Abstract
Objectives
To compare the effect of sildenafil citrate (SC) and low molecular weight heparin (LMWH) on neonatal birth weight (BW) and the fetoplacental blood flow in pregnancies with FGR.
Study design
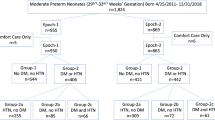
A parallel groups, randomized clinical trial was conducted at a university hospital, between June 2017 and September 2018, involving 100 pregnant women with placental mediated FGR between 28 and 35 weeks of gestation who were randomly assigned to receive either SC or LMWH started at FGR diagnosis till delivery.
Results
The neonatal BW in LMWH group was higher than SC group (p < 0.000) with a longer time from randomization till delivery, LMWH group had significant improvement in Ut A PI, UA PI, and MCA PI compared with SC treated group with p values 0.005, <0.000001, and 0.014, respectively.
Conclusion
The neonatal BW, time from randomization to delivery, and fetoplacental blood flow indices were significantly better with LMWH use compared with SC.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Yu YH, Shen LY, Zou H, Wang ZJ, Gong SP. Heparin for patients with growth restricted fetus: a prospective randomized controlled trial. J Matern Fetal Neonatal Med. 2010;23:980–7. https://doi.org/10.3109/14767050903443459.
Abd El-Wahed MA, El-Farghali OG, ElAbd HSA, El-Desouky ED, Hassan SM. Metabolic derangements in IUGR neonates detected at birth using UPLC-MS. Egypt J Med Hum Genet. 2017;18:281–7. https://doi.org/10.1016/j.ejmhg.2016.12.002.
Trapani A, Gonçalves LF, Trapani TF, Franco MJ, Galluzzo RN, Pires MM. Comparison between transdermal nitroglycerin and sildenafil citrate in intrauterine growth restriction: effects on uterine, umbilical and fetal middle cerebral artery pulsatility indices. Ultrasound Obstet Gynecol. 2016;48:61–65. https://doi.org/10.1002/uog.15673.
Cotechini T, Graham CH. Aberrant maternal inflammation as a cause of pregnancy complications: a potential therapeutic target. Placenta. 2015;36:960–6. https://doi.org/10.1016/j.placenta.2015.05.016.
Hossain N, Paidas MJ. Adverse pregnancy outcome, the uteroplacental interface, and preventive strategies. Semin Perinatol. 2007;31:208–12. https://doi.org/10.1053/j.semperi.2007.05.002.
Scifres CM, Nelson DM. Intrauterine growth restriction, human placental development and trophoblast cell death. J Physiol. 2009;587:3453–8. https://doi.org/10.1113/jphysiol.2009.173252.
Figueras F, Gratacós E. Update on the diagnosis and classification of fetal growth restriction and proposal of a stage-based management protocol. Fetal Diagn Ther. 2014;36:86–98. https://doi.org/10.1159/000357592.
Royal College of Obstetricians and Gynaecologists. The investigation and management of the small–for–gestational–age fetus. Green-top Guideline No. 31. London: RCOG; 2013.
Sibley CP. Treating the dysfunctional placenta. J Endocrinol. 2017;234:81–97. https://doi.org/10.1530/JOE-17-0185.
Say L, Gülmezoglu AM, Hofmeyr GJ. Maternal nutrient supplementation for suspected impaired fetal growth. Cochrane Database Syst Rev. 2003;CD000148. https://doi.org/10.1002/14651858.CD000148.
Gülmezoglu AM, Hofmeyr GJ. Maternal oxygen administration for suspected impaired fetal growth. Cochrane Database Syst Rev. 2000;CD000137. https://doi.org/10.1002/14651858.CD000137.
Say L, Gülmezoglu AM, Hofmeyr GJ. Plasma volume expansion for suspected impaired fetal growth. Cochrane Database Syst Rev. 1996;CD000167. https://doi.org/10.1002/14651858.CD000167.
Newnham JP, Godfrey M, Walters BJ, Phillips J, Evans SF. Low dose aspirin for the treatment of fetal growth restriction: a randomized controlled trial. Aust N Z J Obstet Gynaecol 1995;35:370 https://doi.org/10.1111/j.1479-828X.1995.tb02144.x.
Gülmezoglu AM, Hofmeyr GJ. Bed rest in hospital for suspected impaired fetal growth. Cochrane Database Syst Rev. 2000;CD000034. https://doi.org/10.1002/14651858.CD000034.
Resnik R. Fetal growth restriction: evaluation and management. UpToDate. 2018. Topic 6768 Version 77.0. https://www.uptodate.com/contents/fetal-growth-restriction-evaluation-and-management?source=history_widget#H8. Accessed 6 Apr 2018.
Bose P, Black S, Kadyrov M, Weissenborn U, Neulen J, Regan L, et al. Heparin and aspirin attenuate placental apoptosis in vitro: Implications for early pregnancy failure. A J Obstet Gynecol. 2005;192:23–30. https://doi.org/10.1016/j.ajog.2004.09.029.
Oberkersch R, Attorresi AI, Calabrese GC. Low-molecular-weight heparin inhibition in classical complement activaton pathway during pregnancy. Thrombosis Res. 2010;125:e240–5. https://doi.org/10.1016/j.thromres.2009.11.030.
D’Ippolito S, Di Nicuolo F, Marana R, Castellani R, Stinson J, Tersigni C, et al. Emerging non anticoagulant role of low molecular weight heparins on extravillous trophoblast functions and on heparin binding-epidermal growth factor and cystein-rich angiogenic inducer 61 expression. Fertil Steril. 2012;98:1028–36. https://doi.org/10.1016/j.fertnstert.2012.06.042.
Yinon Y, Ben Meir E, Margolis L, Lipitz S, Schiff E, Mazaki-Tovi S, et al. Low molecular weight heparin therapy during pregnancy is associated with elevated circulatory levels of placental growth factor. Placenta. 2015;36:121–4. https://doi.org/10.1016/j.placenta.2014.12.008.
Panda S, Das A. Sildenafil citrate in fatal growth restriction. J Reprod Infertil. 2014;15:168–9.
Satterfield MC, Bazer FW, Spencer TE, Wu G. Sildenafil citrate treatment enhances amino acid availability in the conceptus and fetal growth in an ovine model of intrauterine growth restriction. J Nutr. 2010;140:251–8. https://doi.org/10.3945/jn.109.114678.
Oysto C, Stanley JL, Oliver MH, Bloomfield FH, Baker PN. Maternal administration of sildenafil citrate alters fetal and placental growth and fetal–placental vascular resistance in the growth-restricted ovine fetus. Hypertension. 2016;68:760–7. https://doi.org/10.1161/HYPERTENSIONAHA.116.07662.
Dastjerdi MV, Hosseini S, Bayani L. Sildenafil citrate and uteroplacental perfusion in fetal growth restriction. J Res Med Sci. 2012;17:632–6.
El-Sayed MA, Saleh SA, Maher MA, Khidre AM. Utero-placental perfusion Doppler indices in growth restricted fetuses: effect of sildenafil citrate. J Matern Fetal Neonatal Med. 2018;31:1045–50. https://doi.org/10.1080/147670c8.2017.1306509.
Wareing M, Myers JE, O’Hara M, Baker PN. Sildenafil citrate (Viagra) enhances vasodilatation in fetal growth restriction. J Clin Endocrinol Metab. 2005;90:2550–5. https://doi.org/10.1210/jc.2004-1831.
Sharp A, Cornforth C, Jackson R, Harrold J, Turner MA, Kenny LC, et al. Maternal sildenafil for severe fetal growth restriction (STRIDER): a multicentre, randomised, placebo-controlled, double-blind trial. Lancet Child Adolesc Health. 2018;2:93–102. https://doi.org/10.1016/S2352-4642(17)30173-6. STRIDER group.
Groom KM, McCowan LM, Mackay LK, Lee AC, Gardener G, Unterscheider J. STRIDER NZAus: a multicentre randomised controlled trial of sildenafil therapy in early-onset fetal growth restriction. BJOG. 2019;126:997–1006. https://doi.org/10.1111/1471-0528.15658.
Royal College of Obstetricians and Gynaecologists. Reducing the risk of venous thromboembolism during pregnancy and the puerperium. Green-top Guideline No. 37a. London: RCOG; 2015.
American College of Obstetricians and Gynecologists. Moderate caffeine consumption during pregnancy. Committee Opinion No. 462. Obstet Gynecol. 2010;116:467–8. https://doi.org/10.1097/AOG.0b013e3181eeb2a1.
Prochaska JJ, Grossman W, Young-Wolff KC, Benowitz NL. Validity of self-reported adult secondhand smoke exposure. Tob Control. 2013;24:48–53. https://doi.org/10.1136/tobaccocontrol-2013-051174.
Odibo AO, Riddick C, Pare E, Stamilio DM, Macones GA. Cerebro-placental Doppler ratio and adverse perinatal outcomes in intrauterine growth restriction: evaluating the impact of using gestational age-specific. J Ultrasound Med. 2005;24:1223–8. https://doi.org/10.7863/jum.2005.24.9.1223.
Gris JC, Chauleur C, Faillie JL, Baer G, Marès P, Fabbro-Peray P, et al. Enoxaparin for the secondary prevention of placental vascular complications in women with abruptio placentae: the pilot randomised controlled NOH-AP trial. Thromb Haemost. 2010;104:771–9. https://doi.org/10.1160/TH10-03-0167.
Rey E, Garneau P, David M, et al. Dalteparin for the prevention of recurrence of placental-mediated complications of pregnancy in women without thrombophilia: a pilot randomized controlled trial. J Thromb Haemost. 2009;7:58–64. https://doi.org/10.1111/j.1538-7836.2008.03230.x.
Kupferminc M, Rimon E, Many A, Maslovitz S, Lessing JB, Gamzu R. Low molecular weight heparin versus no treatment in women with previous severe pregnancy complications and placental findings without thrombophilia. Blood Coagul Fibrinolysis. 2011;22:123–6. https://doi.org/10.1097/MBC.0b013e328343315c.
Groom KM, David AL. The role of aspirin, heparin, and other interventions in the prevention and treatment of fetal growth restriction. Am J Obstet Gynecol. 2017;218:829–40. https://doi.org/10.1016/j.ajog.2017.11.565.
Dodd JM, McLeod A, Windrim RC, Kingdom J. Antithrombotic therapy for improving maternal or infant health outcomes in women considered at risk of placental dysfunction. Cochrane Database Syst Rev. 2015; CD006780. https://doi.org/10.1002/14651858.CD006780.pub3.
Yu YH, Shen LY, Wang ZJ, Zhang Y, Su GD. Effect of heparin on umbilical blood flow in patients with fetal growth retardation. Di Yi Jun Yi Da Xue Xue Bao. 2004;24:423–5.
Chen J, Gong X, Chen P, Luo K, Zhang X. Effect of L-arginine and sildenafil citrate on intrauterine growth restriction fetuses: a meta-analysis. BMC Pregnancy Childbirth. 2016;16:225 https://doi.org/10.1186/s12884-016-1009-6.
Choudhary R, Desai K, Parekh H, Ganla K. Sildenafil citrate for the management of fetal growth restriction and oligohydramnios. Int J Women’s Health. 2016;8:367–72. https://doi.org/10.2147/IJWH.S108370.
Groom KM, Ganzevoort W, Alfirevic Z, Lim K, Papageorghiou AT. Clinicians should stop prescribing sildenafil for fetal growth restriction (FGR): comment from the STRIDER Consortium. Ultrasound Obstet Gynecol. 2018;52:295–6. https://doi.org/10.1002/uog.19186.
Dunn L, Greer R, Flenady V, Kumar S. Sildenafil in pregnancy: a systematic review of maternal tolerance and obstetric and perinatal outcomes. Fetal Diagn Ther. 2017;41:81–88. https://doi.org/10.1159/000453062.
Many A, Koren G. Low-molecular-weight heparins during pregnancy. Can Fam Physician Med de Famille Canadien. 2005;51:199–201.
Acknowledgements
The authors thank the participants of this study.
Author information
Authors and Affiliations
Contributions
RR contributed in literature search, study design, data analysis, data interpretation, and drafted the article, EBG contributed in literature search, data analysis, and supervision, and TR was responsible for data collection.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Rasheedy, R., El Bishry, G. & Tarek, R. Maternal low molecular weight heparin versus sildenafil citrate for fetal growth restriction: a randomized, parallel groups, open-label clinical trial. J Perinatol 40, 715–723 (2020). https://doi.org/10.1038/s41372-019-0544-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-019-0544-1