Abstract
Objective
To examine neonatology providers’ preferences regarding periviability guidelines.
Study design
An online cross-sectional survey of American Academy of Pediatrics Section on Neonatal-Perinatal Medicine members.
Results
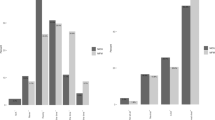
Most of the 480 respondents desired standardized guidelines for upper (85%) and lower (87%) gestational age limits for offering resuscitation and comfort care. Standardization was most to least frequently desired at the national, institutional, and regional levels. Within scenarios involving parents’ preferences conflicting with institutional guidelines, respondents chose parent-preferred options more often (66 vs. 34%). Overall, resuscitation (48%) versus comfort care (52%) were nearly equally chosen. In emergency scenarios, more versus less experienced respondents favored parent-preferred options over guidelines (55 vs. 46%, p = 0.003) and chose resuscitation over comfort care (50 vs. 36%, p < 0.001).
Conclusions
Neonatal providers desire age-based periviability guidelines, but do not agree on the level of standardization. Such limits may be insufficient to guide clinical practice. Policies should include processes that direct providers through fair transparent decision-making.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Arzuaga BH, Meadow W. National variability in neonatal resuscitation practices at the limit of viability. Am J Perinatol. 2014;31:521–8.
Batton DG, Newborn CoFa. Clinical report—antenatal counseling regarding resuscitation at an extremely low gestational age. Pediatrics. 2009;124:422–7.
Cummings J, NEWBORN COFA. Antenatal counseling regarding resuscitation and intensive care before 25 weeks of gestation. Pediatrics. 2015;136:588–95.
Raju TN, Mercer BM, Burchfield DJ, Joseph GF. Periviable birth: executive summary of a joint workshop by the Eunice Kennedy Shriver National Institute of Child Health and Human Development, Society for Maternal-Fetal Medicine, American Academy of Pediatrics, and American College of Obstetricians and Gynecologists. Obstet Gynecol. 2014;123:1083–96.
Feltman DM, Williams DD, Carter BS. How are neonatology fellows trained for antenatal periviability counseling? Am J Perinatol. 2017;34:1279–85.
Kaempf JW, Tomlinson M, Arduza C, Anderson S, Campbell B, Ferguson LA, et al. Medical staff guidelines for periviability pregnancy counseling and medical treatment of extremely premature infants. Pediatrics. 2006;117:22–29.
Pignotti MS, Donzelli G. Perinatal care at the threshold of viability: an international comparison of practical guidelines for the treatment of extremely preterm births. Pediatrics. 2008;121:e193–198.
Miljeteig I, Markestad T, Norheim OF. Physicians’ use of guidelines and attitudes to withholding and withdrawing treatment for extremely premature neonates in Norway. Acta Paediatr. 2007;96:825–9.
Wilkinson AR, Ahluwalia J, Cole A, Crawford D, Fyle J, Gordon A, et al. Management of babies born extremely preterm at less than 26 weeks of gestation: a framework for clinical practice at the time of birth. Arch Dis Child Fetal Neonatal Ed. 2009;94:F2–5.
Geurtzen R, van Heijst A, Draaisma J, Ouwerkerk L, Scheepers H, Woiski M, et al. Professionals’ preferences in prenatal counseling at the limits of viability: a nationwide qualitative Dutch study. Eur J Pediatr. 2017;176:1107–19.
American Academy of Pediatrics Section on Neonatal Perinatal Medicine. Section on Neonatal Perinatal Medicine Who We Are. 2018. Accessed on 6 September 2018. https://www.aap.org/en-us/about-the-aap/Committees-Councils-Sections/Neonatal-Perinatal-Medicine/Pages/Who-We-Are.aspx
Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, Conde JG. Research electronic data capture (REDCap)—a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform. 2009;42:377–81.
Gray MM, Umoren RA, Harris S, Strandjord TP, Sawyer T. Use and perceived safety of stylets for neonatal endotracheal intubation: a national survey. J Perinatol. 2018;38:1331–6.
Jacobs AP, Subramaniam A, Tang Y, Philips JB, Biggio JR, Edwards RK, et al. Trisomy 18: a survey of opinions, attitudes, and practices of neonatologists. Am J Med Genet A. 2016;170:2638–43.
Burnsed J, Zanelli SA. Neonatal therapeutic hypothermia outside of standard guidelines: a survey of U.S. neonatologists. Acta Paediatr. 2017;106:1772–9.
Feltman DM, Du H, Leuthner SR. Survey of neonatologists’ attitudes toward limiting life-sustaining treatments in the neonatal intensive care unit. J Perinatol. 2012;32:886–92.
Geurtzen R, Van Heijst A, Hermens R, Scheepers H, Woiski M, Draaisma J, et al. Preferred prenatal counselling at the limits of viability: a survey among Dutch perinatal professionals. BMC Pregnancy Childbirth. 2018;18:7.
Martinez AM, Partridge JC, Yu V, Wee Tan K, Yeung CY, Lu JH, et al. Physician counselling practices and decision-making for extremely preterm infants in the Pacific Rim. J Paediatr Child Health. 2005;41:209–14.
Geurtzen R, Draaisma J, Hermens R, Scheepers H, Woiski M, van Heijst A, et al. Perinatal practice in extreme premature delivery: variation in Dutch physicians’ preferences despite guideline. Eur J Pediatr. 2016;175:1039–46.
Janvier A, Barrington KJ, Aziz K, Bancalari E, Batton D, Bellieni C, et al. CPS position statement for prenatal counselling before a premature birth: simple rules for complicated decisions. Paediatr Child Health. 2014;19:22–24.
Janvier A, Lantos J. Delivery room practices for extremely preterm infants: the harms of the gestational age label. Arch Dis Child Fetal Neonatal Ed. 2016;101:F375–376.
Tyson JE, Parikh NA, Langer J, Green C, Higgins RD, Network NIoCHaHDNR. Intensive care for extreme prematurity—moving beyond gestational age. N Engl J Med. 2008;358:1672–81.
Sjörs G. Treatment decisions for extremely preterm newborns: beyond gestational age. Acta Paediatr. 2010;99:1761–2.
Wilkinson DJ. Gestational ageism. Arch Pediatr Adolesc Med. 2012;166:567–72.
Wilkinson D, Verhagen E, Johansson S. Thresholds for resuscitation of extremely preterm infants in the UK, Sweden, and Netherlands. Pediatrics. 2018;142(Suppl 1):S574–S584.
Alleman BW, Bell EF, Li L, Dagle JM, Smith PB, Ambalavanan N, et al. Individual and center-level factors affecting mortality among extremely low birth weight infants. Pediatrics. 2013;132:e175–184.
Rysavy MA, Li L, Bell EF, Das A, Hintz SR, Stoll BJ, et al. Between-hospital variation in treatment and outcomes in extremely preterm infants. N Engl J Med. 2015;372:1801–11.
Kunkel MD, Downs SM, Tucker Edmonds B. Influence of maternal factors in neonatologists’ counseling for periviable pregnancies. Am J Perinatol. 2017;34:787–94.
Nayeri F, Asghari F, Baser A, Janani L, Shariat M, Eabrhim B. Views and decisions of physicians in encountering neonates with poor prognosis. Arch Iran Med. 2017;20:172–7.
Wilkinson D, Hayden D. In search of consistency: scandinavian approaches to resuscitation of extremely preterm infants. Pediatrics. 2018;142(Suppl 1):S603–S606.
Duffy D, Reynolds P. Babies born at the threshold of viability: attitudes of paediatric consultants and trainees in South East England. Acta Paediatr. 2011;100:42–46.
Arzuaga BH, Cummings CL. Practices and education surrounding anticipated periviable deliveries among neonatal-perinatal medicine and maternal-fetal medicine fellowship programs. J Perinatol. 2016;36:699–703.
Acknowledgements
We thank our colleagues at the University of Washington and Evanston Hospital for improving our survey through their pilot feedback. Data management was possible through grant support for REDCap from NorthShore University HealthSystem.
Funding
Data management was possible through grant support for REDCap from NorthShore University HealthSystem.
Author contributions
JAK and DMF developed the concept for the project, designed the survey, analyzed the data, and wrote the manuscript together.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Krick, J.A., Feltman, D.M. Neonatologists’ preferences regarding guidelines for periviable deliveries: do we really know what we want?. J Perinatol 39, 445–452 (2019). https://doi.org/10.1038/s41372-019-0313-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-019-0313-1
This article is cited by
-
Perspectives on Resuscitation Decisions at the Margin of Viability among Specialist Newborn Care Providers in Ghana and Ethiopia: A Qualitative Analysis
BMC Pediatrics (2022)
-
The child with medical complexity
Italian Journal of Pediatrics (2021)
-
Prevalence and predictors of donor milk programs among U.S. advanced neonatal care facilities
Journal of Perinatology (2020)
-
Joint periviability counseling between neonatology and obstetrics is a rare occurrence
Journal of Perinatology (2020)