Abstract
Background
This study aimed to investigate the influence of body weight, exercise modality, and pace on physiological and perceptual responses to determine the relation between perceptual and physiological responses.
Methods
Aerobically untrained, normal weight, and overweight males and females participated. Participants were randomly assigned to one exercise condition for a 1-mile walk.
Results
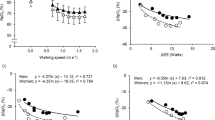
Prescribed pace resulted in a greater physiological stress than self-selected pace (all p < 0.001) through blood lactate (1.3 ± 0.4 vs 1.7 ± 0.5 mmol), systolic blood pressure (128.9 ± 10.3 vs 139.2 ± 13.2 mmHg), heart rate recovery (2.1 ± 1.7 vs 4.5 ± 2.6 min), oxygen consumption (15.1 ± 2.6 vs 18.1 ± 3.6 ml/kg/min), heart rate (111.7 ± 16.6 vs 134.4 ± 8.3 bpm), and energy expenditure (5.5 ± 1.4 vs 6.8 ± 1.7 kcal/min). Overweight individuals exhibited higher values than normal weight for heart rate (113 ± 8.8 vs 125.5 ± 13.2 bpm, p < 0.001), percentage of max heart rate (60.7 vs 69.0%, p < 0.001), percent of VO2peak (42.2 vs 55.6%, p < 0.001), and total energy expenditure (100.9 ± 27.4 vs 114.1 ± 33.5 kcal, p = 0.022). Greater perceived effort was seen on a treadmill (6.3 ± 0.5 vs 12.5 ± 2.0 RPE, p < 0.001) and at prescribed pace (6.5 ± 1.1 vs 8.9 ± 1.9 RPE, p < 0.001).
Conclusion
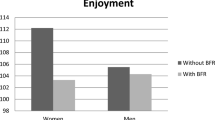
A novel finding of this study was the increased physiological stress and perception of effort on a treadmill and at a prescribed pace, while total energy expenditure showed no significant differences. This could indicate an unfavorable perception and less affective response to the treadmill modality. These results indicate exercise at self-selected pace in preferred environments promotes enjoyable experiences with similar health benefits as those during prescribed higher intensity exercise.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Dunn AL, Marcus BH, Kampert JB, Garcia ME, Kohl HW 3rd, Blair SN. Comparison of lifestyle and structured interventions to increase physical activity and cardiorespiratory fitness: a randomized trial. JAMA. 1999;281:327–34.
Greene NP, Lambert BS, Greene ES, Carbuhn AF, Green JS, Crouse SF. Comparative efficacy of water and land treadmill training for overweight or obese adults. Med Sci Sports Exerc. 2009;41:1808–15.
Cox KL, Burke V, Gorely TJ, Beilin LJ, Puddey IB. Controlled comparison of retention and adherence in home- vs center-initiated exercise interventions in women ages 40-65 years: the S.W.E.A.T. Study (Sedentary Women Exercise Adherence Trial). Prev Med. 2003;36:17–29.
Freitas LAG, Ferreira SDS, Freitas RQ, Januario RSB, Alves RC, Silva AC, et al. Effect of self-selected and imposed-intensity walking programs on fat oxidation in obese women. J Exerc Physiol Online. 2015;18:62–70.
Physical Activity Guidelines Advisory Committee. Physical activity guidelines advisory committee report, 2008. Nutr Rev. 2009;67:114–20.
Haskell WL, Lee IM, Pate RR, Powell KE, Blair SN, Franklin BA, et al. Physical activity and public health: updated recommendation for adults from the American College of Sports Medicine and the American Heart Association. Med Sci Sports Exerc. 2007;39:1423–34.
Browning RC, Baker EA, Herron JA, Kram R. Effects of obesity and sex on the energetic cost and preferred speed of walking. J Appl Physiol. 2006;100:390–8.
Morris C, Garner J, Owens S, Valliant M, Debusk H, Loftin M. A prospective study comparing distance-based vs. time-based exercise prescriptions of walking and running in previously sedentary overweight adults. Int J Exerc Sci. 2017;10:782–97.
Peyrot N, Thivel D, Isacco L, Morin JB, Belli A, Duche P. Why does walking economy improve after weight loss in obese adolescents? Med Sci Sports Exerc. 2012;44:659–65.
Donnelly JE, Blair SN, Jakicic JM, Manore MM, Rankin JW, Smith BK. American College of Sports Medicine Position Stand. Appropriate physical activity intervention strategies for weight loss and prevention of weight regain for adults. Med Sci Sports Exerc. 2009;41:459–71.
Loftin M, Waddell DE, Robinson JH, Owens SG. Comparison of energy expenditure to walk or run a mile in adult normal weight and overweight men and women. J Strength Conditioning Res. 2010;24:2794–8.
Manson JE, Greenland P, LaCroix AZ, Stefanick ML, Mouton CP, Oberman A, et al. Walking compared with vigorous exercise for the prevention of cardiovascular events in women. N Engl J Med. 2002;347:716–25.
Antoniewicz F, Brand R. Dropping out or keeping up? Early-dropouts, late-dropouts, and maintainers differ in their automatic evaluations of exercise already before a 14-week exercise course. Front Psychol. 2016;7:838.
Hall CW, Holmstrup ME, Koloseus J, Anderson D, Kanaley JA. Do overweight and obese individuals select a “moderate intensity” workload when asked to do so? J Obes. 2012;2012:919051.
Caserta MS, Gillett PA. Older women’s feelings about exercise and their adherence to an aerobic regimen over time. Gerontologist. 1998;38:602–9.
Baldwin AS, Kangas JL, Denman DC, Smits JA, Yamada T, Otto MW. Cardiorespiratory fitness moderates the effect of an affect-guided physical activity prescription: a pilot randomized controlled trial. Cogn Behav Ther. 2016;45:445–57.
Jung ME, Bourne JE, Little JP. Where does HIT fit? An examination of the affective response to high-intensity intervals in comparison to continuous moderate- and continuous vigorous-intensity exercise in the exercise intensity-affect continuum. PLoS ONE. 2014;9:e114541.
Garber CE, Blissmer B, Deschenes MR, Franklin B, Lamonte MJ, Lee IM, et al. American College of Sports Medicine position stand. Quantity and quality of exercise for developing and maintaining cardiorespiratory, musculoskeletal, and neuromotor fitness in apparently healthy adults: guidance for prescribing exercise. Med Sci Sports Exerc. 2011;43:1334–59.
Ekblom O, Ekblom-Bak E, Rosengren A, Hallsten M, Bergstrom G, Borjesson M. Cardiorespiratory fitness, sedentary behaviour and physical activity are independently associated with the metabolic syndrome, results from the SCAPIS Pilot Study. PLoS ONE. 2015;10:e0131586.
American College of Sports Medicine. ACSM’s guidelines for exercise testing and prescription. Philadelphia: Lippincott Williams & Wilkins; 2017.
Abe D, Yoshida T, Ueoka H, Sugiyama K, Fukuoka Y. Relationship between perceived exertion and blood lactate concentrations during incremental running test in young females. BMC Sports Sci Med Rehabil. 2015;7:5.
Buckley JD, Bourdon PC, Woolford SM. Effect of measuring blood lactate concentrations using different automated lactate analysers on blood lactate transition thresholds. J Sci Med Sport. 2003;6:408–21.
Coutts AJ, Rampinini E, Marcora SM, Castagna C, Impellizzeri FM. Heart rate and blood lactate correlates of perceived exertion during small-sided soccer games. J Sci Med Sport. 2009;12:79–84.
Medbo JI, Mamen A, Holt Olsen O, Evertsen F. Examination of four different instruments for measuring blood lactate concentration. Scand J Clin Lab Investig. 2000;60:367–80.
Browning RC, Kram R. Energetic cost and preferred speed of walking in obese vs. normal weight women. Obes Res. 2005;13:891–9.
Ali S, Bhatti A, Khan H, Jan R. Correlation between pre and post exercise blood lactate and pH. Gomal. J Med Sci. 2008;6:1–3.
Goodwin ML, Harris JE, Hernandez A, Gladden LB. Blood lactate measurements and analysis during exercise: a guide for clinicians. J Diabetes Sci Technol. 2007;1:558–69.
Marcora S. Perception of effort during exercise is independent of afferent feedback from skeletal muscles, heart, and lungs. J Appl Physiol. 2009;106:2060–2.
Dasilva SG, Guidetti L, Buzzachera CF, Elsangedy HM, Krinski K, DeCampos W, et al. Psychophysiological responses to self-paced treadmill and overground exercise. Med Sci Sports Exerc. 2011;43:1114–24.
Lind E, Joens-Matre RR, Ekkekakis P. What intensity of physical activity do previously inactivity middle-aged women select? Evidence of a coherent pattern from physiological, perceptual, and affective markers. Prev Med. 2005;40:407–19.
Levinger I, Bronks R, Cody DV, Linton I, Davie A. Perceived exertion as an exercise intensity indicator in chronic heart failure patients on beta-blockers. J Sports Sci Med. 2004;3:23–27.
Perri MG, Anton SD, Durning PE, Ketterson TU, Sydeman SJ, Berlant NE, et al. Adherence to exercise prescriptions: effects of prescribing moderate versus higher levels of intensity and frequency. Health Psychol. 2002;21:452–8.
Ekkekakis P, Lind E. Exercise does not feel the same when you are overweight: the impact of self-selected and imposed intensity on affect and exertion. Int J Obes. 2006;30:652–60.
Garcin M, Mille-Hamard L, Billat V. Influence of aerobic fitness level on measured and estimated perceived exertion during exhausting runs. Int J Sports Med. 2004;25:270–7.
Lewis JE, Nash MS, Hamm LF, Martins SC, Groah SL. The relationship between perceived exertion and physiologic indicators of stress during graded arm exercise in persons with spinal cord injuries. Arch Phys Med Rehabil. 2007;88:1205–11.
Figard-Fabre H, Fabre N, Leonardi A, Schena F. Physiological and perceptual responses to Nordic walking in obese middle-aged women in comparison with the normal walk. Eur J Appl Physiol. 2010;108:1141–51.
Ceci R, Hassmen P. Self-monitored exercise at three different RPE intensities in treadmill vs field running. Med Sci Sports Exerc. 1991;23:732–8.
Author information
Authors and Affiliations
Contributions
All authors have made significant contributions to research design, data collection and analysis, and development of the manuscript. RG: developed study design, conducted all data collection, and made significant contribution to manuscript development and revision. RB: made significant contribution to manuscript development and revision in all sections. ML: assisted in study design and data collection along with development of the “Methods” section of the manuscript. MEH: assisted in development of all sections and reviewing of manuscript. JG: conducted data filtering and statistical analysis and also contributed significantly to manuscript review and revisions.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Galloway, R., Booker, R., Loftin, M. et al. Physiological and perceptual responses during walking at set and preferred pace in normal and overweight adults. Int J Obes 46, 100–106 (2022). https://doi.org/10.1038/s41366-021-00963-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-021-00963-7