Abstract
Background and objective
Intermittent energy restriction continues to gain popularity as a weight loss strategy; however, data assessing it’s long-term viability is limited. The objective of this study was to follow up with participants 12 months after they had completed a 12-month dietary intervention trial involving continuous energy restriction and two forms of intermittent energy restriction; a week-on-week-off energy restriction and a 5:2 programme, assessing long-term changes on weight, body composition, blood lipids and glucose.
Subjects and methods
109 overweight and obese adults, aged 18–72 years, attended a 12-month follow-up after completing a 12-month dietary intervention involving three groups: continuous energy restriction (1000 kcal/day for women and 1200 kcal/day for men), week-on-week-off energy restriction (alternating between the same energy restriction as the continuous group for one week and one week of habitual diet), or 5:2 (500 kcal/day on modified fast days each week for women and 600 kcal/day for men). The primary outcome was weight change at 24 months from baseline, with secondary outcomes of change in body composition, blood lipids and glucose.
Results
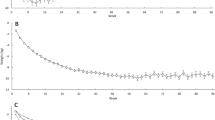
For the 109 individuals who completed the 12-month follow-up (82 female, 15 male, mean BMI 33 kg/m2), weight decreased over time with no differences between week-on and week-off and continuous energy restriction or 5:2 and continuous energy restriction with −4.5 ± 4.9 kg for continuous energy restriction, −2.8 ± 6.5 kg for week-on, week-off and −3.5 ± 5.1 kg for 5:2. Total cholesterol reduced over time and glucose, HDL, LDL and triglycerides were unchanged.
Discussion and conclusion
Intermittent energy restriction was as successful in achieving modest weight loss over a 24-month period as continuous energy restriction.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Varady KA. Intermittent versus daily calorie restriction: which diet regimen is more effective for weight loss? Obes Rev. 2011;12:e593–601.
Wing RR, Jeffery RW. Prescribed “breaks” as a means to disrupt weight control efforts. Obes Res. 2003;11:287–91.
Harvie M, Pegington M. The effects of intermittent or continuous energy restriction on weight loss and metabolic disease risk markers: a randomized trial in young overweight women. Int J Obes. 2011;35:714–27.
Harvie M, Wright C, Pegington M, McMullan D, Mitchell E, Martin B, et al. The effect of intermittent energy and carbohydrate restriction v. daily energy restriction on weight loss and metabolic disease risk markers in overweight women. Br J Nutr. 2013;110:1534–47.
Conley M, Le Fevre L, Haywood C, Proietto J. Is two days of intermittent energy restirction per week a feasible weight loss approach in obese males? A randomsied pilot study. Nutr Diet. 2017;75:65–72.
Keogh JB, Pedersen E, Petersen KS, Clifton PM. Effects of intermittent compared to continuous energy restriction on short-term weight loss and long-term weight loss maintenance. Clin Obes. 2014;4:150–6.
Byrne NM, Sainsbury A, King NA, Hills AP, Wood RE. Intermittent energy restriction improves weight loss efficiency in obese men: the MATADOR study. Int J Obes. 2017;42:129–38.
Headland M, Clifton PM, Carter S, Keogh JB. Weight loss outcomes: a systematic review and meta-analysis of intermittent energy restriction trials lasting a minimum of 6 months. Nutrients. 2015;8:1–12.
Trepanowski JF, Kroeger CM, Barnosky AR, Klempel M, Bhutani S, Hoddy KK, et al. Effect of alternate-day fasting on weight loss, weight maintenance, and cardioprotection among metabolically healthy obese adults a randomized clinical trial. JAMA Intern Med. 2017;177:930–8.
Sundfor T, Svendsen M, Tonstad S. Effect of intermittent versus continuous energy restriction on weight loss, maintenance and cardiometabolic risk: a randomized 1-year trial. Nutr Metab Cardio Dis. 2018;28:698–706.
Headland ML, Clifton PM, Keogh JB. Effect of intermittent compared to continuous energy restriction on weight loss and weight maintenance after 12 months in healthy overweight or obese adults. Int J Obes. 2019;43:2028–36.
Noakes M, Keogh JB, Foster PR, Clifton PM. Effect of an energy-restricted, high-protein, low-fat diet relative to a conventional high-carbohydrate, low-fat diet on weight loss, body composition, nutritional status, and markers of cardiovascular health in obese women. Am J Clin Nutr. 2005;81:1298–306.
Anastasiou CA, Karfopoulou E, Yannakoulia M. Weight regaining: from statistics and behaviours to physiology and metabolism. Metabolism. 2015;64:1395–407.
Harvie M, Howell A. Potential benefits and harms of intermittent energy restriction and intermittent fasting amongst obese, overweight and normal weight subjects—a narrative review of human and animal evidence. Behav Sci. 2017;7:1–22.
National Health and Medical Research Council. Clinical practice guidelines for the management of overweight and obesity In adults, adolescents and children in Australia. Melbourne: National Health and Medical Research Council; 2013.
Wadden T, Butryn ML, Byrne KJ. Efficacy of lifestyle modification for long-term weight control. Obes Res. 2012;12 S12:151S–62S.
Botoseneanu A, Liang J. Social stratification of body-weight trajectory in middle age and older americans: results from a 14-year longitudinal study. J Aging Health. 2011;23:454–80.
Gomersall SR, Dobson AJ, Brown WJWeightGain. Overweight, and obesity: determinants and health outcomes from the Australian Longitudinal Study on women’s health. Curr Obes Rep. 2014;3:46–53.
Anderson KM, Castelli WP, Levy D. Cholesterol and mortality 30 years of follow-up from the Framingham Study. JAMA. 1987;257:2176–80.
Thomas JG, Bond DS, Phelan S, Hill JO, Wing RR. Weight-loss maintenance for 10 years in the National Weight Control Registry. Am J Prev Med. 2014;46:17–23.
Keller KL, Kral TVE, Rolls BJ. Impacts of energy density and portion size on satiation and satiety. In: Blundell JE, Bellisle F, editors. Oxford, UK: Woodhead Publishing; 2013.
Tremblay A, Bellisle F. Nutrients, satiety, and control of energy intake. Appl Physiol Nutr Metab. 2015;40:971–9.
Chapelot D, Aubert R, Mamonier C, Chabert M, Louis-Sylvestre J. An endocrine and metabolic definition of the intermeal interval in humans: evidence for a role of leptin on the prandial pattern through fatty acid disposal. Am J Clin Nutr. 2000;72:421–31.
Melanson K, Westerterp-Plantenga MS, Sarris WH, Smith FJ, Campfield LA. Blood glucose patterns and appetite in time-blinded humans: carbohydrate versus fat. Am J Physiol. 1999;277:R337–45.
Cummings DE, Frayo RS, Marmonier C, Aubert R, Chapelot D. Plasma ghrelin levels and hunger scores in humans initiating meals voluntarily without time—and food-related cues. Am J Physiol Endocrinol Metab. 2004;287:E297–304.
Blom WA, de Graaf C, Lluch A, Stafleu A, Schaafsma G, Hendriks HF. Postprandial ghrelin responses are associated with the intermeal interval in time-blinded normal weight men, but not in obese men. Physiol Behav. 2009;96:742–48.
Callahan HS, Cummings DE, Pepe MS, Breen PA, Matthys CC, Weigle DS. Postprandial suppression of plasma ghrelin level is proportional to ingested caloric load but does not predict intermeal interval in humans. J Clin Endocrinol Metab. 2004;89:1319–24.
Acknowledgements
We would like to thank Louise Massie for her assistance with study organisation and study participants, as well as the study participants for their willingness to participate in the trial. The authors’ responsibilities were as follows: PMC and JBK designed the research, MLH conducted the research and had primary responsibility for the final content of the manuscript, MLH and PMC analysed the data and all the authors revised the manuscript, and read and approved the final manuscript.
Funding
MLH was supported by a University of South Australia Postgraduate Award, funded jointly by the University of South Australia and the Research Training Program. The University of South Australia funded the study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Headland, M.L., Clifton, P.M. & Keogh, J.B. Impact of intermittent vs. continuous energy restriction on weight and cardiometabolic factors: a 12-month follow-up. Int J Obes 44, 1236–1242 (2020). https://doi.org/10.1038/s41366-020-0525-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-020-0525-7