Abstract
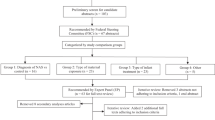
Kratom is a legal, widely available substance that contains opioid agonist alkaloids. Due to the marketing of kratom as an opioid alternative for treatment of pain, anxiety, depression, or to reduce opioid withdrawal symptoms, the use of kratom has increased among persons in the USA including pregnant women. This systematic review of the peer-reviewed literature regarding kratom in relation to maternal and infant outcomes resulted in analysis of six case reports of prenatal kratom exposure. Maternal and infant withdrawal from kratom exposure was described in each case, resulting in pharmacologic treatment for both mothers and infants.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Change history
28 September 2021
A Correction to this paper has been published: https://doi.org/10.1038/s41372-021-01212-5
References
Khey DN, Stogner JM, Miller BL. Emerging trends in drug use and distribution. New York, NY: Springer; 2014.
O’Neill-Dee C, Spiller HA, Casavant MJ, Kistamgari S, Chounthirath T, Smith TA. Natural psychoactive substance-related exposures reported to United States poison control centers, 2000–2017. Clin Toxicol. 2019. https://doi.org/10.1080/15563650.2019.1688341.
National Center for Biotechnology Information. Mitragynine. PUBCHEM database. National Center for Biotechnology Information. 2021. https://pubchem.ncbi.nlm.nih.gov/compound/Mitragynine.
Raffa RB, Pergolizzi JV, Taylor R, Ossipov MH. NEMA Research Group. Natur’s first “atypical opioid”: kratom and mitragynines. J Clin Pharmacol. 2018;43:437–41. https://doi.org/10.1111/jcpt.12676.
Takayama H. Chemistry and pharmacology of analgesic indole alkaloids from the rubiaceous plant, Mitragyna speciosa. Chem Pharm Bull. 2004;52:916–28.
Griffin OH III, Daniels JA, Gardner EA. Do you get what you paid for? An examination of products advertised as kratom. J Psychoactive Drugs. 2016;1–6. https://doi.org/10.1080/02791072.2016.1229876.
Lydecker AG, Sharma A, McCurdy CR, Avery BA, Babu KM, Boyer EW. Suspected adulteration of commercial kratom products with 7-hydro-xymitragynine. J Med Toxicol. 2016:12:341–9. https://doi.org/10.1007/s13181-016-0588-y.
Warner ML, Kaufman NC, Grundmann O. The pharmacology and toxicology of kratom: from traditional herb to drug of abuse. Int J Leg Med. 2016;130:127–38. https://doi.org/10.1007/s00414-015-1279-y.
Lee J, Park J, Go A, Moon H, Kim S, Jung S, et al. Urine multi-drug screening with GC-MS or LC–MS-MS using SALLE-hybrid PPT/SPE. J Anal Toxicol. 2018;42:617–24. https://doi.org/10.1093/jat/bky032.
Sharma A, Kamble SH, Leon F, Chear HJY, King TL, Bethold EC, et al. Simultaneous quantification of ten key kratom alkaloids in Mitragyna speciose lef actrates and commercial products by untra-performance liquid chromatography-tandem mass spectrometry. Drug Test Anal. 2019;11:8.
Garcia-Romeu A, Cox DJ, Smith KE, Dunn KE, Griffiths RR. Kratom (Mitragyna speciose): user demographics, use patterns and implications for the opioid epidemic. Drug Alcohol Depend. 2020;208. https://doi.org/10.1016/j.drugalcdep.2020.107849.
Singh D, Chear JY, Narayanan S, Leon F, Sharma A, McCurdy R, et al. Patterns and reasons for kratom (Mitragyna speciose) use among current and former opioid poly-drug users. J Ethnopharmacol. 2020;249. https://doi.org/10.1016/j.jep.219.112462.
Smith K, Lawson T. Prevalence and motivations for kratom use in a sample of substance users enrolled in a residential treatment program. Drug Alcohol Depend. 2017;180:340–8. https://doi.org/10.1016/j.drugalcdep.2017.08.034.
Boyer EW, Baby KM, Adkins JE, McCurdy CR, Halpern JH. Self-treatment of opioid withdrawal using kratom (Mitragyna speciose Korth). Addiction. 2008;103:2145–57. https://doi.org/10.1111/j.1360-0443.2008.02209.
Grundmann O. Patterns of kratom use and health impact in the US—results from an online survey. Drug Alcohol Depend. 2017;176:63–70. https://doi.org/10.1016/j.drugalcdep.2017.03.007.
Smith KE, Lawson T. Prevalence and motivations of kratom use in a sample of substance users enrolled in a residential treatment program. Drug Alcohol Depend. 2017;180:340–8. https://doi.org/10.1016/j.drugalcdep.2017.08.034.
Coe MA, Pilllitteri JL, Sembower MA, Gerlach KK, Henningfield JE. Kratom as a substitute for opioids: results from an online survey. Drug Alcohol Depend. 2019;202:24–32. https://doi.org/10.1016/j.drugalcdep.2019.05.005.
Saref A, Suraya S, Singh D, Grundmann O, Narayanan S, Swogger MT, et al. Self-reported prevalence and severity of opioid and kratom (Mitragyna speciose Korth) side effects. J Ethnopharmacol. 2019;238. https://doi.org/10.1016/j.jep.2019.111876.
US Food and Drug Administration. Statement from FDA Commissioner Scott Gottlieb, M.D., on the agency’s scientific evidence on the presence of opioid compounds in kratom, underscoring its potential for abuse. US Food and Drug Administration. 2018. https://www.Fda.gov/NewsEvents/Newsroom/PressAnnouncements/ucm595622.
FDA. Statement from FDA Commissioner Scott Gottlieb, M.D., on new warning letters FDA is issuing to companies marketing kratom with unproven medical claims; and the agency’s ongoing concerns about kratom. FDA; 2018. https://www.fda.gov/news-events/press-announcements/statement-fda-commissioner-scott-gottlieb-md-new-warning-letters-fda-issuing-companies-marketing.
U.S. Food and Drug Administration. FDA investigates multistate outbreak of salmonella infections linked to products reported to contain kratom. U.S. Food and Drug Administration. 2018. https://www.fda.gov/Food/RecallsOutbreaksEmergencies/Outbreaks/ucm597265.htm.
Prozioleck WC, Avery BA, Boyer EW, Grundmann O, Henningfield JE, Kruegel AC, et al. Kratom policy: the challenge of balancing therapeutic potential with public safety. Int J Drug Policy. 2019;70:70–7. https://doi.org/10.1016/j.drugpo.2019.05.003.
Davidson L, Rawat M, Stojanovski S, Chandrasekharan P. Natural drugs, not so natural effects: neonatal abstinence syndrome secondary to ‘kratom’. J Neonatal-Perinat Med. 2019;12:109–12. https://doi.org/10.3233/NPM-1863.
Mackay L, Abrahams R. Novel case of maternal and neonatal kratom dependence and withdrawal. Can Fam Phys. 2018;64:121–2.
Murthy P, Clark D. An usual cause for neonatal abstinence syndrome. Pediatr Child Health. 2019;24:12–14. https://doi.org/10.1093/pch/pxy084.
Eldridge WB, Foster C, Wyble L. Neonatal abstinence syndrome due to maternal kratom use. Pediatrics. 2018;142:e20181839. https://doi.org/10.1542/peds.2018-1839.
Smid MC, Charles JE, Gordon AJ, Wright TE. Opioids case report use of kratom, an opioid-like traditional her, in pregnancy. Obstet Gynecol. 2018;132:926–8. https://doi.org/10.1097/aog.0000000000002871.
Loudin S, Murray S, Prunty L, Davies T, Evans J, Werthammer J. An atypical withdrawal syndrome in neonates prenatally exposed to gabapentin and opioids. J Pediatr. 2017;181:286–8.
Bastiaens L, Galus J, Mazur C. Abuse of gabapentin is associated with opioid addiction. Psychiatr Q. 2016;87:763–7. https://doi.org/10.1007/s11126-016-9421-7.
Farah T. Fears about kratom use during pregnancy are overblown. 2018. https://filtermag.org/fears-kratom-pregnancy-overblown/.
Wright ME, Temples HS. I do love my baby: stories of mothers with addiction and recovery. Columbia, SC: Amazon KDP publishing; 2019.
Saingam D, Assanangkornchai S, Geater AF, Lerkiatbundit S. Validation of krathom (Mitragyna speciose Korth.) dependence scale (KDS): a dependence screen for internationally emerging psychoactive substance. Subst Abus. 2014;35:276–83. https://doi.org/10.1080/08897077.2014.924464.
Acknowledgements
The project was partially supported by the Clemson Creative Inquiry Program.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: Madison Sherbondy has been added to the author list.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wright, M.E., Ginsberg, C., Parkison, A.M. et al. Outcomes of mothers and newborns to prenatal exposure to kratom: a systematic review. J Perinatol 41, 1236–1243 (2021). https://doi.org/10.1038/s41372-021-00952-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-021-00952-8
This article is cited by
-
Receptor Selectivity and Therapeutic Potential of Kratom in Substance Use Disorders
Current Addiction Reports (2023)