Abstract
Objective
We sought to determine the association of gastrostomy placement on post-NICU-discharge resource utilization in premature infants.
Study design
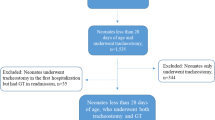
We performed a propensity-matched retrospective cohort study of NICU infants born under 32-week gestation in US Children’s Hospitals. Multivariable logistic regression and propensity score-matching were used to determine the association of gastrostomy placement on 90-day hospital readmissions and emergency department visits adjusting for salient patient characteristics.
Result
A total of 12,621 premature infants were included of which 697 (5.5%) underwent gastrostomy placement. After propensity matching, infants who underwent gastrostomy placement have a higher rate of 90-day inpatient readmission (41.9 vs 26.3%, p < 0.001) and emergency department visit (27.1 vs 16%, p < 0.001).
Conclusion
Premature infants who undergo gastrostomy placement have increased the risk of inpatient readmission and emergency department visits after NICU discharge. Gastrostomy placement likely is both a driver and marker for increased resource utilization in premature infants post-NICU discharge.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Villar J, Giuliani F, Barros F, Roggero P, Coronado Zarco IA, Rego MAS, et al. Monitoring the postnatal growth of preterm infants: a paradigm change. Pediatrics. 2018;141:e20172467. https://doi.org/10.1542/peds.2017-2467.
McSweeney ME, Smithers CJ. Advances in pediatric gastrostomy placement. Gastrointest Endosc Clin N Am. 2016;26:169–85. https://doi.org/10.1016/j.giec.2015.09.001.
Greene NH, Greenberg RG, O’Brien SM, Kemper AR, Miranda ML, Clark RH, et al. Variation in gastrostomy tube placement in premature infants in the United States. Am J Perinatol. 2018. https://doi.org/10.1055/s-0038-1676591.
Jadcherla SR, Khot T, Moore R, Malkar M, Gulati IK, Slaughter JL. Feeding methods at discharge predict long-term feeding and neurodevelopmental outcomes in preterm infants referred for gastrostomy evaluation. J Pediatr. 2017;181:125–30 e121. https://doi.org/10.1016/j.jpeds.2016.10.065.
Kapadia MZ, Joachim KC, Balasingham C, Cohen E, Mahant S, Nelson K, et al. A core outcome set for children with feeding tubes and neurologic impairment: a systematic review. Pediatrics. 2016, 138. https://doi.org/10.1542/peds.2015-3967.
Prodhan P, Tang X, Gossett J, Beam B, Simsic J, Ghanayem N, et al. Gastrostomy tube placement among infants with hypoplastic left heart syndrome undergoing stage 1 palliation. Congenit Heart Dis. 2018;13:519–27. https://doi.org/10.1111/chd.12610.
Mahant S, Jovcevska V, Cohen E. Decision-making around gastrostomy-feeding in children with neurologic disabilities. Pediatrics. 2011;127:e1471–1481. https://doi.org/10.1542/peds.2010-3007.
Goldin AB, Heiss KF, Hall M, Rothstein DH, Minneci PC, Blakely ML, et al. Emergency department visits and readmissions among children after gastrostomy tube placement. J Pediatr. 2016;174:139–45 e132. https://doi.org/10.1016/j.jpeds.2016.03.032.
Arca MJ, Rangel SJ, Hall M, Rothstein DH, Blakely ML, Minneci PC, et al. Case volume and revisits in children undergoing gastrostomy tube placement. J Pediatr Gastroenterol Nutr. 2017;65:232–6. https://doi.org/10.1097/MPG.0000000000001523.
Mason CA, Skarda DE, Bucher BT. Outcomes after laparoscopic gastrostomy suture techniques in Children. J Surg Res. 2018;232:26–32. https://doi.org/10.1016/j.jss.2018.05.022.
Barnhart DC, Hall M, Mahant S, Goldin AB, Berry JG, Faix RG, et al. Effectiveness of fundoplication at the time of gastrostomy in infants with neurological impairment. JAMA Pediatr. 2013;167:911–8. https://doi.org/10.1001/jamapediatrics.2013.334.
Zhang Z. Propensity score method: a non-parametric technique to reduce model dependence. Ann Transl Med. 2017;5:7. https://doi.org/10.21037/atm.2016.08.57.
Kuo DZ, Berry JG, Hall M, Lyle RE, Stille CJ. Health-care spending and utilization for children discharged from a neonatal intensive care unit. J Perinatol. 2018;38:734–41. https://doi.org/10.1038/s41372-018-0055-5.
Lee JH, Chang YS, Committee on Data C, Statistical Analysis tKSoN. Use of medical resources by preterm infants born at less than 33 weeks’ gestation following discharge from the neonatal intensive care unit in korea. J Korean Med Sci. 2015;30:S95–S103. https://doi.org/10.3346/jkms.2015.30.S1.S95.
Khalil ST, Uhing MR, Duesing L, Visotcky A, Tarima S, Nghiem-Rao TH. Outcomes of infants with home tube feeding: comparing nasogastric vs gastrostomy tubes. JPEN J Parenter Enter Nutr. 2017;41:1380–5. https://doi.org/10.1177/0148607116670621.
Jadcherla SR, Dail J, Malkar MB, McClead R, Kelleher K, Nelin L. Impact of process optimization and quality improvement measures on neonatal feeding outcomes at an all-referral neonatal intensive care unit. JPEN J Parenter Enter Nutr. 2016;40:646–55. https://doi.org/10.1177/0148607115571667.
Khan A, Nakamura MM, Zaslavsky AM, Jang J, Berry JG, Feng JY, et al. Same-hospital readmission rates as a measure of pediatric quality of care. JAMA Pediatr. 2015;169:905–12. https://doi.org/10.1001/jamapediatrics.2015.1129.
Funding
This work was supported by the National Institutes of Health (T35DK103596, TLD, and JU) and the Agency for Healthcare Research and Quality (1K08HS025776, BTB).
Author information
Authors and Affiliations
Contributions
TLD conceptualized the design of the study; contributed to the acquisition, analysis and interpretation of data; drafted the article and revised the manuscript. JU significantly contributed to the design of the study, data analysis and critically reviewed the manuscript for intellectual content. BTB conceptualized the design of the study, supervised data acquisition and analysis, and critically reviewed the manuscript for intellectual content. All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Duncan, T.L., Ulugia, J. & Bucher, B.T. Association of gastrostomy placement on hospital readmission in premature infants. J Perinatol 39, 1485–1491 (2019). https://doi.org/10.1038/s41372-019-0504-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-019-0504-9
This article is cited by
-
Enteral tube feeding selection at NICU discharge and resource utilization
Journal of Perinatology (2023)
-
Risk factors for hospital readmission among infants with prolonged neonatal intensive care stays
Journal of Perinatology (2022)