Abstract
Background
Obesity is major cause of cardiovascular diseases. Metabolically healthy obesity (MHO) may increase heart failure risk early in life, and may be reflected in impaired cardiac structure and function. Therefore, we aimed to examine the relationship between MHO in young adulthood and cardiac structure and function.
Methods
A total of 3066 participants from the Coronary Artery Risk Development in Young Adults (CARDIA) study were included, who completed echocardiography in young adulthood and middle age. The participants were grouped by obesity status (body mass index ≥30 kg/m2) and poor metabolic health (≥2 criteria for metabolic syndrome) into four metabolic phenotypes as follows: metabolically healthy non-obesity (MHN), MHO, metabolically unhealthy non-obesity (MUN), metabolically unhealthy obesity (MUO). The associations of the metabolic phenotypes (MHN serving as the reference) with left ventricular (LV) structure and function were evaluated using multiple linear regression models.
Results
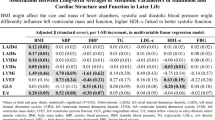
At baseline, mean age was 25 years, 56.4% were women, and 44.7% were black. After a follow-up 25 years, MUN in young adulthood was associated with worse LV diastolic function (E/é ratio, β [95% CI], 0.73 [0.18, 1.28]), worse systolic function (global longitudinal strain [GLS], 0.60 [0.08, 1.12]) in comparison with MHN. MHO and MUO were associated with LV hypertrophy (LV mass index, 7.49 g/m2 [4.63, 10.35]; 18.23 g/m2 [12.47, 23.99], respectively), worse diastolic function (E/é ratio, 0.67 [0.31, 1.02]; 1.47 [0.79, 2.14], respectively), and worse systolic function (GLS, 0.72 [0.38, 1.06]; 1.35 [0.64, 2.05], respectively) in comparison with MHN. These results were consistent in several sensitivity analyses.
Conclusions
In this community-based cohort using data from the CARDIA study, obesity in young adulthood was significantly associated with LV hypertrophy, worse systolic and diastolic function regardless of metabolic status.

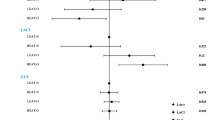
Relationship of Baseline Metabolic Phenotypes with Young Adulthood and Midlife Cardiac Structure and Function. Adjusted for year 0 covariates: age, sex, race, educational level, smoking status, drinking status, and physical activity; metabolically healthy non-obesity was used as a reference category for comparison. † Criteria for metabolic syndrome are listed in Supplementary Table S6. MUN metabolically unhealthy non-obesity, MHO metabolically healthy obesity, LVMi left ventricular mass index, LVEF left ventricular ejection fraction, E/A early to late peak diastolic mitral flow velocity ratio, E/é mitral inflow velocity to early diastolic mitral annular velocity, CI confidence interval.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
The data used and/or analyzed in this study are available to all researchers upon reasonable request.
References
Afshin A, Forouzanfar MH, Reitsma MB, Sur P, Estep K, Lee A, et al. Health effects of overweight and obesity in 195 countries over 25 years. N Engl J Med. 2017;377:13–27.
Kivimäki M, Kuosma E, Ferrie JE, Luukkonen R, Nyberg ST, Alfredsson L, et al. Overweight, obesity, and risk of cardiometabolic multimorbidity: pooled analysis of individual-level data for 120 813 adults from 16 cohort studies from the USA and Europe. Lancet Public Health. 2017;2:e277–e85.
Neeland IJ, Poirier P, Després JP. Cardiovascular and metabolic heterogeneity of obesity: clinical challenges and implications for management. Circulation. 2018;137:1391–406.
Wildman RP, Muntner P, Reynolds K, McGinn AP, Rajpathak S, Wylie-Rosett J, et al. The obese without cardiometabolic risk factor clustering and the normal weight with cardiometabolic risk factor clustering: prevalence and correlates of 2 phenotypes among the US population (NHANES 1999-2004). Arch Internal Med. 2008;168:1617–24.
Blüher M. Metabolically healthy obesity. Endocr Rev. 2020;41:bnaa004.
Commodore-Mensah Y, Lazo M, Tang O, Echouffo-Tcheugui JB, Ndumele CE, Nambi V, et al. High burden of subclinical and cardiovascular disease risk in adults with metabolically healthy obesity: the atherosclerosis risk in communities (ARIC) study. Diabetes Care. 2021;44:1657–63.
Zhou Z, Macpherson J, Gray SR, Gill JMR, Welsh P, Celis-Morales C, et al. Are people with metabolically healthy obesity really healthy? A prospective cohort study of 381,363 UK Biobank participants. Diabetologia. 2021;64:1963–72.
Heidenreich PA, Bozkurt B, Aguilar D, Allen LA, Byun JJ, Colvin MM, et al. 2022 AHA/ACC/HFSA guideline for the management of heart failure: a report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation. 2022;145:e895–e1032.
Wang YC, Liang CS, Gopal DM, Ayalon N, Donohue C, Santhanakrishnan R, et al. Preclinical systolic and diastolic dysfunctions in metabolically healthy and unhealthy obese individuals. Circ Heart Fail. 2015;8:897–904.
Dobson R, Burgess MI, Sprung VS, Irwin A, Hamer M, Jones J, et al. Metabolically healthy and unhealthy obesity: differential effects on myocardial function according to metabolic syndrome, rather than obesity. Int J Obesity. 2016;40:153–61.
Lee HJ, Kim HL, Lim WH, Seo JB, Kim SH, Zo JH, et al. Subclinical alterations in left ventricular structure and function according to obesity and metabolic health status. PloS One. 2019;14:e0222118.
Wang Y, Liang J, Zheng S, He A, Chen C, Zhao X, et al. Combined associations of obesity and metabolic health with subclinical left ventricular dysfunctions: Danyang study. ESC Heart Fail. 2021;8:3058–69.
Tsai MC, Lee CC, Liu SC, Tseng PJ, Chien KL. Combined healthy lifestyle factors are more beneficial in reducing cardiovascular disease in younger adults: a meta-analysis of prospective cohort studies. Sci Rep. 2020;10:18165.
Friedman GD, Cutter GR, Donahue RP, Hughes GH, Hulley SB, Jacobs DR Jr, et al. CARDIA: study design, recruitment, and some characteristics of the examined subjects. J Clin Epidemiol. 1988;41:1105–16.
Physical status: the use and interpretation of anthropometry. Report of a WHO Expert Committee. World Health Organ Tech Rep Ser. 1995;854:1–452.
Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults. Executive summary of the third report of the National Cholesterol Education Program (NCEP) expert panel on detection, evaluation, and treatment of high blood cholesterol in adults (Adult Treatment Panel III). JAMA. 2001;285:2486–97.
Armstrong AC, Ricketts EP, Cox C, Adler P, Arynchyn A, Liu K, et al. Quality control and reproducibility in M-mode, two-dimensional, and speckle tracking echocardiography acquisition and analysis: the CARDIA study, year 25 examination experience. Echocardiography. 2015;32:1233–40.
Gidding SS, Xie X, Liu K, Manolio T, Flack JM, Gardin JM. Cardiac function in smokers and nonsmokers: the CARDIA study. The Coronary Artery Risk Development in Young Adults Study. J Am Coll Cardiol. 1995;26:211–6.
Ward ZJ, Bleich SN, Cradock AL, Barrett JL, Giles CM, Flax C, et al. Projected U.S. state-level prevalence of adult obesity and severe obesity. N Engl J Med. 2019;381:2440–50.
Kishi S, Armstrong AC, Gidding SS, Colangelo LA, Venkatesh BA, Jacobs DR Jr, et al. Association of obesity in early adulthood and middle age with incipient left ventricular dysfunction and structural remodeling: the CARDIA study (Coronary Artery Risk Development in Young Adults). JACC Heart Fail. 2014;2:500–8.
Wormser D, Kaptoge S, Di Angelantonio E, Wood AM, Pennells L, Thompson A, et al. Separate and combined associations of body-mass index and abdominal adiposity with cardiovascular disease: collaborative analysis of 58 prospective studies. Lancet. 2011;377:1085–95.
Lanoye A, Brown KL, LaRose JG. The transition into young adulthood: a critical period for weight control. Curr Diab Rep. 2017;17:114.
Visseren FLJ, Mach F, Smulders YM, Carballo D, Koskinas KC, Bäck M, et al. 2021 ESC Guidelines on cardiovascular disease prevention in clinical practice. Eur Heart J. 2021;42:3227–337.
Kuk JL, Ardern CI. Are metabolically normal but obese individuals at lower risk for all-cause mortality? Diabetes Care. 2009;32:2297–9.
van Vliet-Ostaptchouk JV, Nuotio ML, Slagter SN, Doiron D, Fischer K, Foco L, et al. The prevalence of metabolic syndrome and metabolically healthy obesity in Europe: a collaborative analysis of ten large cohort studies. BMC Endocrine Disorders. 2014;14:9.
Slagter SN, Corpeleijn E, van der Klauw MM, Sijtsma A, Swart-Busscher LG, Perenboom CWM, et al. Dietary patterns and physical activity in the metabolically (un)healthy obese: the Dutch Lifelines cohort study. Nutr J. 2018;17:18.
Velho S, Paccaud F, Waeber G, Vollenweider P, Marques-Vidal P. Metabolically healthy obesity: different prevalences using different criteria. Eur J Clin Nutr. 2010;64:1043–51.
Lin H, Zhang L, Zheng R, Zheng Y. The prevalence, metabolic risk and effects of lifestyle intervention for metabolically healthy obesity: a systematic review and meta-analysis: a PRISMA-compliant article. Medicine. 2017;96:e8838.
Mulye TP, Park MJ, Nelson CD, Adams SH, Irwin CE Jr, Brindis CD. Trends in adolescent and young adult health in the United States. J Adolesc Health. 2009;45:8–24.
Eckel N, Li Y, Kuxhaus O, Stefan N, Hu FB, Schulze MB. Transition from metabolic healthy to unhealthy phenotypes and association with cardiovascular disease risk across BMI categories in 90 257 women (the Nurses’ Health Study): 30 year follow-up from a prospective cohort study. Lancet Diabetes Endocrinol. 2018;6:714–24.
Lee YB, Kim DH, Kim SM, Kim NH, Choi KM, Baik SH, et al. Hospitalization for heart failure incidence according to the transition in metabolic health and obesity status: a nationwide population-based study. Cardiovasc Diabetol. 2020;19:77.
Bray GA, Heisel WE, Afshin A, Jensen MD, Dietz WH, Long M, et al. The science of obesity management: an endocrine society scientific statement. Endocr Rev. 2018;39:79–132.
Khera R, Pandey A, Chandar AK, Murad MH, Prokop LJ, Neeland IJ, et al. Effects of weight-loss medications on cardiometabolic risk profiles: a systematic review and network meta-analysis. Gastroenterology. 2018;154:1309–19.e7.
Kramer CK, Zinman B, Retnakaran R. Are metabolically healthy overweight and obesity benign conditions? A systematic review and meta-analysis. Ann Internal Med. 2013;159:758–69.
Eckel N, Meidtner K, Kalle-Uhlmann T, Stefan N, Schulze MB. Metabolically healthy obesity and cardiovascular events: a systematic review and meta-analysis. Eur J Prev Cardiol. 2016;23:956–66.
Acknowledgements
We thank all the staff and participants of the CARDIA study for their contributions. This study was supported by the National Natural Science Foundation of China (81870195, 82070384 to XL; 81900329 to YG), Guangdong Basic and Applied Basic Research Foundation (2019A1515011582, 2021A1515011668 to XL; 2019A1515011098, 2022A1515010416 to YG).
Author information
Authors and Affiliations
Contributions
XL, LP, PW and ML conceived and designed the study. XL, LP, PW, ML, XZ, ZX, YG, LH, ZZ and ZC contributed to the acquisition, analysis and interpretation of the data. PW and ML were responsible for writing the manuscript. All authors contributed to revising the manuscript draft for important intellectual content and approved the final submitted manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, P., Liu, M., Zhuang, X. et al. Association of metabolically healthy obesity in young adulthood with myocardial structure and function. Int J Obes 47, 399–405 (2023). https://doi.org/10.1038/s41366-023-01288-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-023-01288-3