Abstract
Background/Objectives
Body composition and protein-energy partitioning changes are important factors of body weight regulation, but have not been studied in the context of clinical obesity treatment setting. Thus, the aim of the present study was to investigate the pattern of body weight loss, body composition, and energy partitioning changes during a 9-month multidisciplinary weight loss program and 4-month follow up and to test the associations among these changes in adolescents with severe obesity.
Subjects/Methods
Twenty-five adolescents (14.1 ± 1.5 years old; 13 girls) with severe obesity joined a pediatric obesity center for a 9-month inpatient multidisciplinary weight loss program. All participants performed body composition assessment (i.e. fat mass-FM, and fat-free mass-FFM) and completed a 36-h session in indirect calorimetric chamber before the start (T0), at the end of the intervention (T1) and 4 months follow-up to the intervention (T2). The protein-energy partitioning (P ratio) was calculated as urinary nitrogen loss/total energy expenditure over 24 hours.
Interventions
9-month individualized multidisciplinary weight loss program consisting of lifestyle education, psychological support, physical activity, and dietary intervention.
Results
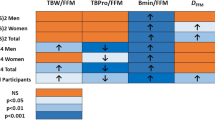
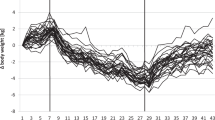
Initial P ratio was positively associated with changes in body weight from T0 to T1 (p = 0.038). The changes in FFM/FM were negatively associated with body weight changes in boys (p = 0.006) from T0 to T1 and in girls (p < 0.001) from T1 to T2. Urinary nitrogen excretion (p < 0.001) and total energy expenditure (p < 0.001) significantly decreased during the weight loss program while the P ratio did not significantly change.
Conclusion
The present results suggest that baseline and changes in energy partitioning may be associated with changes in body weight in adolescents with severe obesity. In addition, sexual dimorphism in these patterns of change suggest the need for specific dietary and physical activity strategies in boys and girls to optimize body weight loss and to prevent or slow weight regain.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Zaki ME, El-Bassyouni HT, El-Gammal M, Kamal S. Indicators of the metabolic syndrome in obese adolescents. Arch Med Sci. 2015;11:92–98.
Graf C, Ferrari N. Metabolic Syndrome in Children and Adolescents. Visc Med. 2016;32:357–62.
Bianchini JAA, Da Silva DF, Nardo CCS, Carolino IDR, Hernandes F, Junior NN. Multidisciplinary therapy reduces risk factors for metabolic syndrome in obese adolescents. Eur J Pediatr. 2013;172:215–21.
Caranti DA, de Mello MT, Prado WL, Tock L, Siqueira KO, de Piano A, et al. Short- and long-term beneficial effects of a multidisciplinary therapy for the control of metabolic syndrome in obese adolescents. Metabolism. 2007;56:1293–1300.
Gueugnon C, Mougin F, Simon-Rigaud ML, Regnard J, Nègre V, Dumoulin G. Effects of an in-patient treatment program based on regular exercise and a balanced diet on high molecular weight adiponectin, resistin levels, and insulin resistance in adolescents with severe obesity. Appl Physiol Nutr Metab. 2012;37:672–9.
Ryder JR, Kaizer AM, Jenkins TM, Kelly AS, Inge TH, Shaibi GQ. Heterogeneity in Response to Treatment of Adolescents with Severe Obesity: The Need for Precision Obesity Medicine. Obesity. 2019;27:288–94.
Greenway FL. Physiological adaptations to weight loss and factors favouring weight regain. Int J Obes. 2015;39:1188–96.
Payne PR, Dugdale AE. A model for the prediction of energy balance and body weight. Ann Hum Biol. 1977;4:525–35.
Payne PR, Dugdale AE. MECHANISMS FOR THE CONTROL OF BODY-WEIGHT. Lancet. 1977;309:583–6.
Dugdale AE, Payne PR. Pattern of lean and fat deposition in adults [15]. Nature. 1977;266:349–51.
Forbes GB Lean Body Mass‐Body Fat Interrelationships in Humans. Nutr Rev. 1987. https://doi.org/10.1111/j.1753-4887.1987.tb02684.x.
Dulloo AG, Jacquet J. The control of partitioning between protein and fat during human starvation: Its internal determinants and biological significance. Br J Nutr. 1999;82:339–56.
Dulloo AG, Jacquet J, Girardier L. Autoregulation of body composition during weight recovery in human: The Minnesota Experiment revisited. Int J Obes. 1996;20:393–405.
Lazzer S, Boirie Y, Montaurier C, Vernet J, Meyer M, Vermorel M. A weight reduction program preserves fat-free mass but not metabolic rate in obese adolescents. Obes Res. 2004;12:233–40.
Lazzer S, Vermorel M, Montaurier C, Meyer M, Boirie Y. Changes in adipocyte hormones and lipid oxidation associated with weight loss and regain in severely obese adolescents. Int J Obes. 2005;29:1184–91.
Lazzer S, Boirie Y, Poissonnier C, Petit I, Duché P, Taillardat M, et al. Longitudinal changes in activity patterns, physical capacities, energy expenditure, and body composition in severely obese adolescents during a multidisciplinary weight-reduction program. Int J Obes. 2005;29:37–46.
Lazzer S, Meyer M, Derumeaux H, Boirie Y, Vermorel M. [Longitudinal changes in body composition and basal metabolic rate in institutionalized or domiciled obese adolescents]. Arch Pediatr. 2005;12:1349–57.
Montaurier C, Richard R, Boirie Y. Two Functional Calorimetric Chambers in France Complete the Room Indirect Calorimetry Operating and Reporting Standards (RICORS) 1.0 Guide List. Obesity. 2021;29:631.
Brouwer E Report of the sub-committee on constants and factors. In: KL B (ed). Energy metabolism. Academic Press: New-York; 1965, pp 441–3.
Rothman KJ. No adjustments are needed for multiple comparisons. Epidemiology. 1990;1:43–46.
Bender R, Lange S. Adjusting for multiple testing - When and how? J Clin Epidemiol. 2001;54:343–9.
Feise RJ. Do multiple outcome measures require p-value adjustment? BMC Med Res Methodol. 2002;2:1–4.
Peyrot N, Morin J-B, Thivel D, Isacco L, Taillardat M, Belli A, et al. Mechanical work and metabolic cost of walking after weight loss in obese adolescents. Med Sci Sports Exerc. 2010;42. https://doi.org/10.1249/MSS.0b013e3181da8d1e.
Mendelson M, Borowik A, Michallet AS, Perrin C, Monneret D, Faure P, et al. Sleep quality, sleep duration and physical activity in obese adolescents: effects of exercise training. Pediatr Obes. 2016;11:26–32.
Julian V, Isacco L, Khammassi M, Fillon A, Miguet M, Dutheil F, et al. Appetite control might not be improved afterweight loss in adolescents with obesity, despite non-persistent metabolic syndrome. Nutrients. 2020;12:1–13.
Roche J, Gillet V, Perret F, Mougin F. Obstructive sleep apnea and sleep architecture in adolescents with severe obesity: Effects of a 9-month lifestyle modification program based on regular exercise and a balanced diet. J Clin Sleep Med. 2018;14:967–76.
Millward DJ, Truby H, Fox KR, Livingstone MBE, Macdonald IA, Tothill P. Sex differences in the composition of weight gain and loss in overweight and obese adults. Br J Nutr. 2014;111:933–43.
Diaz EO, Prentice AM, Goldberg GR, Murgatroyd PR, Coward WA. Metabolic response to experimental overfeeding in lean and overweight healthy volunteers. Am J Clin Nutr. 1992;56:641–55.
Norgan NG, Durnin JVGA. The effect of 6 weeks of overfeeding on the body weight, body composition, and energy metabolism of young men. Am J Clin Nutr. 1980;33:978–88.
Bouchard C, Tremblay A, Després J-P, Nadeau A, Lupien PJ, Thériault G, et al. The Response to Long-Term Overfeeding in Identical Twins. N Engl J Med. 1990;322:1477–82.
Dulloo AG, Jacquet J, Montani J-P. Pathways from weight fluctuations to metabolic diseases: focus on maladaptive thermogenesis during catch-up fat. Int J Obes Relat Metab Disord. 2002;26:S46–S57.
Dulloo AG, Jacquet J, Miles-Chan JL, Schutz Y. Passive and active roles of fat-free mass in the control of energy intake and body composition regulation. Eur J Clin Nutr. 2017;71:353–7.
Dulloo AG, Jacquet J, Girardier L. Poststarvation hyperphagia and body fat overshooting in humans: a role for feedback signals from lean and fat tissues. Am J Clin Nutr. 1997;65:717–23.
Turicchi J, O’Driscoll R, Finlayson G, Duarte C, Hopkins M, Martins N, et al. Associations between the proportion of fat-free mass loss during weight loss, changes in appetite, and subsequent weight change: Results from a randomized 2-stage dietary intervention trial. Am J Clin Nutr. 2020;111:536–44.
Acknowledgements
We are grateful to the adolescents who participated in this study and their parents. We thank the Centre Medical Infantile de Romagnat and the CRNH for their support.
Author information
Authors and Affiliations
Contributions
The conception and design of the study: SL, MV, YB; Acquisition of data: SL, CM, MV, YB; Analysis and interpretation of data: LI, SL, BP, FR, YB, DT; Drafting the article: LI, DT; Revising it critically for important intellectual content: SL, NF, FR, YB; Final approval of the version to be submitted: all authors.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Isacco, L., Lazzer, S., Pereira, B. et al. Association of protein-energy partitioning with body weight and body composition changes in adolescents with severe obesity. Int J Obes 46, 2021–2028 (2022). https://doi.org/10.1038/s41366-022-01218-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-022-01218-9