Abstract
Objective
Examine current approaches to addressing social determinants of health (SDOH) in the NICU and perceived appropriateness of a standardized screening and referral process.
Study design
We performed a mixed methods study in two Massachusetts safety-net NICUs. We examined rates that unmet basic needs were assessed and identified among 601 families. We conducted focus groups with NICU staff to understand current methods to assess unmet basic needs and perceived appropriateness of a standardized SDOH screening and referral process.
Result
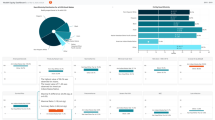
Except employment (89%), other unmet basic needs were infrequently assessed (housing 38%, food/hunger 7%, childcare 3%, transportation 3%, utilities 0.2%). Staff believed: (1) processes to assess SDOH were not standardized and inconsistently performed/documented; (2) addressing SDOH was important; and (3) using a standardized screening and referral process would be feasible.
Conclusions
Current NICU assessment of SDOH is limited and use of a standardized screening and referral process could be useful.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Social Determinants of Health. World Health Organization. https://www.who.int/social_determinants/sdh_definition/en/ (2020).
Marmot M. Social determinants of health inequalities. Lancet. 2005;365:1099–104.
Braveman P, Egerter S, Williams DR. The social determinants of health: coming of age. Annu Rev Public Health. 2011;32:381–98.
Poverty and Child Health in the United States. Council on Community Pediatrics. Pediatrics. 2016;137:e20160339.
Kaiser Family Foundation. A view from the states: key medicaid policy changes: results from a 50-State Mediciad Budget Survey for State Fiscal Years 2019 and 2020. https://www.kff.org/report-section/a-view-from-the-states-key-medicaid-policy-changes-delivery-systems/ (2020).
Profit J, Gould JB, Bennett M, Goldstein BA, Draper D, Phibbs CS, et al. Racial/ethnic disparity in NICU quality of care delivery. Pediatrics. 2017;140:e20170918.
Howell EA, Janevic T, Hebert PL, Egorova NN, Balbierz A, Zeitlin J. Differences in morbidity and mortality rates in Black, White, and Hispanic very preterm infants among New York City Hospitals. JAMA Pediatr. 2018;172:269–77.
Janevic T, Zeitlin J, Auger N, Egorova NN, Hebert P, Balbierz A, et al. Association of race/ethnicity with very preterm neonatal morbidities. JAMA Pediatr. 2018;172:1061–9.
Lewis TP, Andrews KG, Shenberger E, Betancourt TS, Fink G, Pereira S, et al. Caregiving can be costly: a qualitative study of barriers and facilitators to conducting kangaroo mother care in a US tertiary hospital neonatal intensive care unit. BMC Pregnancy Childbirth. 2019;19:227.
Greene MM, Rossman B, Patra K, Kratovil A, Khan S, Meier PP. Maternal psychological distress and visitation to the neonatal intensive care unit. Acta Paediatr. 2015;104:e306–13.
Parker MG, Sandel M, Frank D, Garg A. Unmet material needs among low-income families of US preterm infants. Philidelphia, PA: Pediatric Academic Societies; 2020.
Ivankova NV, Creswell JW, Stick SL. Using mixed-methods sequential explanatory design: from theory to practice. Field Methods. 2006;18:3–20.
Garg A, Toy S, Tripodis Y, Silverstein M, Freeman E. Addressing social determinants of health at well child care visits: a cluster RCT. Pediatrics. 2015;135:e296–304.
Bernard RH. Research methods in anthropology: qualitative and quantitative approaches. Walnut Creek: Altamira Press; 2002.
DeNavas-Walt C, Proctor BD. Income and poverty in the United States: 2014. 2014. https://www.census.gov/content/dam/Census/library/publications/2015/demo/p60-252.pdf. Accessed 21 Aug 2020.
Sokol R, Austin A, Chandler C, Byrum E, Bousquette J, Lancaster C, et al. Screening children for social determinants of health: a systematic review. Pediatrics. 2019;144:e20191622.
Vasan A, Kenyon CC, Palakshappa D. Differences in pediatric residents’ social needs screening practices across health care settings. Hosp Pediatr. 2020;10:443–6.
Joseph RM, O’Shea TM, Allred EN, Heeren T, Kuban KK. Maternal educational status at birth, maternal educational advancement, and neurocognitive outcomes at age 10 years among children born extremely preterm. Pediatr Res. 2018;83:767–77.
Linsell L, Malouf R, Morris J, Kurinczuk JJ, Marlow N. Prognostic factors for poor cognitive development in children born very preterm or with very low birth weight: a systematic review. JAMA Pediatr. 2015;169:1162–72.
Beck AF, Edwards EM, Horbar JD, Howell EA, McCormick MC, Pursley DM. The color of health: how racism, segregation, and inequality affect the health and well-being of preterm infants and their families. Pediatr Res. 2020;87:227–34.
Pursley DM, McCormick MC. Bending the arc for the extremely low gestational age newborn. Pediatr Res. 2018;83:751–3.
Shapiro N, Wachtel EV, Bailey SM, Espiritu MM. Implicit physician biases in periviability counseling. J Pediatr. 2018;197:109–15 e101.
Acknowledgements
We acknowledge the NICU staff that participated in our focus groups and the families that are cared for at the BMC and UMass NICUs. We acknowledge Alyssa Fliter, Mikayla Gordon Wexler, Archana Kalyanasundaram, Jordi Negron, Stephanie Philip, Stephen Rogers, Lindsey Simoncini, and Heather White for their assistance with data collection. This work was supported by the National Institute of Minority Health and Health Disparities (R01MD007793; PI Garg).
Author information
Authors and Affiliations
Contributions
MGP contributed to the conceptualization and design, analysis, and drafted and edited the manuscript. AG, LMR, and SK contributed to the conceptualization and design and edited the manuscript. AB and ESF contributed to acquisition of data, data analysis, and edited the manuscript. M-LD contributed to the conceptualization and design, analysis, and edited the manuscript. All authors approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Parker, M.G., Garg, A., Brochier, A. et al. Approaches to addressing social determinants of health in the NICU: a mixed methods study. J Perinatol 41, 1983–1991 (2021). https://doi.org/10.1038/s41372-020-00867-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-020-00867-w
This article is cited by
-
Identifying barriers and facilitators to care for infants with bronchopulmonary dysplasia after NICU discharge: a prospective study of parents and clinical stakeholders
Journal of Perinatology (2024)
-
Parent and grandparent neonatal intensive care unit visitation for preterm infants
Journal of Perinatology (2024)