Abstract
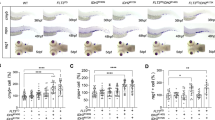
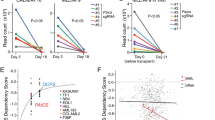
Inactivating mutations in TET2 serve as an initiating genetic lesion in the transformation of hematopoietic stem and progenitor cells (HSPCs). Thus, effective therapy for this subset of patients would ideally include drugs that are selectively lethal in TET2-mutant HSPCs, at dosages that spare normal HSPCs. In this study, we tested 129 FDA-approved anticancer drugs in a tet2-deficient zebrafish model and showed that topoisomerase 1 (TOP1)-targeted drugs and PARP1 inhibitors selectively kill tet2-mutant HSPCs. We found that Tet2-deficient murine bone marrow progenitors and CRISPR-Cas9-induced TET2-mutant human AML cells were more sensitive to both classes of drugs compared with matched control cells. The mechanism underlying the selective killing of TET2-mutant blood cells by these drugs was due to aberrantly low levels of tyrosyl-DNA phosphodiesterase 1 (TDP1), an enzyme that is important for removing TOP1 cleavage complexes (TOP1cc). Low TDP1 levels yield sensitivity to TOP1-targeted drugs or PARP1 inhibitors and an inability to remove TOP1 cleavage complexes, leading to DNA double-strand breaks and cell death. The finding that TET2 mutations render HSPCs uniquely vulnerable to disruption of TOP1 and PARP1 activity may therefore represent a unique opportunity to use relatively low dosages of these drugs for the “precision therapy” of TET2-mutant myeloid malignancies.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Bowman RL, Levine RL. TET2 in normal and malignant hematopoiesis. Cold Spring Harb Persp Med. 2017;7:a026518.
Alderton GK. Leukaemia and lymphoma: the expansive reach of TET2. Nat Rev Cancer. 2011;11:535.
Nakajima H, Kunimoto H. TET2 as an epigenetic master regulator for normal and malignant hematopoiesis. Cancer Sci. 2014;105:1093–9.
Chou WC, Chou SC, Liu CY, Chen CY, Hou HA, Kuo YY, et al. TET2 mutation is an unfavorable prognostic factor in acute myeloid leukemia patients with intermediate-risk cytogenetics. Blood. 2011;118:3803–10.
Liu WJ, Tan XH, Luo XP, Guo BP, Wei ZJ, Ke Q, et al. Prognostic significance of Tet methylcytosine dioxygenase 2 (TET2) gene mutations in adult patients with acute myeloid leukemia: a meta-analysis. Leuk lymphoma. 2014;55:2691–8.
Sato H, Wheat JC, Steidl U, Ito K. DNMT3A and TET2 in the pre-leukemic phase of hematopoietic disorders. Front Oncol. 2016;6:187.
Genovese G, Kahler AK, Handsaker RE, Lindberg J, Rose SA, Bakhoum SF, et al. Clonal hematopoiesis and blood-cancer risk inferred from blood DNA sequence. N. Engl J Med. 2014;371:2477–87.
Jaiswal S, Fontanillas P, Flannick J, Manning A, Grauman PV, Mar BG, et al. Age-related clonal hematopoiesis associated with adverse outcomes. N. Engl J Med. 2014;371:2488–98.
Jae-Sook A, Hyeoung-Joon K, Yeo-Kyeoung K, Sung-Hoon J, Deok-Hwan Y, Je-Jung L, et al. Adverse prognostic effect of homozygous TET2 mutation on the relapse risk of acute myeloid leukemia in patients of normal karyotype. Haematologica. 2015;100:e351–3.
Wakita S, Yamaguchi H, Omori I, Terada K, Ueda T, Manabe E, et al. Mutations of the epigenetics-modifying gene (DNMT3a, TET2, IDH1/2) at diagnosis may induce FLT3-ITD at relapse in de novo acute myeloid leukemia. Leukemia. 2013;27:1044–52.
Chen ES. Targeting epigenetics using synthetic lethality in precision medicine. Cell Mol Life Sci. 2018;75:3381–92.
Mair B, Moffat J, Boone C, Andrews BJ. Genetic interaction networks in cancer cells. Curr Opin Genet Dev. 2019;54:64–72.
Ryan CJ, Bajrami I, Lord CJ. Synthetic lethality and cancer—penetrance as the major barrier. Trends Cancer. 2018;4:671–83.
Smith LM, Willmore E, Austin CA, Curtin NJ. The novel poly(ADP-Ribose) polymerase inhibitor, AG14361, sensitizes cells to topoisomerase I poisons by increasing the persistence of DNA strand breaks. Clin Cancer Res. 2005;11:8449–57.
El-Khamisy SF, Caldecott KW. TDP1-dependent DNA single-strand break repair and neurodegeneration. Mutagenesis. 2006;21:219–24.
Das BB, Huang SY, Murai J, Rehman I, Ame JC, Sengupta S, et al. PARP1-TDP1 coupling for the repair of topoisomerase I-induced DNA damage. Nucleic Acids Res. 2014;42:4435–49.
Pommier Y, Barcelo JM, Rao VA, Sordet O, Jobson AG, Thibaut L, et al. Repair of topoisomerase I‐mediated DNA damage. Prog Nucleic Acid Res Mol Biol. 2006;81:179–229.
Gilbert DC, Chalmers AJ, El-Khamisy SF. Topoisomerase I inhibition in colorectal cancer: biomarkers and therapeutic targets. Br J cancer. 2012;106:18–24.
Gjini E, Mansour MR, Sander JD, Moritz N, Nguyen AT, Kesarsing M, et al. A zebrafish model of myelodysplastic syndrome produced through tet2 genomic editing. Mol Cell Biol. 2015;35:789–804.
Choy H, MacRae R. Irinotecan and radiation in combined-modality therapy for solid tumors. Oncol (Williston Park). 2001;15:22–8.
Chen AY, Chen PM, Chen YJ. DNA topoisomerase I drugs and radiotherapy for lung cancer. J Thorac Dis. 2012;4:390–7.
Bolli N, Payne EM, Grabher C, Lee JS, Johnston AB, Falini B, et al. Expression of the cytoplasmic NPM1 mutant (NPMc+) causes the expansion of hematopoietic cells in zebrafish. Blood. 2010;115:3329–40.
Metscher BD, Ahlberg PE. Zebrafish in context: uses of a laboratory model in comparative studies. Dev Biol. 1999;210:1–14.
Liu D, Wang Z, Xiao A, Zhang Y, Li W, Zu Y, et al. Efficient gene targeting in zebrafish mediated by a zebrafish-codon-optimized cas9 and evaluation of off-targeting effect. J Genet Genomics. 2014;41:43–6.
North TE, Goessling W, Peeters M, Li P, Ceol C, Lord AM, et al. Hematopoietic stem cell development is dependent on blood flow. Cell. 2009;137:736–48.
Gjini E, Jing CB, Nguyen AT, Reyon D, Gans E, Kesarsing M, et al. Disruption of asxl1 results in myeloproliferative neoplasms in zebrafish. Dis Model Mech. 2019;12:dmm035790.
An J, Gonzalez-Avalos E, Chawla A, Jeong M, Lopez-Moyado IF, Li W, et al. Acute loss of TET function results in aggressive myeloid cancer in mice. Nat Commun. 2015;6:10071.
Kushner BH, Kramer K, Modak S, Cheung NK. Camptothecin analogs (irinotecan or topotecan) plus high-dose cyclophosphamide as preparative regimens for antibody-based immunotherapy in resistant neuroblastoma. Clin Cancer Res. 2004;10:84–7.
Linda JK, Yang L-X. γ-H2AX-A novel biomarker for Double-strand Breaks. In vivo 2008;22:305–9.
North TE, Goessling W, Walkley CR, Lengerke C, Kopani KR, Lord AM, et al. Prostaglandin E2 regulates vertebrate haematopoietic stem cell homeostasis. Nature. 2007;447:1007–11.
Gao R, Das BB, Chatterjee R, Abaan OD, Agama K, Matuo R, et al. Epigenetic and genetic inactivation of tyrosyl-DNA-phosphodiesterase 1 (TDP1) in human lung cancer cells from the NCI-60 panel. DNA Repair. 2014;13:1–9.
Hwang WY, Fu Y, Reyon D, Maeder ML, Tsai SQ, Sander JD, et al. Efficient genome editing in zebrafish using a CRISPR-Cas system. Nat Biotechnol. 2013;31:227–9.
Cimmino L, Dolgalev I, Wang Y, Yoshimi A, Martin GH, Wang J, et al. Restoration of TET2 function blocks aberrant self-renewal and leukemia progression. Cell. 2017;170:1079–95. e1020.
Cong L, Ran FA, Cox D, Lin S, Barretto R, Habib N, et al. Multiplex genome engineering using CRISPR/Cas systems. Science. 2013;339:819–23.
Meisenberg C, Ward SE, Schmid P, El-Khamisy SF. TDP1/TOP1 ratio as a promising indicator for the response of small cell lung cancer to topotecan. J Cancer Sci Ther. 2014;6:258–67.
Duma N, Gast KC, Choong GM, Leon-Ferre RA, O’Sullivan CC. Where do we stand on the integration of PARP inhibitors for the treatment of breast cancer? Curr Oncol Rep. 2018;20:63.
Mateo J, Carreira S, Sandhu S, Miranda S, Mossop H, Perez-Lopez R, et al. DNA-repair defects and olaparib in metastatic prostate cancer. N. Engl J Med. 2015;373:1697–708.
Wang L, Hamard PJ, Nimer SD. PARP inhibitors: a treatment option for AML? Nat Med. 2015;21:1393–4.
Esposito MT, Zhao L, Fung TK, Rane JK, Wilson A, Martin N, et al. Synthetic lethal targeting of oncogenic transcription factors in acute leukemia by PARP inhibitors. Nat Med. 2015;21:1481–90.
Zhao L, So CW. PARP-inhibitor-induced synthetic lethality for acute myeloid leukemia treatment. Exp Hematol. 2016;44:902–7.
Acknowledgements
We thank Cicely Jette and John Gilbert for editorial assistance and critical comments. This work was supported by Edward P. Evans Foundation (to ATL); the Andrew McDonough B+ Foundation (to C-BJ), and an International Award of Lady Tata Memorial Trust (to C-BJ).
Author information
Authors and Affiliations
Contributions
C-BJ and CF contributed to experimental work, experimental design, writing, and data analysis and interpretation. NP contributed to serial plating experimental work on Tet2-mutant progenitor cells. MW contributed to the bioinformatics analysis in AML database. SH analyzed the data. ATL directed all experimental activity and contributed to data interpretation, analysis, and writing of manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Jing, CB., Fu, C., Prutsch, N. et al. Synthetic lethal targeting of TET2-mutant hematopoietic stem and progenitor cells (HSPCs) with TOP1-targeted drugs and PARP1 inhibitors. Leukemia 34, 2992–3006 (2020). https://doi.org/10.1038/s41375-020-0927-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41375-020-0927-5