Abstract
Objective
To evaluate whether combined surfactant with inhaled nitric oxide (iNO) use will prevent newborns with hypoxemic respiratory failure (HRF) from developing an Oxygenation Index (OI) > 40.
Methods
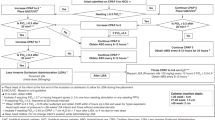
100 term newborns with acute HRF (OI ≥ 20) were randomized to: Surfactant+iNO: received iNO plus up to two doses of surfactant or iNO-Controls: received iNO+placebo. Main outcome was the development of severe HRF (OI > 40) despite iNO use.
Results
Baseline mean ± SD OI was 37.4 ± 14 for the Surfactant+iNO group and 38.2 ± 16 for the controls. Infants receiving surfactant+iNO improved their oxygenation faster, resulting in lower OI at 24 h: 12.9 ± 9 vs 18.7 ± 11 of controls, p < 0.05; and a lower proportion developing OI > 40: 24%(12/50) vs 50%(25/50) of controls, p < 0.02. Fewer infants receiving surfactant+iNO presented the combined outcome of death or ECMO: 16%(8/50) compared to 36%(18/50) of controls, p < 0.05.
Conclusions
Early use of combined surfactant+iNO improves oxygenation preventing the progression to severe HRF. This may reduce mortality and ECMO need.
Trial registration number
ISRCTN13727958
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Change history
08 February 2021
A Correction to this paper has been published: https://doi.org/10.1038/s41372-020-00806-9
References
Morin FC, Stenmark KR. Persistent pulmonary hypertension of the newborn. Am J Respir Crit Care Med. 1995;151:2010–32.
Steurer MA, Jelliffe-Pawlowski LL, Baer RJ, Partridge JC, Rogers EE, Keller RL. Persistent pulmonary hypertension of the newborn in late preterm and term infants in California. Pediatrics. 2017;139:e20161165. https://doi.org/10.1542/peds.2016-1165.
Mena P, Muhlhausen G, Novoa P, editors. Hypoxic respiratory failure and persistent pulmonary hypertension in the neonate. In: Guias Nacionales de Neonatología. Chilean Ministry of Health Publications, Santiago, Chile, 2005.
Steurer MA, Baer RJ, Oltman S, Ryckman KK, Feuer SK, Rogers E, et al. Morbidity of persistent pulmonary hypertension of the newborn in the first year of life. J Pediatr. 2019;213:58–65.
The Neonatal Inhaled Nitric Oxide Study Group. Inhaled nitric oxide in full-term infants with hypoxic respiratory failure. N. Engl J Med. 1997;336:597–604.
Roberts J, Fineman J, Morin F, Shaul P, Rimar S, Schreiber M, et al. Inhaled nitric oxide and persistent pulmonary hypertension of the newborn. N Engl J Med. 1997;336:605–10.
Clark R, Kueser T, Walker M, Southgate WM, Huckaby JL, Perez JA, et al. Low-dose nitric oxide therapy for persistent pulmonary hypertension of the newborn. N Engl J Med. 2000;342:469–74.
Stenmark K, Aldashev A, Orton E, Durmowicz AG, Badesch DB, Parks WC, et al. Cellular adaptation during chronic neonatal hypoxic pulmonary hypertension. Am J Physiol. 1991;261:97–104.
Davey AM, Becker JD, Davis JM. Meconium aspiration syndrome: physiological and inflammatory changes in a newborn piglet model. Pediatr Pulmonol. 1993;16:101–8.
Hallman M, Kankaanoaa K. Evidence of surfactant deficiency in persistent fetal circulation. Eur J Pediatr. 1980;134:129–34.
Hall SB, Notter RH, Smith RJ, Hyde RW. Altered function of pulmonary surfactant in fatty acid lung injury. J Appl Physiol. 1990;69:1143–9.
Findlay RD, Taeusch HW, Walther FJ. Surfactant replacement therapy for meconium aspiration syndrome. Pediatrics. 1996;97:48–52.
Lotze A, Mitchell BR, Bulas DI, Zola EM, Shalwitz RA, Gunkel JH. Multicenter study of surfactant (beractant) use in the treatment of term infants with severe respiratory failure. Survanta in Term Infants Study Group. J Pediatr. 1998;132:40–7.
Konduri G, Solimano A, Sokol G, Singer J, Ehrenkranz RA, Singhal N, et al. A randomized trial of early versus standard inhaled nitric oxide therapy inr term and near term newborn infants with hypoxic respiratory failure. Pediatrics. 2004;113:559–64.
González A, Fabres J, D’Apremont I, Urcelay G, Avaca M, Gandolfi C, et al. Randomized controlled trial of early compared with delayed use of inhaled nitric oxide in newborns with a moderate respiratory failure and pulmonary hypertension. J Perinatol. 2010;30:420–4.
Kattan J, González A, Becker P, Faunes M, Estay A, Toso P, et al. Survival of newborn infants with severe respiratory failure before and after establishing an ECMO program. Pediatr Crit Care Med. 2013;14:876–83.
Chinese Collaborative Study Group for Neonatal Respiratory Diseases. Treatment of severe meconium aspiration syndrome with porcine surfactant: a multicentre, randomized, controlled trial. Acta Pædiatrica. 2005;94:896–902.
El Shahed AI, Dargaville PA, Ohlsson A, Soll R. Surfactant for meconium aspiration syndrome in term and late preterm infants. Cochrane Database Syst Rev. 2014;12:CD002054. https://doi.org/10.1002/14651858.CD002054.
Kattwinkel J. Surfactant lavage for meconium aspiration: a word of caution. Pediatrics. 2002;109:1167–8.
Barrington KJ, Finer N, Pennaforte T, Altit G. Nitric oxide for respiratory failure in infants born at or near term. Cochrane Database Syst Rev. 2017;1:CD000399. https://doi.org/10.1002/14651858.CD000399.
Kinsella J, Truog W, Walsh W, Goldberg RN, Bancalari E, Mayock D, et al. Randomized, multicenter trial of inhaled nitric oxide and high frequency oscillatory ventilation in severe persistent pulmonary hypertension of the newborn. J Pediatr. 1997;131:55–62.
Dadiz R, Nair J, D’Angio CT, Ryan RM, Lakshminrusimha S. Methemoglobin and the response to inhaled nitric oxide in persistent pulmonary hypertension of the newborn. J Neonatal Perinat Med. 2019;10:3233/NPM-180082. https://doi.org/10.3233/NPM-180082.
Afolayan AJ, Eis A, Alexander M, Michalkiewicz T, Teng RJ, Lakshminrusimha S, et al. Decreased endothelial nitric oxide synthase expression and function contribute to impaired mitochondrial biogenesis and oxidative stress in fetal lambs with persistent pulmonary hypertension. Am J Physiol Lung Cell Mol Physiol. 2016;310:L40–49.
Issa A, Lappalainen U, Kleinman M, Bry K, Hallman M. Inhaled nitric oxide decreases hyperoxia-induced surfactant abnormality in preterm rabbits. Pediatr Res. 1999;45:247–54.
Gadzinowski J, Kowalska K, Vidyasagar D. Treatment of MAS with PPHN using combined therapy: SLL, bolus surfactant and iNO. J Perinatol. 2008;28:S56–66.
Dargaville PA, Copnell B, Mills JF, Haron I, Lee JK, Tingay DG. on behalf of the lessMAS Trial Study Group et al. Randomized controlled trial of lung lavage with dilute surfactant for meconium aspiration syndrome. J Pediatr. 2011;158:383–9.
Konduri GG, Sokol G, Van Meurs K, Singer J, Ambalavanan N, Lee T, et al. Impact of early surfactant and inhaled nitric oxide therapies on outcomes in term/late preterm neonates with moderate hypoxic respiratory failure. J Perinatol. 2013;33:944–9.
Acknowledgements
We are grateful to Angélica Domínguez for their statistical assistance and for the valuable help of the group of research collaborators of the five centers listed in Appendix 1.
Funding
Funded by the Chilean Fund for Health Research (FONIS): Project: SA07I20035.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix 1: Collaborators
Appendix 1: Collaborators
The following members from the centers are non-author contributors to this study. They contributed with data collection and provided clinical care for study patients:
Hospital Clínico Universidad Católica de Chile, Santiago: Katherine Flores, Rodrigo Lagos, Claudia Miralles, María Eugenia Pérez, Solange Rojas, Angélica Vives.
Hospital Guillermo Grant, Concepción: Lilian Cifuentes, Andrea Saldías, Claudia Aburto.
Hospital Dr. Luis Tisné, Santiago: María Lidia Poblete, Paula Vasquez.
Hospital San José, Santiago: Ana María Pacheco, Paula Ponce.
Hospital Dr. Sótero del Rio, Santiago: Mónica Ahumada, Patricia Mena, Claudia Toro.
Rights and permissions
About this article
Cite this article
González, A., Bancalari, A., Osorio, W. et al. Early use of combined exogenous surfactant and inhaled nitric oxide reduces treatment failure in persistent pulmonary hypertension of the newborn: a randomized controlled trial. J Perinatol 41, 32–38 (2021). https://doi.org/10.1038/s41372-020-00777-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-020-00777-x
This article is cited by
-
Use of surfactant beyond respiratory distress syndrome, what is the evidence?
Journal of Perinatology (2024)
-
Novel scoring tool of hypoxemic respiratory failure and pulmonary hypertension for defining severity of persistent pulmonary hypertension of newborn
Journal of Perinatology (2023)
-
Surf early to higher tides: surfactant therapy to optimize tidal volume, lung recruitment, and iNO response
Journal of Perinatology (2021)