Abstract
Objective
To determine the etiology and outcome of non-immune hydrops fetalis (NIHF) according to gestational age at diagnosis and intrauterine treatment.
Study design
A total of 122 NIHF cases were included. Medical records and ultrasonographic images were reviewed. The etiology, outcome, and intrauterine treatment were assessed.
Results
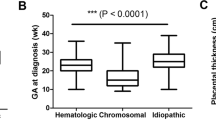
The etiology was determined in 100 cases, and Hb Bart’s disease was the most common. Two cases each of homozygous Southeast Asian ovalocytosis (SAO) and hemoglobin Constant Spring (Hb CS) were found. NIHF diagnosed in early gestation (<24 weeks) had a higher rate of chromosomal abnormalities and fetal demise. Intrauterine treatment was given in 18 cases, and 50% had successful live births.
Conclusion
Hb Bart’s disease was the most common cause of NIHF. SAO and Hb CS were associated with hydrops. NIHF in gestational age <24 weeks was associated with chromosomal abnormalities and fetal demise. Intrauterine treatment should be offered in selected cases.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Norton ME, Chauhan SP, Dashe JS. Society for maternal-fetal medicine (SMFM) clinical guideline #7: nonimmune hydrops fetalis. Am J Obstet Gynecol 2015;212:127–39.
Bellini C, Hennekam RC. Non-immune hydrops fetalis: a short review of etiology and pathophysiology. Am J Med Genet A 2012;158:597–605.
Bellini C, Hennekam RC, Fulcheri E, Rutigliani M, Morcaldi G, Boccardo F, et al. Etiology of nonimmune hydrops fetalis: a systematic review. Am J Med Genet A 2009;149:844–51.
Suwanrath-Kengpol C, Kor-anantakul O, Suntharasaj T, Leetanaporn R. Etiology and outcome of non-immune hydrops fetalis in southern Thailand. Gynecol Obstet Invest 2005;59:134–7.
Liao C, Wei J, Li Q, Li J, Li L, Li D. Nonimmune hydrops fetalis diagnosed during the second half of pregnancy in Southern China. Fetal Diagn Ther 2007;22:302–5.
Ratanasiri T, Komwilaisak R, Sittivech A, Kleebkeaw P, Seejorn K. Incidence, causes and pregnancy outcomes of hydrops fetalis at Srinagarind Hospital, 1996-2005: a 10-year review. J Med Assoc Thai 2009;92:594–9.
He S, Wang L, Pan P, Wei H, Meng D, Du J, et al. Etiology and perinatal outcome of nonimmune hydrops fetalis in southern China. AJP Rep. 2017;7:111–5.
Bellini C, Donarini G, Paladini D, Calevo MG, Bellini T, Ramenghi LA, et al. Etiology of non-immune hydrops fetalis: an update. Am J Med Genet A 2015;167:1082–8.
Moreno CA, Kanazawa T, Barini R, Nomura ML, Andrade KC, Gomes CP, et al. Non-immune hydrops fetalis: a prospective study of 53 cases. Am J Med Genet A 2013;161:3078–86.
Santo S, Mansour S, Thilaganathan B, Homfray T, Papageorghiou A, Calvert S, et al. Prenatal diagnosis of non-immune hydrops fetalis: what do we tell the parents? Prenat Diagn 2011;31:186–95.
Jatavan P, Chattipakorn N, Tongsong T. Fetal hemoglobin Bart’s hydrops fetalis: pathophysiology, prenatal diagnosis and possibility of intrauterine treatment. J Matern Fetal Neonatal Med 2018;31:946–57.
Laosombat V, Dissaneevate S, Wongchanchailert M, Satayasevanaa B. Neonatal anemia associated with Southeast Asian ovalocytosis. Int J Hematol 2005;82:201–5.
Ngouprommin L, Sae-Ung N, Fucharoen S, Fucharoen G, Sanchaisuriya K, Jetsrisuparb A. Genetic compound heterozygosity for Southeast Asian ovalocytosis and thalassemia in Thailand: prevalence and phenotypic analysis. Clin Genet 2014;85:198–200.
Charoenkwan P, Sirichotiyakul S, Chanprapaph P, Tongprasert F, Taweephol R, Sae-Tung R, et al. Anemia and hydrops in a fetus with homozygous hemoglobin constant spring. J Pediatr Hematol Oncol 2006;28:827–30.
Komvilaisak P, Komvilaisak R, Jetsrisuparb A, Wiangnon S, Jirapradittha J, Kiatchoosakun P, et al. Fetal anemia causing hydrops fetalis from an alpha-globin variant: homozygous hemoglobin constant spring. J Pediatr Hematol Oncol 2018;40:405–8.
Sirilert S, Charoenkwan P, Sirichotiyakul S, Tongprasert F, Srisupundit K, Luewan S, et al. Prenatal diagnosis and management of homozygous hemoglobin constant spring disease. J Perinatol 2019;39:927–33.
Palek J. Introduction: red blood cell membrane proteins, their genes and mutations. Semin Hematol 1993;30:1–3.
Maisonneuve E, Ben M’Barek I, Leblanc T, Da Costa L, Friszer S, Pernot F, et al. Managing the unusual causes of fetal anemia. Fetal Diagn Ther 2020;47:156–64.
Sparks TN, Thao K, Lianoglou BR, Boe NM, Bruce KG, Datkhaeva I, et al. Nonimmune hydrops fetalis: identifying the underlying genetic etiology. Genet Med 2019;21:1339–44.
Kosinski P, Krajewski P, Wielgos M, Jezela-Stanek. A nonimmune hydrops fetalis-prenatal diagnosis, genetic investigation, outcomes and literature review. J Clin Med. 2020;9:1789.
Sileo FG, Kulkarni A, Branescu I, Homfray T, Dempsey E, Mansour S, et al. Non-immune fetal hydrops: etiology and outcome according to gestational age at diagnosis. Ultrasound Obstet Gynecol 2020;56:416–21.
Sohan K, Carroll SG, De La Fuente S, Soothill P, Kyle P. Analysis of outcome in hydrops fetalis in relation to gestational age at diagnosis, cause and treatment. Acta Obstet Gynecol Scand 2001;80:726–30.
Heinonen S, Ryynanen M, Kirkinen P. Etiology and outcome of second trimester non-immunologic fetal hydrops. Acta Obstet Gynecol Scand 2000;79:15–8.
Yuan SM. Cardiac etiologies of hydrops fetalis. Z Geburtshilfe Neonatol 2017;221:67–72.
Moodley S, Sanatani S, Potts JE, Sandor GG. Postnatal outcome in patients with fetal tachycardia. Pediatr Cardiol 2013;34:81–7.
Kleinman CS, Copel JA. Electrophysiological principles and fetal antiarrhythmic therapy. Ultrasound Obstet Gynecol 1991;1:286–97.
Acknowledgements
The study was supported by the Prince of Songkla University, Songkhla, Thailand. The authors would like to thank Miss Jirawan Jayuphan from the Epidemiology Unit, Faculty of Medicine, Prince of Songkla University for her assistance in data analysis. We also would like to thank Mr. Dave Patterson from the International Affairs Office, Faculty of Medicine, Prince of Songkla University for English language editing.
Author information
Authors and Affiliations
Contributions
N.C. and W.M. designed, planned, and conducted the study. N.C., W.M., and C.S. contributed to the data analysis and to the first and final drafts of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
This study was performed in accordance with the Declaration of Helsinki and approval was obtained from the Human Research Ethics Committee of the Faculty of Medicine, Prince of Songkla University before the study began.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chainarong, N., Muangpaisarn, W. & Suwanrath, C. Etiology and outcome of non-immune hydrops fetalis in relation to gestational age at diagnosis and intrauterine treatment. J Perinatol 41, 2544–2548 (2021). https://doi.org/10.1038/s41372-021-01202-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-021-01202-7