Abstract
Objective:
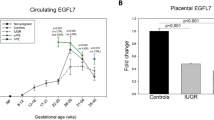
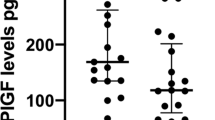
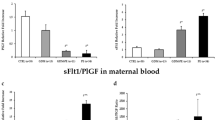
To assess the effect of infant size as a marker of placental function on the association between preeclampsia and the ratio of soluble fms-like tyrosine kinase 1 (sFlt-1) to placental growth factor (PlGF).
Study design:
The angiogenic factors sFlt-1 and PlGF were measured prospectively at 26 weeks gestation in 2322 women. Pregnancies were stratified by whether or not they were complicated by preeclampsia, the timing of delivery, and birthweight Z-score.
Result:
Independent of preeclampsia status, women with small infants (Z < -1.0) have an increased sFlt-1/PlGF ratio, and women with large infants (Z > 1.0) have a decreased ratio. Among pregnancies yielding small infants, the sFlt-1/PlGF ratio is markedly elevated in preeclamptic pregnancies requiring delivery before 37 weeks (110.0 vs. 17.9, p < 0.0001) but not in preeclamptic pregnancies delivered at term. The strength of the association between preeclampsia and the sFlt-1/PlGF ratio is increased for small infants compared to normal-sized or large infants.
Conclusion:
The sFlt-1/PlGF ratio in the late second trimester is similarly elevated in women with preeclampsia and in women with small infant size and more markedly elevated in a syndrome of placental dysfunction characterized by preeclampsia, preterm delivery, and growth restriction.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
American College of Obstetricians and Gynecologists, Task Force on Hypertension in Pregnancy. Hypertension in pregnancy. Obstet Gynecol. 2013;122:1122–31.
Maynard SE, Min JY, Merchan J, Lim KH, Li J, Libermann TA, et al. Excess placental soluble fms-like tyrosine kinase 1 (sFlt1) may contribute to endothelial dysfunction, hypertension, and proteinuria in preeclampsia. J Clin Invest. 2003;111:649–58.
Levine RJ, Maynard SE, Qian C, Lim KH, England LJ, Yu KF, et al. Circulating angiogenic factors and the risk of preeclampsia. N Engl J Med. 2004;350:672–83.
Polliotti BM, Fry AG, Saller DN, Mooney RA, Cox C, Miller RK. Second-trimester maternal serum placental growth factor and vascular endothelial growth factor for predicting severe, early-onset preeclampsia. Obstet Gynecol. 2003;101:1266–74.
Unal ER, Robinson CJ, Johnson DD, Chang EY. Second-trimester angiogenic factors as biomarkers for future-onset preeclampsia. Am J Obstet Gynecol. 2007;197:211.e1–e4.
Villa PM, Hamalainen E, Maki A, Räikkönen K, Pesonen AK, Taipale P, et al. Vasoactive agents for the prediction of early- and late-onset preeclampsia in a high-risk cohort. BMC Pregnancy Childbirth. 2013;3:110.
Verlohren S, Herraiz I, Lapaire O, Schlembach D, Moertl M, Zeisler H, et al. The sFlt-1/PlGF ratio in different types of hypertensive pregnancy disorders and its prognostic potential in preeclamptic patients. Am J Obstet Gynecol. 2012;206:e1–8.
Redman CW, Staff AC. Preeclampsia, biomarkers, syncytiotrophoblast stress, and placental capacity. Am J Obstet Gynecol. 2015;213:S9.e1–S9.e4.
Zeisler HZ, Llurba E, Chantraine F, Vatish M, Staff AC, Sennstrom M, et al. Predictive value of the sFlt-1:PlGF ratio in women with suspected preeclampsia. N Engl J Med. 2016;374:13–22.
Moore AG, Young H, Keller JM, Ojo LR, Yan J, Simas TA, et al. Angiogenic biomarkers for prediction of maternal and neonatal complications in suspected preeclampsia. J Matern Fetal Neonatal Med. 2012;25:2651–57.
Rana S, Powe CE, Salahuddin S, Verlohren S, Perschel FH, Levine RJ, et al. Angiogenic factors and the risk of adverse outcomes in women with suspected preeclampsia. Circulation. 2012;125:911–19.
McElrath TF, Lim KH, Pare E, Rich-Edwards J, Pucci D, Troisi R, et al. Longitudinal evaluation of predictive value for preeclampsia of circulating angiogenic factors through pregnancy. Am J Obstet Gynecol. 2012;207:407.e1–7.
Furuta I, Umazume T, Kojima T, Chiba K, Nakagawa K, Hosokawa A, et al. Serum placental growth factor and soluble fms-like tyrosine kinase 1 at mid-gestation in healthy women: Association with small-for-gestational age neonates. J Obstet Gynaecol Res. 2017;43:1152–58.
Herraiz I, Droge LA, Gomez-Montes E, Henirch W, Galindo A, Verlohren S. Characterization of the soluble fms-like tyrosine kinase-1 to placental growth factor ratio in pregnancies complicated by fetal growth restriction. Obstet Gynecol. 2014;124:265–73.
Honigberg MC, Cantonwine DE, Thomas AM, Lim KH, Parry SI, McElrath TF. Analysis of changes in maternal circulating angiogenic factors throughout pregnancy for the prediction of preeclampsia. J Perinatol. 2016;36:172–77.
PlGF-based testing to help diagnosed suspected preeclampsia. May 2016. Available at: https://www.nice.org.uk/guidance/dg23/chapter/1-Recommendations. [Accessed 20 April 2017].
Di Martino D, Cetin I, Frusca T, Ferrazzi E, Fuse F, Gervasi MT, et al. Italian Advisory Board: sFlt-1/PlGF ratio and preeclampsia, state of the art and developments in diagnostic, therapeutic, and clinical management. Eur J Obstet Gynecol Reprod Biol. 2016;206:70–3.
Chaiworapongsa T, Romero R, Whitten AE, Korzeniewski SJ, Chaemsaithong P, Hernandez-Andrade E, et al. The use of angiogenic biomarkers in maternal blood to identify which SGA fetuses will require preterm delivery and mothers who will develop preeclampsia. J Matern Fetal Neonatal Med. 2016;29:1214–28.
Acknowledgements
This research was supported by an unrestricted grant from Abbott Diagnostics Division (9MZ-04-06N03).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Honigberg, M.C., Seely, E.W., Thomas, A.M. et al. Infant size and the association between maternal circulating angiogenic factors and preeclampsia. J Perinatol 38, 456–461 (2018). https://doi.org/10.1038/s41372-018-0074-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-018-0074-2
This article is cited by
-
Hypothesis: human trophectoderm biopsy downregulates the expression of the placental growth factor gene
Journal of Assisted Reproduction and Genetics (2021)