Abstract
Objective
To determine the effect of timing of expression initiation on mother’s own milk production and time to secretory activation in mothers of preterm infants.
Study design
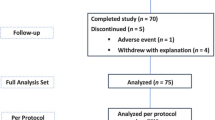
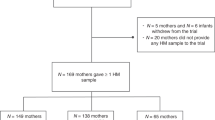
180 mothers delivering infants ≤1500 grams and ≤32 weeks gestation were randomized to begin expression within 60 (early), 61–180 (intermediate) or 181–360 (late) minutes following delivery. Milk volume was measured on days 1–7 and weekly for 6 weeks. Time to secretory activation was determined through self-report.
Results
The late group produced more milk than the early group in the first 3 days (p = 0.015–0.031) and over 6 weeks (p = 0.045). The late group had more expressions on day 1 (early: p = 0.049; intermediate; p = 0.048).
Conclusion
Initiation of expression at 181–360 min following delivery was associated with increased milk production for 6 weeks following delivery. Further research is needed to determine the effect of expression frequency on milk production in the first days following birth.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Cortez J, Makker K, Kraemer DF, Neu J, Sharma R, Hudak ML. Maternal milk feedings reduce sepsis, necrotizing enterocolitis and improve outcomes of premature infants. J Perinatol. 2018;38:71–4.
Corpeleijn WE, Kouwenhoven SM, Paap MC, van Vliet I, Scheerder I, Muizer Y, et al. Intake of own mother’s milk during the first days of life is associated with decreased morbidity and mortality in very low birth weight infants during the first 60 days of life. Neonatology. 2012;102:276–81.
Luo X, Zhai S, Shi N, Li M, Cui S, Xu Y, et al. The risk factors and neonatal outcomes of isolated single umbilical artery in singleton pregnancy: a meta-analysis. Sci Rep. 2017;7:7396.
Huang J, Zhang L, Tang J, Qu Y, Xiong T, Mu D, et al. Human milk as a protective factor for bronchopulmonary dysplasia: a systematic review and meta-analysis. Arch Dis Child Fetal Neonatal Ed. 2018;2:F128–36.
Patel AL, Johnson TJ, Engstrom JL, Fogg LF, Jegier BJ, Bigger HR, et al. Impact of early human milk on sepsis and health-care costs in very low birth weight infants. J Perinatol. 2003;33:514–9.
Fabiyi C, Rankin K, Norr K, Yoder JC, Vasa R, White-Traut R. The association of low social support with breast milk expression in low-income mother-preterm infant dyads. J Hum Lactation. 2015;31:490–7.
Parker LA, Sullivan S, Krueger C, Kelechi T, Mueller M. Effect of early breast milk expression on milk volume and timing of lactogenesis stage II among mothers of very low birth weight infants: a pilot study. J Perinatol. 2012;32:205–9.
Hill PD, Aldag JC, Chatterton RT, Zinaman M. Comparison of milk output between mothers of preterm and term infants: the first 6 weeks after birth. J Hum Lactation. 2005;21:22–30.
Cregan MD, De Mello TR, Kershaw D, McDougall K, Hartmann PE. Initiation of lactation in women after preterm delivery. Acta obstetricia et gynecologica Scandinavica. 2002;81:870–7.
Brownell E, Howard CR, Lawrence RA, Dozier AM. Delayed onset lactogenesis II predicts the cessation of any or exclusive breastfeeding. J Pediatrics. 2012;161:608–14.
Maastrup R, Hansen BM, Kronborg H, Bojesen SN, Hallum K, Frndson A, et al. Factors associated with exclusive breastfeeding of preterm infants. Results from a prospective national cohort study. PloS One. 2014;9:e89077.
Bonet M, Blondel B, Agostino R, Combier E, Maien RF, Cuttini M, et al. Variations in breastfeeding rates for very preterm infants between regions and neonatal units in Europe: results from the MOSAIC cohort. Arch Dis Child Fetal Neonatal Ed. 2011;96:F450–2.
Berkhout DJC, Klaassen P, Niemarkt HJ, de Boode WP, Cossey V, van Goudoeyer JB, et al. Risk factors for necrotizing enterocolitis: a prospective multicenter case-control study. Neonatology. 2018;114:277–84.
Battersby C, Longford N, Mandalia S, Costeloe K, Modi N. Incidence and enteral feed antecedents of severe neonatal necrotising enterocolitis across neonatal networks in England, 2012-13: a whole-population surveillance study. lancet Gastroenterol Hepatol. 2017;2:43–51.
Casavale KO, Ahuja JKC, Wu X, Li Y, Quam J, Olson R, et al. NIH workshop on human milk composition: summary and visions. Am J Clin Nutr. 2019;3:769–79.
Wall EH, Crawford HM, Ellis SE, Dahl GE, McFadden TB. Mammary response to exogenous prolactin or frequent milking during early lactation in dairy cows. J Dairy Sci. 2006;89:4640–8.
Wall EH, McFadden TB. The milk yield response to frequent milking in early lactation of dairy cows is locally regulated. J Dairy Sci. 2007;90:716–20.
Hale SA, Capuco AV, Erdman RA. Milk yield and mammary growth effects due to increased milking frequency during early lactation. J Dairy Sci. 2003;86:2061–71.
Murase M, Nommsen-Rivers L, Morrow AL, Hatsuno M, Mizuna K, Taki M, et al. Predictors of low milk volume among mothers who delivered preterm. J Hum Lactation. 2014;30:425–35.
Bishara R, Dunn MS, Merko SE, Darling P. Volume of foremilk, hindmilk, and total milk produced by mothers of very preterm infants born at less than 28 weeks of gestation. J Hum Lactation. 2009;25:272–9.
Hill PD, Aldag JC, Chatterton RT, Zinaman M. Primary and secondary mediators’ influence on milk output in lactating mothers of preterm and term infants. J Hum Lactation. 2005;21:138–50.
Parker LA, Sullivan S, Krueger C, Mueller M. Association of timing of initiation of breastmilk expression on milk volume and timing of lactogenesis stage II among mothers of very low-birth-weight infants. Breastfeed Med. 2015;10:84–91.
Furman L, Minich N, Hack M. Correlates of lactation in mothers of very low birth weight infants. Pediatrics. 2002;109:e57.
Haase B, Barreira J, Murphy PK, Mueller M, Rhodes J. The development of an accurate test weighing technique for preterm and high-risk hospitalized infants. Breastfeed Med. 2009;4:151–6.
Rankin MW, Jimenez EY, Caraco M, Collinson M, Lostetter L, DuPont TL. Validation of test weighing protocol to estimate enteral feeding volumes in preterm infants. J Pediatrics. 2016;178:108–12.
Chapman DJ, Perez-Escamilla R. Maternal perception of the onset of lactation is a valid, public health indicator of lactogenesis stage II. J Nutr. 2000;130:2972–80.
Perez-Escamilla R, Chapman DJ. Validity and public health implications of maternal perception of the onset of lactation: an international analytical overview. J Nutr. 2001;131:3021S–3024S.
Meier PP, Engstrom JL, Janes JE, Jegier BJ, Loera F. Breast pump suction patterns that mimic the human infant during breastfeeding: greater milk output in less time spent pumping for breast pump-dependent mothers with premature infants. J Perinatol. 2012;32:103–10.
Hill PD, Aldag JC, Demirtas H, Zinaman M, Chatterton RT. Mood states and milk output in lactating mothers of preterm and term infants. J Hum Lactation. 2006;22:305–14.
Smith VA, Preisser JS, Neelon B, Maciejewski ML. A marginalized two-part model for semicontinuous data. Stat Med. 2014;33:4891–903.
Smith VA, Neelon B, Preisser JS, Maciejewski ML. A marginalized two-part model for longitudinal semicontinuous data. Stat Methods Med Res. 2017;26:1949–68.
Voronca D, Gebregziabher M, Durkalski V, Liu L, Egede L. Marginalized two part models for generalized gamma family of distributions. 2015;arXiv:1511.05629.
Akaike H. A new look at the statistical model identification. IEEE Trans Autom Control. 1974;19:716–23.
Nakao Y, Moji K, Honda S, Oishi K. Initiation of breastfeeding within 120 min after birth is associated with breastfeeding at four months among Japanese women: a self-administered questionnaire survey. Int Breastfeed J. 2008;3:1.
Chien LY, Tai CJ. Effect of delivery method and timing of breastfeeding initiation on breastfeeding outcomes in Taiwan. Birth (Berkeley, Calif). 2007;34:123–30.
Hopkinson JM, Schanler RJ, Garza C. Milk production by mothers of premature infants. Pediatrics. 1988;81:815–20.
Hoban R, Patel AL, Medina Poeliniz C, Lai CT, Janes J, Geddes D, et al. Human milk biomarkers of secretory activation in breast pump-dependent mothers of premature infants. Breastfeed Med. 2018;13:352–60.
Patel AL, Johnson TJ, Engstrom JL, Fogg LF, Jegier BJ, Bigger HR, et al. Impact of early human milk on sepsis and health-care costs in very low birth weight infants. J Perinat. 2013;33:514–9.
Chollet-Hinton LS, Stuebe AM, Casbas-Hernandez P, Chetwynd E, Troester MA. Temporal trends in the inflammatory cytokine profile of human breastmilk. Breastfeed Med. 2014;9:530–7.
Wilson E, Christensson K, Brandt L, Altman M, Bonamy AK. Early provision of mother’s own milk and other predictors of successful breast milk feeding after very preterm birth: a regional observational study. J Hum Lactation. 2015;31:393–400.
Purdy IB, Singh N, Le C, Bell C, Whiteside C, Collins M. Biophysiologic and social stress relationships with breast milk feeding pre- and post-discharge from the neonatal intensive care unit. J Obstet Gynecologic Neonatal Nurs. 2012;41:347–57.
Acuna-Muga J, Ureta-Velasco N, de la Cruz-Bertolo J, Ballesteros-Lopez R, Sanchez-Martinez R, Miranda-Casabona E, et al. Volume of milk obtained in relation to location and circumstances of expression in mothers of very low birth weight infants. J Hum Lactation. 2014;30:41–6.
Lee HC, Gould JB. Factors influencing breast milk versus formula feeding at discharge for very low birth weight infants in California. J Pediatrics. 2009;155:657–62. e651-652
Cordero L, Valentine CJ, Samuels P, Giannone PJ, Nankervis CA. Breastfeeding in women with severe preeclampsia. Breastfeed Med. 2012;7:457–63.
Sisk P, Quandt S, Parson N, Tucker J. Breast milk expression and maintenance in mothers of very low birth weight infants: supports and barriers. J Hum Lactation. 2010;26:368–75.
Omarsdottir S, Adling A, Bonamy AK, Legnevall L, Tessma MK, Vanpee M. Predictors of sustained maternal milk feeds in extremely preterm infants. J Perinat. 2015;35(5):367–72.
Tie WJ, Gardner H, Lai CT, Hepworth AR, Al-Tamini Y, Paech MJ, et al. Changes in milk composition associated with pethidine-PCEA usage after Caesarean section. Matern Child Nutr. 2017;13:e12275.
Funding
This work was supported by a grant 1 R15 NR013566-01A1 from the National Institute of Nursing Research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
LAP, SS, CK and MM’s work has been funded by the NIH. None of the authors have additional conflict of interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Parker, L.A., Sullivan, S., Kruger, C. et al. Timing of milk expression following delivery in mothers delivering preterm very low birth weight infants: a randomized trial. J Perinatol 40, 1236–1245 (2020). https://doi.org/10.1038/s41372-020-0688-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-020-0688-z
This article is cited by
-
Lactation support in neonatal intensive care units in Germany from the mothers’ perspective – a mixed-method study of the current status and needs
BMC Pregnancy and Childbirth (2024)
-
Dilemmas in initiation of very preterm infant enteral feeds—when, what, how?
Journal of Perinatology (2023)
-
Leveraging mHealth and a milk expression frequency biomarker during postpartum to prolong lactation among parents of critically ill infants: a pilot study
Journal of Perinatology (2023)
-
Early pumping frequency and coming to volume for mother’s own milk feeding in hospitalized infants
Journal of Perinatology (2023)
-
Multi-prong quality improvement approach for increasing mother’s own milk use for very low birth weight infants
Journal of Perinatology (2023)