Abstract
Objective
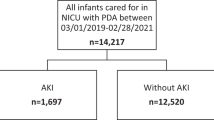
Investigate relationship between management of patent ductus arteriosus (PDA) and acute kidney injury (AKI) in very low birthweight neonates.
Study Design
Retrospective cohort study of neonates, <1500 g, admitted to 24 NICUs, 1/1/14 – 3/31/14. AKI diagnosed using the neonatal modified KDIGO definition; diagnosis and treatment of PDA extracted from the medical record. Demographics, clinical characteristics, and AKI stage compared using chi-square and analysis of variance. A general estimating equation logistic regression used to estimate adjusted odds ratios.
Results
Of 526 neonates with sufficient data to diagnose AKI, 157 (30%) had PDA (61 conservative management, 62 pharmacologic treatment only, 34 surgical ligation). In analyses adjusted for sex, birthweight, gestational age, caffeine, nephrotoxin exposure, vasopressor and mechanical ventilation use, with conservative management as reference, there were no differences among treatment cohorts in the odds of AKI.
Conclusion
The underlying physiology of PDA, not management strategy, may determine the likelihood of AKI in neonates <1500 g.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Elmas AT, Tabel Y, Ozdemir R. Risk factors and mortality rate in premature babies with acute kidney injury. J Clin Lab Anal. 2018;32:e22441.
Jetton JG, Guillet R, Askenazi DJ, Dill L, Jacobs J, Kent AL, et al. Assessment of Worldwide Acute Kidney Injury Epidemiology in Neonates: design of a retrospective cohort study. Front Pediatr. 2016;4:68.
Srinivasan N, Schwartz A, John E, Price R, Amin S. Acute kidney injury impairs postnatal renal adaptation and increases morbidity and mortality in very low-birth-weight infants. Am J Perinatol. 2018;35:39–47.
Weintraub AS, Connors J, Carey A, Blanco V, Green RS. The spectrum of onset of acute kidney injury in preterm infants less than 30 weeks gestation. J Perinatol. 2016;36:47–480.
Velazquez DM, Reidy KJ, Sharma M, Kim M, Vega M, Havranek T. The effect of hemodynamically significant patent ductus arteriosus on acute kidney injury and systemic hypertension in extremely low gestational age newborns. J Matern Fetal Neonatal Med. 2019;32:3209–14.
Bomelburg T, Jorch G. Abnormal blood flow patterns in renal arteries of small preterm infants with patent ductus arteriosus detected by Doppler ultrasonography. Eur J Pediatr. 1989;148:660–4.
Aygün A, Poryo M, Wagenpfeil G, Wissing A, Ebrahimi-Fakhari D, Zemlin M, et al. Birth weight, Apgar scores and gentamicin were associated with acute kidney injuries in VLBW neonates requiring treatment for patent ductus arteriosus. Acta Paediatr. 2019;108:645–53.
Majed B, Bateman DA, Uy N, Lin F. Patent ductus arteriosus is associated with acute kidney injury in the preterm infant. Pediatr Nephrol. 2019;34:1129–39.
Hammerman C, Shchors I, Jacobson S, Schimmel MS, Bromiker R, Kaplan M, et al. Ibuprofen versus continuous indomethacin in premature neonates with patent ductus arteriosus: is the difference in the mode of administration? Pediatr Res. 2008;64:291–7.
Jetton JG, Boohaker LJ, Sethi SK, Wazir S, Rohatgi S, Soranno DE, et al. Incidence and outcomes of neonatal acute kidney injury (AWAKEN): a multicenter, multinational, observational cohort study. Lancet Child Adolesc Health. 2017;1:184–94.
Selewski DT, Charlton JR, Jetton JG, Guillet R, Mhanna MJ, Askenazi DJ, et al. Neonatal acute kidney injury. Pediatrics. 2015;136:e463–e473.
Radicioni M, Bini V, Campus GM, Camerini PG. Terlipressin-induced modifications of Doppler ultrasound signals of systemic arteries in preterm infants with vasoactive-resistant patent ductus arteriosus: a pilot study. J Clin Ultrasound. 2018;46:202–8.
Bonsante F, Ramful D, Binquet C, Samperiz S, Daniel S, Gouyon JB, et al. Low renal oxygen saturation at near-infrared spectroscopy on the first day of life is associated with developing acute kidney injury in very preterm infants. Neonatology. 2019;115:198–204.
Guignard JP. The adverse renal effects of prostaglandin-synthesis inhibitors in the newborn rabbit. Semin Perinatol. 2002;26:398–405.
Van-Bel F, Van-Zoeren D, Schipper J, Guit GL, Baan J. Effect of indomethacin on superior mesenteric artery blood flow velocity in preterm infants. J Pediatr. 1990;116:965–70.
Van-Bel F, Guit GL, Schipper J, van-de-Bor M, Baan J. Indomethacin-induced changes in renal blood flow velocity waveform in premature infants investigated with color Doppler imaging. J Pediatr. 1991;118:621–6.
Bensman A. Non-steroidal anti-inflammatory drugs (NSAIDs) systemic use: the risk of renal failure. Front Pediatr. 2020;7:517.
Kent AL, Brown L, Broom M, Broomfield A, Dahlstrom JE. Increased urinary podocytes following indomethacin suggests drug-induced glomerular injury. Pediatr Nephrol. 2012;27:1111–7.
Sellmer A, Bech BH, Bjerre JV, Schmidt MR, Hjortdal VE, Esberg G, et al. Urinary neutrophil gelatinase-associated lipocalin in the evaluation of patent ductus arteriosus and AKI in very preterm neonates: a cohort study. BMC Pediatr. 2017;17:7.
Acknowledgements
The authors thank all the members of the Neonatal Kidney Collaborative who participated in the AWAKEN study: University of Alabama, Birmingham: David Askenazi, MD; N. Ambalavanan, MD; Russell Griffin, PhD; Cincinnati Children’s Hospital: Stuart Goldstein, MD; Amy Nathan, MD; James Greenberg, MD; Canberra Hospital: Alison Kent, MD (currently at the University of Rochester); Jeffrey Fletcher, MD; Farah Sethna, MD; Children’s Hospital of Colorado: Danielle Soranno, MD; Jason Gien, MD; Katja Gist, MD; Children’s Hospital at Montefiore/Albert Einstein: Mamta Fuloria, MD; Kim Reidy, MD; Frederick Kastel, MD; Natalie Uy, MD; Children’s National Medical Center: Mary Revenis, MD; Sofia Perrazo, MD; Shantanu Rastogi, MD; Golisano Children’s Hospital University of Rochester: George Schwartz, MD; Carl T. D’Angio, MD; Ronnie Guillet, MD, PhD; Erin Rademacher, MD; Ahmed El Samra, MD (currently Union Hospital, Terre Haute); Ayesa Mian, MD; Maimonides Medical Center: Juan Kupferman, MD; Alok Bhutada, MD; McGill University: Michael Zappitelli, MD; Pia Wintermark, MD; Medanta, Medicity The Cradle: Sanjay Wazir, MD; Sidharth Sethi, MD; Sandeep Dubey, MD; Metrohealth Medical Center: Maroun Mhanna, MD; Deepak Kumar, MD; Rupesh Raina, MD; Nationwide Children’s Hospital: Susan Ingraham, MD; Arwa Nada, MD; Elizabeth Bonachea, MD; Stonybrook University: Richard Fine, MD; Robert Woroniecki, MD; Shanthy Sridhar, MD; Texas Children’s Hospital: Ayse Ariken, MD; Christopher Rhee, MD; Tufts Medical Center: Lawrence Milner, MD; Alexandra Smith, MD; Julie Nicoletta, MD; University of British Columbia: Cherry Mammen, MD; Avash Jeet Singh, MD; Anne Synnes, MD; University of Iowa: Jennifer Jetton, MD; Tarah Colaizy, MD; Jonathan Klein, MD; Patrick Brophy (currently University of Rochester); University of Kentucky: Aftab Chishti, MD; Mina Hanna, MD; University of Miami: Carolyn Abitbol, MD; Marissa Defreitas, MD; Shahnaz Duara, MD; Salih Yasin, MD; University of Michigan: David Selewski, MD (currently Medical University of South Carolina); Subrata Sarker, MD; University of New Mexico: Craig Wong, MD; A. Staples, MD; Robin Ohls, MD; Catherine Joseph, MD (currently Texas Children’s Hospital); Tara Dupont, MD (currently University of Utah); University of Virginia: Jennifer Charlton, MD; Jonathan Swanson, MD; Matthew Harer (currently University of Wisconsin); Patricio Ray, MD; University of Washington: Sangeeta Hingorani, MD; Christine Hu, MD; Sandra Juul, MD.
The Neonatal Kidney Collaborative
David Askenazi5; N. Ambalavanan5; Russell Griffin5; Stuart Goldstein6; Amy Nathan6; James Greenberg6; Alison Kent7; Jeffrey Fletcher7; Farah Sethna7; Danielle Soranno8; Jason Gien8; Katja Gist8; Mamta Fuloria9; Kim Reidy9; Frederick Kastel9; Natalie Uy9; Mary Revenis10; Sofia Perrazo10; Shantanu Rastogi10; George Schwartz11; Carl T. D’Angio11; Ronnie Guillet11; Erin Rademacher11; Ahmed El Samra11,28; Ayesa Mian11; Juan Kupferman12; Alok Bhutada12; Michael Zappitelli13; Pia Wintermark13; Sanjay Wazir14; Sidharth Sethi14; Sandeep Dubey14; Maroun Mhanna15,29; Deepak Kumar15; Rupesh Raina15; Susan Ingraham16; Arwa Nada16; Elizabeth Bonachea16; Richard Fine17; Robert Woroniecki17; Shanthy Sridhar17; Ayse Ariken18; Christopher Rhee18; Lawrence Milner19; Alexandra Smith19; Julie Nicoletta19; Cherry Mammen20; Avash Jeet Singh20; Anne Synnes20; Jennifer Jetton21; Tarah Colaizy21; Jonathan Klein21; Patrick Brophy21,30; Aftab Chishti22; Mina Hanna22; Carolyn Abitbol23; Marissa Defreitas23; Shahnaz Duara23; Salih Yasin23; David Selewski24,31; Subrata Sarker24; Craig Wong25; A. Staples25; Robin Ohls25; Catherine Joseph25,32; Tara Dupont25,33; Jennifer Charlton26; Jonathan Swanson26; Matthew Harer26,34; Patricio Ray26; Sangeeta Hingorani27; Christine Hu27; Sandra Juul27.
Author information
Authors and Affiliations
Consortia
Contributions
RGu designed the study, acquired data, drafted the manuscript and approved the final version. DS acquired data, contributed to the design of the study, edited the manuscript and approved the final version. RGr performed the statistical analyses, edited the manuscript and approved the final version. SR acquired data, edited the manuscript and approved the final version. DA contributed to the design of the study, edited the manuscript and approved the final version. CD contributed to the design of the study, edited the manuscript and approved the final version.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Members of the Neonatal Kidney Collaborative are listed below Acknowledgements.
Rights and permissions
About this article
Cite this article
Guillet, R., Selewski, D.T., Griffin, R. et al. Relationship of patent ductus arteriosus management with neonatal AKI. J Perinatol 41, 1441–1447 (2021). https://doi.org/10.1038/s41372-021-01054-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-021-01054-1
This article is cited by
-
Indomethacin patent ductus arteriosus prophylaxis in the modern era: renal implications
Journal of Perinatology (2023)
-
Neonatal acute kidney injury during indomethacin therapy: does it predict ductal closure?
Journal of Nephrology (2023)
-
Costs associated with acute kidney injury in critically Ill neonates with patent Ductus arteriosus: pediatric health information system (PHIS) analysis
Journal of Perinatology (2022)
-
When the progresses in neonatology lead to severe congenital nephron deficit: is there a pilot in the NICU?
Pediatric Nephrology (2022)
-
Recent Advances in Acute Kidney Injury in Preterm Infants
Current Pediatrics Reports (2022)