Abstract
Background
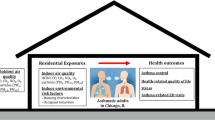
Americans spend most of their time indoors. Indoor particulate matter (PM) 2.5 µm and smaller (PM2.5) concentrations often exceed ambient concentrations. Therefore, we tested whether the use of an air purifying device (electrostatic precipitator, ESP) could reduce PM2.5 in homes of smokers with and without respiratory exacerbations, compared with baseline.
Methods
We assessed PM2.5 concentrations in homes of subjects with and without a recent (≤3 years) history of respiratory exacerbation. We compared PM2.5 concentrations during 1 month of ESP use with those during 1 month without ESP use.
Results
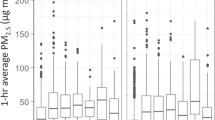
Our study included 19 subjects (53–80 years old), nine with a history of respiratory exacerbation. Geometric mean (GM) PM2.5 and median GM daily peak PM2.5 were significantly lower during ESP deployment compared with the equivalent time-period without the ESP (GSD = 0.50 and 0.37 µg/m3, respectively, p < 0.001). PM2.5 in homes of respiratory exacerbators tended (p < 0.14) to be higher than PM2.5 in homes of those without a history of respiratory exacerbation.
Conclusions
Subjects with a history of respiratory exacerbation tended to have higher mean, median, and mean peak PM2.5 concentrations compared with homes of subjects without a history of exacerbations. The ESP intervention reduced in-home PM2.5 concentrations, demonstrating its utility in reducing indoor exposures.
Novelty of study
Our work characterizes PM air pollution concentrations in homes of study subjects with and without respiratory exacerbations. We demonstrate that PM concentrations tend to be higher in homes of participants with respiratory exacerbations, and that the use of an inexpensive air purifier resulted in significantly lower daily average PM concentrations than when the purifier was not present. Our results provide a helpful intervention strategy for purifying indoor air and may be useful for susceptible populations.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 print issues and online access
$259.00 per year
only $43.17 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Code availability
To access the available code used in our analysis, please contact the corresponding author.
References
Horne BD, Joy EA, Hofmann MG, Gesteland PH, Cannon JB, Lefler JS, et al. Short-term elevation of fine particulate matter air pollution and acute lower respiratory infection. Am J Respir Crit Care Med. 2018;198:759–66.
Dockery DW, Pope CA. Acute respiratory effects of particulate air pollution. Annu Rev Public Health. 1994;15:107–32.
Peel JL, Tolbert PE, Klein M, Metzger KB, Flanders WD, Todd K, et al. Ambient air pollution and respiratory emergency department visits. Epidemiology. 2005;16:164–74.
Kim JJ, Smorodinsky S, Lipsett M, Singer BC, Hodgson AT, Ostro B. Traffic-related air pollution near busy roads: the East Bay Children’s Respiratory Health Study. Am J Respir Crit Care Med. 2004;170:520–6.
Clark NA, Demers PA, Karr CJ, Koehoorn M, Lencar C, Tamburic L, et al. Effect of early life exposure to air pollution on development of childhood asthma. Environ Health Perspect. 2010;118:284–90.
Ni L, Chuang C-C, Zuo L. Fine particulate matter in acute exacerbation of COPD. Front Physiol. 2015;6:294.
Kumar N, Liang D, Comellas A, Chu AD, Abrams T. Satellite-based PM concentrations and their application to COPD in Cleveland, OH. J Expo Sci Environ Epidemiol. 2013;23:637–46.
Sint T, Donohue JF, Ghio AJ. Ambient air pollution particles and the acute exacerbation of chronic obstructive pulmonary disease. Inhal Toxicol 2008;20:25–9.
Hansel NN, McCormack MC, Belli AJ, Matsui EC, Peng RD, Aloe C, et al. In-home air pollution is linked to respiratory morbidity in former smokers with chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2013;187:1085–90.
Klepeis NE, Nelson WC, Ott WR, Robinson JP, Tsang AM, Switzer P, et al. The National Human Activity Pattern Survey (NHAPS): a resource for assessing exposure to environmental pollutants. J Expo Sci Environ Epidemiol. 2001;11:231–52.
Wheeler AJ, Wallace LA, Kearney J, Van Ryswyk K, You H, Kulka R, et al. Personal, indoor, and outdoor concentrations of fine and ultrafine particles using continuous monitors in multiple residences. Aerosol Sci Technol. 2011;45:1078–89.
Gao M, Cao J, Seto E. A distributed network of low-cost continuous reading sensors to measure spatiotemporal variations of PM2. 5 in Xi’an, China. Environ Pollut 2015;199:56–65.
Jiao W, Hagler G, Williams R, Sharpe R, Brown R, Garver D, et al. Community Air Sensor Network (CAIRSENSE) project: evaluation of low-cost sensor performance in a suburban environment in the southeastern United States. Atmos Meas Tech. 2016;9:5281–92.
Ramachandran G, Adgate JL, Hill N, Sexton K, Pratt GC, Bock D. Comparison of short-term variations (15-minute averages) in outdoor and indoor PM2. 5 concentrations. J Air Waste Manag Assoc. 2000;50:1157–66.
Fromme H, Diemer J, Dietrich S, Cyrys J, Heinrich J, Lang W, et al. Chemical and morphological properties of particulate matter (PM10, PM2. 5) in school classrooms and outdoor air. Atmos Environ. 2008;42:6597–605.
Michaels RA, Kleinman MT. Incidence and apparent health significance of brief airborne particle excursions. Aerosol Sci Technol. 2000;32:93–105.
Adams H, Nieuwenhuijsen M, Colvile R, McMullen M, Khandelwal P. Fine particle (PM2.5) personal exposure levels in transport microenvironments, London, UK. Sci Total Environ. 2001;279:29–44.
Kingham S, Meaton J, Sheard A, Lawrenson O. Assessment of exposure to traffic-related fumes during the journey to work. Transp Res Part D. 1998;3:271–4.
Ruuskanen J, Tuch T, Ten Brink H, Peters A, Khlystov A, Mirme A, et al. Concentrations of ultrafine, fine and PM2.5 particles in three European cities. Atmos Environ. 2001;35:3729–38.
He K, Yang F, Ma Y, Zhang Q, Yao X, Chan CK, et al. The characteristics of PM2.5 in Beijing, China. Atmos Environ 2001;35:4959–70.
Onat B, Stakeeva B. Personal exposure of commuters in public transport to PM2.5 and fine particle counts. Atmos Pollut Res. 2013;4:329–35.
Karottki DG, Spilak M, Frederiksen M, Gunnarsen L, Brauner EV, Kolarik B, et al. An indoor air filtration study in homes of elderly: cardiovascular and respiratory effects of exposure to particulate matter. Environ Health 2013;12:116.
National Academies of Sciences, Engineering, Medicine. Sources of indoor particulate matter. Health risks of indoor exposure to particulate matter: workshop summary. National Academies Press (US), Washington (DC); 2016.
Parker GJ, Ong CH, Manges RB, Stapleton EM, Comellas AP, Peters TM, et al. A novel method to collect and chemically characterize milligram quantities of airborne indoor particulate matter. Aerosol Air Qual Res. 2019;19:2387–95.
Ong CH. Electrostatic precipitator to collect large quantities of particulate matter [MS]. Iowa City, IA: University of Iowa; 2017.
Parker KR. Why an electrostatic precipitator? In: Applied electrostatic precipitation. Springer, Dordrecht; 1997. p. 1–10.
McCain JD, Gooch JP, Smith WB. Results of field measurements of industrial particulate sources and electrostatic precipitator performance. J Air Pollut Control Assoc. 1975;25:117–21.
Sousan S, Koehler K, Hallett L, Peters TM. Evaluation of consumer monitors to measure particulate matter. J aerosol Sci. 2017;107:123–33.
Gordon T, Nadziejko C, Schlesinger R, Chen LC. Pulmonary and cardiovascular effects of acute exposure to concentrated ambient particulate matter in rats. Toxicol Lett. 1998;96:285–8.
Miyata R, van Eeden SF. The innate and adaptive immune response induced by alveolar macrophages exposed to ambient particulate matter. Toxicol Appl Pharmacol. 2011;257:209–26.
Xing Y-F, Xu Y-H, Shi M-H, Lian Y-X. The impact of PM2.5 on the human respiratory system. J Thorac Dis. 2016;8:E69.
McCain RW, Holden EP, Blackwell TR, Christman JW. Leukotriene B4 stimulates human polymorphonuclear leukocytes to synthesize and release interleukin-8 in vitro. Am J Respir Cell Mol Biol. 1994;10:651–7.
Marchini T, Magnani ND, Paz ML, Vanasco V, Tasat D, Maglio DG, et al. Time course of systemic oxidative stress and inflammatory response induced by an acute exposure to residual oil fly ash. Toxicol Appl Pharmacol. 2014;274:274–82.
Aarnio P, Yli-Tuomi T, Kousa A, Mäkelä T, Hirsikko A, Hämeri K, et al. The concentrations and composition of and exposure to fine particles (PM2. 5) in the Helsinki subway system. Atmos Environ. 2005;39:5059–66.
Pillarisetti A, Carter E, Rajkumar S, Young BN, Benka-Coker ML, Peel JL, et al. Measuring personal exposure to fine particulate matter (PM2. 5) among rural Honduran women: a field evaluation of the Ultrasonic Personal Aerosol Sampler (UPAS). Environ Int. 2019;123:50–3.
Mizuno A. Electrostatic precipitation. IEEE Trans Dielectr Electr Insul. 2000;7:615–24.
Lehtimäki M, Heinonen K. Reliability of electret filters. Build Environ. 1994;29:353–5.
Jaworek A, Krupa A, Sobczyk AT, Marchewicz A, Szudyga M, Antes T, et al. Submicron particles removal by charged sprays. Fundamentals. J Electrost. 2013;71:345–50.
Saiyasitpanich P, Keener TC, Khang S-J, Lu M. Removal of diesel particulate matter (DPM) in a tubular wet electrostatic precipitator. J Electrost. 2007;65:618–24.
Knol AB, de Hartog JJ, Boogaard H, Slottje P, van der Sluijs JP, Lebret E, et al. Expert elicitation on ultrafine particles: likelihood of health effects and causal pathways. Part Fibre Toxicol. 2009;6:19.
Kumar P, Morawska L, Birmili W, Paasonen P, Hu M, Kulmala M, et al. Ultrafine particles in cities. Environ Int. 2014;66:1–10.
McCormack MC, Belli AJ, Kaji DA, Matsui EC, Brigham EP, Peng RD, et al. Obesity as a susceptibility factor to indoor particulate matter health effects in COPD. Eur Respir J. 2015;45:1248–57.
Acknowledgements
We would like to thank all study participants for their willingness to maintain both the Foobot and ESP device throughout the study period.
Funding
This work was partly supported by the Origins of Cystic Fibrosis Airway Disease PPG grant (HL091842-11) funded by the National Institutes of Health. Additional funding for this study was provided by The University of Iowa Institute for Clinical and Translational Science, NIH U54 TR001356, and the Environmental Health Sciences Research Center, NIH P30 ES005605.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Stapleton, E.M., Simmering, J.E., Manges, R.B. et al. Continuous in-home PM2.5 concentrations of smokers with and without a history of respiratory exacerbations in Iowa, during and after an air purifier intervention. J Expo Sci Environ Epidemiol 30, 778–784 (2020). https://doi.org/10.1038/s41370-020-0235-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41370-020-0235-1