Abstract
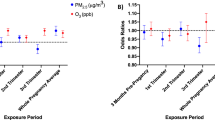
Our aim is to estimate associations between acute increases in particulate matter with diameter of 2.5 µm or less (PM2.5) concentrations and risk of infant bronchiolitis and otitis media among Massachusetts births born 2001 through 2008.Our case-crossover study included 20,017 infant bronchiolitis and 42,336 otitis media clinical encounter visits. PM2.5 was modeled using satellite, remote sensing, meteorological and land use data. We applied conditional logistic regression to estimate odds ratios (ORs) and confidence intervals (CIs) per 10-µg/m3 increase in PM2.5. We assessed effect modification to determine the most susceptible subgroups. Infant bronchiolitis risk was elevated for PM2.5 exposure 1 day (OR = 1.07, 95% CI = 1.03–1.11) and 4 days (OR = 1.04, 95% CI = 0.99–1.08) prior to clinical encounter, but not 7 days. Non-significant associations with otitis media varied depending on lag. Preterm infants were at substantially increased risk of bronchiolitis 1 day prior to clinical encounter (OR = 1.17, 95% CI = 1.08–1.28) and otitis media 4 and 7 days prior to clinical encounter (OR = 1.09, 95% CI = 1.02–1.16 and OR = 1.08, 95% CI = 1.02–1.15, respectively). In conclusion, preterm infants are most susceptible to infant bronchiolitis and otitis media associated with acute PM2.5 exposures.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 print issues and online access
$259.00 per year
only $43.17 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Krzyzanowski M, Cohen A, Anderson R. Quantification of health effects of exposure to air pollution. Occup Environ Med. 2002;59:791–93.
Pope CA III, Burnett RT, Thun MJ. Lung cancer, cardiopulmonary mortality, and long-term exposure to fine particulate air pollution. JAMA. 2002;287:1132–41.
Silva R, West J, Zhange Y, Anenberg SC, Lamarque JF, Shindell DT. Global premature mortality due to anthropogenic outdoor air pollution and the contribution of past climate change. Environ Res Lett. 2013;8:034005.
World Health Organization. Health aspects of air pollution: results from the WHO project “systematic review of air pollution in Europe”. Copenhagen:WHO; 2004.
Laden F, Schwartz J, Speizer FE. Reduction in fine particulate air pollution and mortality: extended follow-up of the Harvard Six Cities study. Am J Respir Crit Care Med. 2006;173:667–72.
US EPA Air quality criteria for ozone and related photochemical oxidants. Washington, DC: United States: Environmental Protection Agency; 2006.
Koehoorn M, Karr CJ, Demers PA, Lencar C, Tamburic L. Descriptive epidemiological features of bronchiolitis in a population-based cohort. Pediatrics. 2008;122:1196–203.
Rovers MM, Schilder AG, Zielhuis GA, Rosenfeld RM. Otitis media. Lancet. 2004;363:465–73.
Bacharier LB, Cohen R, Schweiger T, Yin-Declue H, Christie C, Zheng J, et al. Determinants of asthma after severe respiratory syncytial virus bronchiolitis. J Allergy Clin Immunol. 2012;130:91–100.
Karr CJ, Demers PA, Koehoorn MW, Lencar CC, Tamburic L, Brauer M. Influence of ambient air pollutant sources on clinical encounters for infant bronchiolitis. Am J Respir Crit Care Med. 2009;180:995–1001.
Semple MG, Taylor-Robinson DC, Lane S, Smyth RL. Household tobacco smoke and admission weight predict severe bronchiolitis in infants independent of deprivation: prospective cohort study. PLoS One. 2011;6:e22425.
Boyce TG, Mellen BG, Mitchel EF Jr, Wright PF, Griffin MR. Rates of hospitalization for respiratory syncytial virus infection among children in medicaid. J Pediatr. 2000;137:865–70.
Karr C, Lumly T, Sheperd K, Davis R, Larson T, Ritz B, et al. A case-crossover study of wintertime ambient air pollution and infant bronchiolitis. Environ Health Perspect. 2006;114:227–81.
Karr C, Lumley T, Schreuder A, Davis R, Larson T, Ritz B, et al. Effects of subchronic and chronic exposure to ambient air pollutants on infant bronchiolitis. Am J Epidemiol. 2007;165:553–60.
Vandini S, Corvaglia L, Alessandroni R, Aquilano G, Marsico C, Spinelli M, et al. Respiratory syncytial virus infection in infants and correlation with meteorological factors and air pollutants. Ital J Pediatr. 2013;39:1.
Coker TR, Chan LS, Newberry SJ, Limbos MA, Suttorp MJ, Shekelle PG, et al. Diagnosis, microbial epidemiology, and antibiotic treatment of acute otitis media in children: a systematic review. JAMA. 2010;304:2161.
Soni A. Ear infections (otitis media) in children (0–17): use and expenditures, 2006. Statistical Brief No. 228. Agency for Healthcare Research and Quality. 2007. http://www.meps.ahrq.gov/mepsweb/data_files/publications/st228/stat228.pdf. Accessed 12 Jan 2011.
Teele DW, Klein JO, Rosner B. Epidemiol of otitis media during the first seven years of life in children in greater Boston: a prospective, cohort study. J Infect Dis. 1989;160:83–94.
Costa JL, Navarro A, Neves JB, Martin M. Household wood and charcoal smoke increases risk of otitis media in childhood in Maputo. Int J Epidemiol. 2004;33:583–78.
Daigler GE, Markello SJ, Cummings KM. The effect of indoor air pollutants on otitis media and asthma in children. Laryngoscope. 1991;101:293–96.
DiFranza JR, Aligne CA, Weitzman M. Prenatal and postnatal environmental tobacco smoke exposure and children’s health. Pediatrics. 2004;113(4 Suppl):1007–15.
Lambert AL, Mangum JB, DeLorme MP, Everitt JI. Ultrafine carbon black particles enhance respiratory syncytial virus-induced airway reactivity, pulmonary inflammation, and chemokine expression. Toxicol Sci. 2003;73:339–46.
Brauer M, Gehring U, Brunekreef B, de Jongste J, Gerritsen J, Rovers M, et al. Traffic-related air pollution and otitis media. Environ Health Perspect. 2006;114:1414–8.
MacIntyre EA, Karr CJ, Koehoorn M, Demers PA, Tamburic L, Lencar C, et al. Residential air pollution and otitis media during the first two years of life. Epidemiol . 2011;22:81–9.
Aguilera I, Pedersen M, Garcia-Esteban R, Ballester F, Basterrechea M, Esplugues A, et al. Early-life exposure to outdoor air pollution and respiratory health, ear infections, and eczema in infants from the INMA study. Environ Health Perspect. 2013;121:387–92.
Goldman GT, Mulholland JA, Russell AG, Srivastava A, Strickland MJ, Klein M, et al. Ambient air pollutant measurement error: characterization and impacts in a time-series epidemiologic study in Atlanta. Environl. Sci Technol. 2010;44:7692–8.
Shapiro-Mendoza CK, Tomashek KM, Kotelchuck M, Barfield W, Nannini A, Weiss J, et al. Effect of late-preterm birth and maternal medical conditions on newborn morbidity risk. Pediatrics. 2008;121:223–7.
Girguis MS, Strickland MJ, Hu X, Liu Y, Bartell SM, Vieira VM, Maternal exposure to traffic-related air pollution and birth defects in Massachusetts. Environ Res. 2016;146:1–9.
Liu Y, Paciorek CJ, Koutrakis P. Estimating regional spatial and temporal variability of PM2.5 concentrations using satellite data, meteorology, and land use information. Environ Health Perspect. 2009;117:886–92.
Lee HJ, Liu Y, Coull BA, Schwartz J, Koutrakis P. A novel calibration approach of modis aod data to predict PM2.5 concentrations. Atmos Chem Phys. 2011;11:7991–8002.
Kloog I, Nordio F, Coull BA, Schwartz J. Predicting spatiotemporal mean air temperature using MODISsatelilte surface temperature measurements across the Northeastern USA. Remote Sense. 2014;150:132–9.
Cosgrove BA, Lohmann D, Mitchell KE, Houser PR, Wood EF, Schaake JC, et al. Real-time and retrospective forcing in the North American Land Data Assimilation System (NLDAS) project. J Geophys Res Atmos. 2003;108(D22).
Levy D, Lumley T, Sheppard L, Kaufman J, Checkoway H. Referent selection in case-crossover analyses of acute health effects of air pollution. Epidemiology . 2001;12:186–92.
Navidi W, Weinhadl E. Risk set sampling for case-crossover designs. Epidemiology. 2002;13:100–5.
Janes H, Sheppard L, Lumley T. Overlap bias in the case-crossover design, with application to air pollution exposures. Stat Med. 2005;24:285–300.
Tristram DA, Welliver RC. Respiratory syncytial virus. In: Long SS, Pickering LK, Prober CG, (eds.). Principles and practice of pediatric infectious diseases. 2nd ed. New York, NY: Churchill Livingstone; 2003. p. 213–8.
Lawn E, Gravett G, Nunes M, Rubens E, Stanton C. Global report on preterm birth and stillbirth (1 of 7): definitions, description of the burden and opportunities to improve data. BMC Pregnancy Childbirth. 2010;10(1):S1.
World Health Organization.2015. Air Pollution Ranking. 2014. Website http:faq/2015-05-16/world-health-organization-2014-air-pollution-ranking.
Glasser JR, Mallampalli RK. Surfactant and its role in the pathobiology of pulmonary infection. Microbes Infect. 2012;14:17–25.
Nkadi PO, Merritt TA, Pillers D-AM. An Overview of Pulmonary Surfactant in the Neonate: Genetics, Metabolism, and the Role of Surfactant in Health and Disease. Mol Genet Metab. 2009;97:95–101.
Shukla A, Timblin C, Berube K, Gordon T, McKinney W, Driscoll K, et al. Inhaled particulate matter causes expression of nuclear factor (NF)-kappaB-related genes and oxidant-dependent NF-kappaB activation in vitro. Am J Respir Cell Mol Biol. 2000;23:182–7.
Zemek R, Szyszkowicz M, Rowe BH. Air pollution and emergency department visits for otitis media: a case-crossover study in Edmonton, Canada. Environ Health Perspect. 2010;118:1631–6.
Cowling TE, Cecil EV, Soljak MA, Lee JT, Millett C, Majeed A, et al. Access to Primary Care and Visits to Emergency Departments in England: A Cross-Sectional, Population-Based Study. PLoS ONE. 2013;8:e66699.
Lesser J, Reich NG, Brookmeyer R, Perl TM, Nelson KE, Cummings DA. Incubation periods of acute respiratory viral infections: a systematic review. Lancet Inft Dises. 2009;9:291–300.
Funding
This work was supported by grant number 5R01ES019897 from the National Institute of Environmental Health (NIEHS). Its contents are solely the responsibility of the authors and do not necessarily represent the views of NIH. This work was partially supported by NASA Applied Sciences Program (grant no. NNX11AI53G to Y.L and X.H).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Girguis, M.S., Strickland, M.J., Hu, X. et al. Exposure to acute air pollution and risk of bronchiolitis and otitis media for preterm and term infants. J Expo Sci Environ Epidemiol 28, 348–357 (2018). https://doi.org/10.1038/s41370-017-0006-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41370-017-0006-9
This article is cited by
-
Exposure to outdoor particulate matter and risk of respiratory diseases: a systematic review and meta-analysis
Environmental Geochemistry and Health (2024)
-
Air pollution and bronchiolitis: a case–control study in Antwerp, Belgium
European Journal of Pediatrics (2024)
-
Particular matter influences the incidence of acute otitis media in children
Scientific Reports (2021)
-
Satellite Remote Sensing for Estimating PM2.5 and Its Components
Current Pollution Reports (2021)
-
Impact of air pollution on benign paroxysmal positional vertigo incidence: a retrospective study of the citizens of Seoul, South Korea
Environmental Science and Pollution Research (2021)