Abstract
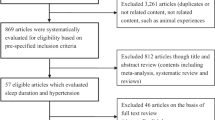
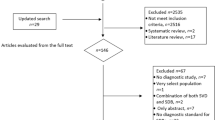
To deeply investigate the correlation between sleep duration and hypertension. The electronic databases Cochrane Library, Pubmed and Embase updated to December 2017 were retrieved, and manual searching for paper-based documents was also performed. After studies were selected according to the predefined screening criteria, their qualities were assessed using Newcastle-Ottawa Scale. Based on R 3.43 software, the association between sleep duration and hypertension was analyzed by dose-response meta-analysis, using relative risk (RR) and 95% confidence interval (95% CI) as effect indexes. Furthermore, publication bias of the eligible studies was evaluated using Egger’s test. In addition, sensitivity analysis was conducted through ignoring one study per time and then observing its influences on the pooled results. A total of 9 studies (involving 48525 objects) were included in this dose-response meta-analysis, which had high qualities. The differences in ≤5 h vs. 7 h, 6 h vs. 7 h, and 9 h vs. 7 h groups had statistical significances, suggesting that hypertension risk was higher for shorter sleep duration (P < 0.05). There was no significant difference in >9 h vs. 7 h group. No publication bias was found for the eligible studies, indicating that our results were highly credible (t = 0.030, P = 0.9766). However, the pooled results were reversed after ignoring each included study per time. Dose-response meta-analysis showed that the hypertension risk reduced for 0.3207% when the sleep duration increased by 1 h. Shorter sleep duration contributes to the increase of hypertension risk.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Riley M, Bluhm B. High blood pressure in children and adolescents. Am Fam Physician. 2012;85:693.
Lackland DT, Weber MA. Global burden of cardiovascular disease and stroke: hypertension at the core. Can J Cardiol. 2015;31:569–71.
Mendis S, Puska P, Norrving B. Global atlas on cardiovascular disease prevention and control. Geneva: World Health Organization, 2011.
Hernandorena I, Duron E, Vidal J, Hanon O. Treatment options and considerations for hypertensive patients to prevent dementia. Expert Opin Pharmacother. 2017;18:989–1000.
Guptamalhotra M, Banker A, Shete S, Hashmi SS, Tyson JE, Barratt MS, et al. Essential hypertension vs. secondary hypertension among children. Am J Hypertens. 2015;28:73–80.
Poulter NR, Prabhakaran D, Caulfield M. Hypertension. Lancet. 2015;386:801–12.
Sox HC. Assessing the trustworthiness of the guideline for management of high blood pressure in adults. JAMA. 2014;311:472–4.
Mensah GA, Bakris GTreatment. and Control of high blood pressure in adults. Cardiol Clin. 2010;28:609–22.
Campbell NR, Lackland DT, Lisheng L, Niebylski ML, Nilsson PM, Zhang XH. Using the Global Burden of Disease study to assist development of nation-specific fact sheets to promote prevention and control of hypertension and reduction in dietary salt: a resource from the World Hypertension League. J Clin Hypertens. 2015;17:165–7.
Gottlieb DJ, Redline S, Nieto FJ, Baldwin CM, Newman AB, Resnick HE, et al. Association of usual sleep duration with hypertension: the Sleep Heart Health Study. Sleep. 2006;29:1009–14.
Vgontzas AN, Liao D, Bixler EO, Chrousos GP, Vela-Bueno A. Insomnia with objective short sleep duration is associated with a high risk for hypertension. Sleep. 2009;32:491–7.
Fernandezmendoza J, Vgontzas AN, Liao D, Shaffer ML, Velabueno A, Basta M, et al. Insomnia with objective short sleep duration and incident hypertension: the penn state cohort. Hypertension. 2012;60:929.
Stranges S, Dorn JM, Cappuccio FP, Donahue RP, Rafalson LB, Hovey KM, et al. A population-based study of reduced sleep duration and hypertension: the strongest association may be in premenopausal women. J Hypertens. 2010;28:896–902.
Eguchi K, Pickering TG, Schwartz JE, Hoshide S, Ishikawa J, Ishikawa S, et al. Short sleep duration as an independent predictor of cardiovascular events in Japanese patients with hypertension. Arch Intern Med. 2008;168:2225–31.
Jf VDB, Tulen JH, Neven AK, Hofman A, Miedema HM, Witteman JC, et al. Sleep duration and hypertension are not associated in the elderly. Hypertension. 2007;50:585.
Wang Q, Xi B, Liu M, Zhang Y, Fu M. Short sleep duration is associated with hypertension risk among adults: a systematic review and meta-analysis. Hypertens Res. 2012;35:1012–8.
Guo X, Zheng L, Wang J, Li Y, Xingang Z, et al. Epidemiological evidence for the links between sleep duration and high blood pressure: a systematic review and meta-analysis. Sleep Med. 2013;14:324.
Meng L, Zheng Y, Hui R. The relationship of sleep duration and insomnia to risk of hypertension incidence: a meta-analysis of prospective cohort studies. Hypertens Res. 2013;36:985–95.
Stang A. Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol. 2010;25:603–5.
Lau J, Ioannidis JP, Schmid CH. Quantitative synthesis in systematic reviews. Ann Intern Med. 1997;127:820–6.
Higgins J, Thompson SG, Deeks JJ, Altman DG. Measuring inconsistency in meta-analyses. Bmj. 2003;327:557–60.
Egger M, Smith GD, Phillips AN. Principles and procedures. Br Med J. 1997;315:1533–7.
Christian R, Florent B, Streibig JC, Daniel G. Dose-response analysis using R. PLoS One. 2015;10:e0146021.
Hallin M, Puri ML. A multivariate Wald-Wolfowitz rank test against serial dependence. Can J Stat. 2010;23:55–65.
Orsini N, Li R, Wolk A, Khudyakov P, Spiegelman D. Meta-analysis for linear and nonlinear dose-response relations: examples, an evaluation of approximations, and software. Am J Epidemiol. 2012;175:66.
Fung MM, Peters K, Ancoli-Israel S, Redline S, Stone KL, Barrett-Connor E. Total sleep time and other sleep characteristics measured by actigraphy do not predict incident hypertension in a cohort of community-dwelling older men. J Clin Sleep Med. 2013;9:585–91.
Gangwisch JE, Heymsfield SB, Bodenalbala B, Buijs RM, Kreier F, Pickering TG, et al. Short sleep duration as a risk factor for hypertension analyses of the first national health and nutrition examination survey. Hypertension. 2006;47:833.
Kim SJ, Lee SK, Kim SH, Yun CH, Kim JH, Thomas RJ, et al. Genetic association of short sleep duration with hypertension incidence--a 6-year follow-up in the Korean genome and epidemiology study. Circ J. 2012;76:907–13.
Lopez-Garcia E, Mhpharm RF, Pilar Guallar-Castillon MD, Leon-Muñoz L, Banegas JR, Fernando Rodriguez-Artalejo MD. Self-reported sleep duration and hypertension in older spanish adults. J Am Geriatr Soc. 2009;57:663–8.
Lu Y, Lu M, Dai H, Yang P, Smithgagen J, Miao R, et al. Lifestyle and risk of hypertension: follow-up of a young pre-hypertensive cohort. Int J Med Sci. 2015;12:605–12.
Song Q, Liu X, Wang X, Wu S. Age- and gender-specific associations between sleep duration and incident hypertension in a Chinese population: the Kailuan study. J Hum Hypertens. 2016;30:503.
Williams MA, Miller RS, Qiu C, Cripe SM, Gelaye B, Enquobahrie D. Associations of early pregnancy sleep duration with trimester-specific blood pressures and hypertensive disorders in pregnancy. Sleep. 2010;33:1363–71.
Wu X, Sun Y, Niu K, Wei Y, Bo B, Yu X, et al. Association of self-reported sleep duration and hypertension: Results of a Chinese prospective cohort study. Clin Exp Hypertens. 2016;38:1514–9.
Yadav D, Hyun DS, Ahn SV, Koh SB, Kim JY. A prospective study of the association between total sleep duration and incident hypertension. J Clin Hypertens. 2017;19:1550–7.
Gangwischm JE, Malaspina D, Posner K, Babiss LA, Heymsfield SB, Turner JB, et al. Insomnia and sleep duration as mediators of the relationship between depression and hypertension incidence. Am J Hypertens. 2010;23:62.
Friedman O, Bradley TD, Ruttanaumpawan P, Logan AG. Independent association of drug-resistant hypertension to reduced sleep duration and efficiency. Am J Hypertens. 2010;23:174.
Gangwisch JE, Feskanich D, Malaspina D, Shen S, Forman JP. Sleep duration and risk for hypertension in women: results from the nurses’ health study. Am J Hypertens. 2013;26:903–11.
Kuciene R, Dulskiene V. Associations of short sleep duration with prehypertension and hypertension among Lithuanian children and adolescents: a cross-sectional study. BMC Public Health. 2014;14:1–8.
Guo X, Zheng L, Li Y, Yu S, Liu S, Zhou X, et al. Association between sleep duration and hypertension among Chinese children and adolescents. Clin Cardiol. 2011;34:774–81.
Gangwisch JE. A review of evidence for the link between sleep duration and hypertension. Am J Hypertens. 2014;27:1235.
Bruno RM, Palagini L, Gemignani A, Virdis A, Di GA, Ghiadoni L, et al. Poor sleep quality and resistant hypertension. Sleep Med. 2013;14:1157.
Pascaline P, Le VM, Nicole M, Audrey P, Thierry P, Xuan-Lan N, et al. Cumulative association of obstructive sleep apnea severity and short sleep duration with the risk for hypertension. PLoS ONE. 2014;9:e115666.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Li, H., Ren, Y., Wu, Y. et al. Correlation between sleep duration and hypertension: a dose-response meta-analysis. J Hum Hypertens 33, 218–228 (2019). https://doi.org/10.1038/s41371-018-0135-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41371-018-0135-1
This article is cited by
-
Factors associated with habitual sleep duration in US adults with hypertension: a cross-sectional study of the 2015–2018 National Health and Nutrition Examination Survey
BMC Public Health (2022)
-
The association of nighttime sleep duration and daytime napping duration with hypertension in Chinese rural areas: a population-based study
Journal of Human Hypertension (2021)
-
The association between sleep duration and hypertension: a meta and study sequential analysis
Journal of Human Hypertension (2021)
-
Sleep and hypertension
Sleep and Breathing (2020)
-
Short sleep duration and the risk of hypertension: snoozing away high blood pressure?
Journal of Human Hypertension (2019)