Abstract
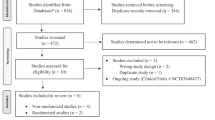
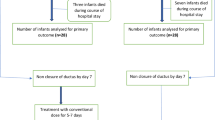
Objective was to compare the rate of successful treatment of hsPDA based on echocardiogram criteria after use of IV acetaminophen or IV indomethacin in very low-birthweight infants. The study was a multi-center, randomized controlled trial. Infants born prior to 32 weeks with birthweight ≤ 1500 g were included if PDA treatment was indicated within the 21 days after birth. hsPDA was defined by strict echocardiogram criteria. Eligible infants were randomized to treatment with either IV acetaminophen or IV indomethacin. Of 86 eligible infants, 17 infants were randomized to acetaminophen and 20 to indomethacin. One (5.9%) hsPDA in the acetaminophen group had successful treatment compared to 11 (55%) in the indomethacin group (p = 0.002). Eight (47%) in the acetaminophen group and 3 (15%) in the indomethacin group received transcatheter PDA closure (p = 0.07). IV indomethacin was more effective than IV acetaminophen for treatment of hsPDAs. More infants in the acetaminophen group received transcatheter closure.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Alagarsamy S, Chhabra M, Gudavalli M, Nadroo AM, Sutija VG, Yugrakh D. Comparison of clinical criteria with echocardiographic findings in diagnosing PDA in preterm infants. J Perinat Med. 2005;33:161–4.
Davis P, Turner-Gomes S, Cunningham K, Way C, Roberts R, Schmidt B. Precision and accuracy of clinical and radiological signs in premature infants at risk of patent ductus arteriosus. Arch Pediatr Adolesc Med. 1995;149:1136–41.
Skelton R, Evans N, Smythe J. A blinded comparison of clinical and echocardiographic evaluation of the preterm infant for patent ductus arteriosus. J Paediatr Child Health. 1994;30:406–11.
Zonnenberg I, de Waal K. The definition of a haemodynamic significant duct in randomized controlled trials: a systematic literature review. Acta Paediatr. 2012;101:247–51.
Silverman NH, Lewis AB, Heymann MA, Rudolph AM. Echocardiographic assessment of ductus arteriosus shunt in premature infants. Circulation. 1974;50:821–5.
Evans N, Iyer P. Longitudinal changes in the diameter of the ductus arteriosus in ventilated preterm infants: correlation with respiratory outcomes. Arch Dis Child Fetal Neonatal Ed. 1995;72:F156–F161.
Kluckow M, Evans N. Early echocardiographic prediction of symptomatic patent ductus arteriosus in preterm infants undergoing mechanical ventilation. J Pediatrics. 1995;127:774–9.
Skinner JR, Boys RJ, Hunter S, Hey EN. Non-invasive assessment of pulmonary arterial pressure in healthy neonates. Arch Dis Child. 1991;66:386–90.
Su BH, Watanabe T, Shimizu M, Yanagisawa M. Echocardiographic assessment of patent ductus arteriosus shunt flow pattern in premature infants. Arch Dis Child Fetal neonatal Ed. 1997;77:F36–40.
Bell EF, Acarregui MJ. Restricted versus liberal water intake for preventing morbidity and mortality in preterm infants. Cochrane Database Syst. Rev. 2014;12:CD000503.
Bell EF, Warburton D, Stonestreet BS, Oh W. Effect of fluid administration on the development of symptomatic patent ductus arteriosus and congestive heart failure in premature infants. N. Engl J Med. 1980;302:598–604.
Vanhaesebrouck S, Zonnenberg I, Vandervoort P, Bruneel E, Van Hoestenberghe MR, Theyskens C. Conservative treatment for patent ductus arteriosus in the preterm. Arch Dis Child Fetal neonatal Ed. 2007;92:F244–247.
Brion LP, Campbell DE. Furosemide for symptomatic patent ductus arteriosus in indomethacin-treated infants. Cochrane Database Syst Rev. 2001;3:Cd001148.
Ohlsson A, Walia R, Shah SS. Ibuprofen for the treatment of patent ductus arteriosus in preterm or low birth weight (or both) infants. Cochrane Database Syst Rev. 2020;2:Cd003481.
Friedman Z, Whitman V, Maisels MJ, Berman W Jr., Marks KH, Vesell ES. Indomethacin disposition and indomethacin-induced platelet dysfunction in premature infants. J Clin Pharmacol. 1978;18:272–9.
Edwards AD, Wyatt JS, Richardson C, Potter A, Cope M, Delpy DT, et al. Effects of indomethacin on cerebral haemodynamics in very preterm infants. Lancet. 1990;335:1491–5.
Cifuentes RF, Olley PM, Balfe JW, Radde IC, Soldin SJ. Indomethacin and renal function in premature infants with persistent patent ductus arteriosus. J Pediatr. 1979;95:583–7.
Nagaraj HS, Sandhu AS, Cook LN, Buchino JJ, Groff DB. Gastrointestinal perforation following indomethacin therapy in very low birth weight infants. J Pediatr Surg. 1981;16:1003–7.
Rheinlaender C, Helfenstein D, Walch E, Berns M, Obladen M, Koehne P. Total serum bilirubin levels during cyclooxygenase inhibitor treatment for patent ductus arteriosus in preterm infants. Acta Paediatr. 2009;98:36–42.
Waldvogel S, Atkinson A, Wilbeaux M, Nelle M, Berger MR, Gerull R. High dose indomethacin for patent ductus arteriosus closure increases neonatal morbidity [published online ahead of print, 2019 Dec 30]. Am J Perinatol. 2019. https://doi.org/10.1055/s-0039-3400996.
Coombs RC, Morgan ME, Durbin GM, Booth IW, McNeish AS. Gut blood flow velocities in the newborn: effects of patent ductus arteriosus and parenteral indomethacin. Arch Dis Child. 1990;65:1067–71.
Wadhawan R, Oh W, Vohr BR, Saha S, Das A, Bell EF, et al. Spontaneous intestinal perforation in extremely low birth weight infants: association with indometacin therapy and effects on neurodevelopmental outcomes at 18–22 months corrected age. Arch Dis Child Fetal neonatal Ed. 2013;98:F127–132.
Hammerman C, Bin-Nun A, Markovitch E, Schimmel MS, Kaplan M, Fink D. Ductal closure with paracetamol: a surprising new approach to patent ductus arteriosus treatment. Pediatrics. 2011;128:e1618–e1621.
Dash SK, Kabra NS, Avasthi BS, Sharma SR, Padhi P, Ahmed J. Enteral paracetamol or intravenous indomethacin for closure of patent ductus arteriosus in preterm neonates: a randomized controlled trial. Indian Pediatrics. 2015;52:573–8.
El-Mashad AE-R, El-Mahdy H, El Amrousy D, Elgendy M. Comparative study of the efficacy and safety of paracetamol, ibuprofen, and indomethacin in closure of patent ductus arteriosus in preterm neonates. Eur J pediatrics. 2017;176:233–40.
Terrin G, Conte F, Oncel MY, Scipione A, McNamara PJ, Simons S, et al. Paracetamol for the treatment of patent ductus arteriosus in preterm neonates: a systematic review and meta-analysis. Arch Dis Child Fetal Neonatal Ed. 2015;101:F127-36.
Ohlsson A, Shah PS. Paracetamol (acetaminophen) for patent ductus arteriosus in preterm or low birth weight infants. Cochrane Database Syst Rev. 2020;1:Cd010061.
El Hajjar M, Vaksmann G, Rakza T, Kongolo G, Storme L. Severity of the ductal shunt: a comparison of different markers. Arch Dis Child Fetal neonatal Ed. 2005;90:F419–422.
Skinner J. Diagnosis of patent ductus arteriosus. Semin Neonatol. 2001;6:49–61.
Thomson R. Neofax 2011. New York: Thomson Reuters; 2011.
Bell MJ, Ternberg JL, Feigin RD, Keating JP, Marshall R, Barton L, et al. Neonatal necrotizing enterocolitis. Therapeutic decisions based upon clinical staging. Ann Surg. 1978;187:1.
Neu J. Necrotizing enterocolitis: the search for a unifying pathogenic theory leading to prevention. Pediatr Clin. 1996;43:409–32.
Papile LA, Burstein J, Burstein R, Koffler H. Incidence and evolution of subependymal and intraventricular hemorrhage: a study of infants with birth weights less than 1,500 gm. J Pediatr. 1978;92:529–34.
Prematurity* CoRo. The international classification of retinopathy of prematurity revisited. Arch Ophthalmol. 2005;123:991–9.
Benitz WE. Patent ductus arteriosus in preterm infants. Pediatrics. 2016;137:e20153730.
Sathanandam S, Whiting S, Cunningham J, Zurakowski D, Apalodimas L, Waller BR, et al. Practice variation in the management of patent ductus arteriosus in extremely low birth weight infants in the United States: survey results among cardiologists and neonatologists. Congenit heart Dis. 2019;14:6–14.
Liebowitz M, Kaempf J, Erdeve O, Bulbul A, Håkansson S, Lindqvist J, et al. Comparative effectiveness of drugs used to constrict the patent ductus arteriosus: a secondary analysis of the PDA-TOLERATE trial (NCT01958320). J Perinatol. 2019;39:599–607.
Malviya M, Ohlsson A, Shah S. Surgical versus medical treatment with cyclooxygenase inhibitors for symptomatic patent ductus arteriosus in preterm infants. Cochrane Database Syst Rev. 2008;1:Cd003951.
Backes CH, Cheatham SL, Deyo GM, Leopold S, Ball MK, Smith CV, et al. Percutaneous Patent ductus arteriosus (PDA) closure in very preterm infants: feasibility and complications. J Am Heart Assoc. 2016;5:e002923. Published 2016 Feb 12. https://doi.org/10.1161/JAHA.115.002923.
Sathanandam S, Agrawal H, Chilakala S, Johnson J, Allen K, Knott-Craig C, et al. Can transcatheter PDA closure be performed in neonates </=1000 grams? The Memphis experience. Congenit Heart Dis. 2019;14:79–84.
Russell JL, Leblanc JG, Potts JE, Sett SS. Is surgical closure of patent ductus arteriosus a safe procedure in premature infants? Int Surg. 1998;83:358–60.
Weisz DE, More K, McNamara PJ, Shah PS. PDA ligation and health outcomes: a meta-analysis. Pediatrics. 2014;133:e1024–1046.
Dang D, Wang D, Zhang C, Zhou W, Zhou Q, Wu H. Comparison of oral paracetamol versus ibuprofen in premature infants with patent ductus arteriosus: a randomized controlled trial. PLoS ONE. 2013;8:e77888.
Oncel MY, Yurttutan S, Erdeve O, Uras N, Altug N, Oguz SS, et al. Oral paracetamol versus oral ibuprofen in the management of patent ductus arteriosus in preterm infants: a randomized controlled trial. J Pediatr. 2014;164:510–514. e511.
Palmer G, Atkins M, Anderson B, Smith K, Culnane T, McNally C, et al. IV acetaminophen pharmacokinetics in neonates after multiple doses. Br J Anaesth. 2008;101:523–30.
Akbari Asbagh P, Zarkesh MR, Nili F, Nayeri FS, Tofighi Naeem A. Prophylactic teatment with oral paracetamol for patent ductus arteriosus in preterm infants: a randomized clinical trial. Tehran Univ Med J TUMS Publ. 2015;73:86–92.
Yang B, Gao X, Ren Y, Wang Y, Zhang Q. Oral paracetamol vs. oral ibuprofen in the treatment of symptomatic patent ductus arteriosus in premature infants: A randomized controlled trial. Exp therapeutic Med. 2016;12:2531–6.
Harkin P, Harma A, Aikio O, Valkama M, Leskinen M, Saarela T, et al. Paracetamol Accelerates closure of the ductus arteriosus after premature birth: a randomized trial. J Pediatr. 2016;177:72–77.e72.
Al-Lawama M, Alammori I, Abdelghani T, Badran E. Oral paracetamol versus oral ibuprofen for treatment of patent ductus arteriosus. J Int Med Res. 2018;46:811–8.
Roofthooft DWE, van Beynum IM, de Klerk JCA, van Dijk M, van den Anker JN, Reiss IKM, et al. Limited effects of intravenous paracetamol on patent ductus arteriosus in very low birth weight infants with contraindications for ibuprofen or after ibuprofen failure. Eur J Pediatrics. 2015;174:1433–40.
Acknowledgements
We thank Dr. Bruce Jenkins (Mednax) for helping with enrollment. We thank LeBonheur Children’s Hospital, Regional One Health and Methodist Germantown Hospital for support during this project.
Funding
No funding was received for this project.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
WMF is a consultant and speaker for Abbott Structural Heart/St Jude Medical. Otherwise, we know of no conflicts of interest associated with this publication, and there has been no significant financial support for this work that could have influences on its outcome.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Davidson, J.M., Ferguson, J., Ivey, E. et al. A randomized trial of intravenous acetaminophen versus indomethacin for treatment of hemodynamically significant PDAs in VLBW infants. J Perinatol 41, 93–99 (2021). https://doi.org/10.1038/s41372-020-0694-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-020-0694-1
This article is cited by
-
Acetaminophen for the patent ductus arteriosus: has safety been adequately demonstrated?
Journal of Perinatology (2023)
-
A Network Meta-Analysis of Intravenous Versus Oral Acetaminophen for Patent Ductus Arteriosus
Pediatric Cardiology (2023)
-
Predictors of successful patent ductus arteriosus closure with acetaminophen in preterm infants
Journal of Perinatology (2021)