Abstract
Objective
To determine the incidence of mental health symptoms in military families after prolonged NICU admission.
Study design
Prospective cohort study of military-affiliated NICU parents participating in serial electronic surveys, which included validated screening tools for acute stress (ASD), post-traumatic stress (PTSD), and depression disorders.
Results
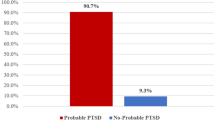
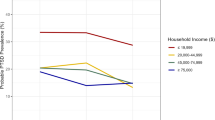
Among 106 military parents surveyed after NICU admission, 24.5% screened positive for ASD and 28.3% for depression. 77 (72.6%) parents continued participation beyond discharge, with 7.8% screening positive for PTSD and 15.6% for late depression. Positive ASD correlated with later symptoms of PTSD (OR 8.4 [2.4–30]) and early depression with both PTSD symptoms (OR 5.7 [1.7–18.8]) and late depression (OR 8.4 [2.4–30]) after discharge. Secondary analysis determined these findings were independent of deployment and other military related factors.
Conclusion
This study highlights the potential mental health burden experienced by military-affiliated NICU parents. Early ASD and depression screening may identify parents at risk for mental health symptoms after discharge.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Lefkowitz DS, Baxt C, Evans JR. Prevalence and correlates of posttraumatic stress and postpartum depression in parents of infants in the Neonatal Intensive Care Unit (NICU). J Clin Psychol Med Settings. 2010;17:230–7.
Joseph RA, Mackley AB, Davis CG, Spear ML, Locke RG. Stress in fathers of surgical neonatal intensive care unit babies. Adv Neonatal Care. 2007;7:321–5.
Miles MS, Holditch-Davis D. Parenting the prematurely born child: pathways of influence. Semin Perinatol. 1997;21:254–66.
Greene MM, Rossman B, Meier P, Patra K. Elevated maternal anxiety in the NICU predicts worse fine motor outcome in VLBW infants. Early Hum Dev. 2018;116:33–9.
Greene MM, Rossman B, Patra K, Kratovil AL, Janes JE, Meier PP. Depression, anxiety, and perinatal-specific posttraumatic distress in mothers of very low birth weight infants in the neonatal intensive care unit. J Dev Behav Pediatr. 2015;36:362–70.
Roque ATF, Lasiuk GC, Radunz V, Hegadoren K. Scoping review of the mental health of parents of infants in the NICU. J Obstet Gynecol Neonatal Nurs. 2017;46:576–87.
Aftyka A, Rybojad B, Rozalska-Walaszek I, Rzonca P, Humeniuk E. Post-traumatic stress disorder in parents of children hospitalized in the neonatal intensive care unit (NICU): medical and demographic risk factors. Psychiatr Danubina. 2014;26:347–52.
Feeley N, Zelkowitz P, Cormier C, Charbonneau L, Lacroix A, Papageorgiou A. Posttraumatic stress among mothers of very low birthweight infants at 6 months after discharge from the neonatal intensive care unit. Appl Nurs Res. 2011;24:114–7.
Kim WJ, Lee E, Kim KR, Namkoong K, Park ES, Rha DW. Progress of PTSD symptoms following birth: a prospective study in mothers of high-risk infants. J Perinatol. 2015;35:575–9.
Shaw RJ, Bernard RS, Deblois T, Ikuta LM, Ginzburg K, Koopman C. The relationship between acute stress disorder and posttraumatic stress disorder in the neonatal intensive care unit. Psychosomatics. 2009;50:131–7.
American Psychiatric Association. DSM-5 Task Force. Diagnostic and statistical manual of mental disorders: DSM-5. 5th edn. American Psychiatric Association; 2013.
Armour C, Mullerova J, Elhai JD. A systematic literature review of PTSD’s latent structure in the Diagnostic and Statistical Manual of Mental Disorders: DSM-IV to DSM-5. Clin Psychol Rev. 2016;44:60–74.
Zerach G, Elsayag A, Shefer S, Gabis L. Long-term maternal stress and post-traumatic stress symptoms related to developmental outcome of extremely premature infants. Stress Health. 2015;31:204–13.
Aftyka A, Rybojad B, Rosa W, Wrobel A, Karakula-Juchnowicz H. Risk factors for the development of post-traumatic stress disorder and coping strategies in mothers and fathers following infant hospitalisation in the neonatal intensive care unit. J Clin Nurs. 2017;26:4436–45.
Shaw RJ, Bernard RS, Storfer-Isser A, Rhine W, Horwitz SM. Parental coping in the neonatal intensive care unit. J Clin Psychol Med Settings. 2013;20:135–42.
Schecter R, Pham T, Hua A, Spinazzola R, Sonnenklar J, Li D, et al. Prevalence and longevity of PTSD symptoms among parents of NICU infants analyzed across gestational age categories. Clin Pediatr. 2020;59:163–9.
Bellini S. NICU families and PTSD: handle with care. Nurs Women’s Health. 2009;13:422–6.
Malin KJ, Johnson TS, McAndrew S, Westerdahl J, Leuthner J, Lagatta J. Infant illness severity and perinatal post-traumatic stress disorder after discharge from the neonatal intensive care unit. Early Hum Dev. 2019;140:104930.
Xue C, Ge Y, Tang B, Liu Y, Kang P, Wang M, et al. A meta-analysis of risk factors for combat-related PTSD among military personnel and veterans. PLoS ONE. 2015;10:e0120270.
Chang HP, Chen JY, Huang YH, Yeh CJ, Huang JY, Su PH, et al. Factors associated with post-traumatic symptoms in mothers of preterm infants. Arch Psychiatr Nurs. 2016;30:96–101.
Cardena E, Koopman C, Classen C, Waelde LC, Spiegel D. Psychometric properties of the Stanford Acute Stress Reaction Questionnaire (SASRQ): a valid and reliable measure of acute stress. J Trauma Stress. 2000;13:719–34.
Classen C, Koopman C, Hales R, Spiegel D. Acute stress disorder as a predictor of posttraumatic stress symptoms. Am J Psychiatry. 1998;155:620–4.
Grieger TA, Staab JP, Cardena E, McCarroll JE, Brandt GT, Fullerton CS, et al. Acute stress disorder and subsequent post-traumatic stress disorder in a group of exposed disaster workers. Depress Anxiety. 2000;11:183–4.
Kroenke K, Spitzer RL, Williams JB. The Patient Health Questionnaire-2: validity of a two-item depression screener. Med Care. 2003;41:1284–92.
Bovin MJ, Marx BP, Weathers FW, Gallagher MW, Rodriguez P, Schnurr PP, et al. Psychometric properties of the PTSD Checklist for Diagnostic and Statistical Manual of Mental Disorders-Fifth Edition (PCL-5) in veterans. Psychol Assess. 2016;28:1379–91.
Weathers FW, Bovin MJ, Lee DJ, Sloan DM, Schnurr PP, Kaloupek DG, et al. The Clinician-Administered PTSD Scale for DSM-5 (CAPS-5): development and initial psychometric evaluation in military veterans. Psychol Assess. 2018;30:383–95.
Ashbaugh AR, Houle-Johnson S, Herbert C, El-Hage W, Brunet A. Psychometric validation of the English and French Versions of the oosttraumatic stress disorder checklist for DSM-5 (PCL-5). PLoS ONE. 2016;11:e0161645.
Vanderbilt D, Bushley T, Young R, Frank DA. Acute posttraumatic stress symptoms among urban mothers with newborns in the neonatal intensive care unit: a preliminary study. J Dev. Behav Pediatr. 2009;30:50–6.
Shaw RJ, Deblois T, Ikuta L, Ginzburg K, Fleisher B, Koopman C. Acute stress disorder among parents of infants in the neonatal intensive care nursery. Psychosomatics. 2006;47:206–12.
Jubinville J, Newburn-Cook C, Hegadoren K, Lacaze-Masmonteil T. Symptoms of acute stress disorder in mothers of premature infants. Adv Neonatal Care. 2012;12:246–53.
Gangi S, Dente D, Bacchio E, Giampietro S, Terrin G, De Curtis M. Posttraumatic stress disorder in parents of premature birth neonates. Procedia Soc Behav Sci. 2013;82:882–5.
Staver MA, Moore TA, Hanna KM. Maternal distress in the neonatal intensive care unit: a concept analysis. Adv Neonatal Care. 2019;19:394–401.
Funding source
The 59th Medical Wing (Joint Base San Antonio, Lackland, TX) and Brooke Army Medical Center Auxiliary Group provided funding for this study.
Author information
Authors and Affiliations
Contributions
JA helped conceptualize the study, drafted the IRB protocol, consented parents for enrollment, oversaw data collection, worked directly with the statistician, and drafted the manuscript. SJ helped conceptualize the study, participated in survey development and administration, collected data, and contributed to the drafting and editing of the manuscript. SD, AF, DB, and CG enrolled participants, collected data, and contributed to drafting and editing of the manuscript. NC initially conceptualized the study, helped extensively with overall study direction, patient enrollment, data collection, statistical analysis, as well as provided significant input on the drafting, editing, and formatting of the final manuscript. All authors approve the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Ethics approval
Informed consent was obtained from all participants. The study was approved by the Institutional Review Board of Brooke Army Medical Center, Fort Sam Houston, TX (Protocol ID Number: C.2017.206d). The study was performed in accordance with the Declaration of Helsinki.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Anchan, J., Jones, S., Aden, J. et al. A different kind of battle: the effects of NICU admission on military parent mental health. J Perinatol 41, 2038–2047 (2021). https://doi.org/10.1038/s41372-021-00994-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-021-00994-y