Abstract
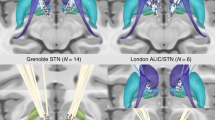
Deep brain stimulation (DBS) of the ventral anterior limb of the internal capsule (vALIC) is effective for refractory obsessive-compulsive disorder (OCD). Retrospective evaluation showed that stimulation closer to the supero-lateral branch of the medial forebrain bundle (slMFB), within the vALIC, was associated with better response to DBS. The present study is the first to compare outcomes of DBS targeted at the vALIC using anatomical landmarks and DBS with connectomic tractography-based targeting of the slMFB. We included 20 OCD-patients with anatomical landmark-based DBS of the vALIC that were propensity score matched to 20 patients with tractography-based targeting of electrodes in the slMFB. After one year, we compared severity of OCD, anxiety and depression symptoms, response rates, time to response, number of parameter adjustments, average current, medication usage and stimulation-related adverse effects. There was no difference in Y-BOCS decrease between patients with anatomical landmark-based and tractography-based DBS. Nine (45%) patients with anatomical landmark-based DBS and 13 (65%) patients with tractography-based DBS were responders (BF10 = 1.24). The course of depression and anxiety symptoms, time to response, number of stimulation adjustments or medication usage did not differ between groups. Patients with tractography-based DBS experienced fewer stimulation-related adverse effects than patients with anatomical landmark-based DBS (38 vs 58 transient and 1 vs. 17 lasting adverse effects; BF10 = 14.968). OCD symptoms in patients with anatomical landmark-based DBS of the vALIC and tractography-based DBS of the slMFB decrease equally, but patients with tractography-based DBS experience less adverse effects.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Bergfeld IO, Dijkstra E, Graat I, de Koning P, van den Boom BJG, Arbab T, et al. Invasive and Non-invasive neurostimulation for OCD. Curr Top Behav Neurosci. 2021;49:399–436.
Denys D, Graat I, Mocking R, de Koning P, Vulink N, Figee M, et al. Efficacy of deep brain stimulation of the ventral anterior limb of the internal capsule for refractory obsessive-compulsive disorder: a clinical cohort of 70 patients. Am J Psychiatry. 2020;177:265–71.
Coenen VA, Schlaepfer TE, Goll P, Reinacher PC, Voderholzer U, Tebartz van Elst L, et al. The medial forebrain bundle as a target for deep brain stimulation for obsessive-compulsive disorder. CNS Spectr. 2017;22:282–9.
Baldermann JC, Schüller T, Kohl S, Voon V, Li N, Hollunder B, et al. Connectomic deep brain stimulation for obsessive-compulsive disorder. Biol Psychiatry. 2021;90:678–88.
Maier-Hein KH, Neher PF, Houde J-C, Côté M-A, Garyfallidis E, Zhong J, et al. The challenge of mapping the human connectome based on diffusion tractography. Nat Commun. 2017;8:1349.
Coenen VA, Schlaepfer TE, Reinacher PC, Mast H, Urbach H, Reisert M. Machine learning-aided personalized DTI tractographic planning for deep brain stimulation of the superolateral medial forebrain bundle using HAMLET. Acta Neurochir. 2019;161:1559–69.
Liebrand LC, Caan MWA, Schuurman PR, van den Munckhof P, Figee M, Denys D, et al. Individual white matter bundle trajectories are associated with deep brain stimulation response in obsessive-compulsive disorder. Brain Stimulation. 2019;12:353–60.
Li N, Baldermann JC, Kibleur A, Treu S, Akram H, Elias GJB, et al. A unified connectomic target for deep brain stimulation in obsessive-compulsive disorder. Nat Commun. 2020;11:3364.
Graat I, Mocking R, Figee M, Vulink N, de Koning P, Ooms P, et al. Long-term outcome of deep brain stimulation of the ventral part of the anterior limb of the internal capsule in a cohort of 50 patients with treatment-refractory obsessive-compulsive disorder. Biol Psychiatry. 2020;90:714–20.
Goodman WK, Price LH, Rasmussen SA, Mazure C, Fleischmann RL, Hill CL, et al. The Yale-Brown Obsessive Compulsive Scale. I. Development, use, and reliability. Arch Gen Psychiatry. 1989;46:1006–11.
Hamilton M. The assessment of anxiety states by rating. Br J Med Psychol. 1959;32:50–5.
Hamilton M. A rating scale for depression. J Neurol Neurosurg Psychiatry. 1960;23:56–62.
Kuss O, Blettner M, Börgermann J. Propensity Score: an alternative method of analyzing treatment effects. Dtsch Arzteblatt Int. 2016;113:597–603.
Ho D, Imai K, King G, Stuart EA. MatchIt: nonparametric preprocessing for parametric causal inference. J Stat Softw. 2011;42:1–28.
Alonso P, Cuadras D, Gabriels L, Denys D, Goodman W, Greenberg BD, et al. Deep brain stimulation for obsessive-compulsive disorder: A meta-analysis of treatment outcome and predictors of response. PLoS ONE. 2015;10:1–16.
Graat I, Mocking RJT, de Koning P, Vulink N, Figee M, van den Munckhof P, et al. Predicting response to vALIC deep brain stimulation for refractory obsessive-compulsive disorder. J Clin Psychiatry. 2021;82.
van Doorn J, van den Bergh D, Böhm U, Dablander F, Derks K, Draws T, et al. The JASP guidelines for conducting and reporting a Bayesian analysis. Psychon Bull Rev. 2020. https://doi.org/10.3758/s13423-020-01798-5.
Widge AS, Zhang F, Gosai A, Papadimitrou G, Wilson-Braun P, Tsintou M, et al. Patient-specific connectomic models correlate with, but do not reliably predict, outcomes in deep brain stimulation for obsessive-compulsive disorder. Neuropsychopharmacol: Offic Publ Am Coll of Neuropsychopharmacol. 2021. 47:965–72.
Hageman SB, van Rooijen G, Bergfeld IO, Schirmbeck F, de Koning P, Schuurman PR, et al. Deep brain stimulation versus ablative surgery for treatment-refractory obsessive-compulsive disorder: A meta-analysis. Acta Psychiatr Scand. 2021. https://doi.org/10.1111/acps.13276.
Schlaepfer TE, Bewernick BH, Kayser S, Mädler B, Coenen VA. Rapid effects of deep brain stimulation for treatment-resistant major depression. Biol Psychiatry. 2013;73:1204–12.
Mar-Barrutia L, Real E, Segalás C, Bertolín S, Menchón JM, Alonso P. Deep brain stimulation for obsessive-compulsive disorder: A systematic review of worldwide experience after 20 years. World J Psychiatry. 2021;11:659–80.
Kim Y, McGee S, Czeczor JK, Walker AJ, Kale RP, Kouzani AZ, et al. Nucleus accumbens deep-brain stimulation efficacy in ACTH-pretreated rats: alterations in mitochondrial function relate to antidepressant-like effects. Transl Psychiatry. 2016;6:e842–e842.
Haber SN, Yendiki A, Jbabdi S, Four deep brain stimulation targets for obsessive-compulsive disorder: are they different? Biol Psychiatry. 2021;90:667–77
Mai JK, Majtanik M, Paxinos G Atlas of the human brain. Academic Press; 2015.
Levitt P, Rakic P, Goldman-Rakic P. Region-specific distribution of catecholamine afferents in primate cerebral cortex: A fluorescence histochemical analysis. J Comp Neurol. 1984;227:23–36.
Lehman JF, Greenberg BD, Mcintyre CC, Rasmussen SA, Haber SN. Rules ventral prefrontal cortical axons use to reach their targets: Implications for diffusion tensor imaging tractography and deep brain stimulation for psychiatric illness. J Neurosci. 2011;31:10392–402.
Haynes WIA, Haber SN. The organization of prefrontal-subthalamic inputs in primates provides an anatomical substrate for both functional specificity and integration: Implications for basal ganglia models and deep brain stimulation. J Neurosci. 2013;33:4804–14.
Coenen VA, Döbrössy MD, Teo SJ, Wessolleck J, Sajonz BEA, Reinacher PC, et al. Diverging prefrontal cortex fiber connection routes to the subthalamic nucleus and the mesencephalic ventral tegmentum investigated with long range (normative) and short range (ex-vivo high resolution) 7T DTI. Brain Struct Funct. 2021. https://doi.org/10.1007/s00429-021-02373-x.
Makris N, Rathi Y, Mouradian P, Bonmassar G, Papadimitriou G, Ing WI, et al. Variability and anatomical specificity of the orbitofrontothalamic fibers of passage in the ventral capsule/ventral striatum (VC/VS): precision care for patient-specific tractography-guided targeting of deep brain stimulation (DBS) in obsessive compulsiv. Brain Imaging Behav. 2016;10:1054–67.
Mosley PE, Windels F, Morris J, Coyne T, Marsh R, Giorni A, et al. A randomised, double-blind, sham-controlled trial of deep brain stimulation of the bed nucleus of the stria terminalis for treatment-resistant obsessive-compulsive disorder. Transl Psychiatry. 2021;11:190.
Shephard E, Stern ER, van den Heuvel OA, Costa DLC, Batistuzzo MC, Godoy PBG, et al. Toward a neurocircuit-based taxonomy to guide treatment of obsessive–compulsive disorder. Mol Psychiatry. 2021;26:4583–604.
Tyagi H, Apergis-Schoute AM, Akram H, Foltynie T, Limousin P, Drummond LM, et al. A randomized trial directly comparing ventral capsule and anteromedial subthalamic nucleus stimulation in obsessive-compulsive disorder: clinical and imaging evidence for dissociable effects. Biol Psychiatry. 2019;85:726–34.
Robbins TW, Vaghi MM, Banca P. Obsessive-compulsive disorder: puzzles and prospects. Neuron 2019;102:27–47.
Funding
The present study received no funding. PR Schuurman acts as independent advisor for Medtronic and Boston Scientific. RJT Mocking and IO Bergfeld are funded by unrestricted ABC Talent Grants. DD, PRS, GvW and IO Bergfeld have received funding from ZonMw (nr 636310016) and Boston Scientific (in kind) for a trial on deep brain stimulation for depression. GvW received research funding from Philips. The other authors have no disclosures to report.
Author information
Authors and Affiliations
Contributions
Conception and design: IG, RM, LL, IO, and DD. Data/literature acquisition: IG and IO. Data/literature analysis and interpretation: IG, IO, and RM. Statistical analysis: IG, IO, and RM. Drafting the manuscript: IG. Critical revision of the manuscript: All authors. Supervision: RM, IO, GvW, and DD.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Graat, I., Mocking, R.J.T., Liebrand, L.C. et al. Tractography-based versus anatomical landmark-based targeting in vALIC deep brain stimulation for refractory obsessive-compulsive disorder. Mol Psychiatry 27, 5206–5212 (2022). https://doi.org/10.1038/s41380-022-01760-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41380-022-01760-y
This article is cited by
-
Closing the loop in psychiatric deep brain stimulation: physiology, psychometrics, and plasticity
Neuropsychopharmacology (2024)