Abstract
Background
Successful long-term weight loss maintenance after caloric restriction (CR) is rarely achieved. Besides known metabolic, behavioural, and cognitive factors, 24-hour energy expenditure (24hEE) relative to body size (i.e., metabolic efficiency) might influence subsequent weight loss maintenance.
Methods
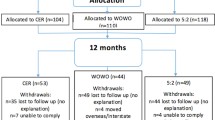
Eleven participants with obesity (BMI = 39.0 ± 8.7 kg/m2, body fat = 36.1 ± 6.4%) had 24hEE measured in a whole-room indirect calorimeter during eucaloric conditions and weight stability prior to starting a 6-week inpatient CR study (50% of daily energy needs). Twenty-four-hour energy expenditure was adjusted via regression analysis for fat free mass (FFM) and fat mass (FM) by DXA. Body composition was reassessed at the end of CR and after 1-year follow-up. Free-living weight was assessed by monthly weight measurements during 12 months.
Results
After 6-week CR, participants lost 8.5 ± 2.7% weight (FFM: –6.3 ± 3.6 kg, FM: –3.4 ± 1.2 kg) but regained 5.1 ± 8.0% 1 year following CR, which was mostly due to FFM regain (+5.7 ± 5.5 kg) and unchanged FM. A relatively higher 24hEE by 100 kcal/day prior to CR was associated with an average greater rate of weight regain by +0.3 kg/month during follow-up and a greater final weight regain by +5.1 kg after 1 year of follow-up.
Conclusion
These results suggest that reduced metabolic efficiency in 24hEE during eucaloric, sedentary conditions may predict greater weight regain after CR-induced weight loss.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Jensen MD, Ryan DH, Apovian CM, Ard JD, Comuzzie AG, Donato KA, et al. 2013 AHA/ACC/TOS guideline for the management of overweight and obesity in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and The Obesity Society. J Am college Cardiol. 2014;63:2985–3023.
Wing RR, Phelan S. Long-term weight loss maintenance. Am J Clin Nutr. 2005;82 Suppl 1:222S–25S.
Muller MJ, Bosy-Westphal A. Adaptive thermogenesis with weight loss in humans. Obesity (Silver Spring). 2013;21:218–28.
Van Baak MA, Mariman ECM. Mechanisms of weight regain after weight loss — the role of adipose tissue. Nat Rev Endocrinol. 2019;15:274–87.
Camps SG, Verhoef SP, Westerterp KR Weight loss, weight maintenance, and adaptive thermogenesis. Am J Clin Nutr. 2013;97:990–4. https://doi.org/10.3945/ajcn.112.050310. Epub 2013 Mar 27.
Leibel RL, Rosenbaum M, Hirsch J. Changes in energy expenditure resulting from altered body weight. N Engl J Med. 1995;332:621–8.
Redman LM, Smith SR, Burton JH, Martin CK, Il’Yasova D, Ravussin E. Metabolic slowing and reduced oxidative damage with sustained caloric restriction support the rate of living and oxidative damage theories of aging. Cell Metab. 2018;27:805–15.e4.
Heinitz S, Hollstein T, Ando T, Walter M, Basolo A, Krakoff J et al. Early adaptive thermogenesis is a determinant of weight loss after six weeks of caloric restriction in overweight subjects. Metabolism 2020; In Press Journal Pre-Proof.
Rosenbaum M, Vandenborne K, Goldsmith R, Simoneau J-A, Heymsfield S, Joanisse DR, et al. Effects of experimental weight perturbation on skeletal muscle work efficiency in human subjects. Am J Physiol-Regul Integr Comp Physiol. 2003;285:R183–92.
Goldsmith R, Joanisse DR, Gallagher D, Pavlovich K, Shamoon E, Leibel RL, et al. Effects of experimental weight perturbation on skeletal muscle work efficiency, fuel utilization, and biochemistry in human subjects. Am J Physiol Regul Integr Comp Physiol. 2010;298:R79–88.
Dulloo AG, Miles-Chan JL, Schutz Y. Collateral fattening in body composition autoregulation: its determinants and significance for obesity predisposition. Eur J Clin Nutr. 2018;72:657–64.
Dulloo AG. Collateral fattening: When a deficit in lean body mass drives overeating. Obesity. 2017;25:277–9.
Jacquet P, Schutz Y, Montani J-P, Dulloo A How dieting might make some fatter: modeling weight cycling toward obesity from a perspective of body composition autoregulation. Int J Obesity. 2020;44:1243–53.
Ellis AC, Hyatt TC, Hunter GR, Gower BA. Respiratory quotient predicts fat mass gain in premenopausal women. Obesity (Silver Spring, Md.). 2010;18:2255–9.
Valtueña S, Salas-Salvadó J, Lorda P. The respiratory quotient as a prognostic factor in weight-loss rebound. Int J Obesity. 1997;21:811–7.
Hainer V, Kunesová M, Parízková J, Stich V, Mikulová R, Slabá S. Respiratory quotient in obesity: its association with an ability to retain weight loss and with parental obesity. Sb Lek. 2000;101:99–104.
Thom G, Dombrowski SU, Brosnahan N, Algindan YY, Rosario Lopez-Gonzalez M, Roditi G, et al. The role of appetite-related hormones, adaptive thermogenesis, perceived hunger and stress in long-term weight-loss maintenance: a mixed-methods study. Eur J Clin Nutr. 2020;74:622–32.
Weise CM, Hohenadel MG, Krakoff J, Votruba SB. Body composition and energy expenditure predict ad-libitum food and macronutrient intake in humans. Int J Obes. 2014;38:243–51.
Basolo A, Votruba SB, Heinitz S, Krakoff J, Piaggi P. Deviations in energy sensing predict long-term weight change in overweight native Americans. Metabolism. 2018;82:65–71.
Piaggi P, Thearle MS, Krakoff J, Votruba SB. Higher daily energy expenditure and respiratory quotient, rather than fat-free mass, independently determine greater ad libitum overeating. J Clin Endocrinol Metab. 2015;100:3011–20.
Piaggi P, Vinales KL, Basolo A, Santini F, Krakoff J. Energy expenditure in the etiology of human obesity: spendthrift and thrifty metabolic phenotypes and energy-sensing mechanisms. J Endocrinol Investig. 2018;41:83–9.
Blundell JE, Caudwell P, Gibbons C, Hopkins M, Naslund E, King N, et al. Role of resting metabolic rate and energy expenditure in hunger and appetite control: a new formulation. Dis Model Mech. 2012;5:608–13.
Blundell JE, Tremblay A. Appetite control and energy (fuel) balance. Nutr Res Rev. 1995;8:225–42.
Piaggi P. Metabolic Determinants of Weight Gain in Humans. Obesity. 2019;27:691–9.
Blundell JE, Finlayson G, Gibbons C, Caudwell P, Hopkins M. The biology of appetite control: do resting metabolic rate and fat-free mass drive energy intake? Physiol Behav. 2015;152:473–8.
Dulloo AG, Jacquet J, Miles-Chan JL, Schutz Y. Passive and active roles of fat-free mass in the control of energy intake and body composition regulation. Eur J Clin Nutr. 2017;71:353–7.
Reinhardt M, Thearle MS, Ibrahim M, Hohenadel MG, Bogardus C, Krakoff J, et al. A human thrifty phenotype associated with less weight loss during caloric restriction. Diabetes. 2015;64:2859–67.
American Diabetes Association. Diagnosis and classification of diabetes mellitus. Diabetes Care 2010; 33 Suppl 1:S62–9.
Ferraro R, Boyce VL, Swinburn B, De Gregorio M, Ravussin E. Energy cost of physical activity on a metabolic ward in relationship to obesity. Am J Clin Nutr. 1991;53:1368–71.
Thearle MS, Pannacciulli N, Bonfiglio S, Pacak K, Krakoff J. Extent and determinants of thermogenic responses to 24 h of fasting, energy balance, and five different overfeeding diets in humans. J Clin Endocrinol Metab. 2013;98:2791–9.
Ravussin E, Lillioja S, Anderson TE, Christin L, Bogardus C. Determinants of 24-hour energy expenditure in man. Methods and results using a respiratory chamber. J Clin Invest. 1986;78:1568–78.
Hollstein T, Piaggi P Supplemental Material - Reduced energy efficiency in eucaloric conditions at low energy turnover predicts long-term weight regain in overweight subjects following sustained caloric restriction and weight loss. In: Harvard Dataverse (Link: https://doi.org/10.7910/DVN/U5SFTH), 2020.
Piaggi P, Thearle MS, Bogardus C, Krakoff J. Lower energy expenditure predicts long-term increases in weight and fat mass. J Clin Endocrinol Metab. 2013;98:E703–7.
Heinitz S, Hollstein T, Ando T, Walter M, Basolo A, Krakoff J, et al. Early adaptive thermogenesis is a determinant of weight loss after six weeks of caloric restriction in overweight subjects. Metabolism. 2020;110:154303.
Ellis MV. Repeated measures designs. Couns Psychol. 1999;27:552–78.
Marshall JA, Scarbro S, Shetterly SM, Jones RH. Improving power with repeated measures: diet and serum lipids. Am J Clin Nutr. 1998;67:934–9.
Keys A, Brožek J, Henschel A, Mickelsen O, Taylor HL The biology of human starvation. Oxford, England, Univ. of Minnesota Press (2 vols). 1950.
Sumithran P, Proietto J. The defence of body weight: a physiological basis for weight regain after weight loss. Clin Sci. 2013;124:231–41.
Pasman WJ, Saris WHM, Westerterp-Plantenga MS. Predictors of weight maintenance. Obesity Research. 1999;7:43–50.
Muller MJ, Enderle J, Pourhassan M, Braun W, Eggeling B, Lagerpusch M, et al. Metabolic adaptation to caloric restriction and subsequent refeeding: the Minnesota Starvation Experiment revisited. Am J Clin Nutr. 2015;102:807–19.
Rosenbaum M, Hirsch J, Gallagher DA, Leibel RL. Long-term persistence of adaptive thermogenesis in subjects who have maintained a reduced body weight. Am J Clin Nutr. 2008;88:906–12.
Fothergill E, Guo J, Howard L, Kerns JC, Knuth ND, Brychta R, et al. Persistent metabolic adaptation 6 years after “The Biggest Loser” competition. Obesity (Silver Spring). 2016;24:1612–9.
Bosy-Westphal A, Schautz B, Lagerpusch M, Pourhassan M, Braun W, Goele K, et al. Effect of weight loss and regain on adipose tissue distribution, composition of lean mass and resting energy expenditure in young overweight and obese adults. Int J Obesity. 2013;37:1371.
Rosenbaum M, Goldsmith RL, Haddad F, Baldwin KM, Smiley R, Gallagher D, et al. Triiodothyronine and leptin repletion in humans similarly reverse weight-loss-induced changes in skeletal muscle. Am J Physiol-Endocrinol Metab. 2018;315:E771–9.
Rosenbaum M, Heaner M, Goldsmith RL, Christian Schulze P, Shukla A, Shen W, et al. Resistance training reduces skeletal muscle work efficiency in weight‐reduced and non–weight‐reduced subjects. Obesity. 2018;26:1576–83.
Hopkins M, Finlayson G, Duarte C, Whybrow S, Ritz P, Horgan GW, et al. Modelling the associations between fat-free mass, resting metabolic rate and energy intake in the context of total energy balance. Int J Obesity. 2016;40:312–8.
McNeil J, Lamothe G, Cameron JD, Riou M-È, Cadieux S, Lafrenière J, et al. Investigating predictors of eating: is resting metabolic rate really the strongest proxy of energy intake? Am J Clin Nutr. 2017;106:1206–12.
Caudwell P, Finlayson G, Gibbons C, Hopkins M, King N, Näslund E, et al. Resting metabolic rate is associated with hunger, self-determined meal size, and daily energy intake and may represent a marker for appetite. Am J Clin Nutr. 2012;97:7–14.
Hollstein T, Piaggi P Metabolic factors determining the susceptibility to weight gain: current evidence. Curr Obes Rep. 2020;9:121–35.
Hollstein T, Ando T, Basolo A, Krakoff J, Votruba SB, Piaggi P Metabolic response to fasting predicts weight gain during low-protein overfeeding in lean men: further evidence for spendthrift and thrifty metabolic phenotypes. Am J Clin Nutr. 2019;110:593–604.
Hollstein T, Basolo A, Ando T, Votruba SB, Walter M, Krakoff J et al. Recharacterizing the metabolic state of energy balance in thrifty and spendthrift phenotypes. J Clin Endocrinol Metab. 2020;105:1375–92.
Pannacciulli N, Salbe AD, Ortega E, Venti CA, Bogardus C, Krakoff J. The 24-h carbohydrate oxidation rate in a human respiratory chamber predicts ad libitum food intake. Am J Clin Nutr. 2007;86:625–32.
Kerns JC, Guo J, Fothergill E, Howard L, Knuth ND, Brychta R, et al. Increased physical activity associated with less weight regain six years after “The Biggest Loser” competition. Obesity. 2017;25:1838–43.
Ostendorf DM, Caldwell AE, Creasy SA, Pan Z, Lyden K, Bergouignan A, et al. Physical activity energy expenditure and total daily energy expenditure in successful weight loss maintainers. Obesity. 2019;27:496–504.
Hägele FA, Büsing F, Nas A, Hasler M, Müller MJ, Blundell JE, et al. Appetite control is improved by acute increases in energy turnover at different levels of energy balance. J Clin Endocrinol Metab. 2019;104:4481–91.
Montesi L, El Ghoch M, Brodosi L, Calugi S, Marchesini G, Dalle Grave R. Long-term weight loss maintenance for obesity: a multidisciplinary approach. Diabetes Metab Syndr Obesity. 2016;9:37.
Acknowledgements
We thank the participants and the clinical staff of the Phoenix Epidemiology and Clinical Research Branch for conducting the examinations. The technical and logistic support of Susan Bonfiglio, PA, in performing procedures and collecting data is gratefully acknowledged.
Funding
This research was supported by the Intramural Research Program of the NIH, The National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). PP was supported by the program “Rita Levi Montalcini for young researchers” from the Italian Minister of Education and Research (Ministero dell’Istruzione, dell’Università e della Ricerca).
Author information
Authors and Affiliations
Contributions
TH, SH, and PP wrote the manuscript. TH, SH, and PP performed data analyses. SBV and JK designed the clinical protocol. AB, JK, and SBV reviewed the manuscript. PP is the guarantor of this work and, as such, had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Hollstein, T., Heinitz, S., Basolo, A. et al. Reduced metabolic efficiency in sedentary eucaloric conditions predicts greater weight regain in adults with obesity following sustained weight loss. Int J Obes 45, 840–849 (2021). https://doi.org/10.1038/s41366-021-00748-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-021-00748-y