Abstract
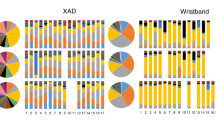
Exposure assessment in children, especially young children, presents difficulties not found with adults. Simple silicone wristbands are passive samplers that have potential applicability in exposure studies of children. We investigated the performance of silicone wristbands as personal nicotine samplers in two wristbands worn by a child (n = 31) for 7 days and for 2 days (worn day 5 to day 7). We compared levels of nicotine in wristbands with urinary cotinine, a metabolite of nicotine, measured in the child’s urine obtained on day 7. Children were recruited who were exposed to contaminants in tobacco smoke and/or vapor from electronic nicotine delivery systems (ENDS; commonly known as electronic cigarettes or EC) as well as children who lived in nonsmoking homes. Caregivers were interviewed to obtain reported measures of the child’s exposure. Analysis was by liquid chromatography with triple quadrupole mass spectrometry and isotope dilution (LC-MS/MS). The nicotine detected in the wristbands worn for 2 days was highly correlated with urinary cotinine concentration (df = 29, r2 = 0.741, p < 0.001), as was nicotine in wristbands worn for 7 days (df = 28, r2 = 0.804, p < 0.001). The 2- and 7-day wristband nicotine amounts were also significantly correlated (df = 28, r2 = 0.852, p < 0.001). Silicone wristbands may be a useful tool for epidemiological and intervention studies of tobacco product exposure in children.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 print issues and online access
$259.00 per year
only $43.17 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
O’Connell SG, Kind LD, Anderson KA. Silicone wristbands as personal passive samplers. Environ Sci Technol. 2014;48:3327–35.
Anderson KA, Points GL, Donald CE, Dixon HM, Scott RP, Wilson G, et al. Preparation and performance features of wristband samplers and considerations for chemical exposure assessment. J Expo Sci Environ Epidemiol. 2017;27:551–9.
Bergmann AJ, North PE, Vasquez L, Bello H, Ruiz MDG, Anderson KA. Multi-class chemical exposure in rural Peru using silicone wristbands. J Expo Sci Environ Epidemiol. 2017;27:560–8.
Paulik LB, Hobbie KA, Rohlman D, Smith BW, Scott RP, Kincl L, et al. Environmental and individual PAH exposures near rural natural gas extraction. Environ Pollut. 2018;241:397–405.
Donald CE, Scott RP, Blaustein KL, Halbleib ML, Sarr M, Jepson PC, Anderson KA. Silicone wristbands detect individuals’ pesticide exposures in West Africa. R Soc Open Sci. 2016;3:160433.
Dixon HM, Scott RP, Holmes D, Calero L, Kincl LD, Waters KM, et al. Silicone wristbands compared with traditional polycyclic aromatic hydrocarbon exposure assessment methods. Anal Bioanal Chem. 2018;410:3059–71.
Kile ML, Scott RP, O’Connell SG, Lipscomb S, MacDonald M, McClelland M, et al. Using silicone wristbands to evaluate preschool children’s exposure to flame retardants. Environ Res. 2016;147:365–72.
Hammel SC, Hoffman K, Webster TF, Anderson KA, Stapleton HM. Measuring personal exposure to organophosphate flame retardants using silicone wristbands and hand wipes. Environ Sci Technol. 2016;50:4483–91.
Lipscomb ST, McClelland MM, MacDonald M, Cardenas A, Anderson KA, Kile ML. Cross-sectional study of social behaviors in preschool children and exposure to flame retardants. Environ Health. 2017;16:23.
Hammel SC, Phillips AL, Hoffman K, Stapleton HM. Evaluating the use of silicone wristbands to measure personal exposure to brominated flame retardants. Environ. Sci. Technol. 2018;52:11875–11885
Homa DM, Neff LJ, King BA, Caraballo RS, Bunnell RE, Babb SD, et al. Vital signs: disparities in nonsmokers’ exposure to secondhand smoke—United States, 1999-2012. MMWR Morb Mortal Wkly Rep. 2015;64:103–8.
Kassem NO, Daffa RM, Liles S, Jackson SR, Kassem NO, Younis MA, et al. Children’s exposure to secondhand and thirdhand smoke carcinogens and toxicants in homes of hookah smokers. Nicotine Tob Res. 2014;16:961–75.
Durmowicz EL. The impact of electronic cigarettes on the paediatric population. Tob Control. 2014;23(Suppl 2):ii41.
Benowitz NL. Cotinine as a biomarker of environmental tobacco smoke exposure. Epidemiol Rev. 1996;18:188–204.
Avila-Tang E, Al-Delaimy WK, Ashley DL, Benowitz N, Bernert JT, Kim S, et al. Assessing secondhand smoke using biological markers. Tob Control. 2013;22:164–71.
Wilson SE, Kahn RS, Khoury J, Lanphear BP. Racial differences in exposure to environmental tobacco smoke among children. Environ Health Perspect. 2005;113:362–7.
Hubal EAC, Sheldon LS, Burke JM, McCurdy TR, Berry MR, Rigas ML, et al. Children’s exposure assessment: a review of factors influencing Children’s exposure, and the data available to characterize and assess that exposure. Environ Health Perspect. 2000;108:475–86.
Hukkanen J, Jacob P III, Benowitz NL. Metabolism and disposition kinetics of nicotine. Pharmacol Rev. 2005;57:79–115.
Benowitz NL, Hukkanen J, Jacob P 3rd. Nicotine chemistry, metabolism, kinetics and biomarkers. Handb Exp Pharmacol. 2009;192:29–60.
Hovell MF, Zakarian JM, Matt GE, Liles S, Jones JA, Hofstetter CR, et al. Counseling to reduce children’s secondhand smoke exposure and help parents quit smoking: a controlled trial. Nicotine Tob Res. 2009;11:1383–94.
Matt GE, Quintana PJ, Zakarian JM, Fortmann AL, Chatfield DA, Hoh E, et al. When smokers move out and non-smokers move in: residential thirdhand smoke pollution and exposure. Tob Control. 2011;20:e1.
Matt GE, Quintana PJE, Fortmann AL, Zakarian JM, Galaviz VE, Chatfield DA, et al. Thirdhand smoke and exposure in California hotels: non-smoking rooms fail to protect non-smoking hotel guests from tobacco smoke exposure. Tob Control. 2014;23:264–72.
Paya P, Anastassiades M, Mack D, Sigalova I, Tasdelen B, Oliva J, et al. Analysis of pesticide residues using the Quick Easy Cheap Effective Rugged and Safe (QuEChERS) pesticide multiresidue method in combination with gas and liquid chromatography and tandem mass spectrometric detection. Anal Bioanal Chem. 2007;389:1697–714.
Lehotay SJ, de Kok A, Hiemstra M, Van Bodegraven P. Validation of a fast and easy method for the determination of residues from 229 pesticides in fruits and vegetables using gas and liquid chromatography and mass spectrometric detection. J AOAC Int. 2005;88:595–614.
Matt GE, Quintana PJE, Hoh E, Zakarian JM, Chowdhury Z, Hovell MF, et al. A Casino goes smoke free: a longitudinal study of secondhand and thirdhand smoke pollution and exposure. Tob Control. 2018;27:643–649.
Matt GE, Quintana PJE, Zakarian JM, Hoh E, Hovell MF, Mahabee-Gittens M, et al. When smokers quit: exposure to nicotine and carcinogens persists from thirdhand smoke pollution. Tob Control. 2016;26:548–56.
Northrup TF, Khan AM, Jacob P III, Benowitz NL, Hoh E, Hovell MF, et al. Thirdhand smoke contamination in hospital settings: assessing exposure risk for vulnerable paediatric patients. Tob Control 2016;25:619–623.
Armbruster DA, Pry T. Limit of blank, limit of detection and limit of quantitation. Clin Biochem Rev. 2008;29(Suppl 1):S49–S52.
Code of Federal Regulations. 40 CFR Appendix B to Part 136—Definition and procedure for the determination of the method detection limit. Revision 1.11. US Federal Government; 2011.
Quintana PJ, Matt GE, Chatfield D, Zakarian JM, Fortmann AL, Hoh E. Wipe sampling for nicotine as a marker of thirdhand tobacco smoke contamination on surfaces in homes, cars, and hotels. Nicotine Tob Res. 2013;15:1555–63.
R Core Team. R: a language and environment for statistical computing Vienna, Austria: R Foundation for Statistical Computing; 2018. https://www.R-project.org/.
Wickham H. Elegant graphics for data analysis. New York: Springer-Verlag; 2016.
Aerts R, Joly L, Szternfeld P, Tsilikas K, De Cremer K, Castelain P, et al. Silicone wristband passive samplers yield highly individualized pesticide residue exposure profiles. Environ Sci Technol. 2018;52:298–307.
Kintz P, Henrich A, Cirimele V, Ludes B. Nicotine monitoring in sweat with a sweat patch. J Chromatogr B Biomed Sci Appl. 1998;705:357–61.
Sekine Y, Sato S, Kimura K, Sato H, Nakai S, Yanagisawa Y. Detection of tobacco smoke emanating from human skin surface of smokers employing passive flux sampler—GCMS system. J Chromatogr B Anal Technol Biomed Life Sci. 2018;1092:394–401.
Vidi PA, Anderson KA, Chen HY, Anderson R, Salvador-Moreno N, Mora DC, et al. Personal samplers of bioavailable pesticides integrated with a hair follicle assay of DNA damage to assess environmental exposures and their associated risks in children. Mutat Res. 2017;822:27–33.
Goniewicz ML, Knysak J, Gawron M, Kosmider L, Sobczak A, Kurek J, et al. Levels of selected carcinogens and toxicants in vapour from electronic cigarettes. Tob Control. 2014;23:133–9.
Acknowledgements
The authors express their gratitude to Christine Batikian, MPH, Viridiana Mendoza, Samuel Padilla, and Madeleine Warman for assisting with data collection, and Mansi Vyas for sample preparation. This research was supported by funds from the California Tobacco Related Disease Research Grants Program Office of the University of California, Grant Number 25IP-0023.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
KAA discloses a financial interest in MyExposome that is marketing products related to the research being reported. The terms of this arrangement have been reviewed and approved by Oregon State University in accordance with its policy on research conflict of interest. The remaining authors declare that they have no conflict of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Quintana, P.J.E., Hoh, E., Dodder, N.G. et al. Nicotine levels in silicone wristband samplers worn by children exposed to secondhand smoke and electronic cigarette vapor are highly correlated with child’s urinary cotinine. J Expo Sci Environ Epidemiol 29, 733–741 (2019). https://doi.org/10.1038/s41370-019-0116-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41370-019-0116-7
Keywords
This article is cited by
-
The Incidence of the XRCC1 rs25487 and PON1 rs662 Polymorphisms in a Population from Central Brazil: Patterns in an Area with a High Level of Agricultural Activity
Biochemical Genetics (2023)
-
Wearable Passive Samplers for Assessing Environmental Exposure to Organic Chemicals: Current Approaches and Future Directions
Current Environmental Health Reports (2023)
-
A systematic review of the use of silicone wristbands for environmental exposure assessment, with a focus on polycyclic aromatic hydrocarbons (PAHs)
Journal of Exposure Science & Environmental Epidemiology (2022)
-
Operationalizing the Exposome Using Passive Silicone Samplers
Current Pollution Reports (2022)
-
Altered microbiomes in thirdhand smoke-exposed children and their home environments
Pediatric Research (2021)