency of visits (D) to the center area of the open field test (OFT). No difference was detected in mice treated with veh or any dose of LSD in the duration of grooming (E) or frequency of rearing (F) assessed during the OFT. Each line represents mean ± SEM and each point represents a single mouse. G Example of horizontal movement traces in the OFT. Two-way ANOVA followed by Bonferroni post-hoc comparison; ***p < 0.001. N.S. not significant, OFT open field test, veh vehicle, CTL non-stressed control, CS chronic restraint stress.
Repeated LSD administration prevents chronic stress-induced anxiety-like behavior in the light-dark box test and in the novelty suppressed feeding test, but not in the elevated plus maze test
To further assess the protective effects of the only effective LSD dose (30 µg/kg) over stress-induced anxiety-like behavior, another cohort of LSD-treated mice and controls were exposed to CS and tested in the EPMT, LDBT and NSFT (Fig. 3A). In the EPMT, CS and CTL mice did not display differences in locomotion (Fig. 3B, stress factor, F (1, 28) = 0.1162, p = 0.7358; treatment factor, F (1, 28) = 2.482, p = 0.1264; interaction stress x treatment, F (1, 28) = 0.0059, p = 0.9395). However, CS mice spent less time in the open arms (Fig. 3C, stress factor, F (1, 28) = 33.26, p = <0.001; treatment factor, F (1, 28) = 1.858, p = 0.1837; interaction stress × treatment, F (1, 28) = 0.1038, p = 0.7497), more time in the closed arms (Fig. 3D, stress factor, F (1, 28) = 33.26, p < 0.0001; treatment factor, F (1, 28) = 1.858, p = 0.1837; interaction stress × treatment, F (1, 28) = 0.1039, p = 0.7496), and entered less the open arms (Fig. 3E, stress factor, F (1, 28) = 55.19, p < 0.0001; treatment factor F (1, 28) = 0.3799, p = 5426; interaction stress × treatment, F (1, 28) = 0.1273, p = 0.1273). The repeated LSD treatment failed to alter any of these parameters (p > 0.05). In the LDB test, the CS protocol produced fewer transitions between the light and dark compartments in mice treated with veh, an effect that was prevented by the LSD treatment (Fig. 3F, stress factor, F (1, 28) = 2.706, p = 0.1111; treatment factor, F (1, 28) = 3.568, p = 0.0693; interaction stress × treatment, F (1, 28) = 8.554, p = 0.0068). LSD treatment did not affect the time spent in the light compartment of the LDBT, for which the Two-way ANOVA analysis revealed a main effect of stress (Fig. 3G, F (1, 28) = 15.41, p = 0.0005) but not of treatment (F (1, 28) = 2.437, p = 0.1297), or of the interaction of the two (F (1, 28) = 0.1152, p = 0.7369). Finally, the same cohort of mice was tested in the NSFT. As expected, CS mice showed an increased latency to feed in the novel arena compared to CTL (Fig. 3H, stress factor, F (1, 28) = 6.564, p = 0.0159; treatment factor, F (1, 28) = 5.436, p = 0.0269; interaction stress × treatment, F (1, 28) = 3.163, p = 0.0005), confirming that the stress protocol exacerbated anxiety-like behavior. Importantly, LSD-treated stressed mice (last dose 24 h before the test) had a reduced latency to feed compared to veh-treated CS mice (p < 0.05). No difference was found in the latency to feed in the home cage (Fig. 3I, stress factor, F (1, 28) = 0.2289, p = 0.6359; treatment factor, F (1, 28) = 0.5332, p = 0.4711; interaction stress × treatment, F (1, 28) = 3.345, p = 0.0777). Overall, these data indicate that the repeated LSD at the dose of 30 µg/kg prevents the exacerbation of stress-induced anxiety-like behavior.
A Schematic timeline showing the stress procedure, drug treatment and behavioral procedures. Distance traveled (B), percentage of time spent in the open arm (C), percentage of time spent in the closed arm (D), and number of entries in the open arm (E) during the EPMT. F LSD normalizes the number of transition between the dark and the light compartment in the LDBT, which were decreased after CS. G Time spent in the light compartment during the LDBT. H Repeated LSD prevents the decreased latency to feed in stressed mice in the novel environment during the NSFT. No effect was detected in the home cage (I). Each bar represents mean ± SEM and each point represents a single mouse. LSD treatment and chronic stress procedure were ineffective to produce any change in the immobility time in the FST (J) and in the % of sucrose intake in the SPT (K). LSD treatment prevents the reduced spine density induced by the chronic stress paradigm and elicits an increase in spine density in veh-treated mice (L, M). Each bar or line represents mean ± SEM and each point represents a single mouse. Two-way ANOVA followed by Bonferroni post-hoc comparison; *p < 0.05; ***p < 0.001. N.S. not significant, veh vehicle, EPMT elevated plus maze, LDBT light-dark box test, NSFT novelty suppressed feeding test, FST forced swim test, SPT sucrose preference test, veh vehicle, CTL non-stressed control, CS chronic restraint stress.
Chronic restraint stress does not exacerbate depressive- and anhedonic-like behavior
Next, we assess whether the CS paradigm employed in the study produces depressive- and/or anhedonic-like behavior, as we previously observed using a model of chronic unpredictable stress [18]. Using another cohort of mice, we performed the sucrose preference test (SPT) and the forced swim test (FST). No differences were detected due to stress or repeated LSD (30 µg/kg) in the immobility time (Fig. 3J, stress factor, F (1, 36) = 0.2973, p = 0.2973; treatment factor, F (1, 36) = 0.8832, p = 0.3536; interaction stress × treatment, F (1, 36) = 0.0232, p = 0.8797) or sucrose preference (Fig. 3K, stress factor, F (1, 36) = 1.590, p = 0.2155; treatment factor, F (1, 36) = 0.6355, p = 0.4306; interaction stress × treatment, F (1, 36) = 0.5810, p = 0.4509).
Repeated LSD administration prevents the chronic stress-induced reduction of cortical spine density
Stress induces a remodeling of brain architecture, which is underpinned by changes in dendritic spines morphology and density [24, 25], particularly within the PFC [26]. Since previous experiments demonstrated that acute in vitro LSD administration increased the number of dendritic spines in rodent primary neuronal cultures [27], we thought to investigate whether repeated LSD during exposure to a repeated stressogenic insult prevents the stress-induced reduction in the number of apical dendritic spines in the mPFC. As expected, 15 days of chronic restraint stress reduced the number of dendritic spines, while LSD (30 µg/kg/day for 7 days, last dose 24 hours before the brain dissection) prevented this decline while also increasing spinogenesis in control mice (Fig. 3L, M, stress factor, F (1, 17) = 22.92, p < 0.001; treatment factor, F (1, 17) = 61.57, p < 0.001; interaction stress x treatment, F (1, 17) = 61.57, p < 0.001).
Acute and repeated LSD administration differentially impact 5-HT transmission in the DRN
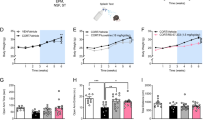
Drugs used to treat anxiety and depression like selective serotonin re-uptake inhibitors (SSRIs) produce a short-term decrease in 5-HT firing activity, followed by a desensitization of the 5- HT1A somatodendritic autoreceptors, leading, after some days of treatment, to a net increase in 5-HT neurotransmission [28, 29]. Given that acute LSD at the tested doses failed to produce any behavioral effects, whereas repeated LSD prevented the development of stress-induced anxiety-like phenotype and the decrease in cortical spinogenesis, we hypothesized that LSD could impact the DRN 5-HT transmission similarly to the SSRIs. Firstly, we tested the ability of acute cumulative injections of the 3 different doses of LSD employed in the CS protocol to modulate the 5-HT DRN activity in anesthetized mice (Fig. 4A, B). We found in non-stressed mice that acute LSD (5, 15 and 30 µg/kg, i.p.) decreased the spontaneous firing activity of DRN 5-HT neurons (Fig. 4C, D, RM One-way ANOVA, F (1.985, 7.941) = 34.41, p = 0.0001), similarly to the response previously observed in non-stressed rats [11, 30, 31]. Post-hoc analyses showed that LSD completely shut down DRN 5-HT activity at the dose of 30 µg/kg. We then tested how repeated administration of this dose of LSD (30 µg/kg, i.p., daily for 7 days, last dose 24 h before recording) affected 5-HT neurotransmission. The dose was chosen because i) it was the minimal dose to completely inhibit the 5-HT firing activity, ii) it was the only dose that could prevent the development of stress-induced anxiety-like behavior when administered for 7 days, iii) it produced a low extent of stereotypies. Intriguingly, following 7 days of treatment, LSD (30 µg/kg) significantly increased the mean spontaneous cell firing frequency of DRN 5-HT neurons (14 neurons recorded in 4 mice) compared with veh (10 neurons recorded in 4 mice) (Fig. 4E, F, t = 3.751, df = 26, p < 0.001). These effects were coupled to an increased numbers of spikes events in 200 s (Fig. 4G, F, t = 6.504, df = 26, p < 0.001. In addition, LSD produced an increased coefficient of variation percentage (Fig. 4H, t = 3.170, df = 26, p < 0.01) suggesting that repeated LSD administration triggered a more irregular firing activity as opposed to the regular or rhythmic firing activity in mice treated with veh. Indeed, interspike interval (ISI) histograms generated from the mean 5-HT neural activity showed a skewed ISI profile of mice treated with LSD compared with the normally distributed ISI profile of mice treated with veh (Fig. 4I). No significant difference was found in the percentage of neurons discharging in burst in mice treated with veh or LSD (Fig. 4J, χ2 test = 0.6222, df = 1, p = 0.4302).
A Representation of coronal sections of the mouse brain with the photomicrograph of the recording site in the DRN. Lateral periaqueductal gray (L-PAG); aqueduct (Aq). The black arrow indicates the site of the electrode recording labeled with pontamine sky blue dye. B The typical spike waveform of 5-HT neuron. C Acute intra-peritoneal (i.p.) LSD administration decreases the firing rate of DRN 5-HT neurons (n = 5 mice, one neuron per animal). Each point of the line represents mean ± SEM is expressed as percentage of baseline before injections of veh and LSD. D Representative firing rate histograms showing the acute response of 5-HT neurons to cumulative LSD administration. Black arrows indicate sequence of a single injection of veh and of increasing doses of LSD. E Short-term (7 days) repeated LSD administration (30 μg /kg/day, i.p.) increases DRN 5-HT mean firing activity compared with veh. Each bar represents mean ± SEM (n = 14 neurons recorded from 4 mice in both veh and LSD-treated groups). F Representative firing rate histograms of the mean DRN 5-HT firing rate activity recorded in mice treated with repeated veh or LSD. G Short-term (7 days) repeated LSD (30 μg /kg/day, i.p.) increases the number (#) of spikes events per 200 s recorded in 5-HT neurons compared to veh. Each bar represents mean ± SEM. H Repeated LSD reduces the regular firing pattern of 5-HT neurons as measured by the increased mean percentage of the coefficient of variation (COV) compared to veh. Each bar represents mean ± SEM and each point represent a single neuron recorded in each group. I ISI histograms of DRN 5-HT neural activity of mice treated with veh (black bars) and LSD (red bars) show irregular firing activity in mice treated with LSD (skewed ISI profile), as opposed to the regular or rhythmic firing activity in mice treated with veh (normally distributed ISI). J Contingency pie chart showing no significant difference in the number (#) of non-bursting (top) and bursting (bottom) DRN 5-HT neurons in mice treated with repeated veh or LSD. K Microiontophoretic ejection of increasing 8-OH-DPAT currents shows a significant difference in the response of DRN 5-HT neurons of mice treated with LSD compared to veh. Each point of the line represents mean ± SEM. L Representative firing rate histogram showing the effect of microiontophoretic ejection of 8-OH-DPAT currents on 5-HT DRN neurons in mice treated with repeated veh (black) or LSD (red) *p < 0.05, **p < 0.01 and ***p < 0.001 vs veh. ##p < 0.01, ##p < 0.001 vs baseline. mv millivolt, ms millisecond, veh vehicle, nA nanoampere, s seconds.
To determine whether the increase in DRN 5-HT firing after repeated LSD administration was due to altered 5-HT1A autoreceptor sensitivity, as observed for SSRIs [32], we performed in vivo electrophysiological recordings with multi-barreled electrodes for microionthophoretic ejections [33]. To assess the 5-HT1A receptor sensitivity, we tested the inhibitory response to microionthophoretic ejections of increasing doses of the 5-HT1A selective agonist 8-OH-DPAT [33]. While the 5-HT1A agonist decreased in a current-dependent manner the DRN 5-HT firing activity of mice treated with veh, LSD-treated mice showed a statistically significant attenuation of the inhibitory response (Fig. 4K, L, current factor, F (2.353, 61.17) = 46.30, p < 0.001; treatment factor F (1,26) = 11.89, p < 0.001; interaction current × treatment F (3,78) = 11.89, p < 0.001). Together, these data indicate that 7-day treatment with LSD (30 µg/kg) reduced the sensitivity of DRN 5-HT neurons to the inhibitory effect of the 5-HT1A agonist. Given the affinity of the 8-OH-DPAT for the 5-HT7 receptor [34, 35], and also to confirm that the 5-HT1A is desensitized even when 8-OH-DPAT is systemically injected, we performed additional electrophysiological experiments in naïve animals treated with LSD alone or vehicle, by administering the 5-HT7 receptor antagonist SB269970 (1 mg;kg, i.p. [36, 37]) 10 min prior to the acute cumulative injections of 8-OH-DPAT (5–20 µg/kg, i.p. given every 5 min). SB269970 did not affect the inhibitory effect of cumulative injection of 8-OH-DPAT in 7-day vehicle-treated animals (8-OH-DPAT effect, F (4, 20) = 5.797, p = 0.0029; treatment effect, F (1, 5) = 0.04544, p = 0.8396; interaction 8-OH-DPAT effect × treatment, F (4, 20) = 0.02983, P = 0.9981). In mice treated with 7-day LSD (30 µg/kg), the cumulative injection of 8-OH-DPAT produced an attenuated response, compared to vehicle-treated animals, and the injection of the SB269970 prior 8-OH-DPAT did not impact this effect, confirming that 7-day LSD treatment induces a desensitization of the 5-HT1A receptors and this effects is not mediated by the 5-HT7 receptors (8-OH-DPAT main effect, F (4, 44) = 7.146, p = 0.0002; treatment F (2, 11) = 12.95, p = 0.0013; interaction 8-OH-DPAT effect × treatment, F(8, 44) = 4.712, p = 0.0003) (Supplementary Fig. S1).
Repeated LSD administration prevents the stress-induced decline of 5-HT DRN neurons firing
We previously demonstrated that chronic unpredictable stress produces a decline of the 5-HT DRN firing activity in rats and impairs the 5-HT1A receptor responsiveness [18]. Therefore, we investigated if chronic restraint stress produces the same effects and if a repeated LSD regimen (30 µg/kg daily for 7 days) could prevent the stress-induced decline of DRN 5-HT neuronal activity (Fig. 5A, B). We performed in vivo electrophysiological recordings in an additional cohort of stressed and non-stressed mice. As expected, CS decreased the spontaneous firing rate activity of DRN 5-HT neurons compared to control (stress factor, F (1, 156) = 22.87, p < 0.001; treatment factor, F (1, 156) = 44.58, p < 0.001; interaction stress x treatment, F (1, 156) = 3.999, p = 0.0473). Importantly, post-hoc analysis revealed that the firing rate of DRN 5-HT neurons in stressed mice treated with LSD was higher compared to stressed mice treated with veh (Fig. 5C, D, p < 0.001). Our results confirm that chronic stress impairs 5-HT neurotransmission in the DRN and show that a 7-day repeated LSD treatment during the last 7 days of stress prevents this neuronal impairment.
A Schematic timeline showing the stress procedure, drug treatment and electrophysiological procedure. B Representation of coronal sections of the mouse DRN region. C 15 day regimen of CS reduced the 5-HT DRN firing activity. 7 day treatment of LSD at the dose of 30 μg/kg, but not at 5 μg/kg and 15 μg/kg, normalizes the neuronal activity to CTL level. D Representative firing rate histogram of the 5-HT DRN neuronal activity in CTL and CS mice treated with veh or 7 days LSD (30 μg/kg/day). Each line represents mean ± SEM and each point represents a single recorded neuron. Two-way ANOVA followed by Bonferroni post-hoc comparison; *p < 0.05; ***p < 0.001; n.s. not significant, veh vehicle, CTL non-stressed control, CS chronic restraint stress.
Discussion
Recently, psychedelic compounds have come to the forefront as potential novel therapeutics in psychiatry, especially at low- and non-hallucinogenic doses [1,2,3, 38]. Despite ongoing research efforts, the neurobiological mechanism(s) of action mediating their therapeutic effects remain elusive. Here, we explored two potential mechanisms of anxiolytic action of psychedelics, specifically LSD. While acute LSD did not affect anxiety-like and depressive-like behavior in naïve mice, repeated administration (30 μg/kg/day for 7days, but not 5 and 15 μg/kg) during stress exposure prevented the development of anxiety-like behavior, suggesting an anxiolytic-like effect of repeated LSD under anxiogenic conditions. In parallel, we found that repeated LSD administration prevented the CS-induced cortical synaptogenesis impairments, while also increasing spine density in naïve mice. Interestingly, while acute cumulative injections of LSD decreased the 5-HT neuronal activity in the DRN, repeated LSD administration increased the 5-HT firing activity likely via desensitizing the 5-HT1A receptor in naïve animals. On the other hand, LSD prevented the CS-induced decline of the 5-HT firing rate, thus maintaining an average firing rate within control values. These data show that while behaviorally the effects of LSD were only detectable in stressed mice, electrophysiological and morphological changes were observable also in the non-stress conditions.
Our findings corroborate clinical results pointing toward an anxiolytic effect of LSD [39]. Indeed, studies on patients experiencing anxiety and distress associated with a terminal disease reported rapid and sustained improvements in anxiety scores, for up to six months following one or two administrations of LSD [9] or other psychedelics such as psilocybin [40, 41]. Preclinical evidence concerning the anxiolytic- and antidepressants-like effects of LSD remains controversial. In a recent study LSD did not elicit anxiolytic-like effects in the elevated plus maze test in rats, but it induced a sustained antidepressant-like effect in the forced swim test 5 weeks after a single LSD administration (0.15 mg/kg) [42]. A previous study found that repeated LSD (0.13 mg/kg daily for 11 days) reversed the stress-induced deficits in active avoidance learning and normalized 5-HT2A receptor-mediated hippocampal 5-HT signaling in a model of depression [43]. Another recent study reported that a high dose of LSD (0.3 mg/kg) induces an antidepressant-like trend in the tail suspension test (TST), but this trend did not reach statistical significance [44]. Similarly, in zebrafish, LSD was reported to induce anxiolytic-like effects [45]. Concerning other serotonergic psychedelics, chronic intermittent administration of N,N-Dimethyltryptamine (1 mg/kg, once every 3 days for 30 days), elicited antidepressant-like effect in female, but not male, rats [46]. Moreover, while psilocybin did not rescue the depressive-like phenotype of the Flinders Sensitive Line rat model of depression [47], it reversed some of the behavioral and electrophysiological effects of chronic stress in mice [48]. Lastly, a Psilocybe cubensis extract at the dose of 10 and 40 mg/kg did not induce antidepressant-like effects in the FST [49]. In the present study, in naïve mice, none of the chosen doses (5, 15, 30 and 60 µg/kg) elicited anxiolytic- and/or antidepressant-like effects. Therefore, to assess potential anxiolytic effects of LSD in stress conditions we performed a 15 day-chronic restraint stress paradigm, which exacerbates anxiety-like behavior [50,51,52,53]. Indeed, 7 days of repeated LSD at the dose of 30 µg/kg prevented the exacerbation of stress-induced anxiety-like behavior, uncovering a protective role of LSD on stress-induced phenotypes which was not detectable under basal conditions. Considering these results, it will be worth to investigate if even a single LSD injection produces protective/anxiolytic effects after 7–8 days in acute restraint stress model.
Neurogenesis and synaptogenesis are evoked as plasticity mechanism underlying the mechanism of action of approved antidepressants [54, 55] and psychedelic compounds [27], attenuating the negative effects of stress and depression on hippocampal [56] and prefrontal cortex [57] plasticity. This is supported by the stimulation of dendritic spines growth, synapse formation and dendritic arbor complexity in cortical rat cell cultures [27]. Accordingly, a recent study reported powerful neurogenic effects of DMT in the subgranular zone of the mouse dentate gyrus of the hippocampus accompanied by an enhancement of memory [58]. In partial contrast, a study investigating the effects of repeated DMT administration in mice reported a decrease in cortical dendritic spines density in females, but not male rats [46]. In the present study we observed that repeated LSD increased the number of apical dendritic spines in the mPFC in naïve animals, while preventing the stress-induced decrease of apical dendritic spines. Previously, we showed that LSD induced an increase in firing rate of a subset of neurons of the mouse infralimbic cortex, while modulating the cortico-thalamo-cortical system [59]. Further supporting a potential synaptogenic effect of LSD, human studies reported that microdoses of LSD transiently increase BDNF levels [60], as also reported for Ayahuasca [61]. BDNF-induced glutamate release has been shown to decrease following chronic restraint stress, together with glucocorticoid receptor expression [52]. In line with the current findings, LSD increased synaptic plasticity in brain organoids, an effect accompanied by increased expression of proteins involved in synaptogenesis and plasticity, such as synaptophysin, glutamate metabotropic receptor 7, and synaptic vesicle glycoprotein 2A [62].
LSD shares with antidepressants not only the capacity to increase the density of apical dendritic spines in the mPFC [57], which is hypothesized to endure antidepressant effects but also the capacity to potentiate the 5-HT neurotransmission. Being LSD a 5-HT1A receptor agonist, as expected [63] after acute injection, it decreased DRN 5-HT firing activity, by acting on the 5-HT1A autoreceptors [64]. However, after a 7-day regimen, it increased DRN 5-HT firing activity, likely due to a desensitization of the 5-HT1A autoreceptors. Interestingly, in these experiments we also observed that a 15 day restraint stress protocol reduces DRN 5-HT firing activity similarly to a 3-week chronic unpredictable stress paradigm [18], and that LSD can prevent this decrease.
The behavioral outcomes of this study should be interpreted in light of their limitations. We have used a battery of tests which are considered the gold-standard test for the screening of putative antianxiety/antidepressant drugs even if they show limitations in the interpretation of the real behavior [65,66,67]. The chronic stress paradigm used in this study did not induce depressive-like behavior. This is in line with other reports suggesting that chronic restraint stress is a paradigm which reliably induces anxiety-like behavior, but less reliably induces depressive-like behavior [50,51,52,53]. Studies investigating potential antidepressant-like effects of LSD could use different chronic stress paradigms, which more reliably exacerbate depressive-like behavior in rodents, such as the chronic unpredictable stress model [18] or the chronic social defeat stress paradigm [68]. Moreover, previous animal research highlighted that chronic stress protocols might affect memory. Even if the results are still controversial [69, 70], we cannot rule out that the effects of stress and the reversal induced by LSD may be linked to its direct effects on memory and not on anxiety per se. In this study we showed that LSD prevented the development of anxiety-like phenotype and 5-HT decline following the stress procedure; however, whether this protective effect would persist for weeks or even months after the last LSD injection remains unknown and more investigations are needed. Another limitation of the study is the lack of sex difference outcomes following LSD administration. Studies in the literature concerning the differential impact of psychedelics on sex are still unclear in animal models [71] and further research on this topic is necessary.
In conclusion, repeated, but not acute, low doses of LSD prevent the exacerbation of stress-induced anxiety-like behavior without affecting depressive-like behavior or other behavioral measures. Moreover, while acute LSD decreases 5-HT neuronal firing in the DRN, repeated LSD enhances it, likely through a desensitization of the 5-HT1A somatodendritic autoreceptors. Lastly, repeated LSD administration increases dendritic spine density in mPFC pyramidal neurons and prevents the stress-induced decrease in cortical dendritic spines density. Together, these results suggest that the anxiolytic properties of LSD might be mediated by a mechanism of action involving an enhancement of 5-HT neurotransmission, an increase in cortical synaptogenesis, or both. Together with our previous finding showing that the repeated treatment employed here is associated to an activation of mTORC1 and a potentiation of AMPA/5-HT2A responses in the mPFC [15], the current findings provide a potential mechanistic explanation of neurobiological mechanisms which might underlie the anxiolytic and antidepressant effects of psychedelic compounds. Clinical studies are warranted to determine the minimum acute and repeated LSD dose necessary to induce anxiolytic outcomes in psychiatric populations, while assessing the duration of such effects, and determine the most effective regimen. Future studies should assess the anxiolytic effects of repeated LSD administration in people diagnosed with anxiety disorders not associated with a terminal illness [9]. These efforts could help elucidate whether LSD elicits similar protective effects on anxiety, neurotransmission and neuroplasticity in anxiety disorders.
References
Nutt D. Psychedelic drugs-a new era inpsychiatry? Dialogues Clin Neurosci. 2019;21:139–47.
Inserra A, De Gregorio D, Gobbi G. Psychedelics in psychiatry: neuroplastic, immunomodulatory, and neurotransmitter mechanisms. Pharm Rev. 2021;73:202–77.
Vollenweider FX, Preller KH. Psychedelic drugs: neurobiology and potential for treatment of psychiatric disorders. Nat Rev Neurosci. 2020;21:611–24.
Dolder PC, Schmid Y, Müller F, Borgwardt S, Liechti ME. LSD acutely impairs fear recognition and enhances emotional empathy and sociality. Neuropsychopharmacology. 2016;41:2638.
Mueller F, Lenz C, Dolder PC, Harder S, Schmid Y, Lang UE, et al. Acute effects of LSD on amygdala activity during processing of fearful stimuli in healthy subjects. Transl Psychiatry. 2017;7:e1084.
Schmid Y, Liechti ME. Long-lasting subjective effects of LSD in normal subjects. Psychopharmacology. 2018;235:535–45.
Carhart-Harris RL, Kaelen M, Bolstridge M, Williams T, Williams L, Underwood R, et al. The paradoxical psychological effects of lysergic acid diethylamide (LSD). Psychological Med. 2016;46:1379–90.
Gasser P, Kirchner K, Passie T. LSD-assisted psychotherapy for anxiety associated with a life-threatening disease: a qualitative study of acute and sustained subjective effects. J Psychopharmacol. 2015;29:57–68.
Gasser P, Holstein D, Michel Y, Doblin R, Yazar-Klosinski B, Passie T, et al. Safety and efficacy of lysergic acid diethylamide-assisted psychotherapy for anxiety associated with life-threatening diseases. J Nerv Ment Dis. 2014;202:513.
ClinicalTrials.gov. LSD therapy for persons suffering from major depression (LAD). ClinicalTrials.gov Identifier: NCT03866252; https://clinicaltrials.gov/ct2/show/NCT03866252. 2019.
De Gregorio D, Posa L, Ochoa-Sanchez R, McLaughlin R, Maione S, Comai S, et al. The hallucinogen d-lysergic diethylamide (LSD) decreases dopamine firing activity through 5-HT1A, D2 and TAAR1 receptors. Pharmacol Res. 2016;113:81–91.
De Gregorio D, Comai S, Posa L, Gobbi G. d-Lysergic acid diethylamide (LSD) as a model of psychosis: mechanism of action and pharmacology. Int J Mol Sci. 2016;17:1953.
Marona-Lewicka D, Chemel BR, Nichols DE. Dopamine D 4 receptor involvement in the discriminative stimulus effects in rats of LSD, but not the phenethylamine hallucinogen DOI. Psychopharmacology. 2009;203:265–77.
Martin DA, Marona-Lewicka D, Nichols DE, Nichols CD. Chronic LSD alters gene expression profiles in the mPFC relevant to schizophrenia. Neuropharmacology. 2014;83:1–8.
De Gregorio D, Popic J, Enns JP, Inserra A, Skalecka A, Markopoulos A, et al. Lysergic acid diethylamide (LSD) promotes social behavior through mTORC1 in the excitatory neurotransmission. Proc Natl Acad Sci. 2021;118:e2020705118.
Lowry CA, Hale MW, Evans AK, Heerkens J, Staub DR, Gasser PJ, et al. Serotonergic systems, anxiety, and affective disorder: focus on the dorsomedial part of the dorsal raphe nucleus. Ann N Y Acad Sci. 2008;1148:86–94.
Nishitani N, Nagayasu K, Asaoka N, Yamashiro M, Andoh C, Nagai Y, et al. Manipulation of dorsal raphe serotonergic neurons modulates active coping to inescapable stress and anxiety-related behaviors in mice and rats. Neuropsychopharmacology. 2019;44:721–32.
Bambico FR, Nguyen N-T, Gobbi G. Decline in serotonergic firing activity and desensitization of 5-HT1A autoreceptors after chronic unpredictable stress. Eur Neuropsychopharmacol. 2009;19:215–28.
Pittenger C, Duman RS. Stress, depression, and neuroplasticity: a convergence of mechanisms. Neuropsychopharmacology. 2008;33:88–109.
Hill MN, Kumar SA, Filipski SB, Iverson M, Stuhr KL, Keith JM, et al. Disruption of fatty acid amide hydrolase activity prevents the effects of chronic stress on anxiety and amygdalar microstructure. Mol Psychiatry. 2013;18:1125–35.
Aghajanian GK, Foote WE, Sheard MH. Lysergic acid diethylamide: sensitive neuronal units in the midbrain raphe. Science. 1968;161:706–08.
De Gregorio D, Popic J, Enns JP, Inserra A, Skalecka A, Markopoulos A, et al. Lysergic acid diethylamide (LSD) promotes social behavior through mTORC1 in the excitatory neurotransmission. Proc Natl Acad Sci. 2021;118:e2020705118.
Borison RL, Havdala HS, Diamond BI. Chronic phenylethylamine stereotypy in rats: a new animal model for schizophrenia? Life Sci. 1977;21:117–22.
Duman RS, Aghajanian GK, Sanacora G, Krystal JH. Synaptic plasticity and depression: new insights from stress and rapid-acting antidepressants. Nat Med. 2016;22:238–49.
Popoli M, Yan Z, McEwen BS, Sanacora G. The stressed synapse: the impact of stress and glucocorticoids on glutamate transmission. Nat Rev Neurosci. 2012;13:22–37.
Liston C, Miller MM, Goldwater DS, Radley JJ, Rocher AB, Hof PR, et al. Stress-induced alterations in prefrontal cortical dendritic morphology predict selective impairments in perceptual attentional set-shifting. J Neurosci. 2006;26:7870–74.
Ly C, Greb AC, Cameron LP, Wong JM, Barragan EV, Wilson PC, et al. Psychedelics promote structural and functional neural plasticity. Cell Rep. 2018;23:3170–82.
Blier P, de Montigny C. Current advances and trends in the treatment of depression. Trends Pharmacol Sci. 1994;15:220–6.
Artigas F, Romero L, de Montigny C, Blier P. Acceleration of the effect of selected antidepressant drugs in major depression by 5-HT1A antagonists. Trends Neurosci. 1996;19:378–83.
Aghajanian GK, Foote WE, Sheard MH. Action of psychotogenic drugs on single midbrain raphe neurons. J Pharmacol Exp Therap. 1970;171:178–87.
Haigler HJ, Aghajanian GK. Mescaline and LSD: direct and indirect effects on serotonin-containing neurons in brain. Eur J Pharmacol. 1973;21:53–60.
Gobbi G, Blier P. Effect of neurokinin-1 receptor antagonists on serotoninergic, noradrenergic and hippocampal neurons: comparison with antidepressant drugs. Peptides. 2005;26:1383–93.
Bambico FR, Cassano T, Dominguez-Lopez S, Katz N, Walker CD, Piomelli D, et al. Genetic deletion of fatty acid amide hydrolase alters emotional behavior and serotonergic transmission in the dorsal raphe, prefrontal cortex, and hippocampus. Neuropsychopharmacology. 2010;35:2083–100.
Hedlund PB, Kelly L, Mazur C, Lovenberg T, Sutcliffe JG, Bonaventure P. 8-OH-DPAT acts on both 5-HT1A and 5-HT7 receptors to induce hypothermia in rodents. Eur J Pharmacol. 2004;487:125–32.
Sprouse J, Reynolds L, Li X, Braselton J, Schmidt A. 8-OH-DPAT as a 5-HT7 agonist: phase shifts of the circadian biological clock through increases in cAMP production. Neuropharmacology. 2004;46:52–62.
Nikiforuk A, Kos T, Fijał K, Hołuj M, Rafa D, Popik P. Effects of the selective 5-HT7 receptor antagonist SB-269970 and amisulpride on ketamine-induced schizophrenia-like deficits in rats. PLoS One. 2013;8:e66695.
Guscott M, Egan E, Cook G, Stanton J, Beer M, Rosahl T, et al. The hypothermic effect of 5-CT in mice is mediated through the 5-HT7 receptor. Neuropharmacology. 2003;44:1031–37.
Markopoulos A, Inserra A, De Gregorio D, Gobbi G. Evaluating the potential use of serotonergic psychedelics in autism spectrum disorder. Front Pharmacol. 2022;12:749068.
dos Santos RG, Osório FL, Crippa JAS, Riba J, Zuardi AW, Hallak JEC. Antidepressive, anxiolytic, and antiaddictive effects of ayahuasca, psilocybin and lysergic acid diethylamide (LSD): a systematic review of clinical trials published in the last 25 years. Therap Adv Psychopharmacol. 2016;6:193–213.
Grob CS, Danforth AL, Chopra GS, Hagerty M, McKay CR, Halberstadt AL, et al. Pilot study of psilocybin treatment for anxiety in patients with advanced-stage cancer. Arch Gen Psychiatry. 2011;68:71–78.
Griffiths RR, Johnson MW, Carducci MA, Umbricht A, Richards WA, Richards BD, et al. Psilocybin produces substantial and sustained decreases in depression and anxiety in patients with life-threatening cancer: a randomized double-blind trial. J Psychopharmacol. 2016;30:1181–97.
Hibicke M, Landry AN, Kramer HM, Talman ZK, Nichols CD. Psychedelics, but not ketamine, produce persistent antidepressant-like effects in a rodent experimental system for the study of depression. ACS Chem Neurosci. 2020;11:864–71.
Buchborn T, Schröder H, Höllt V, Grecksch G. Repeated lysergic acid diethylamide in an animal model of depression: normalisation of learning behaviour and hippocampal serotonin 5-HT2 signalling. J Psychopharmacol. 2014;28:545–52.
Vesuna S, Kauvar IV, Richman E, Gore F, Oskotsky T, Sava-Segal C, et al. Deep posteromedial cortical rhythm in dissociation. Nature. 2020;586:87–94.
Grossman L, Utterback E, Stewart A, Gaikwad S, Chung KM, Suciu C, et al. Characterization of behavioral and endocrine effects of LSD on zebrafish. Behavioural Brain Res. 2010;214:277–84.
Cameron LP, Benson CJ, DeFelice BC, Fiehn O, Olson DE. Chronic, intermittent microdoses of the psychedelic N, N-Dimethyltryptamine (DMT) produce positive effects on mood and anxiety in rodents. ACS Chem Neurosci. 2019;10:3261–70.
Jefsen O, Højgaard K, Christiansen SL, Elfving B, Nutt DJ, Wegener G, et al. Psilocybin lacks antidepressant-like effect in the Flinders Sensitive Line rat. Acta Neuropsychiatrica. 2019;31:213–19.
Hesselgrave N, Troppoli TA, Wulff AB, Cole AB, Thompson SM. Harnessing psilocybin: antidepressant-like behavioral and synaptic actions of psilocybin are independent of 5-HT2R activation in mice. Proc Natl Acad Sci. 2021;118:e2022489118.
Mahmoudi E, Faizi M, Hajiaghaee R, Razmi A. Alteration of depressive-like behaviors by psilocybe cubensis alkaloid extract in mice: the role of glutamate pathway. Res J Pharmacogn. 2018;5:17–24.
Wong M-L, Inserra A, Lewis M, Mastronardi CA, Leong L, Choo J, et al. Inflammasome signaling affects anxiety-and depressive-like behavior and gut microbiome composition. Mol Psychiatry. 2016;21:797–805.
Strekalova T, Couch Y, Kholod N, Boyks M, Malin D, Leprince P, et al. Update in the methodology of the chronic stress paradigm: internal control matters. Behav Brain Funct. 2011;7:1–18.
Chiba S, Numakawa T, Ninomiya M, Richards MC, Wakabayashi C, Kunugi H. Chronic restraint stress causes anxiety-and depression-like behaviors, downregulates glucocorticoid receptor expression, and attenuates glutamate release induced by brain-derived neurotrophic factor in the prefrontal cortex. Prog Neuro-Psychopharmacol Biol Psychiatry. 2012;39:112–19.
Li H, Buisman-Pijlman FTA, Nunez-Salces M, Christie S, Frisby CL, Inserra A, et al. Chronic stress induces hypersensitivity of murine gastric vagal afferents. Neurogastroenterol Motil. 2019;31:e13669.
Bambico FR, Belzung C. Novel insights into depression and antidepressants: a synergy between synaptogenesis and neurogenesis? Curr Top Behav Neurosci. 2013;15:243–91.
Li N, Lee B, Liu RJ, Banasr M, Dwyer JM, Iwata M, et al. mTOR-dependent synapse formation underlies the rapid antidepressant effects of NMDA antagonists. Science. 2010;329:959–64.
Santarelli L, Saxe M, Gross C, Surget A, Battaglia F, Dulawa S, et al. Requirement of hippocampal neurogenesis for the behavioral effects of antidepressants. Science. 2003;301:805–9.
Moda-Sava RN, Murdock MH, Parekh PK, Fetcho RN, Huang BS, Huynh TN, et al. Sustained rescue of prefrontal circuit dysfunction by antidepressant-induced spine formation. Science. 2019;364:eaat8078.
Morales-Garcia JA, Calleja-Conde J, Lopez-Moreno JA, Alonso-Gil S, Sanz-SanCristobal M, Riba J, et al. N,N-dimethyltryptamine compound found in the hallucinogenic tea ayahuasca, regulates adult neurogenesis in vitro and in vivo. Transl Psychiatry. 2020;10:331.
Inserra A, De Gregorio D, Rezai T, Lopez-Canul MG, Comai S, Gobbi G. Lysergic acid diethylamide differentially modulates the reticular thalamus, mediodorsal thalamus, and infralimbic prefrontal cortex: An in vivo electrophysiology study in male mice. J Psychopharmacol. 2021;35:469–82.
NRPW Hutten, Mason NL, Dolder PC, Theunissen EL, Holze F, Liechti ME, et al. Low doses of LSD acutely increase BDNF blood plasma levels in healthy volunteers. ACS Pharmacol Trans Sci. 2021;4:461–66.
Almeida RND, Galvão ACDM, da Silva FS, Silva EADS, Palhano-Fontes F, Maia-de-Oliveira JP, et al. Modulation of serum brain-derived neurotrophic factor by a single dose of ayahuasca: observation from a randomized controlled trial. Front Psychol. 2019;10:1234.
Cini FA, Ornelas I, Marcos E, Goto-Silva L, Nascimento J, Ruschi S, et al. d-Lysergic acid diethylamide has major potential as a cognitive enhancer. bioRxiv. 2019, https://www.biorxiv.org/content/10.1101/866814v1.
Willner P. Antidepressants and serotonergic neurotransmission: an integrative review. Psychopharmacology. 1985;85:387–404.
Andrade R, Huereca D, Lyons JG, Andrade EM, McGregor KM. 5-HT1A receptor-mediated autoinhibition and the control of serotonergic cell firing. ACS Chem Neurosci. 2015;6:1110–15.
Anyan J, Amir S. Too depressed to swim or too afraid to stop? A reinterpretation of the forced swim test as a measure of anxiety-like behavior. Neuropsychopharmacology. 2018;43:931–33.
Molendijk ML, de Kloet ER. Coping with the forced swim stressor: current state-of-the-art. Behavioural brain Res. 2019;364:1–10.
Commons KG, Cholanians AB, Babb JA, Ehlinger DG. The rodent forced swim test measures stress-coping strategy, not depression-like behavior. ACS Chem Neurosci. 2017;8:955–60.
Der-Avakian A, Mazei-Robison MS, Kesby JP, Nestler EJ, Markou A. Enduring deficits in brain reward function after chronic social defeat in rats: susceptibility, resilience, and antidepressant response. Biol Psychiatry. 2014;76:542–49.
Moreira PS, Almeida PR, Leite-Almeida H, Sousa N, Costa P. Impact of chronic stress protocols in learning and memory in rodents: systematic review and meta-analysis. PLoS One. 2016;11:e0163245.
Patki G, Solanki N, Atrooz F, Allam F, Salim S. Depression, anxiety-like behavior and memory impairment are associated with increased oxidative stress and inflammation in a rat model of social stress. Brain Res. 2013;1539:73–86.
Meehan SM, Schechter MD. LSD produces conditioned place preference in male but not female fawn hooded rats. Pharmacol Biochem Behav. 1998;59:105–08.
Funding
This work was supported by Grant 436986 from the CIHR, and the Quebec Network for Suicide, Mood Disorders, and Related Disorders (RQSHA, FRQS Grant 268065).
Author information
Authors and Affiliations
Contributions
DDG and GG designed research; DDG, AI, AM, JPE, MP, YER, ML-C, performed experiments and analyzed data; SC analyzed data and wrote manuscript; DDG, AI and GG wrote manuscript. GG supervised the whole work.
Corresponding author
Ethics declarations
Competing interests
DDG is a consultant at Diamond Therapeutics Inc, Toronto, ON, Canada. GG and DDG are inventors of a pending patent regarding the use of LSD. DDG was a recipient of Fond Recherche Québec-Santé (FRQS) and a Canadian Institutes for Health Research (CIHR) postdoctoral fellowships. AI is a recipient of a CIHR, FRQS and a Quebec Autism Research Training Program (QART) postdoctoral fellowships. ML-C was a recipient of a Faculty of Medicine of McGill University/Ferring postdoctoral fellowship. The other authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
De Gregorio, D., Inserra, A., Enns, J.P. et al. Repeated lysergic acid diethylamide (LSD) reverses stress-induced anxiety-like behavior, cortical synaptogenesis deficits and serotonergic neurotransmission decline. Neuropsychopharmacol. 47, 1188–1198 (2022). https://doi.org/10.1038/s41386-022-01301-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41386-022-01301-9
This article is cited by
-
Modulation of long-term potentiation following microdoses of LSD captured by thalamo-cortical modelling in a randomised, controlled trial
BMC Neuroscience (2024)
-
Therapeutic mechanisms of psychedelics and entactogens
Neuropsychopharmacology (2024)
-
The role of neurotrophic factors in novel, rapid psychiatric treatments
Neuropsychopharmacology (2024)
-
Repeated microdoses of LSD do not alter anxiety or boldness in zebrafish
Scientific Reports (2024)
-
Towards an understanding of psychedelic-induced neuroplasticity
Neuropsychopharmacology (2023)