Abstract
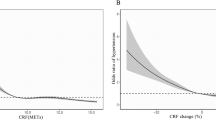
The combination of having a low physical performance and obesity results in a vicious cycle, but the effect of this combination on the incidence of hypertension is still unknown. This article aims to examine the effect of obesity and low physical performance on the incidence of hypertension in older adults. The sample was comprised of 349 Chinese community-dwelling participants (199 women; mean age 66.30 ± 5.78 years) without hypertension at baseline. Obesity was defined as having a body mass index (BMI) greater than or equal to 28 kg/m2. Participants scoring in the top 20% on the Timed Up and Go Test (TUGT) or in the slowest 20% of the 4-m walking test were defined as having a low physical performance. The outcome was new onset hypertension at the 1-year follow-up. We found that 89 (25.5%) of the 349 participants without hypertension at baseline had developed hypertension at their 1-year follow-up. After multivariate adjustments, it was found that the incidence of hypertension was associated with the combination of obesity and having a low physical performance (OR = 7.30, 95% CI = 1.36–39.11), but not solely with obesity (OR = 1.40, 95% CI = 0.68–2.88) or solely with low physical performance (OR = 0.98, 95% CI = 0.29–3.27). Hence, although obesity and low physical performance did not independently affect the incidence of hypertension after one year, the combination of the two can significantly increase the incidence of hypertension in Chinese community-dwelling older adults.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others

References
Zhang Y, Zhou Z, Gao J, Wang D, Zhang Q, Zhou Z, et al. Health-related quality of life and its influencing factors for patients with hypertension: evidence from the urban and rural areas of Shaanxi Province, China. BMC Health Serv Res. 2016; 16:277.
Sheng CS, Liu M, Kang YY, Wei FF, Zhang L, Li GL, et al. Prevalence, awareness, treatment and control of hypertension in elderly Chinese. Hypertens Res. 2013;36:824–8.
Collaborators GRF. Global, regional, and national comparative risk assessment of 79 behavioural, environmental and occupational, and metabolic risks or clusters of risks, 1990–2015: a systematic analysis for the Global Burden of Disease Study 2015. Lancet 2016;388:1659–724.
Yang X, Yang G, Li W, Zhang Y, Wang J. Therapeutic effect of Ilex hainanensis Merr. extract on essential hypertension: a systematic review and meta-analysis of randomized controlled trials. Front Pharm. 2018;9:424.
Prospective Studies Collaboration, Whitlock G, Lewington S, Sherliker P, Clarke R, Emberson J, et al. Body-mass index and cause-specific mortality in 900 000 adults: collaborative analyses of 57 prospective studies. Lancet. 2009;373:1083–96.
Wang Y, Wang QJ. The prevalence of prehypertension and hypertension among US adults according to the new joint national committee guidelines: new challenges of the old problem. Arch Intern Med. 2004;164:2126–34.
Ma WJ, Tang JL, Zhang YH, Xu YJ, Lin JY, Li JS, et al. Hypertension prevalence, awareness, treatment, control, and associated factors in adults in southern China. Am J Hypertens. 2012;25:590–6.
Flegal KM, Kit BK, Orpana H, Graubard BI. Association of all-cause mortality with overweight and obesity using standard body mass index categories. JAMA. 2013;309:71–82.
Veronese N, Cereda E, Solmi M, Fowler SA, Manzato E, Maggi S, et al. Inverse relationship between body mass index and mortality in older nursing home residents: a meta-analysis of 19,538 elderly subjects. Obes Rev. 2015;16:1001–15.
Wang J, Taylor AW, Zhang T, Appleton S, Shi Z. Association between body mass index and all-cause mortality among oldest old Chinese. J Nutr Health Aging. 2018;22:262–8.
Emmerzaal TL, Kiliaan AJ, Gustafson DR. 2003-2013: a decade of body mass index, alzheimer’s disease, and dementia. J Alzheimers Dis. 2015;43:739–55.
Yu R, Wong M, Leung J, Lee J, Auyeung TW, Woo J. Incidence, reversibility, risk factors and the protective effect of high body mass index against sarcopenia in community-dwelling older Chinese adults. Geriatr Gerontol Int. 2014;14(Suppl 1):15–28.
Han P, Zhao J, Guo Q, Wang J, Zhang W, Shen S, et al. Incidence, risk factors, and the protective effect of high body mass index against sarcopenia in suburb-dwelling elderly Chinese populations. J Nutr Health Aging. 2016;20:1056–60.
Busch TDA, Duarte YA, Pires Nunes D, Lebrão ML, Satya Naslavsky M, Dos Santos Rodrigues A. et al. Factors associated with lower gait speed among the elderly living in a developing country: a cross-sectional population-based study. BMC Geriatr. 2015;15:35.
Rosano C, Longstreth WT, Boudreau R, Taylor CA, Du Y, Kuller LH, et al. High blood pressure accelerates gait slowing in well-functioning older adults over 18-years of follow-up. J Am Geriatr Soc. 2011;59:390–7.
Dumurgier J, Elbaz A, Dufouil C, Tavernier B, Tzourio C. Hypertension and lower walking speed in the elderly: the three-city study. J Hypertens. 2010;28:1506–14.
Odden MC, Peralta CA, Berlowitz DR, Johnson KC, Whittle J, Kitzman DW, et al. Effect of intensive blood pressure control on gait speed and mobility limitation in adults 75 years or older. JAMA Intern Med. 2017;177:500–7.
Forhan M, Gill SV. Obesity, functional mobility and quality of life. Best Pr Res Cl En. 2013;27:129–37.
de Munter JS, Tynelius P, Ahlström G, Rasmussen F. The bidirectional association between body weight and mobility disability: a population based cohort. Disabil Health J 2016;9:632–7.
Craig CL, Marshall AL, Sjöström M, Bauman AE, Booth ML, Ainsworth BE, et al. International physical activity questionnaire: 12-Country reliability and validity. Med Sci Sports Exerc. 2003;35:1381–95.
Zhang W, Shen S, Wang W, Zhou C, Xu L, Qiu J, et al. Poor lower extremity function was associated with Pre-Diabetes and diabetes in older chinese people. PLoS One. 2014;9:e115883.
Writing Group of 2010 Chinese Guidelines for the Management of Hypertension 2010 Chinese guidelines for the management of hypertension. Chin J Hypertens. 2011;19:701–43.
Zhou BF. China CMGO. Predictive values of body mass index and waist circumference for risk factors of certain related diseases in chinese adults - study on optimal cut-off points of body mass index and waist circumference in chinese adults. Biomed Environ Sci. 2002;15:83–96.
Lauretani F, Russo CR, Bandinelli S, Bartali B, Cavazzini C, Di Iorio A, et al. Age-associated changes in skeletal muscles and their effect on mobility: an operational diagnosis of sarcopenia. J Appl Physiol. 1985;2003:1851–60.
Shimada H, Suzuki T, Suzukawa M, Makizako H, Doi T, Yoshida D, et al. Performance-based assessments and demand for personal care in older Japanese people: a cross-sectional study. BMJ Open. 2013;3:e2424.
Ishii S, Tanaka T, Shibasaki K, Ouchi Y, Kikutani T, Higashiguchi T, et al. Development of a simple screening test for sarcopenia in older adults. Geriatr Gerontol Int. 2014;14:93–101.
Li CI, Li TC, Lin WY, Liu CS, Hsu CC, Hsiung CA, et al. Combined association of chronic disease and low skeletal muscle mass with physical performance in older adults in the Sarcopenia and Translational Aging Research in Taiwan (START) study. BMC Geriatr. 2015;15:11.
Dauphinot V, Roche F, Kossovsky MP, Schott A, Pichot V, Gaspoz J, et al. C-reactive protein implications in new-onset hypertension in a healthy population initially aged 65 years: the proof study. J Hypertens. 2009;27:736–43.
Fujii M, Ohnishi H, Saitoh S, Akasaka H, Miura T, Mori M. The combination of abdominal obesity and high-sensitivity C-reactive protein predicts new-onset hypertension in the general Japanese population: the Tanno-Sobetsu study. Hypertens Res. 2015;38:426–32.
Gupta S, Kapoor S. Optimal cut-off values of anthropometric markers to predict hypertension in north indian population. J Commun Health. 2012;37:441–7.
Nguyen TT, Adair LS, He K, Popkin BM. Optimal cutoff values for overweight: using body mass index to predict incidence of hypertension in 18- to 65-year-old Chinese adults1,2. J Nutr. 2008;138:1377–82.
Nyamdorj R. BMI compared with central obesity indicators in relation to diabetes and hypertension in asians. Obes (Silver Spring) 2008;16:1622–35.
Uchiyama A, Shimizu T, Nakagawa T, Tanaka T. Association of hypertension with changes in the body mass index of university students. Environ Health Prev Med. 2008;13:271–80.
Chen PC, Sung FC, Su TC, Chien KL, Hsu HC, Lee YT. Two-year change in body mass index and subsequent risk of hypertension among men and women in a Taiwan community. J Hypertens. 2009;27:1370–6.
Luo W, Chen F, Guo Z, Wu M, Hao C, Zhou Z, et al. Comparison of the suitability of 2 years change in waist circum- ference and body mass index in predicting hypertension risk: a prospective study in Chinese-Han. Iran J Public Health. 2014;43:1212–20.
Zanchetti A, Facchetti R, Cesana GC, Modena MG, Pirrelli A, Sega R, et al. Menopause-related blood pressure increase and its relationship to age and body mass index: the SIMONA epidemiological study. J Hypertens. 2005;23:2269–76.
Welmer AK, Angleman S, Rydwik E, Fratiglioni L, Qiu C. Association of cardiovascular burden with mobility limitation among elderly people: a population-based study. PLoS One. 2013;8:e65815.
Odden MC, Peralta CA, Haan MN, Covinsky KE. Rethinking the association of high blood pressure with mortality in elderly adults. Arch Intern Med. 2012;172:1162–8.
Ostir GV, Markides KS, Black SA, Goodwin JS. Lower body functioning as a predictor of subsequent disability among older Mexican Americans. J Gerontol A Biol Sci Med Sci. 1998;53:M491–5.
Bohannon RW, DePasquale L. Physical Functioning Scale of the Short-Form (SF) 36: internal consistency and validity with older adults. J Geriatr Phys Ther. 2010;33:16–18.
Anandacoomarasamy A, Caterson I, Sambrook P, Fransen M, March L. The impact of obesity on the musculoskeletal system. Int J Obes. 2008;32:211–22.
Guh DP, Zhang W, Bansback N, Amarsi Z, Birmingham CL, Anis AH. The incidence of co-morbidities related to obesity and overweight: a systematic review and meta-analysis. BMC Public Health. 2009;9:88.
Bell JA, Sabia S, Singh-Manoux A, Hamer M, Kivimaki M. Healthy obesity and risk of accelerated functional decline and disability. Int J Obes. 2017;41:866–72.
Neter JE, Stam BE, Kok FJ, Grobbee DE, Geleijnse JM. Influence of weight reduction on blood pressure. Hypertension. 2003;42:878–84.
Acknowledgements
The authors thank Guiyan Shao from the Chadian public health center and Xiaofang Ren from Hangu welfare house for providing place and organization.
Funding
This work was supported by the National Natural Science Foundation of China (81372118); the Hygiene and Health Commission of Shanghai Municipality (2019HP76).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Liu, Y., Chen, Y., Han, P. et al. Combined effect of obesity and low physical performance on the incidence of hypertension in Chinese community-dwelling older population. J Hum Hypertens 35, 970–977 (2021). https://doi.org/10.1038/s41371-020-00442-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41371-020-00442-y