Abstract
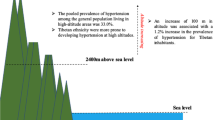
We aimed to evaluate the association of altitudes with the prevalence of hypertension among residents aged 15 years and above in Tibet, China. Data for 11,407 Tibetan residents from the National Health Services Survey in 2013 were analyzed. Association between altitudes and prevalence of physician-diagnosed hypertension was assessed by two logistic regression models as follows: (i) a base model adjusted for age and gender, and (ii) a full model additionally adjusted for body mass index, education, marital status, area of residence, distance to the nearest medical institute, smoking, drinking, and exercise. Nonlinear relationship between altitudes and prevalence of hypertension was explored by restricted cubic spline analyses. Sensitivity analyses were conducted by restricting to residents of rural and/or nomadic areas. The prevalence of hypertension was estimated to be 37.6%. We found a U-shaped association between altitudes and prevalence of physician-diagnosed hypertension with a turning point at around 3800 m (12,467 ft). For residents living above 3800 m, a 1000 m increase in altitudes was associated with 2.05 (95% confidence interval [CI]: 1.62–2.61) times higher odds of having physician-diagnosed hypertension, after adjusting for age and gender. When further controlling for all covariates, the odds ratio (OR) dropped to 1.87 (95% CI: 1.46–2.41). For residents living below 3800 m, a 1000 m increase was associated with 0.29 (95% CI: 0.19–0.44) times less likelihood of having physician-diagnosed hypertension in the full model. Sensitivity analyses among residents in rural and/or nomadic areas showed similar associations. To conclude, altitudes were in a U-shaped association with prevalence of hypertension.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Forouzanfar MH, Liu P, Roth GA, Ng M, Biryukov S, Marczak L, et al. Global burden of hypertension and systolic blood pressure of at least 110 to 115 mm Hg, 1990-2015. JAMA. 2017;317:165–82.
Mills KT, Bundy JD, Kelly TN, Reed JE, Kearney PM, Reynolds K, et al. Global disparities of hypertension prevalence and control: a systematic analysis of population-based studies from 90 countries. Circulation. 2016;134:441–50.
Wang J, Zhang L, Wang F, Liu L, Wang H.China National Survey of Chronic Kidney Disease Working Group. Prevalence, awareness, treatment, and control of hypertension in China: results from a national survey. Am J Hypertens. 2014;27:1355–61.
Lu J, Lu Y, Wang X, Li X, Linderman GC, Wu C, et al. Prevalence, awareness, treatment, and control of hypertension in China: data from 1.7 million adults in a population-based screening study (China PEACE Million Persons Project). Lancet. 2017;390:2549–58.
Duoji ZW, Jianhua People’s life. In: Duoji ZW, Jianhua W, editors. Tibet Statistical Yearbook 2018. Beijing, China: China Statistics Press; 2018.
Deji Dawapuchi, Danzeng Zhuoma, Xiaoduoji. [Prevalence of hypertension among 30 to 70 years old citizens of Lhasa, Tibet China]. Zhonghua Xin Xue Guan Bing Za Zhi. 2010;38:755–8.
Sherpa LY, Deji, Stigum H, Chongsuvivatwong V, Nafstad P, Bjertness E. Prevalence of metabolic syndrome and common metabolic components in high altitude farmers and herdsmen at 3700 m in Tibet. High Alt Med Biol. 2013;14:37–44.
Xu S, Jiayong Z, Li B, Zhu H, Chang H, Shi W, et al. Prevalence and clustering of cardiovascular disease risk factors among Tibetan adults in China: a population-based study. PLoS ONE. 2015;10:e0129966.
Zhao X, Li S, Ba S, He F, Li N, Ke L, et al. Prevalence, awareness, treatment, and control of hypertension among herdsmen living at 4,300 m in Tibet. Am J Hypertens. 2012;25:583–9.
Zheng X, Yao DK, Zhuo-Ma CR, Tang J, Wang TR, Zhang HH, et al. Prevalence, self-awareness, treatment, and control of hypertension in Lhasa, Tibet. Clin Exp Hypertens. 2012;34:328–33.
Parati G, Agostoni P, Basnyat B, Bilo G, Brugger H, Coca A, et al. Clinical recommendations for high altitude exposure of individuals with pre-existing cardiovascular conditions: a joint statement by the European Society of Cardiology, the Council on Hypertension of the European Society of Cardiology, the European Society of Hypertension, the International Society of Mountain Medicine, the Italian Society of Hypertension and the Italian Society of Mountain Medicine. Eur Heart J. 2018;39:1546–54.
Bärtsch P, Gibbs JS. Effect of altitude on the heart and the lungs. Circulation. 2007;116:2191–202.
Donegani E, Hillebrandt D, Windsor J, Gieseler U, Rodway G, Schöffl V, et al. Pre-existing cardiovascular conditions and high altitude travel. Consensus statement of the Medical Commission of the Union Internationale des Associations d’Alpinisme (UIAA MedCom) Travel Medicine and Infectious Disease. Travel Med Infect Dis. 2014;12:237–52.
Messerli-Burgy N, Meyer K, Steptoe A, Laederach-Hofmann K. Autonomic and cardiovascular effects of acute high altitude exposure after myocardial infarction and in normal volunteers. Circ J. 2009;73:1485–91.
Parati G, Bilo G, Faini A, Bilo B, Revera M, Giuliano A, et al. Changes in 24 h ambulatory blood pressure and effects of angiotensin II receptor blockade during acute and prolonged high-altitude exposure: a randomized clinical trial. Eur Heart J. 2014;35:3113–22.
Boussuges A, Molenat F, Burnet H, Cauchy E, Gardette B, Sainty JM, et al. Operation Everest III (Comex ‘97): modifications of cardiac function secondary to altitude-induced hypoxia. An echocardiographic and Doppler study. Am J Respir Crit Care Med. 2000;161:264–70.
Bilo G, Villafuerte FC, Faini A, Anza-Ramirez C, Revera M, Giuliano A, et al. Ambulatory blood pressure in untreated and treated hypertensive patients at high altitude: the High Altitude Cardiovascular Research-Andes study. Hypertension. 2015;65:1266–72.
Hanna JM. Climate, altitude, and blood pressure. Hum Biol. 1999;71:553–82.
Mazzeo RS, Wolfel EE, Butterfield GE, Reeves JT. Sympathetic response during 21 days at high altitude (4,300 m) as determined by urinary and arterial catecholamines. Metabolism. 1994;43:1226–32.
Siques P, Brito J, Banegas JR, Leon-Velarde F, de la Cruz-Troca JJ, Lopez V, et al. Blood pressure responses in young adults first exposed to high altitude for 12 months at 3550 m. High Alt Med Biol. 2009;10:329–35.
Aryal N, Weatherall M, Bhatta YK, Mann S. Blood pressure and hypertension in adults permanently living at high altitude: a systematic review and meta-analysis. High Alt Med Biol. 2016;17:185–93.
Marticorena E, Ruiz L, Severino J, Galvez J, Penaloza D. Systemic blood pressure in white men born at sea level: changes after long residence at high altitudes. Am J Cardiol. 1969;23:364–8.
Mingji C, Onakpoya IJ, Perera R, Ward AM, Heneghan CJ. Relationship between altitude and the prevalence of hypertension in Tibet: a systematic review. Heart. 2015;101:1054–60.
Center for Health Statistics and Information Network. An Analysis Report of National Health Services Survey in China, 2013. Beijing, China: Center for Health Statistics and Information, NHFPC; 2016.
Li C, Liu T, Sun W, Wu L, Zou ZY, Li C, et al. Prevalence and risk factors of arthritis in a middle-aged and older Chinese population: the China health and retirement longitudinal study. Rheumatology. 2015;54:697–706.
Feng XL, Pang M, Beard J. Health system strengthening and hypertension awareness, treatment and control: data from the China Health and Retirement Longitudinal Study. Bull World Health Organ. 2014;92:29–41.
Murakami D. Tourism development and propaganda in contemporary Lhasa, Tibet Autonomous Region (TAR), China. In: Asian Tourism: Growth and Change. 55–67. London: Elsevier, 2007.
Niu Y. Tourist resources and tourism development in Tibet. Sci Resources. 2002;24:31–6.
Yang KJ, Mei, Chen Yaling. Study on tourist destination image of Tibet based on online travel notes. Financ Econ Xinjiang. 2013;6:60–5.
Durrleman S, Simon R. Flexible regression models with cubic splines. Stat Med. 1989;8:551–61.
Xue B, Pamidimukkala J, Lubahn DB, Hay M. Estrogen receptor-alpha mediates estrogen protection from angiotensin II-induced hypertension in conscious female mice. Am J Physiol Heart Circ Physiol. 2007;292:H1770–6.
Hinton AO, He Y, Xia Y, Xu P, Yang Y, Saito K, et al. Estrogen receptor-α in the medial amygdala prevents stress-induced elevations in blood pressure in females. Hypertension. 2016;67:1321–30.
Dasgupta C, Chen M, Zhang H, Yang S, Zhang L. Chronic hypoxia during gestation causes epigenetic repression of the estrogen receptor-alpha gene in ovine uterine arteries via heightened promoter methylation. Hypertension. 2012;60:697–704.
Yildirim AO, Bulau P, Zakrzewicz D, Kitowska KE, Weissmann N, Grimminger F, et al. Increased protein arginine methylation in chronic hypoxia: role of protein arginine methyltransferases. Am J Respir Cell Mol Biol. 2006;35:436–43.
Klahr S. The role of nitric oxide in hypertension and renal disease progression. Nephrol Dial Transpl. 2001;16(Suppl 1):60–2.
Fish JE, Yan MS, Matouk CC, St Bernard R, Ho JJ, Gavryushova A, et al. Hypoxic repression of endothelial nitric-oxide synthase transcription is coupled with eviction of promoter histones. J Biol Chem. 2010;285:810–26.
Li K, Liang Y, Sun Y, Zhang LX, Yi X, Chen Y, et al. The relationship between polymorphisms at 17 gene sites and hypertension among the Aboriginal Tibetan people. Biomed Environ Sci. 2012;25:526–32.
Acknowledgements
This study was supported by the China Medical Board (CMB) (Project ID:11-086), Tibet’s Health Human Resource Development Research (Project ID: 201804), and Tibet University university-level Cultivation Fund (Project ID: 0800013).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Labasangzhu, L., Zhang, R., Qi, Y. et al. The U-shaped association of altitudes with prevalence of hypertension among residents in Tibet, China. J Hum Hypertens 35, 546–555 (2021). https://doi.org/10.1038/s41371-020-0367-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41371-020-0367-8
This article is cited by
-
Trends and regional variations in chronic diseases and their risk factors in China: an observational study based on National Health Service Surveys
International Journal for Equity in Health (2023)
-
Prevalence of hypertension and its relationship with altitude in highland areas: a systematic review and meta-analysis
Hypertension Research (2022)
-
The association between altitude and the prevalence of hypertension among permanent highlanders
Hypertension Research (2022)
-
Impact of Increased Hemoglobin on Spontaneous Intracerebral Hemorrhage
Neurocritical Care (2022)