Abstract
Morphine remains one of the most widely prescribed opioids for alleviation of persistent and/or severe pain; however, multiple preclinical and clinical studies report that morphine is less efficacious in females compared to males. Morphine primarily binds to the mu opioid receptor, a prototypical G-protein coupled receptor densely localized in the midbrain periaqueductal gray. Anatomical and physiological studies conducted in the 1960s identified the periaqueductal gray, and its descending projections to the rostral ventromedial medulla and spinal cord, as an essential descending inhibitory circuit mediating opioid-based analgesia. Remarkably, the majority of studies published over the following 30 years were conducted in males with the implicit assumption that the anatomical and physiological characteristics of this descending inhibitory circuit were comparable in females; not surprisingly, this is not the case. Several factors have since been identified as contributing to the dimorphic effects of opioids, including sex differences in the neuroanatomical and neurophysiological characteristics of the descending inhibitory circuit and its modulation by gonadal steroids. Recent data also implicate sex differences in opioid metabolism and neuroimmune signaling as additional contributing factors. Here we cohesively present these lines of evidence demonstrating a neural basis for sex differences in opioid modulation of pain, with a focus on the PAG as a sexually dimorphic core of descending opioid-induced inhibition and argue for the development of sex-specific pain therapeutics.
Similar content being viewed by others
Introduction
Pain is a submodality of somatosensation that is necessary for survival, yet pain may also occur and/or persist in the absence of actual or threatened tissue damage. Chronic pain, defined as pain lasting more than 3–6 months, will affect more than one in three Americans in our lifetime [1]. In the most recent National Health Interview Survey, it was reported that 55.7% of adults in the United States experienced acute pain within the past 3 months, while 11.2% reported experiencing chronic pain (reported as daily pain for 3 months) [2]. The prevalence and ineffective management of chronic pain is burdensome not only to the individual sufferer, but also to family members, employers, and the healthcare system [3]. Chronic pain disproportionately affects women who are 2–3× more likely to be diagnosed with and treated for chronic pain disorders, including fibromyalgia, headaches and migraine, temporomandibular joint disorder pain, irritable bowel syndrome, and osteoarthritis [4,5,6,7,8,9].
Despite their introduction over five millennia ago, opioids remain the most common therapeutic treatment for the management of chronic pain [10, 11]. It has been reported that as many as 3–5% of adults in the United States are prescribed long-term opioid therapy [12]. A recent survey of persistent pain patients showed that 60% were prescribed morphine, 37% fentanyl, and 2.5% buprenorphine, with an average length of treatment of 105 days [13]. While opioids are highly effective and often necessary for the management of many persistent and severe pain conditions, prolonged use results in decreased analgesic efficacy (i.e., tolerance) and the requirement for steadily larger doses of opioids for pain management (i.e., dose-escalation) [14, 15]. Opioids also elicit a multitude of undesired central nervous system-mediated side effects including sedation, decreased motor coordination and cognition, depressed pulmonary ventilation, reduced cardiac output, increased risk of mortality by overdose [16, 17], and severe constipation requiring secondary pharmaceutical interventions [18]. For some, pain management with opioids results in opioid-induced hyperalgesia, a paradoxical effect of opioids resulting in enhanced sensitivity to pain [19].
From these reports, it is discernible that the development of tolerance and the requirement for dose-escalation not only leads to many or all of the aforementioned negative side effects but also heightens the risk of developing opioid addiction in chronic pain patients. This issue has been at the forefront of recent headlines as reporting heightens amidst the current opioid crisis in America. According to the Department of Defense Survey of Health-related Behaviors in active military service members, a demographic currently dealing with an increase in chronic pain patients, there was a tripling of prescription drug abuse between 2005 and 2008 [20]. Curbing addiction to prescription painkillers is now a top priority of the Office of The Army Surgeon General (May 2010) [177].
The analgesic properties of systemically administered opioids are mediated primarily via the endogenous descending pain modulatory circuit, consisting of the midbrain periaqueductal gray (PAG) and its descending projections to the rostral ventromedial medulla (RVM) and spinal dorsal horn (SDH) (see Fig. 1) [21,22,23,24,25]. Opioid receptors are densely populated within all three regions, and administration of opioids can elicit analgesia at each of these target sites [26,27,28,29,30,31,32]. Although the PAG, RVM, and spinal cord dorsal horn are all critical for opioid modulation of pain, this review focuses on the PAG as numerous lines of evidence indicate that the PAG is a primary site for opiate action. Direct administration of morphine into the PAG produces long-lasting analgesia, while site-specific blockade of opioid receptors in the PAG attenuates the analgesic effects of systemic morphine [29, 33, 34]. Additionally, repeated administration of morphine directly into the PAG induces tolerance [34,35,36,37,38,39]. Opioid-induced cardiorespiratory dampening has also been attributed to the effect of PAG signaling on cardiorespiratory regulation [40, 41].
A schematic of the descending inhibitory pathway for pain modulation illustrating the projections from the caudal ventrolateral column of the midbrain periaqueductal gray to the rostral ventromedial medulla in the brainstem and the dorsal horn of the spinal cord at the level of incoming stimulation from sensory neurons of the dorsal root ganglia. Also indicated are local GABAergic interneurons (purple) and PAG–RVM output neurons (orange) and a local glial cell population (blue) that also signals to the PAG–RVM output neurons. Mu opioid receptors expressed on local GABAergic interneurons and PAG–RVM output neurons are also indicated
Sex differences in morphine analgesia
Both preclinical and clinical research over the last three decades has implicated sex as a biological variable influencing opioid modulation of pain. Sex differences in morphine attenuation of persistent and/or severe pain have been attributed, in part, to sexual dimorphism in the neuroanatomical, neurophysiological, and neuroimmunological aspects of the descending inhibitory circuit. Here we cohesively present the formative preclinical and clinical studies evidencing sex differences in morphine analgesia and provide support for five major factors underlying sex differences in opioid modulation of pain: (1) sex differences in the neuroanatomical organization of the PAG–RVM pathway; (2) sexually dimorphic activation of the PAG by inflammatory pain and morphine; (3) gonadal hormone-related plasticity in opioid receptor expression in the PAG; (4) sex differences in opioid metabolism and the central effects of metabolites; and (5) the role of PAG glia and neuroimmune signaling. We further argue that the current literature clearly illustrates the necessity of sex-specific research on opioid and non-opioid modulation of pain, particularly in light of the current opioid crisis in America.
Clinical studies
Clinical studies that include sex as an independent variable are limited. This is unfortunate given the significantly higher prevalence of pain reports and disorders in women (see recent review by Sorge and Totsch [42]). Of the studies that include sex as a factor, the majority demonstrate decreased analgesic efficacy of opioids in women [8, 43,44,45,46,47]. Indeed, one clinical study reported that females required 30% more morphine to reach the same level of analgesia as males [46]. In contrast, other studies report that the analgesic efficacy of opioids was comparable between the sexes [48,49,50,51]. Sex differences in morphine consumption (i.e., patient-controlled analgesia) have also been reported; however, importantly, morphine consumption is not a reliable indicator of morphine analgesia as women consistently experience a greater number of negative side effects associated with acute opioid consumption, including nausea, dysphoria, headache, and constipation [50, 52,53,54]. Perspective on the topic is also limited by the reliance on self-report in clinical studies which is remarkably subjective, due in part to cultural and societal influences [55, 56], as well as individual differences in the pain experience [57, 58]. Preclinical behavioral models of persistent and/or severe pain provide an excellent alternative method to assess sex differences in morphine action.
Preclinical studies
Preclinical research on opioid modulation of acute or persistent pain in rodents has consistently demonstrated that morphine is more efficacious in males [26, 30, 59,60,61,62,63,64,65,66,67]. Sex differences in morphine action are not trivial; in both persistent inflammatory pain [26, 29, 61, 65, 68,69,70,71,72,73] and visceral pain [65, 74,75,76,77], the 50% effective dose (ED50) for females is approximately 2-fold higher than the ED50 for males. Indeed, in our recent studies using a rat model of persistent inflammatory pain, we report morphine ED50 values of 4.07 mg/kg in males versus 10.39 mg/kg in females [26]. Furthermore, morphine-induced hyperalgesia is also exacerbated in females [78, 79]. Sex differences in opioid analgesia are not limited to morphine; indeed, greater pain relief is observed in male rats for almost every opioid tested [80,81,82,83,84].
While the majority of preclinical data noted above indicate that female rats have an attenuated response to morphine compared to males, some behavioral studies report either no sex differences [85, 86] or effects in the opposite direction [87]. These discrepancies are thought to be due primarily to differences between rat and/or mouse strains, type and route of analgesic administered, the duration of pain (acute versus chronic), modality of pain examined (e.g., orofacial, visceral, inflammatory) [4], and estrous cycle status in females (discussed in a later section). A more thorough evaluation of the neuroanatomical pathways mediating opioid analgesia, specifically within the PAG and its projections to the RVM, have recently offered new evidence for an anatomical substrate contributing to sex differences in opioid analgesia [88].
Neural mechanisms underlying sex differences in analgesia
The PAG–RVM pathway
One of the first demonstrations for a role of the PAG in pain modulation was conducted by D.V. Reynolds in 1969, who, in the absence of anesthesia, performed exploratory laparotomy in rats while electrically stimulating the PAG [89]. Since then, anatomical and physiological studies conducted in a variety of species have shown that the midbrain PAG plays a modulatory role in a variety of behaviors including antinociception [24, 89,90,91,92], reproduction [93,94,95,96], fear and anxiety [96], aggression [98,99,100,101], and vocalization [102, 103]. The PAG projects heavily to the RVM, which in turn projects to the dorsal horn of the spinal cord (Fig. 1) comprising a primary neural pathway mediating the effects of opioids. Morphine binds to the mu opioid receptor (MOR), an inhibitory G protein-coupled receptor, to modulate pain [26, 29, 31]. MOR activation decreases voltage-gated calcium channel conductance, in part through low voltage-activated T-type channels [104], and increases presynaptic potassium conductance [105,106,107] to hyperpolarize the membrane and decrease the probability of presynaptic transmitter release.
The lateral and ventrolateral columns of the PAG contain a high density of MOR, which are localized directly on PAG–RVM output neurons (45%), as well as GABAergic neurons located presynaptic to PAG–RVM output neurons (50%) [108,109,110,111,112]. Two primary mechanisms have been proposed to account for mu opioid-induced activation of the PAG–RVM descending circuit. The morphine disinhibition hypothesis was proposed to account for the fact that morphine, which is inhibitory, paradoxically excites PAG–RVM output neurons [24, 113, 114]. The disinhibition hypothesis proposes that MOR + GABAergic neurons exert tonic inhibitory tone over PAG–RVM glutamatergic neurons; administration of morphine disinhibits this circuit, resulting in its activation and the inhibition of pain [106, 113, 115, 116]. Support for this hypothesis comes from in vitro studies in which MOR binding on PAG neurons reduces inhibitory postsynaptic potential frequency and decreases the probability of presynaptic GABA release [105, 106, 117]. In vivo, injection of GABA antagonists into the PAG partially mimics the effects of morphine [118] and potentiates morphine analgesia [119]. Last, selective knockdown of PAG α1G T-type channels, which are selectively expressed on intrinsic GABAergic neurons, significantly impairs morphine analgesia [119].
A second mechanism proposed to account for mu opioid-induced activation of the PAG–RVM descending circuit is a direct action of morphine on PAG–RVM output neurons. As mentioned above, MOR is also expressed on PAG–RVM output neurons [110], and opioid application to GABA-sensitive PAG–RVM neurons in a slice preparation has a predominantly inhibitory effect [120]. Both GABAergic [27] and glutamatergic [118] PAG–RVM output neurons have been identified in male rats and mice. In mice, Samineni et al. [121] reported no overlap in the distribution of glutamatergic and GABAergic neurons in the PAG, indicating two neurochemically distinct populations. Interestingly, chemogenetic activation of PAG glutamatergic neurons or inhibition of GABAergic neurons attenuates thermal pain [121]. Together, these studies indicate that opiates may act either directly on PAG–RVM neurons or indirectly via GABAergic interneurons to inhibit pain. Further adding to the complexity of morphine action in the PAG, MOR-GABAergic signaling is directly influenced by neuron–glia interactions, discussed later in this review.
Sex differences in the anatomy and physiology of the PAG–RVM pathway
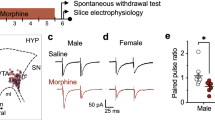
The PAG and its projections to the RVM and spinal cord are sexually dimorphic in both their anatomy and physiology. Quantitatively, females have approximately twice as many output neurons in the PAG–RVM pathway as their male counterparts; however, persistent inflammatory pain or systemic administration of morphine preferentially engages this circuit in males [59, 122] (Fig. 2a, b). Males have higher levels of MOR protein and binding within the PAG [26], likely contributing to the increased analgesic efficacy of morphine observed in males. In support, site-specific lesions of PAG MOR-containing neurons in rats results in a significant rightward shift in the morphine dose–response curve in males (ED50 4.07–12.55 mg/kg), making them ‘female-like’ in their response to morphine [26]. In contrast, lesions of PAG MOR-containing neurons in females had no effect on morphine ED50 (10.39–9.21 mg/kg). Together, these data indicate that anatomical and physiological differences in the PAG–RVM circuit, and in particular MOR expression, contribute to the sexually dimorphic actions of morphine. As microinjection of morphine into the RVM also results in greater antinociception in male rats in comparison to females [30], sex differences in opioidergic signaling in the RVM may also contribute to the dimorphic effects of systemic morphine.
Proposed model of factors contributing to sex differences in pain and morphine potency elicited by the PAG. Despite a greater number of PAG–RVM neurons (orange) in female rats, persistent inflammatory pain evoked by CFA injection into the rat hindpaw elicits greater activation of the PAG–RVM pathway in males compared to females (a). Similarly, systemic morphine at 4.5 mg/kg evokes greater activation of the PAG–RVM pathway in males compared to females (b). Repeated morphine administration leads to the development of tolerance in males, while no effect of morphine or development of tolerance was observed in females at 4.5 mg/kg (c). TLR4 activation of glial cells (blue) in the ventrolateral PAG of males opposes the acute effects of morphine and contributes to the development of tolerance (d)
Both pain and analgesia are modulated by emotional, motivational, and cognitive factors indicating higher-order cortical and subcortical forebrain modulation of PAG–RVM signaling. Anatomical studies in rats have demonstrated that in males, the PAG predominately receives afferents from cortical and sub-cortical sites implicated in pain and emotion, including the medial preoptic area (MPO), the central and medial nuclei of the amygdala (MeA, CeA), and the ventromedial and paraventricular hypothalamic nuclei (VMH, PVN) [123, 124]. These forebrain projections terminate with a high degree of topographical specificity within the PAG, preferentially terminating among PAG–RVM output neurons [125]. In contrast, our recent preliminary data in females suggest that MPO-PAG and CeA-PAG neurons are activated by inflammatory pain to a greater degree in female rats, while MeA-PAG neurons are more activated in male rats (unpublished data). These findings suggest that forebrain sites projecting to the PAG may also exert sexually dimorphic modulation of pain and analgesia.
Development of morphine tolerance in the PAG
Repeated administration of morphine, either systemically or directly into the ventrolateral PAG (vlPAG) results in the development of tolerance, defined as a state in which an organism no longer responds to a drug so that a higher dose is required to achieve comparable levels of analgesia [34,35,36,37,38,39]. Not surprisingly, repeated administration of systemic morphine induces tolerance to a greater degree in male versus female rats [122]. Specifically, in male rats, tolerance is accompanied by a two-fold rightward shift in the morphine dose response curve (increase in ED50 from 3.0 to 6.3 mg/kg). In contrast, a non-significant shift in morphine ED50 is observed in females (6.0 to 8.3 mg/kg). Further, the activation of PAG–RVM neurons is significantly attenuated following repeated morphine administration in males, but not females [122, 126] (Fig. 2c). This tolerance-induced reduction in PAG MOR signaling efficacy [107] is reversed when MOR coupling is enhanced via upregulated adenylate cyclase activity [127].
Chronic, but not acute, opioid administration also induces a robust neuroinflammatory response in the male rat PAG via the innate immune receptor toll-like receptor 4 (TLR4) [128, 129]. TLR4 is located on microglia, and to a lesser degree on astrocytes [130, 130]. Opioids, including morphine, bind to the glycoprotein myeloid differentiation factor-2 (MD-2) on TLR4 to initiate an inflammatory response through nuclear factor kappa B (NFκB) activation and p38 mitogen activated protein kinase (MAPK) phosphorylation [128, 132, 133]. Activation of the NFκB pathway results in the robust release of proinflammatory cytokines, including tumor necrosis factor (TNF), interleukin 1 beta (IL-1β), and interleukin 6 (IL-6). Our recent studies demonstrate that TLR4 activity within the vlPAG (Fig. 2d) directly opposes the acute effects of morphine and contribute to the development of tolerance [129, 134]. Specifically, we report that tolerance, induced by systemic morphine, decreases astrocytic glutamate transporter 1 and glutamate aspartate transporter (GLT-1 and GLAST, respectively), but not neuronal excitatory amino acid transporter 1 (EAACI) mRNA in the vlPAG, resulting in an increased neuro-excitatory environment. These changes in astrocytic glutamate transporter expression are dependent on vlPAG soluble TNF (solTNF) signaling as site-specific sequestration of solTNF via a dominant-negative virus or solTNF biologic reverses the decrease in GLT-1 and GLAST expression and significantly attenuates the development of tolerance [135].
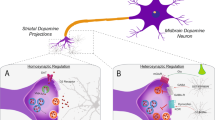
Together these studies suggest that morphine binds to neuronal MOR and glial TLR4 in the vlPAG, and that concurrent activity at these receptors modulates the analgesic efficacy of morphine via two opposing mechanisms: (1) opioid binding at MOR results in hyperpolarization of GABAergic neurons and induction of opioid analgesia [106, 115]; and (2) opioid binding at glial TLR4 leads to increased vlPAG solTNF signaling that simultaneously promotes neuroinflammation and disrupts the ability of astrocytes to scavenge excess glutamate, counteracting MOR-mediated hyperpolarization of GABAergic neurons and inducing tolerance [135] (Fig. 3). The presence of MOR on microglia remains somewhat controversial [136]; however, a recent study by Corder et al. [137] using multiple histological approaches and RNA-seq of non-cultured, acutely purified adult rat spinal microglia found no evidence of MOR expression in microglia [137].
Morphine binds to MOR on neurons and to TLR4 on microglia and astrocytes. While MOR binding hyperpolarizes GABAergic interneurons, TLR4 binding leads to the release of solTNF and other cytokines, which affect astrocytes by decreasing glutamate transporter proteins, and affect neurons by downregulating GABA receptors and upregulating AMPA receptors. Together, these inflammatory-induced changes increase excess glutamate and result in hyperexcitability of GABAergic interneurons, sustained GABA release, and inhibition of PAG–RVM projection neurons that dampen incoming pain signals
Although our studies clearly implicate a role for TLR4 signaling in the PAG in the development of opioid tolerance in rats, results to the contrary using TLR4 null or mutant mice have also been reported. Not surprising, TLR4 mutant mice display normal levels of antinociception following acute morphine administration; however, they also developed tolerance following repeated systemic administration [138, 139]. TLR4 null or mutant mice also displayed normal levels of opioid-induced hyperalgesia and naloxone-precipitated withdrawal following repeated morphine administration, both of which are thought to be mediated by TLR4 signaling. It is not clear why TLR4 null or mutant mice displayed tolerance and opioid-induced hyperalgesia. As stated above, opioids bind to the glycoprotein MD-2 located on TLR4 to initiate neuroinflammation and the release of TNF, and it is unknown if MD-2 signaling remains functionally intact in TLR4 null or mutant mice. In rats, although depletion of spinal microglia via the toxin saporin completely blocked morphine-induced hyperalgesia, it had no effect on tolerance [136]. Similar results were reported following intrathecal administration of the TLR4 antagonist (+)-naloxone, and together, suggest the possibility that opioid signaling at sites other than the spinal cord (e.g., PAG or primary afferent) may be more critical for the development and maintenance of morphine tolerance [137].
Effects of gonadal hormones on morphine analgesia
Studies in rodents indicate that sex differences in the organizational and activational effects of the gonadal hormones estradiol and testosterone influence morphine analgesia (Table 1). Male rats castrated at birth demonstrate decreased morphine potency in adulthood, while female rats masculinized at birth demonstrate greater morphine potency as adults [62, 66]. Similarly, morphine is reportedly less effective in gonadectomized adult males and more effective in ovariectomized adult females [66, 68, 73, 82, 140,141,142]; these effects are reversed with hormone replacement [75, 140, 143]. Moreover, the antinociceptive potency of morphine is reportedly greater during diestrus, when circulating estradiol levels are lowest [68, 70, 82, 142, 144]. In fact, it was recently reported that microinjection of morphine directly into the PAG produces less antinociception during estrus (high estradiol), and no sex difference in morphine potency was observed between diestrus females and males [29].
The PAG is a likely anatomical substrate whereby gonadal steroids influence pain and analgesia. Both androgen (AR) and estrogen receptors (ERα) have been localized in the PAG of the rat [94, 145], cat [146], golden hamster [147], guinea pig [148], and rhesus monkey [149, 150]. Male rats have a significantly greater number of AR immunoreactive neurons within the dorsomedial, lateral, and vlPAG compared to females, while PAG ERα expression is comparable between the sexes [151]. Further, approximately 30–37% of PAG–RVM output neurons in both male and female rats express AR and/or ERα, with the highest density of co-labeling observed in the lateral/ventrolateral region of PAG [151]. While the overall density of steroid receptors is similar between the sexes, fluctuating steroid levels in males and females can clearly influence this circuit. Approximately 27–50% of PAG–RVM neurons are MOR-positive [109]; given the greater density of MOR in the PAG of males than females [26], the interaction between morphine and sex hormones is likely greater in the PAG of male compared to female rats.
Several mechanisms have been proposed whereby gonadal steroids may modulate opioid-sensitive PAG–RVM output neurons, resulting in a dimorphic response to morphine. First, estradiol has been shown to uncouple the MOR from G protein-gated inwardly rectifying potassium channels [151], resulting in an attenuation of morphine-induced hyperpolarization. Second, estradiol has been shown to induce MOR internalization [152], thereby reducing available opioid binding sites on the cell membrane. Interestingly, ERα is required for estradiol-induced MOR internalization [153] supporting the hypothesis that colocalization of MOR and ERα in PAG–RVM output neurons provides a unique mechanism through which estrogens may differentially affect morphine potency in male and female rats.
Further contributions of glia
As discussed above, our lab as well as others [71, 133, 135, 155,156,157,158,159,160,161,162,163] have shown that morphine action at TLR4 initiates a neuroinflammatory response within the PAG that directly opposes the analgesic effects of morphine (although see [164]). These findings led us to test the hypothesis that the attenuated response to morphine observed in females is the result of increased microglia activation in the PAG. In these studies, male and female rats were administered morphine (or saline) and the density and phenotype of microglia (activated/reactive or non-activated/quiescent) were quantified for the vlPAG. Interestingly, we report that although there is no sex difference in the overall number or density of microglia in the vlPAG, the percentage of microglia that showed an activated phenotype (i.e., reactive) was significantly higher in females than males regardless of treatment [71]. In these studies, we also examined if the degree of microglia activation could predict an animal’s response to morphine. We observed a significant relationship between morphine potency and the percentage of reactive microglia in females (r = 0.68), but not males (r = 0.32). Although acute morphine treatment did not change microglia morphology in either sex, administration of the glial TLR4 agonist lipopolysaccharide (LPS) increased the percentage of activated microglia in the vlPAG of females to a greater degree than males. This LPS-induced increase in microglia activation in females was accompanied by significantly increased proinflammatory IL-1β transcription and decreased anti-inflammatory IL-10 transcription in the PAG. We further showed that priming microglia with LPS significantly attenuated morphine analgesia in both sexes, and completely abolished the antinociceptive response to morphine in a subset of females (33%). Similarly, inhibition of vlPAG microglia with the TLR4 antagonist (+)-naloxone significantly potentiated morphine analgesia in females (ED50 decreased from 7.9 to 3.16 mg/kg), but not males (ED50 shifted from 3.04 to 5.25 mg/kg), abolishing the sex difference in opioid response. Together, these data indicate that vlPAG microglia are innately different in males and females in terms of their morphological state (both basal and following immune challenge with LPS), and further implicate TLR4 in the attenuated response to morphine observed in females.
Future research directions
Development of designer and alternative analgesics
Morphine, as well as other opioids that are metabolized via glucuronidation, produce a physiological response within the PAG at both MOR and TLR4 to promote and oppose opioid analgesia, respectively. Two active metabolites are produced via glucuronidation: morphine-3-glucuronide (M3G) and morphine-6-glucuronide (M6G). M3G, which has a high affinity for TLR4 [133] and little to no affinity for MOR [132], induces robust microglia activation that is accompanied by cytokine release and the development of hyperalgesia [132, 165]. In contrast, M6G, which binds preferentially to MOR with little to no affinity for TLR4 [133], is the pro-analgesic metabolite of morphine [166]. Thus, M6G, and other opioids that do not activate immune cells, may produce greater analgesia and represent a favorable alternative to the commonly used immune-activating opioids.
We have recently reported that direct PAG administration of the MOR-selective metabolite M6G results in a greater analgesic response in females than morphine alone [72]. M6G analgesia was reversed with co-administration of the MOR selective antagonist (−)-naloxone, but not the TLR4 selective antagonist (+)-naloxone, indicating that this effect is MOR mediated. In contrast, intra-PAG administration of M3G significantly attenuated the analgesic effects of systemic morphine in males only, increasing the morphine ED50 two-fold (5.0 versus 10.3 mg/kg) and eliminating the previously observed sex difference. Together, these data implicate sex differences in morphine metabolism, and specifically the metabolite M3G, as a contributing factor in the attenuated response to morphine observed in females. More importantly, these data demonstrate that in the absence of TLR4 signaling, opioid analgesia is equally effective, if not more effective, in females as compared with males.
Historically, M6G has not been used for the treatment of clinical pain in humans, in part due to its low blood brain barrier permeability and tendency to accumulate in plasma in patients with impaired renal function [167, 168]. However, clinical trials of M6G demonstrate comparable analgesia to morphine at appropriate doses, while reducing the negative side effects typically associated with morphine, including nausea and sedation, in both men and women [169,170,171,172]. Future research is clearly necessary to address the relevance of treatment with M6G, as these studies may provide insight into improved treatment strategies for pain management in women.
Clinical implications
The National Institutes of Health (NIH) recently reported new requirements for the inclusion of female subjects in NIH-funded research, as appropriate for the scientific goals of the study (Public Health Service Act sec. 492B, 42 U.S.C. sec. 289a-2). Although increasing the number of research laboratories that analyze sex-based data is clearly necessary, it is important to note that utilizing female subjects presents additional challenges that researchers need to consider in experimental design. In 2006, the Sex, Gender, and Pain Special Interest Group of the International Association for the Study of Pain (IASP) reviewed what is known about sex differences in pain and analgesia and published a seminal consensus report on the best practice guidelines for pain research including sex as an independent variable [173]. These guidelines are an excellent reference and should be consulted when designing preclinical and clinical studies utilizing female subjects.
Despite growing literature reporting sex differences in pain and morphine analgesia, the overwhelming majority of preclinical studies of pain (approximately 79%) are still conducted exclusively in males [4]. At this point, we hope it is clear that sex differences in opioid modulation of pain exist and warrant additional, comprehensive investigation into the underlying mechanisms. Building on what is currently known regarding sex differences in pain and analgesia will likely identify additional targets for the development of novel pain therapeutics; only then will we be able to advance effective pain management in both women and men.
The work referenced in this review highlights several inherent differences in how the central nervous system of males and females responds to pain and opioids. Multiple lines of evidence implicate the PAG as a key anatomical substrate underlying the observed sex differences in opioid analgesia. Based on this, we argue that morphine may not be the drug of choice for pain management in women. As both preclinical and clinical research indicate that opioids are less effective in females, it is interesting that women are more likely to be prescribed opioids at higher doses and for longer periods of time than men [174,175,176]. Perhaps this is illustrative of the observed lower potency of opioids in women, and mirrors preclinical studies on lower opioid potency in rodents. Further, women may be especially at risk for developing opioid addiction and overdose, which are currently being underscored in our society as an opioid crisis. These sex differences and potential vulnerabilities must be considered in pain management regimens in women until novel, non-opioid therapeutics that are equivalently effective in men and women alike, are identified.
References
Martin PR. Headaches in health care: A behavioral approach. Sydney, Australia: Grune & Stratton; 1986.
Nahin RL. Estimates of pain prevalence and severity in adults: United States, 2012. J Pain. 2015;16:769–80.
Medicine Io. Relieving pain in America: A blueprint for transforming prevention, care, education, and research. Washington, DC: The National Academies Press; 2011.
Mogil JS. Sex differences in pain and pain inhibition: multiple explanations of a controversial phenomenon. Nat Rev Neurosci. 2012;13:859–66.
Ruau D, Liu LY, Clark JD, Angst MS, Butte AJ. Sex differences in reported pain across 11,000 patients captured in electronic medical records. J Pain. 2012;13:228–34.
Unruh AM. Gender variations in clinical pain experience. Pain. 1996;65:123–67.
Buse DC, Loder EW, Gorman JA, Stewart WF, Reed ML, Fanning KM, et al. Sex differences in the prevalence, symptoms, and associated features of migraine, probable migraine and other severe headache: results of the American Migraine Prevalence and Prevention (AMPP) Study. Headache. 2013;53:1278–99.
Fillingim RB, King CD, Ribeiro-Dasilva MC, Rahim-Williams B, Riley JL 3rd. Sex, gender, and pain: a review of recent clinical and experimental findings. J Pain. 2009;10:447–85.
Kennedy J, Roll JM, Schraudner T, Murphy S, McPherson S. Prevalence of persistent pain in the U.S. Adult population: new data from the 2010 national health interview survey. J Pain. 2014;15:979–84.
Brookoff D. Chronic pain: 1. A new disease? Hosp Pract (1995). 2000;35:45–52, 59.
Brookoff D. Chronic pain: 2. The case for opioids. Hosp Pract (1995). 2000;35:69–72, 75–66, 81–64.
Boudreau D, Von Korff M, Rutter CM, Saunders K, Ray GT, Sullivan MD, et al. Trends in long-term opioid therapy for chronic non-cancer pain. Pharmacoepidemiol Drug Saf. 2009;18:1166–75.
Roggeri D, Saramin C, Terrazzani G, Zusso M, Giusti P, Chinellato A. Resource consumption and costs of treating pain in patients affected by cancer in a district of northeast Italy. Pharmacol Res. 2007;56:329–34.
Trescot AM, Glaser SE, Hansen H, Benyamin R, Patel S, Manchikanti L. Effectiveness of opioids in the treatment of chronic non-cancer pain. Pain Physician. 2008;11:S181–200.
Al-Hasani R, Bruchas MR. Molecular mechanisms of opioid receptor-dependent signaling and behavior. Anesthesiology. 2011;115:1363–81.
Sarzi-Puttini P, Vellucci R, Zuccaro SM, Cherubino P, Labianca R, Fornasari D. The appropriate treatment of chronic pain. Clin Drug Investig. 2012;32:21–33.
Labianca R, Sarzi-Puttini P, Zuccaro SM, Cherubino P, Vellucci R, Fornasari D. Adverse effects associated with non-opioid and opioid treatment in patients with chronic pain. Clin Drug Investig. 2012;32:53–63.
Pasternak GW, Pan YX. Mu opioids and their receptors: evolution of a concept. Pharmacol Rev. 2013;65:1257–317.
Angst MS, Clark JD. Opioid-induced hyperalgesia: a qualitative systematic review. Anesthesiology. 2006;104:570–87.
Bray RM, Pemberton MR, Lane ME, Hourani LL, Mattiko MJ, Babeu LA. Substance use and mental health trends among U.S. military active duty personnel: key findings from the 2008 DoD Health Behavior Survey. Mil Med. 2010;175:390–9.
Basbaum AI, Clanton CH, Fields HL. Three bulbospinal pathways from the rostral medulla of the cat: an autoradiographic study of pain modulating systems. J Comp Neurol. 1978;178:209–24.
Basbaum AI, Fields HL. Endogenous pain control mechanisms: review and hypothesis. Ann Neurol. 1978;4:451–62.
Basbaum AI, Fields HL. Endogenous pain control systems: brainstem spinal pathways and endorphin circuitry. Annu Rev Neurosci. 1984;7:309–38.
Behbehani MM, Fields HL. Evidence that an excitatory connection between the periaqueductal gray and nucleus raphe magnus mediates stimulation produced analgesia. Brain Res. 1979;170:85–93.
Behbehani MM, Pomeroy SL. Effect of morphine injected in periadueductal gray on the activity of single units in nucleus raphe magnus of the rat. Brain Res. 1978;149:266–9.
Loyd DR, Wang X, Murphy AZ. Sex differences in micro-opioid receptor expression in the rat midbrain periaqueductal gray are essential for eliciting sex differences in morphine analgesia. J Neurosci. 2008;28:14007–17.
Morgan MM, Whittier KL, Hegarty DM, Aicher SA. Periaqueductal gray neurons project to spinally projecting GABAergic neurons in the rostral ventromedial medulla. Pain. 2008;140:376–86.
Thomas A, Miller A, Roughan J, Malik A, Haylor K, Sandersen C, et al. Efficacy of intrathecal morphine in a model of surgical pain in rats. PLoS ONE. 2016;11:e0163909.
Bernal SA, Morgan MM, Craft RM. PAG mu opioid receptor activation underlies sex differences in morphine antinociception. Behav Brain Res. 2007;177:126–33.
Boyer JS, Morgan MM, Craft RM. Microinjection of morphine into the rostral ventromedial medulla produces greater antinociception in male compared to female rats. Brain Res. 1998;796:315–8.
Jensen TS, Yaksh TL. Comparison of antinociceptive action of morphine in the periaqueductal gray, medial and paramedial medulla in rat. Brain Res. 1986;363:99–113.
Kumar A, Liu NJ, Madia PA, Gintzler AR. Contribution of endogenous spinal endomorphin 2 to intrathecal opioid antinociception in rats is agonist dependent and sexually dimorphic. J Pain. 2015;16:1200–10.
Zambotti F, Zonta N, Parenti M, Tommasi R, Vicentini L, Conci F, et al. Periaqueductal gray matter involvement in the muscimol-induced decrease of morphine antinociception. Naunyn Schmiede Arch Pharmacol. 1982;318:368–9.
Lane DA, Patel PA, Morgan MM. Evidence for an intrinsic mechanism of antinociceptive tolerance within the ventrolateral periaqueductal gray of rats. Neuroscience. 2005;135:227–34.
Morgan MM, Fossum EN, Levine CS, Ingram SL. Antinociceptive tolerance revealed by cumulative intracranial microinjections of morphine into the periaqueductal gray in the rat. Pharmacol Biochem Behav. 2006;85:214–9.
Siuciak JA, Advokat C. Tolerance to morphine microinjections in the periaqueductal gray (PAG) induces tolerance to systemic, but not intrathecal morphine. Brain Res. 1987;424:311–9.
Tortorici V, Morgan MM, Vanegas H. Tolerance to repeated microinjection of morphine into the periaqueductal gray is associated with changes in the behavior of off- and on-cells in the rostral ventromedial medulla of rats. Pain. 2001;89:237–44.
Tortorici V, Robbins CS, Morgan MM. Tolerance to the antinociceptive effect of morphine microinjections into the ventral but not lateral-dorsal periaqueductal gray of the rat. Behav Neurosci. 1999;113:833–9.
Jacquet YF, Lajtha A. The periaqueductal gray: site of morphine analgesia and tolerance as shown by 2-way cross tolerance between systemic and intracerebral injections. Brain Res. 1976;103:501–13.
Pereira EA, Lu G, Wang S, Schweder PM, Hyam JA, Stein JF, et al. Ventral periaqueductal grey stimulation alters heart rate variability in humans with chronic pain. Exp Neurol. 2010;223:574–81.
Dampney RA, Furlong TM, Horiuchi J, Iigaya K. Role of dorsolateral periaqueductal grey in the coordinated regulation of cardiovascular and respiratory function. Auton Neurosci. 2013;175:17–25.
Sorge RE, Totsch SK. Sex differences in pain. J Neurosci Res. 2017;95:1271–81.
Miller PL, Ernst AA. Sex differences in analgesia: a randomized trial of mu versus kappa opioid agonists. South Med J. 2004;97:35–41.
Mogil JS, Bailey AL. Sex and gender differences in pain and analgesia. Prog Brain Res. 2010;186:141–57.
Berkley KJ. Sex differences in pain. Behav Brain Sci. 1997;20:371–80. discussion 435–513.
Cepeda MS, Carr DB. Women experience more pain and require more morphine than men to achieve a similar degree of analgesia. Anesth Analg. 2003;97:1464–8.
Aubrun F, Salvi N, Coriat P, Riou B. Sex- and age-related differences in morphine requirements for postoperative pain relief. Anesthesiology. 2005;103:156–60.
Sarton E, Olofsen E, Romberg R, den Hartigh J, Kest B, Nieuwenhuijs D, et al. Sex differences in morphine analgesia: an experimental study in healthy volunteers. Anesthesiology. 2000;93:1245–54. discussion 1246A
Bijur PE, Esses D, Birnbaum A, Chang AK, Schechter C, Gallagher EJ. Response to morphine in male and female patients: analgesia and adverse events. Clin J Pain. 2008;24:192–8.
Fillingim RB, Ness TJ, Glover TL, Campbell CM, Hastie BA, Price DD, et al. Morphine responses and experimental pain: sex differences in side effects and cardiovascular responses but not analgesia. J Pain. 2005;6:116–24.
Glasson JC, Sawyer WT, Lindley CM, Ginsberg B. Patient-specific factors affecting patient-controlled analgesia dosing. J Pain Palliat Care Pharmacother. 2002;16:5–21.
Myles PS, Hunt JO, Moloney JT. Postoperative ‘minor’ complications. Comparison between men and women. Anaesthesia. 1997;52:300–6.
Cepeda MS, Farrar JT, Baumgarten M, Boston R, Carr DB, Strom BL. Side effects of opioids during short-term administration: effect of age, gender, and race. Clin Pharmacol Ther. 2003;74:102–12.
Comer SD, Cooper ZD, Kowalczyk WJ, Sullivan MA, Evans SM, Bisaga AM, et al. Evaluation of potential sex differences in the subjective and analgesic effects of morphine in normal, healthy volunteers. Psychopharmacology (Berl). 2010;208:45–55.
Pool GJ, Schwegler AF, Theodore BR, Fuchs PN. Role of gender norms and group identification on hypothetical and experimental pain tolerance. Pain. 2007;129:122–9.
Edwards R, Eccleston C, Keogh E. Observer influences on pain: an experimental series examining same-sex and opposite-sex friends, strangers, and romantic partners. Pain. 2017;158:846–55.
Belfer I, Segall SK, Lariviere WR, Smith SB, Dai F, Slade GD, et al. Pain modality- and sex-specific effects of COMT genetic functional variants. Pain. 2013;154:1368–76.
Gatchel RJ, Peng YB, Peters ML, Fuchs PN, Turk DC. The biopsychosocial approach to chronic pain: scientific advances and future directions. Psychol Bull. 2007;133:581–624.
Loyd DR, Murphy AZ. Sex differences in the anatomical and functional organization of the periaqueductal gray-rostral ventromedial medullary pathway in the rat: a potential circuit mediating the sexually dimorphic actions of morphine. J Comp Neurol. 2006;496:723–38.
Posillico CK, Terasaki LS, Bilbo SD, Schwarz JM. Examination of sex and minocycline treatment on acute morphine-induced analgesia and inflammatory gene expression along the pain pathway in Sprague-Dawley rats. Biol Sex Differ. 2015;6:33.
Wang X, Traub RJ, Murphy AZ. Persistent pain model reveals sex difference in morphine potency. Am J Physiol Regul Integr Comp Physiol. 2006;291:R300–6.
Cicero TJ, Nock B, O’Connor L, Meyer ER. Role of steroids in sex differences in morphine-induced analgesia: activational and organizational effects. J Pharmacol Exp Ther. 2002;300:695–701.
Craft RM, Stratmann JA, Bartok RE, Walpole TI, King SJ. Sex differences in development of morphine tolerance and dependence in the rat. Psychopharmacology (Berl). 1999;143:1–7.
Holtman JR Jr., Jing X, Wala EP. Sex-related differences in the enhancement of morphine antinociception by NMDA receptor antagonists in rats. Pharmacol Biochem Behav. 2003;76:285–93.
Ji Y, Murphy AZ, Traub RJ. Sex differences in morphine-induced analgesia of visceral pain are supraspinally and peripherally mediated. Am J Physiol Regul Integr Comp Physiol. 2006;291:R307–14.
Kepler KL, Kest B, Kiefel JM, Cooper ML, Bodnar RJ. Roles of gender, gonadectomy and estrous phase in the analgesic effects of intracerebroventricular morphine in rats. Pharmacol Biochem Behav. 1989;34:119–27.
Krzanowska EK, Ogawa S, Pfaff DW, Bodnar RJ. Reversal of sex differences in morphine analgesia elicited from the ventrolateral periaqueductal gray in rats by neonatal hormone manipulations. Brain Res. 2002;929:1–9.
Stoffel EC, Ulibarri CM, Craft RM. Gonadal steroid hormone modulation of nociception, morphine antinociception and reproductive indices in male and female rats. Pain. 2003;103:285–302.
Craft RM. Sex differences in opioid analgesia: “from mouse to man”. Clin J Pain. 2003;19:175–86.
Craft RM, Mogil JS, Aloisi AM. Sex differences in pain and analgesia: the role of gonadal hormones. Eur J Pain. 2004;8:397–411.
Doyle HH, Eidson LN, Sinkiewicz DM, Murphy AZ. Sex differences in microglia activity within the periaqueductal gray of the rat: a potential mechanism driving the dimorphic effects of morphine. J Neurosci. 2017;37:3202–14.
Doyle HH, Murphy AZ. Sex-dependent influences of morphine and its metabolites on pain sensitivity in the rat. Physiol Behav. 2018;187:32–41.
Krzanowska EK, Bodnar RJ. Morphine antinociception elicited from the ventrolateral periaqueductal gray is sensitive to sex and gonadectomy differences in rats. Brain Res. 1999;821:224–30.
Murphy AZ, Suckow SK, Johns M, Traub RJ. Sex differences in the activation of the spinoparabrachial circuit by visceral pain. Physiol Behav. 2009;97:205–12.
Ji Y, Murphy AZ, Traub RJ. Estrogen modulation of morphine analgesia of visceral pain in female rats is supraspinally and peripherally mediated. J Pain. 2007;8:494–502.
Ji Y, Tang B, Traub RJ. The visceromotor response to colorectal distention fluctuates with the estrous cycle in rats. Neuroscience. 2008;154:1562–7.
Larauche M, Mulak A, Kim YS, Labus J, Million M, Tache Y. Visceral analgesia induced by acute and repeated water avoidance stress in rats: sex difference in opioid involvement. Neurogastroenterol Motil. 2012;24:1031–547.
Holtman JR Jr, Wala EP. Characterization of morphine-induced hyperalgesia in male and female rats. Pain. 2005;114:62–70.
Juni A, Klein G, Kowalczyk B, Ragnauth A, Kest B. Sex differences in hyperalgesia during morphine infusion: effect of gonadectomy and estrogen treatment. Neuropharmacology. 2008;54:1264–70.
Barrett AC, Smith ES, Picker MJ. Sex-related differences in mechanical nociception and antinociception produced by mu- and kappa-opioid receptor agonists in rats. Eur J Pharmacol. 2002;452:163–73.
Peckham EM, Traynor JR. Comparison of the antinociceptive response to morphine and morphine-like compounds in male and female Sprague-Dawley rats. J Pharmacol Exp Ther. 2006;316:1195–201.
Stoffel EC, Ulibarri CM, Folk JE, Rice KC, Craft RM. Gonadal hormone modulation of mu, kappa, and delta opioid antinociception in male and female rats. J Pain. 2005;6:261–74.
Terner JM, Lomas LM, Smith ES, Barrett AC, Picker MJ. Pharmacogenetic analysis of sex differences in opioid antinociception in rats. Pain. 2003;106:381–91.
Bai X, Zhang X, Li Y, Lu L, Li B, He X. Sex differences in peripheral mu-opioid receptor mediated analgesia in rat orofacial persistent pain model. PLoS ONE. 2015;10:e0122924.
Islam AK, Beczkowska IW, Bodnar RJ. Interactions among aging, gender, and gonadectomy effects upon naloxone hypophagia in rats. Physiol Behav. 1993;54:981–92.
Kepler KL, Standifer KM, Paul D, Kest B, Pasternak GW, Bodnar RJ. Gender effects and central opioid analgesia. Pain. 1991;45:87–94.
Ali BH, Sharif SI, Elkadi A. Sex differences and the effect of gonadectomy on morphine-induced antinociception and dependence in rats and mice. Clin Exp Pharmacol Physiol. 1995;22:342–4.
Loyd DR, Murphy AZ. The role of the periaqueductal gray in the modulation of pain in males and females: are the anatomy and physiology really that different? Neural Plast. 2009;2009:462879.
Reynolds DV. Surgery in the rat during electrical analgesia induced by focal brain stimulation. Science. 1969;164:444–5.
Behbehani MM. Functional characteristics of the midbrain periaqueductal gray. Prog Neurobiol. 1995;46:575–605.
Budai D, Harasawa I, Fields HL. Midbrain periaqueductal gray (PAG) inhibits nociceptive inputs to sacral dorsal horn nociceptive neurons through alpha2-adrenergic receptors. J Neurophysiol. 1998;80:2244–54.
Heinricher MM, Cheng ZF, Fields HL. Evidence for two classes of nociceptive modulating neurons in the periaqueductal gray. J Neurosci. 1987;7:271–8.
McCarthy MM, Pfaff DW, Schwartz-Giblin S. Midbrain central gray GABAA receptor activation enhances, and blockade reduces, sexual behavior in the female rat. Exp Brain Res. 1991;86:108–16.
Murphy AZ, Hoffman GE. Distribution of gonadal steroid receptor-containing neurons in the preoptic-periaqueductal gray-brainstem pathway: a potential circuit for the initiation of male sexual behavior. J Comp Neurol. 2001;438:191–12.
Ogawa S, Kow L-M, McCarthy MM, Pfaff DW, Schwartz-Giblin S. Midbrain PAG control of female reproductive behavior: in vitro electrophysiological characterization of actions of lordosis-relevant substances. In: Depaulis A, Bandler R, editors. The midbrain periaqueductal gray matter. New York, NY: Plenum Press; 1991. p. 211–38.
Daniels D, Miselis RR, Flanagan-Cato LM. Central neuronal circuit innervating the lordosis-producing muscles defined by transneuronal transport of pseudorabies virus. J Neurosci. 1999;19:2823–33.
Kim JJ, Rison RA, Fanselow MS. Effects of amygdala, hippocampus, and periaqueductal gray lesions on short- and long-term contextual fear. Behav Neurosci. 1993;107:1093–8.
Scordalakes EM, Rissman EF. Aggression and arginine vasopressin immunoreactivity regulation by androgen receptor and estrogen receptor alpha. Genes Brain Behav. 2004;3:20–26.
Depaulis A, Keay KA, Bandler R. Longitudinal neuronal organization of defensive reactions in the midbrain periaqueductal gray region of the rat. Exp Brain Res. 1992;90:307–18.
Bandler R, Carrive P. Integrated defence reaction elicited by excitatory amino acid microinjection in the midbrain periaqueductal grey region of the unrestrained cat. Brain Res. 1988;439:95–106.
Bandler R, Depaulis A, Vergnes M. Identification of midbrain neurones mediating defensive behaviour in the rat by microinjections of excitatory amino acids. Behav Brain Res. 1985;15:107–19.
Zhang SP, Davis PJ, Bandler R, Carrive P. Brain stem integration of vocalization: role of the midbrain periaqueductal gray. J Neurophysiol. 1994;72:1337–56.
Davis PJ, Zhang SP, Bandler R. Pulmonary and upper airway afferent influences on the motor pattern of vocalization evoked by excitation of the midbrain periaqueductal gray of the cat. Brain Res. 1993;607:61–80.
Dogrul A, Yesilyurt O, Isimer A, Guzeldemir ME. L-type and T-type calcium channel blockade potentiate the analgesic effects of morphine and selective mu opioid agonist, but not to selective delta and kappa agonist at the level of the spinal cord in mice. Pain. 2001;93:61–8.
Vaughan CW, Christie MJ. Presynaptic inhibitory action of opioids on synaptic transmission in the rat periaqueductal grey in vitro. J Physiol. 1997;498:463–72.
Vaughan CW, Ingram SL, Connor MA, Christie MJ. How opioids inhibit GABA-mediated neurotransmission. Nature. 1997;390:611–4.
Bagley EE, Chieng BC, Christie MJ, Connor M. Opioid tolerance in periaqueductal gray neurons isolated from mice chronically treated with morphine. Br J Pharmacol. 2005;146:68–76.
Behbehani MM, Jiang MR, Chandler SD, Ennis M. The effect of GABA and its antagonists on midbrain periaqueductal gray neurons in the rat. Pain. 1990;40:195–204.
Wang H, Wessendorf MW. Mu- and delta-opioid receptor mRNAs are expressed in periaqueductal gray neurons projecting to the rostral ventromedial medulla. Neuroscience. 2002;109:619–34.
Commons KG, Aicher SA, Kow LM, Pfaff DW. Presynaptic and postsynaptic relations of mu-opioid receptors to gamma-aminobutyric acid-immunoreactive and medullary-projecting periaqueductal gray neurons. J Comp Neurol. 2000;419:532–42.
Commons KG, van Bockstaele EJ, Pfaff DW. Frequent colocalization of mu opioid and NMDA-type glutamate receptors at postsynaptic sites in periaqueductal gray neurons. J Comp Neurol. 1999;408:549–59.
Gutstein HB, Mansour A, Watson SJ, Akil H, Fields HL. Mu and kappa opioid receptors in periaqueductal gray and rostral ventromedial medulla. Neuroreport. 1998;9:1777–81.
Sandkuhler J, Willmann E, Fu QG. Blockade of GABAA receptors in the midbrain periaqueductal gray abolishes nociceptive spinal dorsal horn neuronal activity. Eur J Pharmacol. 1989;160:163–6.
Yeung JC, Yaksh TL, Rudy TA. Concurrent mapping of brain sites for sensitivity to the direct application of morphine and focal electrical stimulation in the production of antinociception in the rat. Pain. 1977;4:23–40.
Lau BK, Vaughan CW. Descending modulation of pain: the GABA disinhibition hypothesis of analgesia. Curr Opin Neurobiol. 2014;29:159–64.
Heinricher MM, Tavares I, Leith JL, Lumb BM. Descending control of nociception: Specificity, recruitment and plasticity. Brain Res Rev. 2009;60:214–25.
Vaughan CW, Bagley EE, Drew GM, Schuller A, Pintar JE, Hack SP, et al. Cellular actions of opioids on periaqueductal grey neurons from C57B16/J mice and mutant mice lacking MOR-1. Br J Pharmacol. 2003;139:362–7.
Moreau JL, Fields HL. Evidence for GABA involvement in midbrain control of medullary neurons that modulate nociceptive transmission. Brain Res. 1986;397:37–46.
Park C, Kim JH, Yoon BE, Choi EJ, Lee CJ, Shin HS. T-type channels control the opioidergic descending analgesia at the low threshold-spiking GABAergic neurons in the periaqueductal gray. Proc Natl Acad Sci USA. 2010;107:14857–62.
Osborne PB, Vaughan CW, Wilson HI, Christie MJ. Opioid inhibition of rat periaqueductal grey neurones with identified projections to rostral ventromedial medulla in vitro. J Physiol. 1996;490:383–9.
Samineni VK, Grajales-Reyes JG, Copits BA, O’Brien DE, Trigg SL, Gomez AM, et al. Divergent modulation of nociception by glutamatergic and gabaergic neuronal subpopulations in the periaqueductal gray. eNeuro. 2017;4:0129–16.
Loyd DR, Morgan MM, Murphy AZ. Morphine preferentially activates the periaqueductal gray-rostral ventromedial medullary pathway in the male rat: a potential mechanism for sex differences in antinociception. Neuroscience. 2007;147:456–68.
Shipley M, Ennis M, Rizvi TA. Topographical specificity of forebrain inputs to the midbrain periaqueductal gray: evidence for discrete longitudinally organized input columns. In: Depaulis A, Bandler R, editors. The midbrain periaqueductal gray matter. New York, NY: Plenum Press; 1991. p. 417–48.
Beitz AJ. The organization of afferent projections to the midbrain periaqueductal gray of the rat. Neuroscience. 1982;7:133–59.
Loyd DR, Murphy AZ. Forbrain modulation of the periaqueductal gray and its modulation by pain. In: Gebhart GF, Schmidt RF, editors. Encyclopedia of Pain. Vol. LXXVI. Berlin, Heidelberg: Springer-Verlag; 2013.
Loyd DR, Morgan MM, Murphy AZ. Sexually dimorphic activation of the periaqueductal gray-rostral ventromedial medullary circuit during the development of tolerance to morphine in the rat. Eur J Neurosci. 2008;27:1517–24.
Hack SP, Vaughan CW, Christie MJ. Modulation of GABA release during morphine withdrawal in midbrain neurons in vitro. Neuropharmacology. 2003;45:575–84.
Wang X, Loram LC, Ramos K, de Jesus AJ, Thomas J, Cheng K, et al. Morphine activates neuroinflammation in a manner parallel to endotoxin. Proc Natl Acad Sci USA. 2012;109:6325–30.
Eidson LN, Murphy AZ. Blockade of Toll-like receptor 4 attenuates morphine tolerance and facilitates the pain relieving properties of morphine. J Neurosci. 2013a;33:15952–63.
Lehnardt S, Massillon L, Follett P, Jensen FE, Ratan R, Rosenberg PA, et al. Activation of innate immunity in the CNS triggers neurodegeneration through a Toll-like receptor 4-dependent pathway. Proc Natl Acad Sci USA. 2003;100:8514–9.
Jou I, Lee JH, Park SY, Yoon HJ, Joe EH, Park EJ. Gangliosides trigger inflammatory responses via TLR4 in brain glia. Am J Pathol. 2006;168:1619–30.
Lewis SS, Hutchinson MR, Rezvani N, Loram LC, Zhang Y, Maier SF, et al. Evidence that intrathecal morphine-3-glucuronide may cause pain enhancement via toll-like receptor 4/MD-2 and interleukin-1beta. Neuroscience. 2010;165:569–83.
Hutchinson MR, Zhang Y, Shridhar M, Evans JH, Buchanan MM, Zhao TX, et al. Evidence that opioids may have toll-like receptor 4 and MD-2 effects. Brain Behav Immun. 2010;24:83–95.
Eidson LN, Murphy AZ. Persistent peripheral inflammation attenuates morphine-induced periaqueductal gray glial cell activation and analgesic tolerance in the male rat. J Pain. 2013b;14:393–404.
Eidson LN, Inoue K, Young LJ, Tansey MG, Murphy AZ. Toll-like receptor 4 mediates morphine-induced neuroinflammation and tolerance via soluble tumor necrosis factor signaling. Neuropsychopharmacology. 2017;42:661–70.
Ferrini F, Trang T, Mattioli TA, Laffray S, Del’Guidice T, Lorenzo LE, et al. Morphine hyperalgesia gated through microglia-mediated disruption of neuronal Cl(-) homeostasis. Nat Neurosci. 2013;16:183–92.
Corder G, Tawfik VL, Wang D, Sypek EI, Low SA, Dickinson JR, et al. Loss of mu opioid receptor signaling in nociceptors, but not microglia, abrogates morphine tolerance without disrupting analgesia. Nat Med. 2017;23:164–73.
Mattioli TA, Leduc-Pessah H, Skelhorne-Gross G, Nicol CJ, Milne B, Trang T, et al. Toll-like receptor 4 mutant and null mice retain morphine-induced tolerance, hyperalgesia, and physical dependence. PLoS ONE. 2014;9:e97361.
Fukagawa H, Koyama T, Kakuyama M, Fukuda K. Microglial activation involved in morphine tolerance is not mediated by toll-like receptor 4. J Anesth. 2013;27:93–7.
Ratka A, Simpkins JW. Effects of estradiol and progesterone on the sensitivity to pain and on morphine-induced antinociception in female rats. Horm Behav. 1991;25:217–28.
Terner JM, Barrett AC, Grossell E, Picker MJ. Influence of gonadectomy on the antinociceptive effects of opioids in male and female rats. Psychopharmacology (Berl). 2002;163:183–93.
Terner JM, Lomas LM, Picker MJ. Influence of estrous cycle and gonadal hormone depletion on nociception and opioid antinociception in female rats of four strains. J Pain. 2005;6:372–83.
Kiefel JM, Bodnar RJ. Roles of gender and gonadectomy in pilocarpine and clonidine analgesia in rats. Pharmacol Biochem Behav. 1992;41:153–8.
Okamoto K, Tashiro A, Hirata H, Bereiter DA. Differential modulation of TMJ neurons in superficial laminae of trigeminal subnucleus caudalis/upper cervical cord junction region of male and cycling female rats by morphine. Pain. 2005;114:203–1.
Murphy AZ, Hoffman GE. Distribution of androgen and estrogen receptor containing neurons in the male rat periaqueductal gray. Horm Behav. 1999;36:98–108.
VanderHorst VG, Schasfoort FC, Meijer E, van Leeuwen FW, Holstege G. Estrogen receptor-alpha-immunoreactive neurons in the periaqueductal gray of the adult ovariectomized female cat. Neurosci Lett. 1998;240:13–6.
Boers J, Gerrits PO, Meijer E, Holstege G. Estrogen receptor-alpha-immunoreactive neurons in the mesencephalon, pons and medulla oblongata of the female golden hamster. Neurosci Lett. 1999;267:17–20.
Turcotte JC, Blaustein JD. Immunocytochemical localization of midbrain estrogen receptor- and progestin receptor-containing cells in female guinea pigs. J Comp Neurol. 1993;328:76–87.
Vanderhorst VG, Terasawa E, Ralston HJ 3rd. Estrogen receptor-alpha immunoreactive neurons in the ventrolateral periaqueductal gray receive monosynaptic input from the lumbosacral cord in the rhesus monkey. J Comp Neurol. 2002;443:27–42.
VanderHorst VG, Terasawa E, Ralston HJ 3rd. Projections from estrogen receptor-alpha immunoreactive neurons in the periaqueductal gray to the lateral medulla oblongata in the rhesus monkey. Neuroscience. 2004;125:243–53.
Loyd DR, Murphy AZ. Androgen and estrogen (alpha) receptor localization on periaqueductal gray neurons projecting to the rostral ventromedial medulla in the male and female rat. J Chem Neuroanat. 2008;36:216–26.
Kelly MJ, Qiu J, Ronnekleiv OK. Estrogen modulation of G-protein-coupled receptor activation of potassium channels in the central nervous system. Ann N Y Acad Sci. 2003;1007:6–16.
Eckersell CB, Popper P, Micevych PE. Estrogen-induced alteration of mu-opioid receptor immunoreactivity in the medial preoptic nucleus and medial amygdala. J Neurosci. 1998;18:3967–76.
Micevych PE, Rissman EF, Gustafsson JA, Sinchak K. Estrogen receptor-alpha is required for estrogen-induced mu-opioid receptor internalization. J Neurosci Res. 2003;71:802–10.
Sun J, Liu S, Mata M, Fink DJ, Hao S. Transgene-mediated expression of tumor necrosis factor soluble receptor attenuates morphine tolerance in rats. Gene Ther. 2012;19:101–8.
Watkins LR, Hutchinson MR, Johnston IN, Maier SF. Glia: novel counter-regulators of opioid analgesia. Trends Neurosci. 2005;28:661–9.
Watkins LR, Hutchinson MR, Rice KC, Maier SF. The “toll” of opioid-induced glial activation: improving the clinical efficacy of opioids by targeting glia. Trends Pharmacol Sci. 2009;30:581–91.
Watkins LR, Milligan ED, Maier SF. Spinal cord glia: new players in pain. Pain. 2001;93:201–5.
Hao S, Liu S, Zheng X, Zheng W, Ouyang H, Mata M, et al. The role of TNFalpha in the periaqueductal gray during naloxone-precipitated morphine withdrawal in rats. Neuropsychopharmacology. 2011;36:664–76.
Hutchinson MR, Bland ST, Johnson KW, Rice KC, Maier SF, Watkins LR. Opioid-induced glial activation: mechanisms of activation and implications for opioid analgesia, dependence, and reward. ScientificWorldJournal. 2007;7:98–111.
Hutchinson MR, Coats BD, Lewis SS, Zhang Y, Sprunger DB, Rezvani N, et al. Proinflammatory cytokines oppose opioid-induced acute and chronic analgesia. Brain Behav Immun. 2008;22:1178–89.
Hutchinson MR, Northcutt AL, Chao LW, Kearney JJ, Zhang Y, Berkelhammer DL, et al. Minocycline suppresses morphine-induced respiratory depression, suppresses morphine-induced reward, and enhances systemic morphine-induced analgesia. Brain Behav Immun. 2008;22:1248–56.
Hutchinson MR, Zhang Y, Brown K, Coats BD, Shridhar M, Sholar PW, et al. Non-stereoselective reversal of neuropathic pain by naloxone and naltrexone: involvement of toll-like receptor 4 (TLR4). Eur J Neurosci. 2008;28:20–9.
Sorge RE, LaCroix-Fralish ML, Tuttle AH, Sotocinal SG, Austin JS, Ritchie J, et al. Spinal cord Toll-like receptor 4 mediates inflammatory and neuropathic hypersensitivity in male but not female mice. J Neurosci. 2011;31:15450–4.
Grace PM, Strand KA, Galer EL, Urban DJ, Wang X, Baratta MV, et al. Morphine paradoxically prolongs neuropathic pain in rats by amplifying spinal NLRP3 inflammasome activation. Proc Natl Acad Sci USA. 2016;113:E3441–50.
Carrigan KA, Lysle DT. Morphine-6 beta-glucuronide induces potent immunomodulation. Int Immunopharmacol. 2001;1:821–31.
Lotsch J, Geisslinger G. Morphine-6-glucuronide: an analgesic of the future? Clin Pharmacokinet. 2001;40:485–99.
Kilpatrick GJ, Smith TW. Morphine-6-glucuronide: actions and mechanisms. Med Res Rev. 2005;25:521–44.
Romberg R, Olofsen E, Sarton E, den Hartigh J, Taschner PE, Dahan A. Pharmacokinetic-pharmacodynamic modeling of morphine-6-glucuronide-induced analgesia in healthy volunteers: absence of sex differences. Anesthesiology. 2004;100:120–33.
Cann C, Curran J, Milner T, Ho B. Unwanted effects of morphine-6-glucoronide and morphine. Anaesthesia. 2002;57:1200–3.
Dahan A, van Dorp E, Smith T, Yassen A. Morphine-6-glucuronide (M6G) for postoperative pain relief. Eur J Pain. 2008;12:403–11.
Hanna MH, Elliott KM, Fung M. Randomized, double-blind study of the analgesic efficacy of morphine-6-glucuronide versus morphine sulfate for postoperative pain in major surgery. Anesthesiology. 2005;102:815–21.
Greenspan JD, Craft RM, LeResche L, Arendt-Nielsen L, Berkley KJ, Fillingim RB, et al. Studying sex and gender differences in pain and analgesia: a consensus report. Pain. 2007;132:S26–45.
Manubay J, Davidson J, Vosburg S, Jones J, Comer S, Sullivan M. Sex differences among opioid-abusing patients with chronic pain in a clinical trial. J Addict Med. 2015;9:46–52.
Campbell CI, Weisner C, Leresche L, Ray GT, Saunders K, Sullivan MD, et al. Age and gender trends in long-term opioid analgesic use for noncancer pain. Am J Public Health. 2010;100:2541–7.
Frenk SM, Porter KS, Paulozzi LJ. Prescription opioid analgesic use among adults: United States, 1999-2012. NCHS Data Brief. 2015;1–8.
Pain Management Task Force: providing a standardized DoD and VHA vision and approach to pain management to optimize the care for warriors and their families. Department of the Army, Office of the Surgeon General, USA; 2010. purl.fdlp.gov. http://www.dvcipm.org/site/assets/files/1070/pain-task-force-finalreport-may-2010.pdf
Baamonde AI, Hidalgo A, Andrés-Trelles F. Sex-related differences in the effects of morphine and stress on visceral pain. Neuropharmacology. 1989;28:967–70.
Cicero TJ, Nock B, Meyer ER. Gender-related differences in the antinociceptive properties of morphine. J Pharmacol Exp Ther. 1996;279:767–73.
Barrett AC, Cook CD, Terner JM, Craft RM, Picker MJ. Importance of sex and relative efficacy at the mu opioid receptor in the development of tolerance and crosstolerance to the antinociceptive effects of opioids. Psychopharmacology (Berl). 2001;158:154–64.
Cook CD, Nickerson MD. Nociceptive sensitivity and opioid antinociception and antihyperalgesia in Freund's adjuvant-induced arthritic male and female rats. J Pharmacol Exp Ther. 2005;313:449--59.
Acknowledgements
This work was supported by NIH grants DA16272 and DA041529 awarded to AZM.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Averitt, D.L., Eidson, L.N., Doyle, H.H. et al. Neuronal and glial factors contributing to sex differences in opioid modulation of pain. Neuropsychopharmacol 44, 155–165 (2019). https://doi.org/10.1038/s41386-018-0127-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41386-018-0127-4
This article is cited by
-
Distinct neurochemical influences on fMRI response polarity in the striatum
Nature Communications (2024)
-
Identification of sex-specific genetic associations in response to opioid analgesics in a White, non-Hispanic cohort from Southeast Minnesota
The Pharmacogenomics Journal (2022)
-
Novelty-induced locomotor behavior predicts heroin addiction vulnerability in male, but not female, rats
Psychopharmacology (2022)
-
Cohort-based analysis of paternal opioid use in relation to offspring’s BMI and plasma lipid profile
Scientific Reports (2021)
-
Sex and Estrous Cycle Differences in Analgesia and Brain Oxycodone Levels
Molecular Neurobiology (2021)