Abstract
Objective
A post hoc appraisal of the PDA RCT to assess the relationship between early patent ductus arteriosus (PDA) shunt elimination and chronic lung disease or death (CLD/Death).
Study design
Infants <29 weeks were divided into four groups: intervention arm in whom PDA closure was achieved (n = 17); intervention arm in whom PDA closure was not achieved (n = 13); placebo arm (n = 30); low risk infants (n = 13). The main outcome measure was CLD/Death.
Results
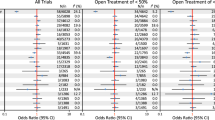
The rates of CLD/Death were lower in the Intervention Success Group (29%) when compared to the Intervention Failure Group (85%) or the Placebo Group (60%, all p < 0.05). There was no difference in CLD/Death between the Intervention Success and Low Risk Groups (8%, p > 0.05). A persistent PDA beyond Day 8 was associated with CLD/Death (aOR 6.5 [1.7–25.5]).
Conclusions
Early shunt elimination in preterm infants with a PDA may reduce respiratory morbidity when compared to infants with prolonged shunt exposure.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Availability of data and materials
Data will be kept confidential in compliance with the European General Data Protection Regulation.
References
El-Khuffash A, James AT, Corcoran JD, Dicker P, Franklin O, Elsayed YN, et al. A patent ductus arteriosus severity score predicts chronic lung disease or death before discharge. J Pediatr. 2015;167:1354–1361 e1352.
Sellmer A, Bjerre JV, Schmidt MR, McNamara PJ, Hjortdal VE, Host B, et al. Morbidity and mortality in preterm neonates with patent ductus arteriosus on day 3. Arch Dis Child Fetal Neonatal Ed. 2013;98:F505–F510.
Fink D, El-Khuffash A, McNamara PJ, Nitzan I, Hammerman C. Tale of two patent ductus arteriosus severity scores: similarities and differences. Am J Perinatol. 2018;35:55–58.
Benitz WE. Treatment of persistent patent ductus arteriosus in preterm infants: time to accept the null hypothesis? J Perinatol. 2010;30:241–52.
El-Khuffash A, Levy PT, Gorenflo M, Frantz ID III. The definition of a hemodynamically significant ductus arteriosus. Pediatr Res. 2019;85:740–1.
Smith A, El-Khuffash AF. Defining “haemodynamic significance” of the patent ductus arteriosus: do we have all the answers? Neonatology. 2020;117:225–32.
El-Khuffash A, Bussmann N, Breatnach CR, Smith A, Tully E, Griffin J, et al. A pilot randomized controlled trial of early targeted patent ductus arteriosus treatment using a Risk Based Severity Score (The PDA RCT). J Pediatr. 2021;229:127–33.
Bancalari E, Claure N. Definitions and diagnostic criteria for bronchopulmonary dysplasia. Semin Perinatol. 2006;30:164–70.
Papile LA, Burstein J, Burstein R, Koffler H. Incidence and evolution of subependymal and intraventricular hemorrhage: a study of infants with birth weights less than 1,500 gm. J Pediatr. 1978;92:529–34.
Bell MJ. Neonatal necrotizing enterocolitis. N. Engl J Med. 1978;298:281–2.
de Boode WP, Singh Y, Gupta S, Austin T, Bohlin K, Dempsey E, et al. Recommendations for neonatologist performed echocardiography in Europe: Consensus Statement endorsed by European Society for Paediatric Research (ESPR) and European Society for Neonatology (ESN). Pediatr Res. 2016;80:465–71.
Nestaas E, Schubert U, de Boode WP, El-Khuffash A.European Special Interest Group “Neonatologist Performed Echocardiography" Tissue Doppler velocity imaging and event timings in neonates: a guide to image acquisition, measurement, interpretation, and reference values. Pediatr Res. 2018;84(Suppl 1):S18–S29.
van Laere D, van Overmeire B, Gupta S, El-Khuffash A, Savoia M, McNamara PJ, et al. Application of NPE in the assessment of a patent ductus arteriosus. Pediatr Res. 2018;84(Suppl 1):S46–S56.
Groves AM, Singh Y, Dempsey E, Molnar Z, Austin T, El-Khuffash A, et al. Introduction to neonatologist-performed echocardiography. Pediatr Res. 2018;84(Suppl 1):S1–S12.
El-Khuffash A, Schubert U, Levy PT, Nestaas E, de Boode WP.European Special Interest Group “Neonatologist Performed Echocardiography Deformation imaging and rotational mechanics in neonates: a guide to image acquisition, measurement, interpretation, and reference values. Pediatr Res. 2018;84(Suppl 1):S30–S45.
Smith A, Maguire M, Livingstone V, Dempsey EM. Peak systolic to end diastolic flow velocity ratio is associated with ductal patency in infants below 32 weeks of gestation. Arch Dis Child Fetal Neonatal Ed. 2015;100:F132–F136.
Evans N. Preterm patent ductus arteriosus: a continuing conundrum for the neonatologist? Semin Fetal Neonatal Med. 2015;20:272–7.
Chang LY, McCurnin D, Yoder B, Shaul PW, Clyman RI. Ductus arteriosus ligation and alveolar growth in preterm baboons with a patent ductus arteriosus. Pediatr Res. 2008;63:299–302.
Kluckow M, Jeffery M, Gill A, Evans N. A randomised placebo-controlled trial of early treatment of the patent ductus arteriosus. Arch Dis Child Fetal Neonatal Ed. 2014;99:F99–F104.
Clyman RI, Liebowitz M, Kaempf J, Erdeve O, Bulbul A, Hakansson S, et al. PDA-TOLERATE trial: an exploratory randomized controlled trial of treatment of moderate-to-large patent ductus arteriosus at 1 week of age. J Pediatr. 2019;205:41–48 e46.
Liebowitz M, Katheria A, Sauberan J, Singh J, Nelson K, Hassinger DC, et al. Lack of equipoise in the PDA-TOLERATE trial: a comparison of eligible infants enrolled in the trial and those treated outside the trial. J Pediatr. 2019;213:222–226 e222.
Mitra S, Florez ID, Tamayo ME, Mbuagbaw L, Vanniyasingam T, Veroniki AA, et al. Association of placebo, indomethacin, ibuprofen, and acetaminophen with closure of hemodynamically significant patent ductus arteriosus in preterm infants: a systematic review and meta-analysis. JAMA. 2018;319:1221–38.
Lago P, Salvadori S, Opocher F, Ricato S, Chiandetti L, Frigo AC. Continuous infusion of ibuprofen for treatment of patent ductus arteriosus in very low birth weight infants. Neonatology. 2014;105:46–54.
Mitra S, Scrivens A, von Kursell AM, Disher T. Early treatment versus expectant management of hemodynamically significant patent ductus arteriosus for preterm infants. Cochrane Datab Syst Rev. 2020;12:CD013278.
Funding
This study was funded by a research grant from the Temple Street Hospital Foundation (Ref: RPAC 16-03). The National Children’s Research Centre funded Ph.D. fees associated with this project.
Author information
Authors and Affiliations
Contributions
AEL-K and PMcN devised the study protocol and analysis plan, which was approved by all the authors, and provided oversight for the conduct of the trial. NB recruited the patients, performed the blinded echocardiography analysis and data collection. CB and AS assisted in patient recruitment and echocardiography studies. NMcC provided expert neonatal oversight. BC provided oversight of drug preparation and administration. OF provided cardiology expertise. All the listed authors made substantial contributions to either the conception or design of the work, or the acquisition, analysis, or interpretation of data for the work. NB wrote the first draft but all the listed authors revised it critically for important intellectual content, approve the final version of the manuscript and agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interest.
Ethical approval and consent to participate
Ethical approval was obtained from our institutional ethics board (The National Maternity Hospital, Reference Number: EC 09.2016) and written informed consent was obtained from all parents. The study was performed in accordance with the Declaration of Helsinki.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Trial Registration: The trial was registered with the ISRCTN (13281214) and the European Union Drug Regulating Authorities Clinical Trials Database (2015-004526-33).
Supplementary information
Rights and permissions
About this article
Cite this article
Bussmann, N., Smith, A., Breatnach, C.R. et al. Patent ductus arteriosus shunt elimination results in a reduction in adverse outcomes: a post hoc analysis of the PDA RCT cohort. J Perinatol 41, 1134–1141 (2021). https://doi.org/10.1038/s41372-021-01002-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-021-01002-z
This article is cited by
-
Clinical and echocardiography predictors of response to first-line acetaminophen treatment in preterm infants with hemodynamically significant patent ductus arteriosus
Journal of Perinatology (2024)
-
Hospital variation in neonatal echocardiography among very preterm infants at US children’s hospitals
Journal of Perinatology (2023)
-
Correspondence: “Patent ductus arteriosus shunt elimination results in a reduction in adverse outcomes: a post hoc analysis of the PDA RCT cohort”
Journal of Perinatology (2022)
-
Reply to correspondence
Journal of Perinatology (2022)
-
The patent ductus arteriosus management debate: it’s not over yet
Journal of Perinatology (2021)