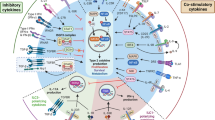
Abstract
Group 2 innate lymphoid cells (ILC2s) represent the major player during hyperresponsive airway inflammation. Peroxisome proliferator-activated receptor-γ (PPARγ) was highly expressed on ILC2 and its potential role in asthma has been suggested. However, the detailed mechanism underlying the effects of PPARγ on ILC2-induced airway inflammation remains to be fully understood. Here we identified PPARγ as a positive regulator of lung ILC2. Expression of PPARγ on ILC2 was dramatically induced upon interleukin-33 (IL-33) challenge. Deficiency of PPARγ in hematopoietic system in mice (PPARγfl/fl Vav1Cre) significantly impaired the function of ILC2 in lung, which led to apparent alleviation of airway inflammation in response to IL-33 or Papain challenge, when compared with those in PPARγfl/fl littermates control. Mechanistic studies identified IL-33 receptor ST2 as a transcriptional target of PPARγ. Overexpression of ST2 rescued the functional defects of ILC2 lacking PPARγ. Collectively, these results demonstrated PPARγ as an important regulator of ILC2 during allergic airway inflammation, which sheds new lights on the importance of PPARγ in asthma.
Similar content being viewed by others
Introduction
The incidence of hyperresponsive allergic airway inflammation, or asthma, has increased over recent years. It affects over 300 million of people worldwide.1 Over-activation of type 2 helper T cells (Th2) has long been considered to be the dominant mechanism in the pathogenesis of asthma. In the last decade, however, group 2 innate lymphoid cells (ILC2s) were identified as a major player in the initiation of airway inflammation.2 Upon allergen exposure, airway epithelium secrete alarmins, including interleukin (IL)-33, IL-25, and thymic stromal lymphopoietin (TSLP), thereby causing the activation of resident ILC2s in lung.2,3 Activated ILC2s produce large amounts of type 2 effector cytokines and cause eosinophilic infiltration, goblet cell proliferation, and mucus production, which ultimately lead to airway inflammation.4 In addition to the crucial role in the initiation of airway inflammation, the important role of ILC2s in the facilitation of Th2 activation has also been suggested.5,6 Therefore, ILC2s could initiate and promote the progression of asthma.
The development of ILC2s happens in the bone marrow: they differentiate from common lymphoid progenitor (CLP), followed by distinct stages of progenitors including α4β7+ lymphoid progenitor (α-LP), common helper-like ILC progenitor (ChILP), and immature ILC2.7,8 After that, ILC2s migrate and reside in the peripheral tissues.9,10 Upon stimulations from the tissue microenvironment, such as danger signals, tissue injury or pathogen infections, ILC2s are activated by secreted cytokines, neuropeptides, or hormones.11 Activated ILC2s exert a variety of functions in a context or tissue-dependent manner, including but not limited to tissue homeostasis, allergic inflammation, defense against pathogens, as well as energy metabolism.12,13,14 Multiple transcriptional factors and cell–cell interaction molecules have been identified to be important regulators of ILC2,8,15 among which GATA3 was considered to be the master regulator.16,17
Peroxisome proliferator-activated receptor-γ (PPARγ) is a ligand-activated transcription regulator that belongs to the nuclear hormone receptor superfamily. PPARγ is ubiquitously expressed in most cell types. Through sensing a wide range of exogenous or endogenous signals from the environment, such as lipid mediators or inflammatory stimuli, PPARγ is activated and regulates the transcription of downstream targets.18,19 The importance of PPARγ in adipocyte differentiation and lipogenesis has been well-documented.20 Its emerging role in the immune system and inflammation is just being recognized.21 It was reported that PPARγ expression was upregulated during allergen ovalbumin (OVA)-induced airway inflammation.22 Furthermore, asthma patients presented higher level of PPARγ expression in the airways when compared with healthy controls.23 Retrospective studies have also revealed a correlation between PPARγ single nucleotide polymorphisms (SNPs) and the risk of asthma.24,25 Clinical trials in both short-term and long-term studies showed a modest effect of PPARγ agonists on the alleviation of asthma symptoms in smokers.26 Additionally, administration of PPARγ agonists exerted strong beneficial effects on murine airway inflammation models.27,28 These observations suggested a potential role of PPARγ in the pathogenesis of asthma.
The mechanisms underlying the effects of PPARγ on airway inflammation remain to be fully elucidated. Both anti-inflammatory and pro-inflammatory effects have been reported, which may be cell type dependent. PPARγ expression in airway epithelial cells was increased after allergen exposure in sensitized mice.29 PPARγ agonists reduced cigarette smoke-induced mucin production by epithelial cells,29 thus significantly suppressing mucus secretion and collagen deposition.22 A lack of PPARγ expression in the early stage of hematopoiesis impaired alveolar macrophage (AM) development and caused severe symptoms of influenza virus infection in mice.30 On the contrary, dendritic cells treated with PPARγ agonist aggravated airway inflammation after transfer into asthmatic mice,31 and specific depletion of PPARγ in dendritic cells significantly relieved airway inflammation.32 Additionally, PPARγ is a positive regulator of Th2 cells during airway inflammation. Th2 cells express higher level of PPARγ than other T cell subsets, and type 2 cytokines production in CD4+ T cells strongly depends on PPARγ. Mice lacking PPARγ expression in T cell fail to develop Th2 cell responses in airway inflammation.32,33 These observations collectively indicate that the complicated role of PPARγ in lung is highly cell-type dependent.
The potential role of PPARγ in ILC2 has recently been indicated. PPARγ was found to be highly expressed in ILC2 when compared with other ILC subsets, based on single cell sequencing analysis.34 PPARγ facilitated lipid uptake and transient lipid storage in lipid droplets, which was required for the fuel of pathogenic ILC2 responses during airway inflammation.35 PD-1 has been revealed to be essential for ILC2 function,36 while PPARγ regulated PD-1 expression on ILC2.37 The detailed mechanism of PPARγ-mediated ILC2 activation, however, remains to be fully explored. In this study, it was found that PPARγ deficiency in the hematopoietic system dramatically impaired ILC2 responses to IL-33 or papain challenge, thereby relieving airway inflammation. Further studies showed that IL-33 receptor ST2 mediated the effect of PPARγ on ILC2. This study identifies PPARγ as an important regulator of ILC2 in lung, which sheds new light on the role of PPARγ in asthma.
Results
PPARγ is dispensable for the development of ILC2
To investigate the potential role of PPARγ in ILC2, we first evaluated the expression of PPARγ in ILC2 and other types of immune cells. Consistent with previous report,38 PPARγ was highly expressed in ILC2(CD45+Lin−CD90.2+CD25+) both at mRNA and protein levels when compared with those in other ILC subsets and adaptive lymphocytes (Fig. 1a, b). Abundant expression of PPARγ in macrophages was observed as expected39 (Fig. 1a, b). Challenge with IL-33, the most potent driver of ILC2 activation,3,40 significantly induced the expression of PPARγ and other effector genes in ILC2, including Il5, Il13, and Arg1 (Fig. 1c). The induction of PPARγ by IL-33 was further evidenced by flow cytometry (Fig. 1d). Similar observations were noted in human ILC2(CD45+Lin−CD127+CRTH2+CD161+), including high expression of PPARγ in ILC2 and its upregulation by IL-33 (Fig. 1e, f). The gating strategies of mice and human ILC2 are shown in Supplementary Fig. S1.7,41 These observations indicate the potential importance of PPARγ in ILC2 function.
a The mRNA expression of PPARγ on macrophage, NK cell, ILC subsets, as well as T and B lymphocytes. b Representative flow cytometric analysis of PPARγ expression on immune cells in a. c Lung ILC2s from WT mice were cultured in the presence of IL-2, IL-7 with or without IL-33 for 3 days, the mRNA expression of Il5, Il13, Pparg, and Arg1 were analyzed. d Lung cells from WT mice were cultured in the presence of IL-2, IL-7 with or without IL-33 for 3 days, the expression of PPARγ on ILC2 was evaluated by flow cytometry. e Flow analysis of PPARγ expression on human PBMC-derived ILC subsets. f Human PBMCs were cultured in the presence of IL-2 and IL-7 with or without IL-33 for 3 days, the PPARγ expression was evaluated by flow cytometry. Data are representative of two independent experiments. Error bars show mean ± SEM; **P < 0.01; ***P < 0.001 by unpaired Student’s t test.
We next asked whether PPARγ regulates the homeostasis of ILC2 under steady-state condition. Flow cytometric analysis showed that the expression of PPARγ in the progenitors of ILC2, including CLP, αLP, and ChILP, was considerably lower when compared with that in immature ILC2 from bone marrow (Supplementary Fig. S2a, b). Next, PPARγ was specifically deleted in the hematopoietic system by cross-breeding the Vav1Cre strain with PPARγfl/fl mice (termed PPARγfl/fl Vav1Cre thereafter). Flow cytometric analysis showed that the frequencies of distinct ILC2 progenitors did not differ between PPARγfl/fl Vav1Cre mice and PPARγfl/fl controls (Supplementary Fig. S2c), thereby indicating that the development of ILC2 was not affected by PPARγ. Furthermore, the numbers of ILC2 in the peripheral tissues, including lung, visceral adipose tissue (VAT), and lamina propria from the large intestine (LI), were comparable between PPARγfl/fl Vav1Cre and PPARγfl/fl mice (Supplementary Fig. S2d). Other ILC subsets, including NK cell in the spleen, ILC1 in the mesenteric lymph node (mLN) and large intestine (Supplementary Fig. S2e), and ILC3 in mLN and large intestine (Supplementary Fig. S2f, g), were not apparently affected by PPARγ deficiency. These observations indicate that PPARγ is dispensable for the development of ILC2 and other ILC subsets.
PPARγ enhances ILC2 function both in vitro and in vivo
To study the role of PPARγ in the biological function of ILC2, lung ILC2s were sorted and cultured in the presence of IL-2, IL-7, and IL-33 for 3 days in vitro. The amounts of IL-5 and IL-13 in the supernatants were determined by ELISA. Results showed that ILC2 from PPARγfl/fl Vav1Cre mice produced remarkably lower level of effector cytokines when compared with PPARγfl/fl ILC2 (Fig. 2a), which were further confirmed by the proportions of IL-5+IL-13+ILC2 (Fig. 2b). In line with these observations, PPARγ agonist rosiglitazone enhanced the cytokines production and cell proliferation of ILC2, whereas PPARγ antagonist GW9662 displayed opposite effects (Fig. 2c, d). Similar results were obtained for human ILC2 (Fig. 2e). PPARγ deficiency did not affect the apoptosis of ILC2 under steady and IL-33 stimuli situation (Fig. 2f). These observations indicate that PPARγ is a positive regulator of ILC2.
a Lung ILC2 from PPARγfl/fl and PPARγfl/fl Vav1Cre mice were cultured in the presence of IL-2, IL-7, and IL-33 for 3 days, IL-5 and IL-13 amount in supernatant were determined by ELISA. b Flow cytometric analysis of IL-5+IL-13+ ILC2 of a. c Lung ILC2 from WT mice were cultured in the presence of IL-2, IL-7, and IL-33 for 3 days and treated with rosiglitazone (10 μM) or GW9662 (10 μM), DMSO was used as control. The amount of IL-5 and IL-13 in supernatant were determined by ELISA. d Ki67+ lung ILC2 was analyzed by flow cytometry. e Human PBMC-derived ILC2 were cultured in the presence of IL-2, IL-7, and IL-33 for 3 days and treated with rosiglitazone (10 μM) or GW9662 (10 μM), DMSO was used as control, IL-5 and IL-13 amount in supernatant were determined by ELISA. f Flow analysis of Annexin V+ lung ILC2 levels from PPARγfl/fl and PPARγfl/fl Vav1Cre after PBS or IL-33 i.n. challenge. Data are representative of two independent experiments. Error bars show mean ± SEM; *P < 0.05; **P < 0.01; *** P < 0.001 by unpaired Student’s t test.
We next explored whether PPARγ affects the function of ILC2 by evaluation of their responses to IL-33 challenge in vivo. PPARγfl/fl and PPARγfl/fl Vav1Cre mice were treated with IL-33 intranasally for 3 consecutive days (Fig. 3a). As expected, the numbers of lung ILC2 were dramatically increased after intranasal administration of IL-33 in both PPARγfl/fl Vav1Cre and PPARγfl/fl mice (Fig. 3b), whereas the induction fold was significantly reduced in PPARγfl/fl Vav1Cre mice when compared with that in PPARγfl/fl littermates (Fig. 3b). Production of the effector cytokines IL-5 and IL-13 by lung ILC2, as well as proliferation of ILC2, were clearly diminished in PPARγfl/fl Vav1Cre mice (Fig. 3c, d). Furthermore, the amounts of IL-5 and IL-13, as well as eosinophilic infiltration, in bronchoalveolar lavage fluid (BALF) were apparently reduced in PPARγfl/fl Vav1Cre mice when compared with those in PPARγfl/fl littermates (Fig. 3e, f). The attenuation of lung inflammation in PPARγfl/fl Vav1Cre mice was further evidenced by H&E histological staining (Fig. 3g). These results suggested that PPARγ deletion impairs ILC2 responses to IL-33 in the lung.
a PPARγfl/fl and PPARγfl/fl Vav1Cre mice were intranasally treated with IL-33 (500 ng/mouse/day) or PBS for 3 consecutive days, mice were sacrificed 24 h after last challenge. b Flow cytometric analysis of lung ILC2 pregated on CD45+Lin− from PPARγfl/fl and PPARγfl/fl Vav1Cre mice. c, d Frequencies of IL-5+IL-13+ ILC2 c and Ki67+ ILC2 d in lung. e The amount of IL-5 and IL-13 in BALF was examined by ELISA. f Eosinophils (CD45+CD11c−Siglec-F+) levels in BALF were analyzed by flow cytometry. g H&E staining of lung tissues (bars, 100 µm). Data are representative of two independent experiments (n = 4–6 for PBS groups, n = 6 for IL-33 groups). Error bars show mean ± SEM; **P < 0.01; ***P < 0.001 by unpaired Student’s t test.
For further confirmation, adoptive transfer of ILC2 was performed. Equal numbers of lung ILC2 from PPARγfl/fl and PPARγfl/fl Vav1Cre mice were adoptively transferred into immune-deficient NCG mice, followed by intranasal administration of IL-33 for 3 consecutive days (Fig. 4a). Results showed that the numbers of lung ILC2 in the recipients were significantly increased after IL-33 administration when compared with that in PBS control group (Fig. 4b), whereas the fold induction in recipients of PPARγfl/fl Vav1Cre ILC2s was significantly lower than that in PPARγfl/fl control (Fig. 4b). Consequently, the total number of CD45+ cells, the number of infiltrated eosinophils in BALF, and the amounts of IL-5 and IL-13 in BALF, were consistently lower in recipients of PPARγfl/fl Vav1Cre ILC2 (Fig. 4c–e). The attenuation of lung inflammation was further evidenced by H&E staining (Fig. 4f). Collectively, these observations support that PPARγ deficiency intrinsically impairs ILC2 function.
a PPARγfl/fl or PPARγfl/fl Vav1Cre mice-derived lung ILC2 was sorted and transferred into NCG mice, respectively, followed by IL-33 or PBS i.n. challenge for 3 consecutive days, mice were sacrificed 24 h after last challenge. b The number of ILC2 in lung of recipient mice. c The number of total CD45+ cells in BALF. d The frequencies and number of eosinophils in BALF determined by flow cytometry. e The amount of IL-5 and IL-13 in BALF was examined by ELISA. f H&E staining of lung tissues (bars, 100 µm). Data are representative of two independent experiments (n = 4–6 for PBS groups, n = 6 for IL-33 groups). Error bars show mean ± SEM; **P < 0.01; ***P < 0.001 by unpaired Student’s t test.
In addition to IL-33, IL-25 is another strong inducer of ILC2s. ILC2s induced by IL-25 are termed inflammatory ILC2s (iILC2s).42 PPARγfl/fl and PPARγfl/fl Vav1Cre mice were intraperitoneally (i.p.) injected with recombinant IL-25 for 3 days, the level of inflammatory ILC2 (Lin−ST2−KLRG1hi) in lung was significantly induced in both PPARγfl/fl Vav1Cre and control mice, whereas there was no differences between them (Supplementary Fig. S3a). The production of effector cytokines IL-4 and IL-13 by iILC2s also failed to display any noticeable differences between PPARγfl/fl Vav1Cre and PPARγfl/fl mice (Supplementary Fig. S3b). These observations indicate that deletion of PPARγ may not affect IL-25-induced iILC2s.
Although PPARγ did not affect the production of other ILC subsets, we further investigated whether PPARγ deletion affects the functions of ILC1 and ILC3 in a Citrobacter rodentium infection-induced murine colitis model.43,44 PPARγfl/fl and PPARγfl/fl Vav1Cre mice were orally gavaged with 2 × 109 colony-forming units (CFUs) of C. rodentium and sacrificed on day 6. The results revealed comparable colitis symptoms between PPARγfl/fl and PPARγfl/fl Vav1Cre mice, as indicated by similar weight loss and shortened colon length (Supplementary Fig. S4a, b). The production of interferon (IFN)-γ by ILC1, production of IL-17, IL-22, and IFN-γ by ILC3 in colon, displayed no differences between PPARγfl/fl and PPARγfl/fl Vav1Cre mice (Supplementary Fig. S4c, d). These observations suggest that deletion of PPARγ did not affect the function of other ILC subsets.
PPARγ aggravates ILC2-mediated lung inflammation
Considering the importance of ILC2 in the pathogenesis of airway inflammation,45 we next evaluated the effect of PPARγ deficiency on ILC2-induced lung inflammation. Intranasal instillation of papain for 5 consecutive days was performed. The numbers of infiltrated eosinophils, as well as the amounts of type 2 cytokines in BALF, were clearly diminished in PPARγfl/fl Vav1Cre mice as compared with PPARγfl/fl control upon papain challenge (Fig. 5a, b). The alleviation of lung inflammation in PPARγfl/fl Vav1Cre mice was further supported by H&E staining (Fig. 5c). As expected, the frequencies and absolute numbers of lung ILC2 in PPARγfl/fl Vav1Cre mice were significantly lower than those in PPARγfl/fl mice (Fig. 5d). The cell proliferation and cytokine production of lung ILC2 were consistently decreased in PPARγfl/fl Vav1Cre mice (Fig. 5e, f). As further confirmation, Alternaria alternata, a clinically relevant allergen, was used to induce lung inflammation. In line with the observations from papain model, the tissue inflammation in lung (Supplementary Fig. S5a, b, c) and the responses of ILC2 in lung (Supplementary Fig. S5d, e, f) were dramatically reduced in PPARγfl/fl Vav1Cre mice. These observations suggested that PPARγ aggravates ILC2-driven lung inflammation.
a–f PPARγfl/fl and PPARγfl/fl Vav1Cre mice were administered with papain intranasally for 5 consecutive days, mice were sacrificed 24 h later after last challenge. a The frequencies and number of eosinophils in BALF determined by flow cytometry. b The amount of IL-5 and IL-13 in BALF. c H&E staining of lung tissues (bars, 100 µm). d The frequencies and number of lung ILC2. e and f Frequencies of Ki67+ ILC2(e) and IL-5+IL-13+ ILC2(f) in lung. g–k PPARγfl/fl and PPARγfl/fl Vav1Cre mice were administrated with anti-CD4 antibody to deplete CD4 T cell, followed by papain challenge intranasally. g The frequencies and number of eosinophils in BALF. h The amount of IL-5 and IL-13 in BALF. i H&E staining of lung tissues (bars, 100 µm). j The number of lung ILC2. k The frequencies of IL-5+IL-13+ lung ILC2. Data are representative of two independent experiments (n = 4–6 for PBS groups, n = 6 for papain groups). Error bars show mean ± SEM; **P < 0.01; ***P < 0.001 by unpaired Student’s t test.
PPARγ is essential for the function of Th2 cells,32,33 and there is mutual regulation between Th2 and ILC2.6,46,47 To determine whether the effect of PPARγ on ILC2 was dependent or independent of CD4 T cells, PPARγfl/fl and PPARγfl/fl Vav1Cre mice were treated with anti-CD4 antibody to deplete CD4+ T cells48 and followed by intranasal instillation of papain for 5 consecutive days (Supplementary Fig. S5g). Results showed that PPARγfl/fl Vav1Cre mice consistently exhibited lower levels of eosinophils in BALF (Fig. 5g), reduced amounts of IL-5 and IL-13 in BALF (Fig. 5h), as well as attenuation of lung inflammation (Fig. 5i) upon depletion of CD4+ T cells. The numbers of ILC2 in lung and their secretion of IL-5 and IL-13 in PPARγfl/fl Vav1Cre mice were reduced as expected (Fig. 5j, k). These results indicated that the regulation of ILC2 by PPARγ was independent of CD4 T cells.
ST2 mediates the effects of PPARγ on ILC2
We next explored the mechanisms underlying the effects of PPARγ on ILC2. The level of GATA3, the master regulator of ILC2, was not affected by the presence or absence of PPARγ (Fig. 6a). However, the expression of IL-33 receptor ST2 was significantly downregulated in ILC2 upon PPARγ deletion (Fig. 6b). In addition, RT-PCR analysis confirmed the downregulation of ST2 at the transcriptional level (Fig. 6c). Furthermore, lung ILC2 from wild type mice were sorted and cultured with IL-2, IL-7, and IL-33 in the presence of PPARγ agonist rosiglitazone or antagonist GW9662 for 3 days. Results showed that the expression of ST2 was significantly upregulated by rosiglitazone, whereas it was decreased by GW9662 when compared with DMSO control (Fig. 6d).
a and b Flow cytometric analysis of GATA3 a and ST2 b expression in lung ILC2 from PPARγfl/fl and PPARγfl/fl Vav1Cre mice. c The mRNA expression of Gata3, Il1rl1, Il5, and Il13 in lung ILC2 from PPARγfl/fl and PPARγfl/fl Vav1Cre mice. d Lung ILC2 from WT mice were cultured in the presence of IL-2, IL-7, and IL-33 for 3 days and treated with rosiglitazone (10 μM) or GW9662 (10 μM), DMSO was used as control. MFI of ST2 were measured in lung ILC2. e Three potential PPARγ-binding sites in il1rl1 promotor region. f ChIP assay of PPARγ binding on the Il1rl1 promotor. A region of aP2 promoter with known PPARg-binding site was chosen as positive control (aP2-PPRE), a region in Il1rl1 promoter, where PPARg is not expected to bound was included as negative control (Il1rl1 non). g Lung ILC2 from PPARγfl/fl and PPARγfl/fl Vav1Cre mice were infected with retrovirus overexpression of ST2 or vector control in the presence of IL-2, IL-7, and IL-33 for 3 days. The amount of IL-5 and IL-13 in supernatants were measured by ELISA. Data are representative of two independent experiments (n = 6). Error bars show mean ± SEM; n.s., not significant; *P < 0.05; **P < 0.01; ***P < 0.001 by unpaired Student’s t test a–f or one-way ANOVA with Bonferroni post-test g.
Promoter analysis revealed several potential binding sites of PPARγ in the regulatory region of il1rl1 that encodes ST2 (Fig. 6e). Further ChIP assay showed that PPARγ protein could bind with the locus of site 3 on the il1rl1 promoter, aP2 promoter region with known PPARγ-binding site was used as a positive control, while a region in il1rl1 promoter without predicted PPARγ-binding site (il1rl1 non) was used as a negative control49,50 (Fig. 6f). These results identified il1rl1 as a downstream transcriptional target of PPARγ in ILC2. Next, ST2 was overexpressed in PPARγfl/fl Vav1Cre ILC2 by retroviral infection, the mRNA expression of ST2 in PPARg-deficient ILC2 was dramatically upregulated to wild type level after retroviral infection (Supplementary Fig. S6a, b). Importantly, ST2 overexpression almost completely rescued the defective production of IL-5 and IL-13 in PPARγfl/fl Vav1Cre ILC2 (Fig. 6g), suggesting that ST2 mediated the effect of PPARγ on ILC2 function.
Discussion
The importance of PPARγ in airway inflammation has been appreciated, although conflicting results have been reported from different groups. Clinical trials of asthma treatment by PPARγ agonists showed minor or even negligible effects.51,52,53 These reports indicate the complicated role of PPARγ in lung. Here, we reported that PPARγ is an important regulator of ILC2 via its downstream target ST2. Deficiency of PPARγ in hematopoietic system impaired ILC2 response in lung, thus alleviating ILC2-induced airway inflammation.
In addition to its crucial role in lipid metabolism, the importance of PPARγ in the regulation of immunity and tissue inflammation has been well documented.21 PPARγ may function as a bridge to link metabolism and immunity. Karagiannis et al.35 recently demonstrated that IL-33 promotes FA uptake via induction of PPARγ, which provides fuel for the proliferation of pathogenic ILC2 responses. In our study, we found that PPARγ upregulate IL-33 receptor ST2 expression on ILC2. It is therefore possible that there exists a positive feedback loop between PPARγ and IL-33-ST2 signaling in the regulation of ILC2 activation. Whereas there is no evidence that PPARγ regulates FA uptake via ST2. Another earlier research54 by the same author from Immunity 2020 reported that FA uptake and metabolism are essential for intestinal ILC2 function and ILC2-mediated resistance to helminth infection, in which they showed that pparg as well as other genes regulate FA usage in small intestine (SI) Lin–Thy1.2+KLRG1+ ILC2. As we know, Lin–Thy1.2+KLRG1+ ILC2 in SI under helminth infection was defined as iILC2 that lack ST2 expression.42 These reports indicate that PPARγ controls FA uptake of ILC2 in the absence of ST2 in iILC2. Furthermore, PPARγ regulates FA metabolism in multiple organs, while most of them do not express ST2,55 indicated that ST2 is not necessary for PPARγ-mediated FA uptake. Based on these literatures, whether there is cross-talk between FA uptake and ST2 induction in the regulation of ILC2 by PPARγ deserves to be further investigated.
The effects of PPARγ on airway inflammation were reported by different groups,30,31,32,33 although the observations were not consistent with each other. The possible explanations underlying these contraries may be caused by different animal models or different ways to modulate the expression or activity of PPARγ. PPARγ is expressed in distinct cell types. Administration of PPARγ agonist or antagonists to animals may display different effects which may be dependent on cell type or tissue, utilization of conditional knock-out of PPARγ in specific cell types is therefore helpful to address its complicated roles. In this study, conditional knock-out of PPARγ in the hematopoietic system was conducted to minimize its effect on non-hematopoietic cells. In order to exclude the potential effects of T cells, B cells, NK cells, and myeloid cells, immunodeficient NCG mice were used. Adoptive transfer of ILC2 from PPARγfl/flVav1Cre mice displayed lower capability to induce lung inflammation in recipient mice. Antibody depletion of CD4 T cells was also conducted to further exclude the potential effect of T lymphocytes, since PPARγ was reported to regulate Th2 cells.32,33 The in vitro ILC2 culture system further indicate the direct effect of PPARγ on ILC2. These observations collectively support that the regulation of ILC2 by PPARγ is cell intrinsic and independent of other cell types.
PPARγ is a master regulator in adipose tissue by regulating adipogenesis. ILC2 in fat tissue play an important role in lipogenesis. Min-Woo et al. first reported that activated ILC2 promotes the proliferation of bipotential adipocyte precursors and enhances their commitment to beige fat lineage, which was dependent on IL-33.56 Meanwhile, Jonathan et al. reported ILC2 in white adipose tissue could promote beiging of adipose and limit the development of obesity by production of enkephalin peptides.12 Whether the deficiency of PPARγ affects the function of ILC2 in fat tissue deserves further investigation.
In conclusion, this study demonstrated PPARγ as an important regulator of ILC2 during allergic inflammation. Downregulation of ST2 on the surface of ILC2 may explain the defective ILC2 responses upon PPARγ deletion. This study indicates the complicated role of PPARγ in lung homeostasis.
Methods
Mice
PPARγfl/fl mice (B6.129-Ppargtm2Rev/J, 004584) were kindly provided by Dr. Shengzhong Duan from the Shanghai Ninth People’s Hospital, College of Stomatology, Shanghai Jiao Tong University School of Medicine. Vav1Cre mice (B6.Cg-Commd10Tg(Vav1-icre)A2Kio/J, 008610) were purchased from The Jackson Laboratory. NCG mice (NOD-Prkdcem26Cd52Il2rgem26Cd22/Nju) were purchased from Nanjing Biomedical Research Institute of Nanjing University (Nanjing, China). C57BL/6 mice were purchased from Guangdong Medical Laboratory Animal Center (Guangzhou, China). All mice were used at the age of 6–8 weeks. All animal experiments were approved by the Institutional Animal Care and Use Committee of Tianjin Medical University and Sun Yat-sen University.
Murine airway inflammation models
For IL-33-induced model,57 mice were intranasally treated with recombinant mouse IL-33 (500 ng/mouse/day; BioLegend) or PBS for 3 consecutive days and sacrificed 24 h later after the final treatment. For papain-induced type 2 airway inflammation,58 20 μg papain (in 40 μl PBS/mouse/day, sigma) or PBS was intranasally administrated to mice for 5 consecutive days, BALF and lung samples were analyzed 24 h after last challenge. For Alternaria alternata-induced lung inflammation,57 mice were intranasally treated with Alternaria alternata (100 μg in 40 μl PBS/mouse/day, Greerlabs) for 4 consecutive days.
Flow cytometric analysis and sorting
Single cell suspension was prepared from lung or other tissues. About 2 × 106 cells were incubated with anti-CD16/CD32 before staining with fluorochrome-conjugated antibodies. Dead cells were excluded using cell viability dye (The live/dead fixable far-red dead cell stain kit, Invitrogen). For staining of transcriptional factor, cells were fixed and permeabilized (Foxp3/Transcription Factor Staining Buffer Set, eBioscience), stained with surface markers before incubation with fluorochrome-conjugated antibody against transcriptional factor. For analysis of PPARγ expression, cells were fixed and permeabilized followed by staining with rabbit anti-PPARγ western blot antibody, then labeled with fluorochrome-conjugated goat anti-rabbit IgG secondary antibody. For measuring intracellular cytokine expression, cells were stimulated with 50 ng/ml PMA (Sigma-Aldrich), 1 µg/ml ionomycin (Sigma-Aldrich), and 1 µg/ml brefeldin A in complete RPMI-1640 for 4 h. Cells were labeled with antibodies to surface markers, fixed and permeabilized using an intracellular fixation and permeability kit (eBioscience), then stained with antibodies against cytokines. LSRFortessa flow cytometer (BD Bioscience) was used for samples acquiring, and data were analyzed with Flowjo V10.4. To sort mouse ILC2, cells were depleted of T, B, NK, myeloid, and erythroid lineages by labeling with biotin-conjugated anti-CD3e, anti-CD4, anti-CD5, anti-CD8a, anti-TCRβ, anti-TCRγδ, anti-NK1.1, anti-CD45R/B220, anti-CD11b, anti-Ly6G, anti-Erythroid marker (TER-119), anti-CD11c, followed by streptavidin-paramagnetic particles (BD Bioscience) according to manufacturer’s instructions. The harvested cells were labeled with fluorochrome-conjugated antibodies (CD45+Lin−CD90.2+CD25+) and sorted by Aria III (BD Bioscience). For human ILC2 sorting, PBMCs were labeled with biotin-conjugated anti-CD2, anti-CD3, anti-CD10, anti-CD11b, anti-CD14, anti-CD16, anti-CD19, anti-CD56, anti-CD123, and anti-CD235a to deplete T cells, B cells, NK cells, myeloid cells, granulocytes, and red blood cells, followed by streptavidin-paramagnetic particles. Then, the collected lineage-negative cells were stained with the specific fluorochrome-conjugated antibodies for ILC2s (CD45+Lin−CD127+CRTH2+CD161+). The purity of cell sorting was ≥95%. Antibodies used are listed in Table S1.
Adoptive transfer of ILC2
Lung ILC2s were sorted from IL-33 i.p. treated PPARγfl/fl and PPARγfl/fl Vav1Cre mice, and rested in complete medium for 24 h, before intravenously transferred into NCG mice, respectively (1.5 × 104 cells/mouse). Mice were then challenged with IL-33 intranasally for 3 consecutive days.7 Mice were sacrificed and analyzed 24 h later after the last challenge.
Cell isolation from tissues
To isolate cells from BALF and lung tissue, lungs were flushed by 0.5 ml cold PBS twice via a thin tube inserted into a cut made in the trachea as described. Then, lungs were perfused with 20 ml cold PBS. Lung tissues were cut into small pieces and digested with 0.5 mg/ml type I collagenase (Invitrogen, USA) in RPMI-1640 for 1 h at 37 °C with continuous agitation in an incubator. The crude suspensions were further filtered through 70 μm cell strainers. Mononuclear cells were obtained by a 40%/80% Percoll (GE Healthcare, Uppsala, Sweden) gradient. Splenocytes and mLN cells were obtained by mechanical disruption on 70 µm cell strainers. Isolation of cells from large intestine was performed by digestion with 0.5 mg/ml collagenase I and 5 U/ml DNase for 40 min as described.
Human PBMC isolation
This study was approved by the Ethics Review Board of Sun Yat-sen University. Human peripheral blood mononuclear cells (PBMCs) from fresh blood samples were isolated by Ficoll centrifugation as described.59 Isolated PBMCs were washed and resuspended in cold PBS containing 1% FBS before subsequent use.
ILC2 culture in vitro
For ILC2 function analysis in vitro, 5 × 103 lung ILC2 were cultured in the presence of 20 ng/ml IL-33, 10 ng/ml IL-2, and 20 ng/ml IL-7 for 3 days,7 the supernatants were collected to measure IL-5 and IL-13 by ELISA. For rosiglitazone and GW9662 treatments, both were used at concentration of 10 μM.60,61
Quantitative real-time PCR (qRT-PCR)
Total mRNA were extracted using TRIzol (Invitrogen) and reverse transcribed with a synthesis kit (Takara). Genes mRNA expression were analyzed by qPCR. The primer sequences were listed in Table S2.
C. rodentium model
Mice were orally gavaged with 2 × 109 CFUs of C. rodentium44 and were monitored daily to record weight loss. Mice were sacrificed on day 6, the colon length were measured. The cytokine production of ILC1 and ILC3 from colon lamina propria was evaluated by flow cytometry.
Retroviral transduction
Retroviral transduction was performed as described previously. Lung ILC2 were sorted from PPARγfl/fl and PPARγfl/fl Vav1Cre mice and treated with retrovirus-containing supernatants supplemented with polybrene (8 μg/ml) in 96-well plate, centrifuged at 1000 × g for 2 h at 32 °C, then cultured at 37 °C for another 6 h. Cells were washed and cultured in fresh complete medium with 10 ng/ml of IL-2, IL-7, and IL-33 for 3 days. The efficiency of retroviral infection was evaluated by GFP (+) cells using flow cytometry. The supernatants were collected for the analysis of IL-5 and IL-13 by ELISA.
Chromatin immunoprecipitation (ChIP)
Lineage negative cells were sorted from lung of WT mice, ChIP assay was conducted as previously described. Briefly, Lineage negative cells were fixed with a 1% formaldehyde solution, lysed, and sheared by sonication. Cell lysates were precleared with protein G-agarose and immunoprecipitated with anti-PPARγ antibodies or an anti-IgG control. Antibody–chromatin complexes were collected with protein G-agarose. The DNA was purified and quantified by PCR using indicated primers (Table S2). 10% of the lysate before immunoprecipitation was used as the input control. Data are presented as the folds of immunoprecipitated to input cycle threshold values.
Statistics
All data are derived from at least two independent experiments. Statistical analysis was performed with GraphPad Prism 8.0. Results show mean ± SEM and statistical significance was determined by a two-tailed unpaired Student’s t test or one-way ANOVA with Bonferroni post-test. P value < 0.05 was considered significant.
References
Papi, A., Brightling, C., Pedersen, S. E. & Reddel, H. K. Asthma. Lancet 391, 783–800 (2018).
Lambrecht, B. N. & Hammad, H. The immunology of asthma. Nat. Immunol. 16, 45–56 (2015).
Divekar, R. & Kita, H. Recent advances in epithelium-derived cytokines (IL-33, IL-25, and thymic stromal lymphopoietin) and allergic inflammation. Curr. Opin. Allergy Clin. Immunol. 15, 98–103 (2015).
Monticelli, L. A., Sonnenberg, G. F. & Artis, D. Innate lymphoid cells: critical regulators of allergic inflammation and tissue repair in the lung. Curr. Opin. Immunol. 24, 284–289 (2012).
Halim, T. Y. et al. Group 2 innate lymphoid cells are critical for the initiation of adaptive T helper 2 cell-mediated allergic lung inflammation. Immunity 40, 425–435 (2014).
Mirchandani, A. S. et al. Type 2 innate lymphoid cells drive CD4+ Th2 cell responses. J. Immunol. 192, 2442–2448 (2014).
Lei, A. H. et al. ICAM-1 controls development and function of ILC2. J. Exp. Med. 215, 2157–2174 (2018).
Serafini, N., Vosshenrich, C. A. & Di Santo, J. P. Transcriptional regulation of innate lymphoid cell fate. Nat. Rev. Immunol. 15, 415–428 (2015).
Gasteiger, G., Fan, X., Dikiy, S., Lee, S. Y. & Rudensky, A. Y. Tissue residency of innate lymphoid cells in lymphoid and nonlymphoid organs. Science 350, 981–985 (2015).
Walker, J. A., Barlow, J. L. & McKenzie, A. N. J. Innate lymphoid cells—how did we miss them? Nat. Rev. Immunol. 13, 75–87 (2013).
Kabata, H., Moro, K. & Koyasu, S. The group 2 innate lymphoid cell (ILC2) regulatory network and its underlying mechanisms. Immunol. Rev. 286, 37–52 (2018).
Brestoff, J. R. et al. Group 2 innate lymphoid cells promote beiging of white adipose tissue and limit obesity. Nature 519, 242–246 (2015).
Monticelli, L. A. et al. Innate lymphoid cells promote lung-tissue homeostasis after infection with influenza virus. Nat. Immunol. 12, 1045–1054 (2011).
Vivier, E. et al. Innate lymphoid cells: 10 years on. Cell 174, 1054–1066 (2018).
Hurrell, B. P., Shafiei Jahani, P. & Akbari, O. Social networking of group two innate lymphoid cells in allergy and asthma. Front. Immunol. 9, 2694 (2018).
Hoyler, T. et al. The transcription factor GATA-3 controls cell fate and maintenance of type 2 innate lymphoid cells. Immunity 37, 634–648 (2012).
Mjosberg, J. et al. The transcription factor GATA3 is essential for the function of human type 2 innate lymphoid cells. Immunity 37, 649–659 (2012).
Clark, R. B. The role of PPARs in inflammation and immunity. J. Leukoc. Biol. 71, 388–400 (2002).
Ahmadian, M. et al. PPARgamma signaling and metabolism: the good, the bad and the future. Nat. Med. 19, 557–566 (2013).
Tontonoz, P., Hu, E. & Spiegelman, B. M. Stimulation of adipogenesis in fibroblasts by PPAR gamma 2, a lipid-activated transcription factor. Cell 79, 1147–1156 (1994).
Daynes, R. A. & Jones, D. C. Emerging roles of PPARs in inflammation and immunity. Nat. Rev. Immunol. 2, 748–759 (2002).
Honda, K., Marquillies, P., Capron, M. & Dombrowicz, D. Peroxisome proliferator-activated receptor gamma is expressed in airways and inhibits features of airway remodeling in a mouse asthma model. J. Allergy Clin. Immunol. 113, 882–888 (2004).
Benayoun, L. et al. Regulation of peroxisome proliferator-activated receptor gamma expression in human asthmatic airways: relationship with proliferation, apoptosis, and airway remodeling. Am. J. Respir. Crit. Care Med. 164, 1487–1494 (2001).
Li, W. et al. Association of peroxisome proliferator-activated receptor-gamma gene polymorphisms and gene–gene interaction with asthma risk in a Chinese adults population. Int. J. Clin. Exp. Med. 8, 19346–19352 (2015).
Zhang, Y., Wang, Z. & Ma, T. Associations of genetic polymorphisms relevant to metabolic pathway of vitamin D3 with development and prognosis of childhood bronchial asthma. DNA Cell Biol. 36, 682–692 (2017).
Spears, M. et al. Bronchodilatory effect of the PPAR-gamma agonist rosiglitazone in smokers with asthma. Clin. Pharm. Ther. 86, 49–53 (2009).
Banno, A., Reddy, A. T., Lakshmi, S. P. & Reddy, R. C. PPARs: key regulators of airway inflammation and potential therapeutic targets in asthma. Nucl. Receptor Res. 5, 101306 (2018).
Narala, V. R. et al. Pioglitazone is as effective as dexamethasone in a cockroach allergen-induced murine model of asthma. Respir. Res. 8, 90 (2007).
Lee, S. Y. et al. Peroxisome proliferator-activated receptor-gamma inhibits cigarette smoke solution-induced mucin production in human airway epithelial (NCI-H292) cells. Am. J. Physiol. Lung Cell. Mol. Physiol. 291, L84–L90 (2006).
Schneider, C. et al. Alveolar macrophages are essential for protection from respiratory failure and associated morbidity following influenza virus infection. PLoS Pathog. 10, e1004053 (2014).
Hammad, H. et al. Activation of peroxisome proliferator-activated receptor-gamma in dendritic cells inhibits the development of eosinophilic airway inflammation in a mouse model of asthma. Am. J. Pathol. 164, 263–271 (2004).
Nobs, S. P. et al. PPARgamma in dendritic cells and T cells drives pathogenic type-2 effector responses in lung inflammation. J. Exp. Med. 214, 3015–3035 (2017).
Chen, T. et al. PPAR-γ promotes type 2 immune responses in allergy and nematode infection. Sci. Immunol. 2, pii: eaal5196 (2017).
Pokrovskii, M. et al. Characterization of transcriptional regulatory networks that promote and restrict identities and functions of intestinal innate lymphoid cells. Immunity 51, 185–197. e186 (2019).
Karagiannis, F. et al. Lipid-droplet formation drives pathogenic group 2 innate lymphoid cells in airway inflammation. Immunity 52, 620–634. e626 (2020).
Taylor, S. et al. PD-1 regulates KLRG1(+) group 2 innate lymphoid cells. J. Exp. Med. 214, 1663–1678 (2017).
Batyrova, B. et al. PD-1 expression affects cytokine production by ILC2 and is influenced by peroxisome proliferator-activated receptor-gamma. Immun. Inflamm. Dis. 8, 8–23 (2020).
Robinette, M. L. et al. Transcriptional programs define molecular characteristics of innate lymphoid cell classes and subsets. Nat. Immunol. 16, 306–317 (2015).
Ricote, M. et al. Expression of the peroxisome proliferator-activated receptor gamma (PPARgamma) in human atherosclerosis and regulation in macrophages by colony stimulating factors and oxidized low density lipoprotein. Proc. Natl Acad. Sci. USA 95, 7614–7619 (1998).
Salimi, M. et al. A role for IL-25 and IL-33-driven type-2 innate lymphoid cells in atopic dermatitis. J. Exp. Med. 210, 2939–2950 (2013).
Hazenberg, M. D. & Spits, H. Human innate lymphoid cells. Blood 124, 700–709 (2014).
Huang, Y. et al. IL-25-responsive, lineage-negative KLRG1(hi) cells are multipotential ‘inflammatory’ type 2 innate lymphoid cells. Nat. Immunol. 16, 161–169 (2015).
Abt, M. C. et al. Innate immune defenses mediated by two ILC subsets are critical for protection against acute clostridium difficile infection. Cell Host Microbe 18, 27–37 (2015).
Satoh-Takayama, N. et al. The chemokine receptor CXCR6 controls the functional topography of interleukin-22 producing intestinal innate lymphoid cells. Immunity 41, 776–788 (2014).
Ebbo, M., Crinier, A., Vely, F. & Vivier, E. Innate lymphoid cells: major players in inflammatory diseases. Nat. Rev. Immunol. 17, 665–678 (2017).
Li, B. W. et al. T cells are necessary for ILC2 activation in house dust mite-induced allergic airway inflammation in mice. Eur. J. Immunol. 46, 1392–1403 (2016).
Liu, B., Lee, J. B., Chen, C. Y., Hershey, G. K. & Wang, Y. H. Collaborative interactions between type 2 innate lymphoid cells and antigen-specific CD4+ Th2 cells exacerbate murine allergic airway diseases with prominent eosinophilia. J. Immunol. 194, 3583–3593 (2015).
Moriyama, S. et al. beta2-adrenergic receptor-mediated negative regulation of group 2 innate lymphoid cell responses. Science 359, 1056–1061 (2018).
Guan, H. P., Ishizuka, T., Chui, P. C., Lehrke, M. & Lazar, M. A. Corepressors selectively control the transcriptional activity of PPARgamma in adipocytes. Genes Dev. 19, 453–461 (2005).
Matsusue, K. et al. Hepatic steatosis in leptin-deficient mice is promoted by the PPARgamma target gene Fsp27. Cell Metab. 7, 302–311 (2008).
Anderson, J. R. et al. Evaluation of the PPAR-gamma agonist pioglitazone in mild asthma: a double-blind randomized controlled trial. PLoS ONE 11, e0160257 (2016).
Kaler, M. et al. A randomized, placebo-controlled, double-blinded, crossover trial of pioglitazone for severe asthma. J. Allergy Clin. Immunol. 140, 1716–1718 (2017).
Richards, D. B., Bareille, P., Lindo, E. L., Quinn, D. & Farrow, S. N. Treatment with a peroxisomal proliferator activated receptor gamma agonist has a modest effect in the allergen challenge model in asthma: a randomised controlled trial. Respir. Med. 104, 668–674 (2010).
Wilhelm, C. et al. Critical role of fatty acid metabolism in ILC2-mediated barrier protection during malnutrition and helminth infection. J. Exp. Med. 213, 1409–1418 (2016).
Poulsen, L., Siersbaek, M. & Mandrup, S. PPARs: fatty acid sensors controlling metabolism. Semin. Cell Dev. Biol. 23, 631–639 (2012).
Lee, M. W. et al. Activated type 2 innate lymphoid cells regulate beige fat biogenesis. Cell 160, 74–87 (2015).
Maazi, H. et al. ICOS:ICOS-ligand interaction is required for type 2 innate lymphoid cell function, homeostasis, and induction of airway hyperreactivity. Immunity 42, 538–551 (2015).
Monticelli, L. A. et al. Arginase 1 is an innate lymphoid-cell-intrinsic metabolic checkpoint controlling type 2 inflammation. Nat. Immunol. 17, 656–665 (2016).
Qin, A. et al. Expansion of monocytic myeloid-derived suppressor cells dampens T cell function in HIV-1-seropositive individuals. J. Virol. 87, 1477–1490 (2013).
Wan, J. et al. Pioglitazone modulates the proliferation and apoptosis of vascular smooth muscle cells via peroxisome proliferators-activated receptor-gamma. Diabetol. Metab. Syndr. 6, 101 (2014).
Whiteside, C. et al. Rosiglitazone prevents high glucose-induced vascular endothelial growth factor and collagen IV expression in cultured mesangial cells. Exp. Diabetes Res. 2009, 910783 (2009).
Acknowledgements
This work was supported by the following grants to J.Z.: National Natural Science Foundation of China Grants 81925018, 81771665 (to J.Z.); the Start-Up Fund for High-Level Talents of Tianjin Medical University (to J.Z.).
Author information
Authors and Affiliations
Contributions
Q.X., J.H., and A.L. performed the experiments and analyzed the data. H.X., L.Z., and P.Z. participated in experiments. G.J. provided suggestions for experimental design. J.Z. conceptualized, supervised, interpreted the experiments, and wrote the paper.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Xiao, Q., He, J., Lei, A. et al. PPARγ enhances ILC2 function during allergic airway inflammation via transcription regulation of ST2. Mucosal Immunol 14, 468–478 (2021). https://doi.org/10.1038/s41385-020-00339-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41385-020-00339-6
This article is cited by
-
Maternal antibiotic exposure enhances ILC2 activation in neonates via downregulation of IFN1 signaling
Nature Communications (2023)
-
Multiscale 3D genome organization underlies ILC2 ontogenesis and allergic airway inflammation
Nature Immunology (2023)
-
Adenosine restrains ILC2-driven allergic airway inflammation via A2A receptor
Mucosal Immunology (2022)
-
The devil's in the detail: cell-specific role of PPARγ in ILC2 activation by IL-33
Mucosal Immunology (2021)
-
PPARɣ drives IL-33-dependent ILC2 pro-tumoral functions
Nature Communications (2021)